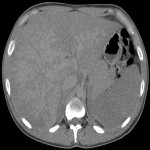
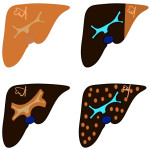
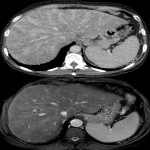
1. CIRRHOSIS:
It is the final stage of chronic liver disease, characterized by progressive fibrosis and increased risk of hepatocarcinoma (HCC). It is a spectrum of presentation ranging from no significant alterations to extensive fibrosis. Some of its main features are described below:
-Liver morphology alterations: right lobe atrophy, left and caudate lobes hypertrophy.
- Hepatic hilum enlargement, indentation of the posterior margin ("right posterior notch sign") and interlobar fissures widening.
- Early heterogeneous enhancement and late wedge-shaped abnormalities (fibrosis) in multiphasic studies.
2. VASCULAR DISEASE
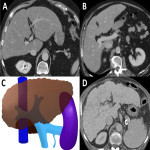
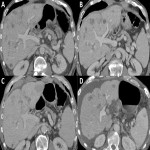
2.1 Budd-Chiari syndrome
Obstruction of the non-portal hepatic venous system. It can be primary (congenital) or secondary (thrombosis related to chemotherapeutic treatments, radiotherapy, or hypercoagulability state).
It can be classified into three types according to the thrombosis location:
- Type I (truncal): inferior vena cava (IVC) occlusion with or without involvement of hepatic veins.
- Type II (radicular): major hepatic veins occlusion.
- Type III (veno-occlusive): small centrilobular veins occlusion.
Typical radiological findings:
In large vessel thrombosis scenario, we can see the IVC and/or hepatic veins hyperdense in non-contrast CT and filling defects after intravenous contrast administration.
- Acute phase: decreased enhancement in peripheral regions with increased uptake in central areas and caudate lobe.
- Advanced stages: heterogeneous peripheral enhancement and development of intrahepatic and systemic venous collateral pathways.
- Heterogeneous hypertrophy of the caudate lobe is characteristic given its different venous drainage (caudate lobe drains directly to the inferior cava vein without depending on hepatic veins).
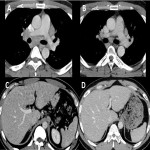
2.3 Congestive hepatopathy
Hepatic manifestations secondary to cardiopulmonary diseases with increased central venous pressure such as congestive heart failure, cardiac surgery, valvular heart disease or constrictive pericarditis. Elevated central venous pressure leads to hepatic flow decrease, with an increase in hepatic venous pressure causing sinusoidal congestion.
Typical radiological findings:
- Contrast reflux from heart to IVC and hepatic veins with increased of its caliber.
- Slowed enhancing parenchyma near hepatic veins secondary to congestion, which appears heterogeneous with irregular hypo-enhancement areas (known as congestive or "nutmeg" liver). This attenuation becomes more homogeneous in later phases. If not resolved, it may progress to fibrosis and cirrhosis.
- It is usually associated with cardiomegaly, pleural effusion and ascites, as well as pericardial thickening/ effusion.
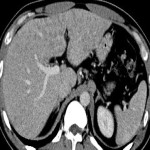
3. METABOLIC DISEASE
Non-alcoholic fatty liver disease (NAFLD) is becoming more frequent in society due to sedentary habits and poor diet.
MRI is the most accurate technique for detecting and quantifying steatosis, using in-phase and out-of-phase sequences.
Typical radiological findings:
- Liver parenchyma decreased attenuation (Liver attenuation <40 HU in non-contrast CT; or difference of 10 - 25 HU less compared to the spleen in studies with or without intravenous contrast).
- Signal drop in out-of-phase MRI sequence.
- Focal involvement when mild (typical adjacent to the falciform ligament, periportal or perivesicular regions) or heterogeneous/diffuse when extended. Distribution can be also lobar or segmental with well-defined and geographic margins.
- No mass effect on adjacent vascular or biliary structures (useful sign when nodular pattern).
4. STORAGE LIVER DISEASE
4.1 Iron overload
Primary (hemochromatosis with deposit in hepatocytes) or secondary (hemosiderosis due to deposit in Kupffer cells in the context of erythropoiesis disorders or repeated transfusions). In most cases, the iron deposit distribution may help to distinguish between primary and secondary disease.
- Primary heamochromatosis typically affects the liver, with spleen sparing; When more significant iron overload, there may be pancreas or even heart and skin involvement.
- Secondary haemosiderosis typically affects the reticuloendothelial system (RES): liver, bone, and spleen.
Radiological findings:
- MRI is the most sensitive technique. Due to iron´s paramagnetic effect, there is a shortening of T2 relaxation time which results in signal decrease (proportional to the degree of iron deposition) and increased signal of liver parenchyma in out-of-phase sequence (unlike steatosis).
