Plain films are useful in initial workup to rule out occult fractures or stress fractures of the elbow ( Table 1 ,
Table 2 ,
Table 3 ).
Indirect signs of tendinosis are bone spur formation or soft tissue calcifications at the insertion of the affected tendon.
Plain films have limited role in early disease.
The same indirect signs can be seen on CT scan,
but CT is not preferred as the preferred imaging technique because of radiation restraints.
Ultrasound is the first line examination in the evaluation of the different elbow compartments.
The probe is placed in a longitudinal and axial plane on the axis of the tendons.
Tendon thickening,
hypoechogenicity,
hyperemia,
calcifications and (partial) tears are seen.
To evaluate hyperemia on echo-Doppler imaging,
compression with the probe should be avoided not to compromise the blood flow.
Hyperemia represents an angiofibroblastic reaction. Elastography is a more recent imaging technique within the ultrasonographic evaluation of soft tissues.
It measures the stiffness of tissues,
representing it on a color map.
Healthy tendons are hard and have low compressibility,
whereas in tendinopathy tendons become softer and have high compressibility.
MRI is a second line examination in the evaluation of elbow pain.
It is excellent to show associated pathology and to rule out other causes of elbow pain than tendon pathologies ( Table 1 ,
Table 2 ,
Table 3 ).
MRI is also helpful in pre-operative planning.
Normal tendons and ligaments are of uniform low signal intensity (SI) on all imaging sequences.
Tendon thickening,
signal intensity changes of the tendon or underlying bone marrow and tears of the tendon and/or adjacent ligaments are seen in pathologic conditions.
Slice thickness of 3 mm and a high resolution coil are recommended.
The preferred field of view is 10-14 cm.
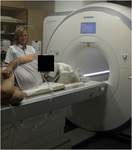
The patient is placed in the gantry preferably in a “superman”-position with the elbow in extension and supination ( Fig. 7 ).
T2-WI and proton density-weighted images with fat saturation are very useful to evaluate fluid.
T1-WI are used for a structural evaluation.
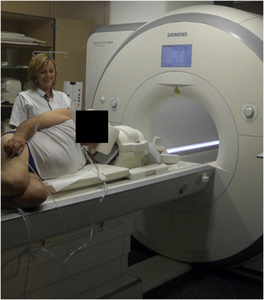
Fig. 7: Photograph of a patient in “superman”-position with the elbow in extension and supination for the best image quality.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
A) The lateral compartment
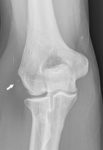
Plain films can show bone spur formation or soft tissue calcifications near the lateral epicondyle in advanced cases ( Fig. 8 ).
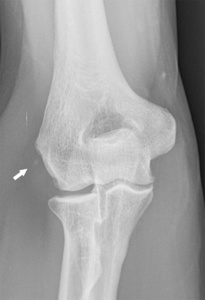
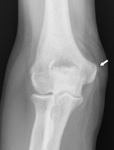
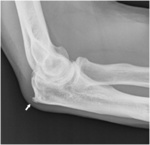
Fig. 8: Plain film of the elbow showing a soft tissue calcification (arrow) near the lateral epicondyle suggesting lateral epicondylitis.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
For sonographic evaluation of the extensor tendons,
the probe is placed in a longitudinal and axial plane of the tendons with the elbow in a flexed position.
The normal common extensor tendon is a continuous band of parallel fibers.
Imaging features of lateral epicondylitis are thickening of the extensor tendons (> 4 mm),
hypoechogenicity,
hyperemia,
calcifications and (partial) tears ( Fig. 9 , Fig. 10 , ).
On elastography,
soft consistency of the affected tendon is seen (Fig.
11).
