A. Review of Gynecologic Cancer-Related Surgical Treatment and Anatomical Changes
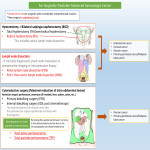
1. Treatment of advanced gynecologic cancer (Fig.2,3)
The basic gynecological surgeries are hysterectomy with bilateral salpingo-oophorectomy (BSO), lymph node dissection, and cytoreductive surgery for ovarian cancer/primary peritoneal cancer/fallopian tube cancer.
- Hysterectomy: Total hysterectomy (TH) is standard procedure, and radical hysterectomy (RH) is usually performed for endometrial carcinoma extending to the uterine cervix and advanced cervical cancer. Radical hysterectomy includes pelvic lymph node dissection (PLN).
- Bilateral salpingo-oophorectomy (BSO): In most gynecologic cancer treatments, the ovaries are often resected; however, in younger patients with early clinical stage or low-grade cancer histology, ovarian-sparing surgery may be performed to preserve fertility and avoid postoperative menopausal symptoms (Fig.6).
- Lymph node dissection: This procedure is performed when clinically diagnosed lymph node metastases in regional lymph node (pelvic and paraaortic lymph node) are detected by preoperative imaging or intraoperative biopsy. The procedure is highly invasive, therefore more detailed indications are considered. As an example, excluding lymph node dissection for advanced ovarian cancer reportedly resulted in a better prognosis in cases wherein complete surgery (≤1 cm residual tumor) was possible and no lymph node metastases were detected[1].
- Cytoreductive surgery: Cytoreductive surgery aims at the maximum reduction of intra-abdominal lesions and is based on peritonectomy and omentectomy; however, in cases involving invasion of other organs such as the liver, spleen, and intestine, lesions should be resected. The maximal diameter of the residual tumor after cytoreductive surgery significantly correlates with prognosis. Therefore, surgeons aim for a residual tumor diameter of ≤1 cm as complete surgery[2]. In recent years, total peritoneal dissection, rather than conventional selective peritoneal dissection, has been reported to target microscopic dissemination and improve prognosis in advanced ovarian cancer[3–6].
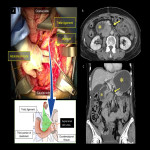
As techniques with high-degree retroperitoneal stress, RH, total parietal peritonectomy (TPP: new treatment), and lymph node dissection are described in detail in Fig.3.
2. Anatomical changes after surgical treatment
If the disease is less advanced and can be treated with a simple hysterectomy, a few selective peritoneal dissections, or a retroperitoneal biopsy, no major anatomic changes occur postoperatively. In case of an advanced disease requiring RH, pelvic or total parietal peritonectomy (TPP), and pelvic with/without para-aortic lymph node dissection (PLN±PAN), there is significant damage to the peritoneum and retroperitoneum, and characteristic findings:
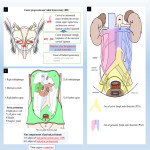
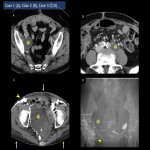
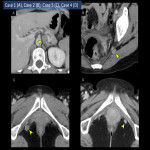
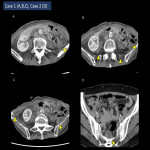
- Intraperitoneal exposure of the retroperitoneal organs (Fig.4): Postoperative ascites is observed near the bone and muscle of the pelvis in the deep retroperitoneum and around the aorta due to the thinning and loss of the retroperitoneum. Peritonectomy may reduce peritoneal irritation symptoms induced by inflammation and urine with urinary tract disruption and may delay absorption of refractory ascites by lymphatic leakage due to reduced peritoneal resorption capacity, thus delaying their detection[6]. As described later, exposed vessels can cause internal herniation followed by strangulated bowel obstruction[7] (Fig.13 D).
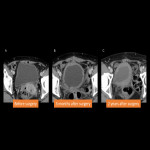
- Retroperitoneal and extrapelvic deviation of postoperative air (Fig.5): The air is seen after radical treatment of advanced gynecological tumors and may extend beyond the pelvis, probably as a result of surgical manipulation.
- Ovarian transportation (Fig.6): If possible, ovarian transportation is performed to avoid postoperative menopause and to preserve fertility. The ovary is often fixed above the pelvis for postoperative pelvic radiotherapy. Note that malignancies such as primary cancer and metastasis may occur in these preserved ovaries.
B. Review of Common and New Post-Treatment Complications
1. Common post-treatment complications
Complications include damage to the retroperitoneal organs such as blood vessels, lymphatic vessels, nerves, and the ureters [8]. These are divided into direct and indirect types:
(1) Complications due to direct involvement
These occur relatively early in the postoperative course and often need intervention.
