Keywords:
Artificial Intelligence, Neuroradiology brain, CT, CAD, Computer Applications-Detection, diagnosis, Ischaemia / Infarction
Authors:
A. Ayobi, P. Chang, D. Chow, C. Filippi, S. Quenet, M. Tassy, Y. Chaibi
DOI:
10.26044/ecr2023/C-19206
Results
For the standalone performance, a total of 2780 ASPECTS regions (139 patients x 20 ASPECTS regions per patient) were analyzed. There were 380 (13.7%) regions with EIC and 2400 (86.3%) negative regions, according to the GT. The mean ± SD of patients’ age was 68.9 ± 13.7 y/o. For the MRMC study, the 40 NCCTs were randomly selected from the initial 139 scans. Both datasets contained a sufficient number of cases from important cohorts in terms of imaging acquisitions (i.e. CT vendors, number of detector rows and slice thickness), patients’ age and ASPECTS infarcted regions.
Standalone Performance
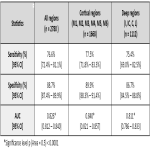
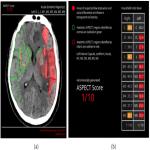
The comparison of CINA-ASPECTS with the GT yielded a region-based sensitivity of 76.6% [95% CI: 72.4% – 81.1%] and a specificity of 88.7% [95% CI: 87.4% – 89.9%]. The ROC AUC was 0.826 (p<0.0001). All the results are displayed in Table 1. False positives were often found in the internal capsule, which is known to be inconsistently scored among expert raters and has been the subject of low agreement in other studies [13]. Most of the false negatives were found in M4 due to the presence of reconstruction artifacts, often seen in this area. In previous studies, similar devices showed sensitivities ranging from 43.6% to 46.5% and specificities from 90.7% to 94.1% [14, 15]. Thus, our software shows promise with a more balanced operating point resulting in a higher sensitivity and a similar specificity. An example of CINA-ASPECTS’ results is shown in Figure 1.
Multi-Reader-Multi-Case Study
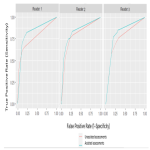
In the MRMC evaluation, the use of CINA-ASPECTS increased the average ROC AUC of all readers to 0.824, compared to a baseline average ROC AUC of 0.776 without software assistance (Table 2). This difference was statistically significant (p<0.05). All readers increased their ROC AUC when assisted by the software. Indeed, radiologists’ assessments were more accurate when using the device, compared to the use of standard NCCT images alone. The ROC curves of each reader are displayed in Figure 2. In addition, the overall standard error was smaller for the aided readings, implying that the readers’ variability decreased with the software assistance.

![Table 2: ROC AUC results for all readers according to the Obuchowski-Rockette-DBM-MRMC methodology [12].](https://epos.myesr.org/posterimage/esr/ecr2023/162514/media/932292?maxheight=150&maxwidth=150)