Our four patients presented with selective pain and tenderness with MRI alterations.
One of them complaint of bilateral pain with bilateral afectation by MRI.
We have considered the patients that presented a signal alteration on the pretibial region.
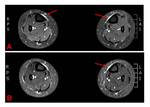
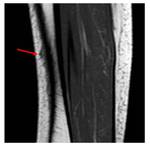
T2W-FSE with fat supression and STIR images showed a hyperintensity on the anteromedial surface of the tibia,
affecting the soft tissue adjacent to periosteum,
which means periosteal edema (fig 1).
All of them affected at middle region of the tibia.
In general,
T1W imaging was able to demonstrate the presence of periosteal edema (fig 2 and 3).
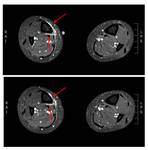
One of the patients presented another affected tibial region (posterior),
which is less common (fig 4 and 5).
Only one patient presented with bone marrow edema (mid-diaphysis of the tibia) as an area of high signal intensity on T2W,
and low signal intensity on T1W (fig 6 and 7),
but on STIR images the bone marrow edema was demonstrated with more confidence (fig 8).
Another one presented with unilateral pain but bilateral findings suggesting tibial stress injury.
Some classifications,
as the Fredericson´s,
has been developed based on the presence of periosteal edema,
bone marrow edema and intracortical signal alteration.
The reason for the classification may lead to asses the severity of stress injuries.
No one of our four patients presented cortical abnormalities,
which are common findings in bone stress injuries.
Sometimes the stress-related cortical abnormalities are appreciable on both T2W and STIR images.
The presentation may be like a round cavitation of high signal intensity or striation showing a hyperintense line extending only through a part of the cortical thickness.
Also it is common to see several parallel hyperintense lines affecting the bone cortical.
Irregularity of subperiosteal bone is a less frequent finding.
T1W FSE images have lesser values in detecting these type of lesions affecting the bone cortical.
Also the radiologist should know that sometimes,
the periosteal edema may be seen as a non-specific soft-tissue mass,
not shown in our patients.
The MRI can sometimes reveal a signal alteration on a non-symptomatic patient,
this is less common but can occur.
It has not been well stablished whether stress reactions detected on MRI are always related to clinical symptoms.
This could be because imaging findings could precede symptoms.
Also the cortical abnormalities may not cause always a source of pain and have been described in asymptomatic runners,
and in symptomatics.
The radiologist always have to exclude different causes of lower leg pain like muscular strain,
myositis,
tendinopathy,
chronic compartment syndrome or neural entrapment syndrome,
which may occur alone or associated (very unlikely) to bone stress.
The specialist will carefully evaluate the different structures of the lower leg afore mentioned.