Through a search in our RIS-PACS database we selected all the post-trauma elbow traditional radiographs requested by the ED from 1st January 2021 to 31st June 2021 for patients under the age of 18. We found a total of 55 pediatric patients. It was decided to narrow the pool of study by choosing only the patients who underwent a second radiological examination (usually required within 24 hours) and/or those who were treated by orthopedics (with a plaster cast or surgically) despite a first radiologic report negative for fracture. This reduced the selected cases to a group of 7 patients. The patients whose elbow x-ray reports were positive for fracture at first examination were excluded from the study. For every selected case we scrupulously analyzed both the first and the follow-up radiograph reporting in a database the major radiological features suggestive for elbow fracture which could have led to a proper diagnosis if properly observed. This let us to create a practical guide with some tips to avoid further mistakes. In order to let this guide be as simple as possible we will show pictures of both occult and clearly visible fractures.
Step 1: Assessment of the lateral elbow radiograph. To estimate if the LL radiograph is correctly taken check for the so-called Hourglass/teardrop/eight sign (Fig.1). The teardrop shape result from the anterior margin of the olecranon fossa, the posterior margin of the coronoid fossa and the inferior portion of the capitellum ossification center profile. If clearly recognized on radiographs this sign indicates that you are looking at a true lateral.
Step2: Anterior and/or posterior fat pad sign (Fig.2). Normally the anterior fat pad lies in the coronoid fossa and the posterior fat pad in the olecranon fossa. On a lateral radiograph the anterior fat pad may be visible as slight triangular lucency area along the anterior side of the distal humerus, while normally no lucency is visualized along the posterior cortex [11].
A posterior increased lucency is never normal and it is usually described on reports as “posterior fat pad sign”. Every time it is found it implies disruption of the joint surface of the bone cortex. Also sometimes it may serve as the only indirect sign to detect occult fractures.
An anterior increased lucency is described as a "sail sign", because it is unusually prominent and bows outward to form a triangular shape. It is related to occult articular fractures.
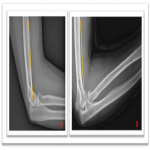
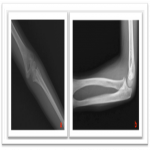
Step 3: Anterior humeral line. This is a virtual line drawn along the anterior cortex of the humerus diaphysis which should intersect the middle third of the capitellum on the lateral view. Unfortunately, if the radiograph is not a true lateral, the interpretation of the anterior humeral line becomes fallible causing diagnostic errors (Fig.3). The anterior humeral line is the key to assess suspected subtle supracondylar fractures which often results in posterior displacement of the capitellum and consequentially anterior displacement of the humeral line. This rule holds for most normal children, but in some cases (especially under the age of 4) it may physiologically pass through the anterior third. In these cases, look for any ancillary signs such as cortical irregularity suggesting elbow fractures.
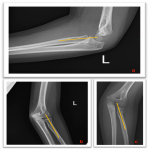
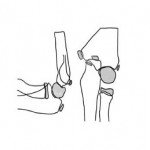
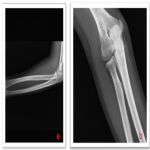
Step 4: Radiocapitellar line. This is a virtual line drawn through the middle of the radius till the humeral distal epiphysis which should bisect the radial head and the capitellum center on both the lateral and the anterior-posterior elbow radiograph (Fig.4). Failure in a proper alignment indicates a radial head dislocation.
Step 5: Ossification center (Fig.5). Check for any cortical disruption or linear lucency in each ossification center.
The distal humerus, the ulna and radio proximal epiphyses have 6 ossification centers around the elbow joint: capitellum (C), radial head (R), internal or medial epicondyle (I), trochlea (T), olecranon (O), lateral or external epicondyle (L). Because they all appear and fuse at different ages, the acronym “CRITOL” is often used, as a mnemonic rule, to describe the usual chronological order of their appearance. The capitellar ossification center appears at 1-2 years of age, the radial head at 2-4 years, the internal epicondyle at 4-6 years, the trochlea at 8-11 years, the olecranon at 9- 11 years, and the lateral epicondyle at 10 -11 years. Remember that this order of appearance may be extremely variable except for the medial epicondyle ossification center that always appears before the trochlear center. After a trauma If the trochlear center is visible and the medial epicondyle is not a displaced medial epicondyle should be suspected.
Step 6: Inspection of the radial had. Look for subtle disruptions of the bone cortex since fracture lines are often not visible at first sight. Non reported intra-articular fracture can cause adequate treatment delay with suboptimal or bad outcome (Fig.6).
Step 7: Distal humerus epiphysis. Signs of humeral fracture are also commonly subtle; all the epiphyseal ossification cores must carefully be analyzed (Fig.7).
Step 8: Olecranon and ulna examination. Look for obvious fracture lines and subtle disruptions in cortical contour (Fig.8).