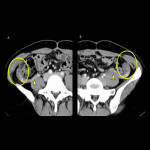
- Lymphatic disruption (Fig.7): The most common complication that requires intervention when accompanied by infection or perforation of the abdominal cavity resulting in refractory ascites.
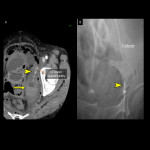
- Vascular injury (Fig.8): An important complication; interventional radiology is often required when there is arterial bleeding into the abdominal cavity.
- Others (Fig.9): Other direct involvement included intestinal injury and hematoma of the abdominal wall. Intestinal injuries require resection. Hematoma of the abdominal wall is treated conservatively unless infected. Acute ureteral injury is often identified intraoperatively and is not discussed here.
(2) Complications due to indirect involvement
It occurs relatively late due to the invasion of the nutrient vessels of organs such as the ureter and bladder. Active intervention is often unnecessary.
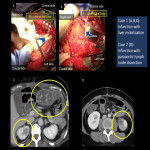
- Subacute ureteral disruption (Fig.10): It is thought to be caused by damage to the nutrient vessels. Although an acute ureteral injury is relatively easy to diagnose from the appearance of the abdominal drain, subacute ureteral injury is often difficult to diagnose. In many cases, the diagnosis can be made by imaging.
- Hydronephrosis (Fig.10): It is often a result of recurrence, but it is also a result of postoperative scarring and one should be familiar with this.
- Postoperative bladder disorder (Fig.11): It is common after highly invasive radical treatments such as RH and thought to be an effect of nutritional vascular and neurological disorders.
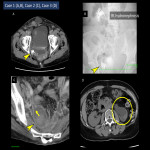
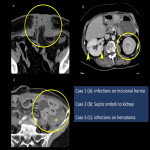
- Infections (Fig.12): Postoperative infections are also crucial, presenting as infection of the abdominal incisional hernia, CV port infection with septic emboli to the kidneys, and an infection of a postoperative hematoma.
2. New post-treatment complications
With the recent expansion of indications for peritonectomy and lymph node dissection to upward extension, complications previously unseen have been identified.
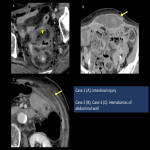
- Diaphragmatic hernias (Fig.13)[6,9]: They may occur intraoperatively or after TPP, and treatment is considered when symptoms are present. Other possible sites of herniation are located in the pelvic region, most commonly the external iliac artery; the common iliac, ureteral, and obturator nerves are also known as the potential sites[7].
- Organ infarction (Fig.14): Infarction of the liver and kidney after liver mobilization in TPP, probably due to the compression of nutritional vessels during TPP. Liver mobilization is common in hepatobiliary and pancreatic surgery and is well-known in this field [6]. In another case, renal infarction after PAN is probably due to renal vascular injury during PAN. Both cases improved with conservative therapy.
- Mobilization of the third portion of the duodenum with ileus (Fig.15): The horizontal duodenum was folded back around the SMA because the suspensory ligament of Treitz and retroperitoneum were resected during PAN, probably due to mechanical stress on the peritoneum in the suprarenal vein area. It caused ileus, but not in all cases. Recently, the expansion of the area of lymph node dissection in the direction of the suprarenal vein area has been studied, and it is expected to be seen more frequently in the future[10,11].
C. Review of Common and New Post-treatment Recurrence
1. Common post-treatment recurrence
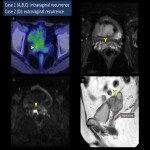
- Intravaginal and extravaginal recurrences near the vaginal stump (Fig.16): Radiation therapy is recommended[12] as a potentially curative treatment for local recurrent cancer; however, in recent years surgical treatment has also been considered [13–15].
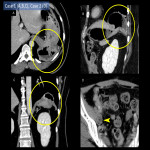
- Recurrence of peritoneal dissemination (Fig.17): Recurrence in the parietal peritoneum is common. It can obstruct the intestine and result in ileus.
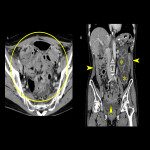
- Recurrence of lymph node metastasis (Fig.18): The regional lymph nodes are common sites of recurrence. After lymph node dissection of these sites, recurrence is common outside the dissected area; suprarenal para-aortic lesions are common. Rare site of lymph node metastasis is greater sciatic foramen or ischiorectal fossa lymph node metastases are rare metastatic lesions (Fig.18). Moreover, mimicker, such as venous dilatation, is present at these sites.
2. New post-treatment recurrence
- Retroperitoneal dissemination (Fig.19): In cases after RH or TPP, recurrence occurs deep in the retroperitoneum due to the absence of the peritoneum. In the early stages of recurrence, the lesions are likely to missed.