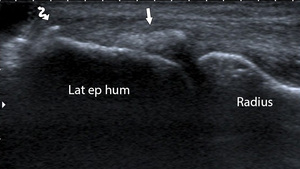
Fig. 9: Longitudinal ultrasound image of the common extensor tendon showing a large calcification (arrow) in the tendon and a smaller calcification more proximally (curved arrow): calcifying tendinopathy.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
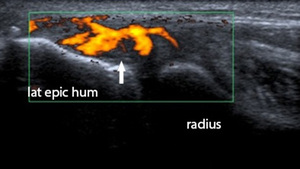
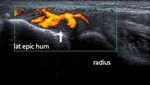
Fig. 10: Longitudinal ultrasound image of the common extensor tendon showing increased Doppler flow (arrow) in the tendon: hyperemia. This hyperemia is caused by an angiofibroblastic reaction, the repairative response to the (micro-)tearing with the formation of scar tissue.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
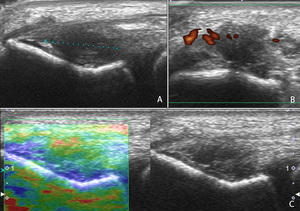
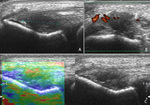
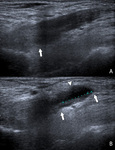
Fig. 11: Longitudinal (A,C) and transversal (B) ultrasound image of the extensor tendons showing a hypoechogenic zone (A,B,C) within the extensor tendons: tendinosis. There is an increased Doppler signal (B): hyperemia. The zone of tendinosis has on elastography (C) an increased compressibility of the tendon. The blue spots on the color map represent hard tissue with low compressibility and the red spots represent soft tissue with high compressibility.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
On MRI,
the tendons and ligaments ( Fig. 12 ) of the lateral compartment are best evaluated on axial and coronal images.
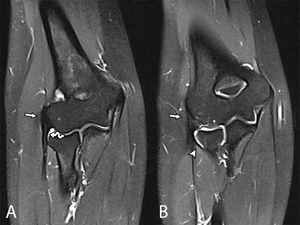
Fig. 12: Coronal fat saturated (FS) T2-WI of the normal elbow. A is 2 slices anterior of B. The common extensor tendon (arrow) inserts on the lateral epicondyle and is in normal circumstances hypointense on all imaging sequences. The radial collateral ligament is deep of the common extensor tendon situated (curved arrow). The lateral ulnar collateral ligament is located posteriorly to the radial head.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
Thickening of the common extensor tendon,
SI-changes,
tears and associated RCL tears can be efficiently evaluated on MRI ( Fig. 13 ,
Fig. 14 ,
Fig. 15 ,
Fig. 16 ).
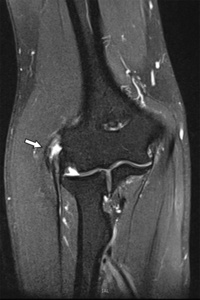
Fig. 13: Coronal T2-WI with FS showing a thickened common extensor tendon with a hyperintense zone in the proximal tendon (arrow): partial tear. There are no associated lesions.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
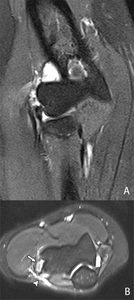
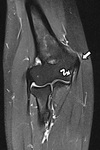
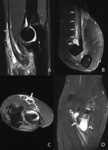
Fig. 14: Coronal (A) T2-WI with FS and axial (B) dixon T2-WI with FS showing a severe tear of the conjoint extensor tendon (arrow) with perilesional edema (arrowhead). There is an associated radial collateral ligament rupture at its insertion on the lateral epicondyle, resulting in posterolateral rotatory instability of the elbow (curved arrow).
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
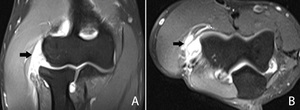
Fig. 15: Coronal (A) and axial (B) T2-WI with FS showing a full thickness tear of the conjoint tendon with retraction and involvement of the radial collateral ligament.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
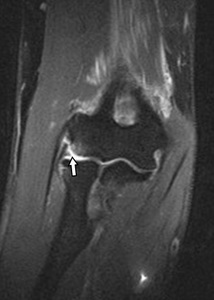
Fig. 16: Coronal pd T2-WI with FS showing a post-traumatic tear of the insertion of the radial collateral ligament at the lateral epicondyle. Avulsion type edema is seen in the lateral epicondyle.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
Osteochondritis dissecans and Panner's disease are possible differential diagnoses of lateral epicondylitis ( Fig. 17 ).
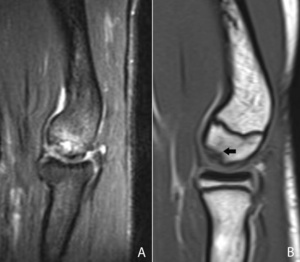
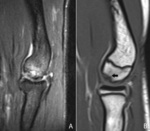
Fig. 17: Sagittal T2-WI with FS of a patient with an osteochondritis dissecans (A) and a sagittal T1-WI of a patient with Panner's disease (B). In Panner's disease, there is also involvement of the growth plate and it is seen in children between the age of 7-12 years old. Osteochondritis dissecans is usually seen in young adolescents between the age of 12-15 years old.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
MRI manifestations of radial tunnel syndrome are denervation edema and atrophy within the muscles innervated by the posterior interosseous nerve ( Fig. 18 ).
