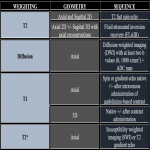
Magnetic resonance imaging (MRI) is the method of choice for investigating white matter lesions, which are a common finding in routine practice. A standard MRI protocol containing the sequences necessary for a reliable characterization of white matter lesions is listed in figure 3.[8]
Additional diagnostic imaging tools such as MR spectroscopy, perfusion measurements or diffusion tensor imaging could provide additional aid in ambiguous cases.[3,4,6]
Imaging findings
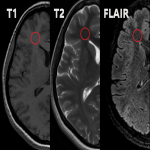
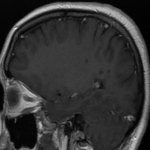
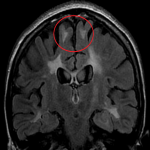
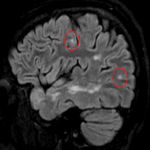
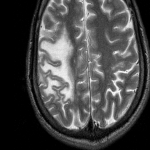
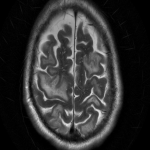
On MR imaging, normal myelinated white matter appears as hyperintense on T1WI and hypointense on T2WI, as a result of decreased water content and increased cholesterol within the myelin sheaths. Lesions in the white matter, either due to demyelinating, dysmyelinating or hypomyelinating processes, usually appear as hyperintensities on T2/FLAIR sequences.[2]
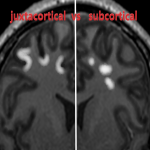
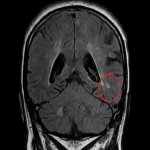
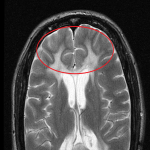
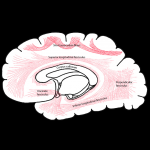
It is important to recognize the distinction between superficial white matter lesion locations:
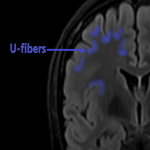
- juxtacortical - directly abuts the cortex (and involving the U fibers);
- subcortical – has an intervening layer of white matter between the lesion and the cortex (and do not involve the U fibers).
Examples of white matter disorders sparing the subcortical U fibers
Cerebral small-vessel diseases have been grouped into 6 aetiopathogenic subtypes [10]:
- Type 1 – arteriolosclerosis;
- Type 2 – cerebral amyloid angiopathy (inherited or sporadic);
- Type 3 – inherited or sporadic, distinct from cerebral amyloid angiopathy;
- Type 4 – inflammatory or immune-mediated;
- Type 5 – venous collagenosis;
- Type 6 – other.
Cerebral Small-Vessel Disease Related to Arteriolosclerosis (type 1)
- One of the most common causes of white matter lesions, being a systemic disease related to vascular risk factors and aging.
- Pathologically it consists of wall thickening and lumen narrowing of the small vessels as a result of lipohyalinosis, fibrinoid necrosis and microscopic atheromatous deposits [5,10].
- The radiological expression is heterogenous and includes white matter lesions, lacunar infarcts, microbleeds and brain atrophy [5,10].
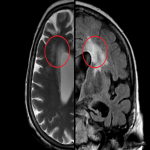
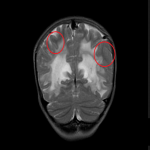
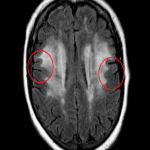
- MRI findings: White matter lesions appear as T2WI hyperintensities located in vascular end-zones within the deep white matter such as the periventricular region, centrum semiovale and corona radiata, usually sparing the subcortical U fibers (due to their protective collateral blood flow mentioned earlier). They can progress in time from infracentimetric lesions to confluent areas of T2WI hyperintensity [2,5].
Cerebral Amyloid Angiopathy (type 2)
- It is characterized by amyloid protein deposition in the vessel walls.
- MRI findings: frequently presents with some form of hemorrhage (from microbleeds to lobar hemorrhages), as well as T2WI white matter hyperintensities secondary to ischemia [10].
Cerebral Small-Vessel Disease Related to Radiotherapy or Chemotherapy (type 6)
- MRI findings: it presents with focal or confluent white matter lesions, typically sparing the subcortical U-fibers [2].
