Type:
Educational Exhibit
Keywords:
Pancreas, CT, MR, Imaging sequences, Education and training
Authors:
J. J. Kolleri, S. B. Ladumor, A. L. F. Yasin, A. Sadiq, A. H. M. Sha'ban, A. M. J. Thabet, M. L. M. Hussein
DOI:
10.26044/ecr2022/C-14169
Background
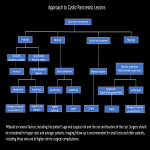
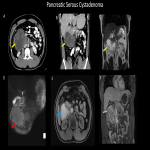
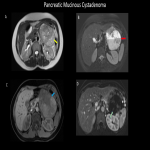
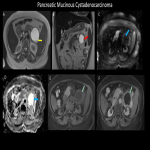
A plethora of cystic pancreatic lesions are encountered on cross sectional imaging in daily practice. The radiology plays a major role in the diagnosis and characterization of these pancreatic lesions. Multi-modality imaging, such as US, multi-detector CT, MRI, endoscopic ultrasonography, SPECT, and PET/CT, can help in prompt diagnosis and helps in management plan. MRI has improved the analysis and morphological distinction of pancreatic lesions, and are now widely accepted as the principal imaging modality. The majority of these lesions are benign or indolent neoplasms of low grade.
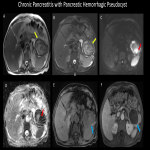
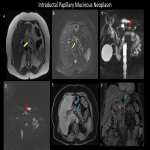
Abdominal pain is the most common manifestation of symptomatic cysts. When a lesion communicates with the pancreatic ductal system or obstructs the pancreatic or biliary duct, it causes jaundice or recurrent pancreatitis. Patients with advanced cystic malignancies may experience symptoms similar to pancreatic cancer (pain, weight loss, jaundice, etc.). Pseudocysts typically occur in acute pancreatitis, but they can also develop slowly into chronic pancreatitis. However, a premalignant or malignant lesion is diagnosed in a considerable number of patients. Cysts in the head of the pancreas require more sophisticated and aggressive surgery than cysts in the tail, hence the location of the cyst can influence the treatment decision. Radiologists play a crucial role in detection and characterization of these lesions. Understanding the various imaging features of pancreatic cystic lesions will aid radiologists achieve more precision in diagnostic reporting.