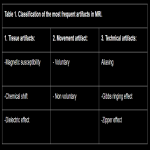
1. Tissue artifacts:
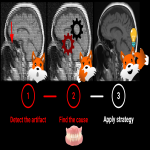
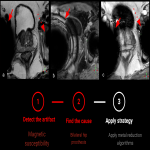
Magnetic susceptibility (also called metal artifact) (fig 2)
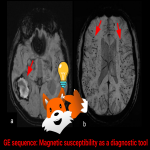
Definition: Magnetic field distortion due to a material with a particular susceptibility. It appears along air-tissue interfaces, near surgical implants or clips, or around metallic bodies or molecules such as deoxyhemoglobin, and in this case it can be used as a diagnostic tool. (fig 3)
Identification: Displacement, blurring and signal dropout artifacts at proximity of some material. The most sensible sequences are the Gradient Echo sequences (GE) and Diffusion Weighted Imaging (DWI). Also, sequences with fat suppression are especially sensitive. (1)
Strategy:
- Remove ferromagnetic foreign bodies if possible
- Reduce voxel size
- Reduce echo time (TE)
- Reduce water fat shift
- Avoid GE and echo-planar sequences
- Avoid use of fused light bulbs in the MR room (use LEDs), because impurities in filament light bulbs can cause this artifice
- Switch patients on a MR device with lower magnetic field strength (2)
- Apply metal reduction algorithms (Philips O-Mar ; Siemens Warp)
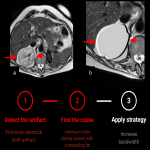
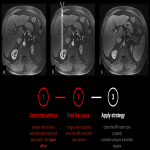
Chemical shift (fig 4)
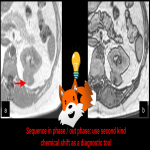
Definition: Chemical shift (CS) phenomenon is also known as “misregistration” or “mismapping”. When substances of markedly different molecular composition are immediately adjacent to each other, localized image misregistration occurs at the interface between the substances. Such artifacts emerge from the chemical shift margin between fat and water (2). There are 2 kinds of CS artifacts. The severity of the pixel shift mainly depends on the receiver bandwidth. The chemical shift artifact occurs on both spin-echo (SE) and GE sequences. This artifact can be used to detect fat content within lesions, e.g. in adrenal adenomas. (1) (fig 5)
Identification: Dark and Light bands on the opposite sides of a structure (For example the kidney) in the frequency direction (first kind), or an entire ghost image of the fat distribution in the anatomy (second kind). (2,3)
Strategy:
- increase bandwidth (larger field of view (FOV))
- increase gradient intensity to decrease limits of the chemical shift
- increase phase or TE for first kind CS ; check TE is in phase (2.2 ms at 1.5T and 1.1 ms at 3T) for second kind CS
- prefer SE to GE sequences
- use a larger gradient to decrease limits of the chemical shift
- fat saturation or inversion recovery are very useful (fat suppression technique eliminates chemical shift artifacts) (4)
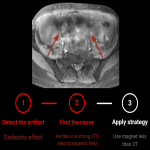
Dielectric effect. (fig 6)
Definition: Also called “standing wave effects”. Conducting artifacts (“dielectric effects”) can be seen in profuse ascites, obese or pregnant patients. It is due to the high magnetic field in the 3T that can't maintain its homogeneity. (4,5)
Identification: Bright or dark “holes” in regions away from the receive coil caused by interference with the standing waves. These artifacts become more pronounced the larger the region of interest.
Strategy:
- pregnant patients should always be explored at 1.5 T
- ascites can be handled by switching to a lower magnetic field device or drained before the exam. (6)
- parallel RF transmission or any other technology improving RF emission homogeneity will reduce dielectric effects (e.g : Philips MultiTransmit, Siemens TimTx, GE MultiDrive, Canon Multiphase Transmit).
2. Movement artifact
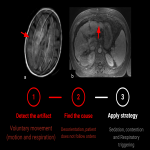
Voluntary (fig 7)
Definition: Artifacts due to patient motion during an examination, in this case voluntary.
Identification: If the motion takes place during a data acquisition, additional phase terms related to the motion path will be created in the data, generating “ghost” lines. On the other hand, motion between acquisition intervals causes inconsistencies because the data acquired before and after the movement do not correspond to the same anatomical arrangement or pose. (7)
Strategy:
- Communication with the patient is essential to manage voluntary movements (e.g : ask patient not to contract muscles during acquisition, explain acquisition phases)
- Any system improving patient comfort within the MR tunnel (cushions, screens and mirrors projecting images, animations or the examination timeline)
- Respiratory triggering and/or breath hold
- Claustrophobia and stress can be managed with a small dose of benzodiazepines (in absence of contraindications).
- Hypnosis has also been proved effective. (8)
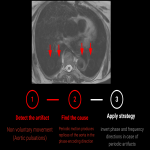
Non voluntary (fig 8)
Definition: non voluntary artifacts can be random (like bowel or ureteral peristalsis) or periodic (like cardiac pulsations or breathing).
Identification: Periodic motion produces ghosts or replicas of the moving structure in abnormal but predictable locations.
Strategy:
- use antiperistaltic drug (phloroglucinol/ triméthylphloroglucinol)
- invert phase and frequency directions in case of periodic artifacts (displaces them on the other axis), as they occur following the phase-encoding direction (9)
- reduce acquisition time
- repeat the sequence (artifacts may appear outside of the region of interest)
- apply AI post-processing algorithms (10)
3. Technical artifacts
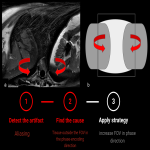
Aliasing (fig 9)
Definition: Occur when the diameter of the imaged object exceeds the FOV. It is due to a low bandwidth in the frequency encoding direction. It has a more complex cause in the phase encoding direction.
Identification: Anatomical structures located outside the FOV are mapped at the opposite end of the image.
Strategy:
- increase FOV in phase direction
- change the direction of the phase encoding gradient (11)
- change foldover direction
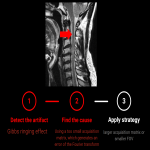
Gibbs ringing effect (fig 10)
Definition: Gibbs ringing artifact (truncation artifact) is caused when using a too small acquisition matrix, which generates an error of the Fourier transform.
Identification: a series of parallel bands like areas of alternating high and low signal intensity in the MR image at sharp transition edges of an object.
Strategy:
- repeat the scan with a larger phase-encode matrix (3,4,9)
- larger acquisition matrix or smaller FOV. Phase encoding matrix should never be less than half of the frequency-encoded matrix (3).
Zipper effect (fig 11)
Definition: Caused by external radio frequency (RF) emission finding its way into the magnet room and being picked up by the receiving coils. This may be due to a break in the Faraday cage, the metal shield built into the walls, floor and ceiling of the scan room.
Identification: It appears as a line of alternating light and dark pixels, sometimes two or three pixels wide, extending across the image in the phase-encoded direction.
Strategy:
- Using all monitoring materials adapted to MRI and closing the door are the most common solutions. (3,9)