- Increased attenuation of organs involved in non-contrast CT, but difficult to diagnose after contrast administration.
When iron overload is very significant and maintained over time, it may increase the risk of cirrhosis and HCC.
4.2 Wilson disease
Copper accumulation in periportal space and hepatic sinusoids that lead to an inflammatory state with progressive evolution to fibrosis.
- Increased attenuation in non-contrast CT (due to copper´s high atomic number), but may show normal attenuation (typically associated with steatosis).
- Hepatomegaly. In advanced cases, cirrhosis.
- MRI: multiple hyperintense siderotic nodules in T1-weighted sequences and hypointense in T2-weighted sequences. Copper does not show in MRI (non-ferromagnetic element).
4.3 Amyloidosis
Hepatomegaly with focal low attenuated areas corresponding to parenchyma with amyloid deposition. Pronounced signal drop in pT2 sequences is also characteristic.
5. TUMORAL
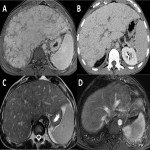
5.1 Diffuse metastatic disease
This affectation can be manifested in many different tumours, being melanoma, neuroendocrine, pancreatic adenocarcinoma, breast and colon cancer the most frequent ones.
- Heterogeneous parenchyma, vascular and architectural distortion, and shape abnormalities.
- In some cases (typically metastases from breast cancer under treatment), this situation may progress to pseudocirrhosis.
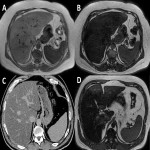
5.2 Pseudocirrhosis
A term used to refer to radiological changes similar to cirrhosis in the absence of such changes on pathologic examination. Mostly described in metastatic breast cancer, but it can also appear in other tumour types. Being the case of this phenomenon unclear, it is postulated that these morphological alterations would be secondary to the metastatic infiltration of healthy tissue (desmoplastic response to an infiltrative tumour) as well as due to toxicity or response to chemotherapy (can produce hepatic capsular retraction).
It can help to distinguish it from actual cirrhosis its short time of evolution (weeks and months after the onset of the QT, with an initial study with no hepatopathy signs) and with very fast progression.
6. INFLAMMATORY-INFECTIOUS PROCESS
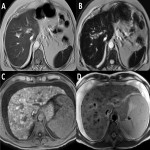
6.1 Fungal infection: most frequent in immunocompromised patients, haematological diseases.
They are characterized by the formation of micro abscesses manifested as multiple rounded lesions with central or peripheral enhancement, hypo-intense in pT1 sequence with intense enhancement and markedly hyperintense in pT2 (may have changes in signal with treatment and evolution).
6.2 Granulomatous disease:
- Sarcoidosis: It is characterized by non-caseating granulomas surrounded by fibrosis in the periportal region. Its manifestations are hepatosplenomegaly with innumerable small hypodense nodules in CT or hypo-intense in pT2 and with enhancement in MRI.
- TB: granulomatous hepatitis may occur secondary to hematogenous dissemination from a primary pulmonary focus. The most typical form of presentation is miliary, which makes it necessary to establish the differential diagnosis with multiple pyogenic or fungal abscesses.
- Histoplasmosis: also secondary to the dissemination of a pulmonary focus, it presents with hepatosplenomegaly with hypodense adenopathy and very similar pattern to fungal involvement.
- b) PATTERNS
Once the different possible aetiologies have been analysed, another way of classifying diffuse liver involvement would be based on its presentation patterns (using MRI as a reference).
- Diffuse homogeneous distribution.
- Segmental distribution.
- Nodular distribution.
- Perivascular distribution.
- Diffuse homogeneous distribution: represents involvement of hepatocytes and reticuloendothelial system. Increased or decreased signal in pT1 and pT2 sequences.It includes entities such as hemochromatosis, steatohepatitis and other metabolic disorders.
- Segmental distribution: present in focal steatosis, subacute hepatitis or ischemia.
- Nodular distribution: such as cirrhosis, steatosis, infections, Wilson's disease or sarcoidosis.Cirrhosis starts with regenerative changes that appear as diffuse hypo-intense micronodular pattern both in pT2 and in gradient echo sequences due to hemosiderin deposition. These nodules have a variable T1 signal: isointense, hypo- or hyperintense depending on their lipid, protein or iron content. It is important to remember that these are nodules with risk of dysplastic degeneration or HCC.
- Perivascular distribution: congestive hepatopathy, schistosomiasis and steatosis (less commonly). Inhomogeneous mottled reticular or mosaic pattern of the parenchyma and perivascular (portal or hepatic veins) low attenuation on CT; and high intensity on T2 sequence.