Dysmyelinating disorders
- Represented by leukodystrophies, a group of diseases characterized by inherited enzymes deficiencies that alter the normal metabolism of myelin and include pathological entities such as Metachromatic Leukodystrophy and X-linked Adrenoleukodystrophy.
- Due to their slow rate of myelin metabolism, the subcortical U-fibers are typically spared until advanced stages of disease progression.
- There are however two notable exceptions to this rule, Alexander disease and Canavan disease.
- MRI findings:
- Metachromatic Leukodystrophy – symmetric deep white matter T2WI hyperintensity, sparing the U fibers.
- X-linked adrenoleukodystrophy – posterior deep white matter confluent T2WI hyperintensity, initially sparing the U fibers; in advanced stages of the disease it progresses to involve association white matter tracts (visual and auditory) and cortico-spinal tracts.[2]
Examples of white matter disorders involving the subcortical U fibers
Multiple Sclerosis (MS)
- Represents a primary demyelinating disease with a perivenular distribution of inflammation and demyelination with axon preservation, having an autoimmune substrate.
- MRI findings:
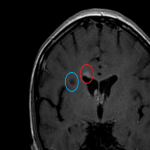
- Nonspecific white matter plaques appearing as T2WI hyperintensities most frequently encountered in contact with the atria and occipital horns of the lateral ventricles, as well as the corpus callosum and in the subcortical U fibers.
- Actively demyelinating plaques can enhance after contrast administration, as well as present restricted diffusion on DWI.
- MRI findings can demonstrate dissemination in space (at least one T2WI hyperintense lesion ≥3 mm in long axis in at least two different regions) and dissemination in time (simultaneous presence of both an enhancing and non-enhancing lesion after contrast administration or new lesions detected on follow-up examinations) and need to be correlated with other clinical and paraclinical investigations according to the McDonald diagnostic criteria (revised in 2017).
- The defining locations for space dissemination of white matter lesions include the periventricular, juxtacortical, infratentorial and spinal regions.[2,5,8,9]
Progressive Multifocal Leukoencephalopathy (PML)
- It is an infectious demyelinating disease caused by the reactivation of the JC virus in immunocompromised patients leading to lysis of oligodendrocytes and subsequent impairment of myelin production.
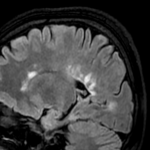
- MRI findings: Asymmetric confluent white matter T2WI hyperintensities located most frequently in the parieto-occipital regions, typically involving the U-fibers with central progression from the subcortical area to the periventricular white matter.[2]
Acute Disseminated Encephalomyelitis (ADEM)
- It is an inflammatory demyelinating disease thought to be caused by immunological cross-reactivity to antigen-antibody complexes which result from prior viral infection or certain types of vaccinations.
- MRI findings: T2WI hyperintensities located in both gray and white matter, frequently involving the U-fibers, sometimes with patchy areas of restricted diffusion and contrast enhancement. Spinal involvement can also be seen, defined as a longitudinally extensive (corresponding to >2 vertebral body heights) T2WI hyperintensity along the spinal cord.[2,5]
Cerebral Autosomal-dominant Arteriopathy with Subcortical Infarcts and Leukoencephalopathy (CADASIL)
- It is an inherited non-arteriosclerotic, non-amyloid small vessel disease (type 3 cerebral small-vessel disease) characterized by deposition of osmiophilic material around the smooth muscle cells of small leptomeningeal and perforating arteries, leading to loss of vascular smooth muscle and subsequent narrowing and obliteration of the vessels.
- MRI findings: White matter T2WI hyperintensities that have a characteristic progression in time, initially being localized in the anterior temporal lobe with ensuing involvement of the frontal and parietal regions, as well as the corpus callosum and external capsule. Subcortical lacunar infarcts are a common finding and U-fiber involvement is possible in certain locations, due to the preferential involvement of cortical arteries in the anterior temporal and superior frontal regions. In the advanced stages of the disease, extensive areas of demyelination, lacunar infarcts and microbleeds are present [2,5].
Alexander and Canavan diseases are an atypical example of dysmyelinating diseases involving the subcortical U-fibers early in the disease progression [2].
Pelizaeus-Merzbacher disease is a rare hypomyelinating disorder, characterized by a global myelin deficit and an abnormal, relatively homogenous and diffuse T2WI hyperintensity of the white matter, including the U fibers, correlated with normal myelination patters of the pediatric population [6].
An overall view on U fiber involvement in a variety of white matter disorders is shown in figure 21.