Background
Dementia is one of the greatest health and social care challenges of our time1. Approximately 50 million people worldwide live with dementia, and this number is projected to rise to 152 million by 20502. Between 25% and 40% of older people admitted to hospitals are diagnosed with dementia, therefore healthcare professionals must be prepared to meet the needs of this growing population3.
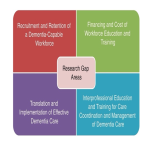
International policy documents support the need to develop interprofessional education (IPE) to enhance and support collaborative dementia care in the community. Education and training have been recommended for all healthcare professionals working in dementia care2. In 2017 a United States National Research Summit on Dementia Care in association with the National Institutes of Health created workgroups to address dementia care and develop recommendations4. Areas of critical workforce gaps have been identified and a key recommendation is the recruitment and retention of a dementia-capable workforce which requires dementia education and training needs to be met (See Fig 1).
It is essential that healthcare students can learn from, with and about each other’s role in dementia care, highlighting the need for interprofessional education to support collaborative dementia care5. Exposing students to interprofessional learning encourages collaborative practice in the workplace including responsibility, accountability, coordination, communication, cooperation, assertiveness, autonomy, mutual trust and respect.
However, the diversity of knowledge, skills, abilities, and qualities required to be a competent healthcare professional in dementia care highlights both the complexity and importance of education in this area. To design dementia educational programmes for healthcare students, it is important to analyse the curricular components of effective educational interventions from across the health-professionals spectrum. A systematic review of the key features of effective dementia training for the health and social care workforce found that active participation, experiential learning, and training that is applicable to the participants’ clinical role were features that enhanced learning6.
Methods
This interprofessional interactive workshop was developed as an educational initiative to expand on a previous endeavour whereby three disciplines were brought together with positive outcomes. In July 2022, a steering group was formed that included representatives from each of the 11 disciplines within the College of Medicine and Health at University College Cork. Healthcare students in the final two years of their programmes in diagnostic radiography, physiotherapy, radiation therapy, medicine, pharmacy, occupational therapy, nursing, audiology, speech & language therapy, paramedics, and dental hygienists were represented. The workshop's curriculum was guided by a literature review that evaluated what constitutes effective dementia education and training for the wider healthcare team. One of the recommendations from previous studies included the importance of having a patient or a patient advocate delivering aspects of the teaching as well as the benefits of a multimodal approach7 which was incorporated into this workshop. The steering group was also guided by previous feedback from students who had participated in other IPE dementia workshops in 2020 and 2021.
A dementia case study was created with input from each of the 11 included disciplines. A medical expert in dementia supervised the development of the case study. The case study covered the entire patient journey, from diagnosis to advanced illness. The case study's key learning objectives were closely aligned with the students' identified learning needs. The format of the 4-hour workshop is shown in Fig. 2.
Ethical approval was obtained and all students in attendance at the workshop were offered the opportunity to partake in completing the pre and post-questionnaire. This participation was voluntary. Statistical analyses of paired pre and post-workshop data (n=102) was carried out using IBM SPSS 28.0 using descriptive and inferential statistics.