Type:
Educational Exhibit
Keywords:
Musculoskeletal joint, Digital radiography, Diagnostic procedure, Motility
Authors:
E. tallamona, G. Belfiore, A. Di Mari, S. Cusumano, T. vasile, R. Farina, I. Pennisi, S. Palmucci, A. Basile
DOI:
10.26044/ecr2022/C-19187
Background
Pediatric elbow fractures constitute up to 15% of all pediatric fractures [1]. According to a study of Emery K. H. et al. the three most common pediatric elbow fractures include supracondylar (56%), radial neck (17%), and lateral condylar (15%) fractures [2].
Most traumatic elbow injuries associate with both hyperextension/rotation movements and valgus/varus stress forces applied to the elbow joint. Less often they could be caused by direct impact forces [3].
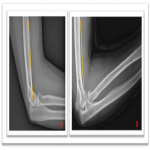
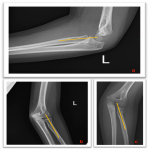
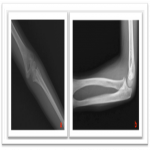
After trauma children admitted to the emergency department (ED) are usually addressed to perform further diagnostic exams. The standard first-line diagnostic examination includes anteroposterior (AP) and lateral (LL) radiographs. On radiographs pediatric elbows fractures are some of the most elusive to detect. Their assessment may be insidious for non-pediatric expert radiologists. Diagnostic pitfalls are mostly due to the lack of knowledge of non-ossified children epiphysis, but also to an often poor quality of the acquired radiographs for the uncooperative children during the exam acquisition [4, 5, 2].
In a study of Bisset et al. a total of 1033 musculoskeletal pediatric elbow radiographs were reviewed; they reported 33 total diagnostic errors with a 3.8% miss rate and a 2.7% overall rate [6].
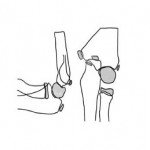
In order to avoid recurrent diagnostic errors it is important to shoot the radiographs following the conventional standard technique and paying attention to the little patient position. In particular, the standard lateral elbow radiograph must be acquired with internal shoulder rotation and full elbow contact with the forearm cassette [4,7]. Only correctly performed AP and LL elbow radiographs lead to a proper evaluation of the virtual anterior humeral line, the fat pad sign, and the virtual radiocapitellar line [8]. In addition, radiologists should always search for the ‘‘teardrop sign” in the LL projection which is useful to check the accuracy of the LL radiograph, but also to verify any persistent instability after reduction in patients with elbow dislocation [4,9]. Never more as in this scenario the evaluation of the anatomical relationship among all the ossification centers with themselves and the main bones appears extremely important [3, 10]. Anatomical variants may resemble pathology and additional potential mistakes to avoid [11].
Elbow fractures include fractures of the humeral blade, of the proximal radius end and the proximal ulna end. Fractures of the humeral blade can be further divided into supracondylar fractures, condyle fractures, trochlea fractures, epicondyle fractures and epitrochlear fractures, to which intercondylar fractures could be add [2]. In a study of Attarian D.E. the non-displaced lateral condyle fractures are considered the most challenging to detect; they are often missed and if left untreated, can potentially produce disastrous outcome [12].