Results:
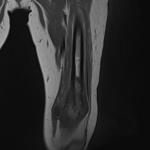
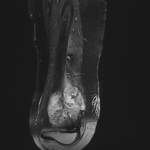
11 patients had osteosarcoma, with radiography and computed tomography (CT) showing osteolytic bone destruction or/andosteoblastic bone sclerosis as well as an aggressive periosteal reaction, a soft-tissue mass and cancerous bone. The tumors appeared as mixed magnetic resonance imaging signals that were inhomogeneously enhanced. A total of 8 patients presented with Ewing sarcoma, with radiography and CT showing invasive bone destruction and a soft-tissue mass. On MRI theyhad mixed low signal on T1-weighted images and high signal on T2-weighted images. 1 patient had chondrosarcoma presenting as a local cortical bone destruction and a soft-tissue mass containing scattered amorphous calcifications. MRI revealed mixed low T1 signal and high T2 signals. 1 patient presented with lymphoma involving the L1 and L2 vertebrae. CT showed vertebral bone destruction, a soft-tissue mass. MRI showed a soft-tissue mass with low T1 signal and high T2 signal and marked inhomogeneous enhancement. Osteosarcoma was the most common primary malignant bone tumor, followed by Ewing sarcoma. Osteoblastic or osteolytic bone destruction, an invasive periosteal reaction, soft-tissue masses, a tumor matrix and inhomogeneous enhancement were important imaging features of malignant bone tumors.
Discussion :
Imaging techniques play an important role in the diagnosis process, work up and staging of malignant bone tumors and thus in deciding the management of these tumors. The diagnosis usually requires multimodality approach; plain radiography, CT scan, MRI, bone scintigraphy and PETCET-PETMRI. Each modality contributes in a different way in evaluating the tumor.
Plain radiography: Usually the first examination be performed for symptoms such as pain and swelling. It’s preferable for the radiographs to be performed in two planes AP and Lateral/oblique. It’s the most optimal way for primary evaluation of bone tumors as it allows characterization of the lesion (margins, edges of the lesion, matrix mineralization, cortical involvement and periosteal reaction) [1,2]
CT scan: This technique allows precise anatomical evaluation of the lesions even in complex anatomical location, it helps detect minor bony changes, calcifications, tumor mineralization as well as cortical changes and periosteal reactions. CT scan allows 3D evaluation of the tumor and provides measurements required for the surgery. CT scan is also used for staging through abdominal and chest CT. However, characterization of soft tissue and medullary extension are better analyzed with MRI [3,4].
MRI : it’s the best tool for local staging of the tumor as it allows excellent characterization of soft tissue and bone marrow changes. MRI is also indicated when plain radiography fails to show any abnormality in symptomatic patients. Newer techniques are used such dynamic contrast enhanced imaging, diffusion weighted imaging and spectroscopy. Diffusion weighted images and perfusion help differentiate malignant and benign tumors by evaluating tissue cellularity and the presence of viable tissue or necrosis. Malignant tumor are characterized with a high cellularity thus a restricted diffusion. Dynamic MRI also help guide the biopsy by delineating the location of viable tumor and also monitoring changes after chemotherapy [5,6,7].
Primary bone tumors have specific radiographic features such as the margins of the lesion, zone of transition, cortical changes and periosteal reaction. Both margins and the zone of transition define the rate of growth of the tumor and can be classified into three types [8,9,10]:
Type 1: geographic lesions with 3 subtypes, 1A : well defined borders and sclerotic margins, 1B: lesions without sclerotic margins and narrow zone of transition and 1C: ill defined margins.
Type 2: non geographical lesions with broad zone of transition and moth eaten pattern of destruction
Type 3: non geographical lesions with broad zone of transition and permeative pattern of destruction
Matrix mineralization determines the morphology of the tumor like osteoid, chondroid or fibrous lesions. Periosteal reaction defines the growth of the potential bone tumor and determine the aggressiveness of the lesion. Solid periosteal reaction indicates slow growth, whereas multilamellated periosteal reaction also known as onionskin appearance indicates intermittent aggressive growth (for example in Ewing sarcoma). Interrupted periosteal reaction giving a sunburst appearance or spiculated appearance is seen in aggressive tumors suggestive of malignancy (osteosarcoma, Ewing …). Extra osseous growing lesions can elevate the periosteum from the underlying cortex resulting in a triangular interface also known as Codman’s triangle [11,12].