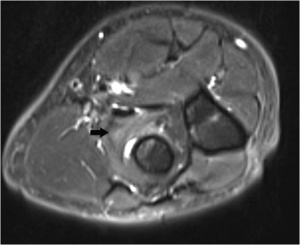
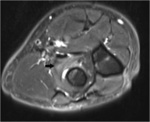
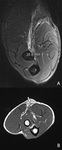
Fig. 18: Axial T2-WI with FS of a patient with a radial tunnel syndrome showing edema in the supinator muscle, a frequent location of entrapment of the posterior interosseous nerve, a branch of the radial nerve.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
B) The medial compartment
Plain films can show bone spur formation or soft tissue calcifications near the medial epicondyle in advanced tendinosis ( Fig. 19 ).
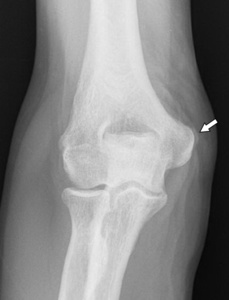
Fig. 19: Plain film of the elbow showing a soft tissue calcification (arrow) near the medial epicondyle suggesting medial epicondylitis.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
For sonographic evaluation of the extensor tendons,
the probe is placed in a longitudinal and axial plane of the tendons with the elbow in an extended position.
Looking at both planes is necessary to exactly locate the lesion ( Fig. 20 ).
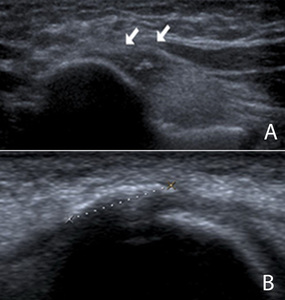
Fig. 20: Ultrasound in a longitudinal (A) and transversal (B) plane of the flexor-pronator mass showing a calcification surrounded by hypoechogenicity: medial epicondylitis. Both planes are necessary to be able to exactly locate the lesion in the anterior aspect of the tendon.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
As in the evaluation of the lateral compartment,
tendons and ligaments of the medial compartment are best evaluated on coronal and axial planes on MRI ( Fig. 21 ).
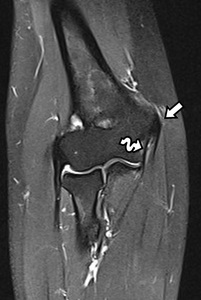
Fig. 21: Coronal T2-WI with FS of the normal elbow. The flexor-pronator mass (arrow) inserts on the medial epicondyle and is in normal circumstances hypointense on all imaging sequences. The medial collateral ligament is deep of the flexor-pronator mass situated (curved arrow).
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
Thickening,
SI-changes,
tears of the flexor-pronator mass and associated MCL tears can be efficiently evaluated on MRI ( Fig. 22 ,
Fig. 23 ,
Fig. 24 ).
Bone marrow edema is more frequently seen in medial epicondylitis than in lateral epicondylitis ( Fig. 22 ).
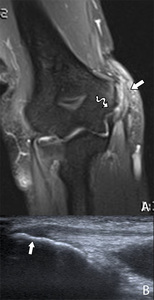
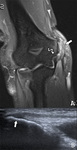
Fig. 22: Coronal pd T2-WI with FS (A) with in the same patient a corresponding ultrasound image in the longitudinal plane at the flexor-pronator mass (B). The MRI shows thickening and hyperintensity (arrow) at the tendon of the flexor-pronator mass. Adjacent bone marrow edema is seen in the medial epicondyle. There is also a rupture of the medial collateral ligament at the insertion on the medial epicondyle (curved arrow). The ultrasound image shows the same tendon thickening with accompanying hypoechogenicity: medial epicondylitis.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
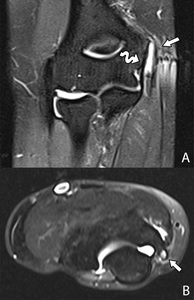
Fig. 23: Coronal (A) and axial (B) pd T2-WI with FS showing a hypointense zone in the tendon of the flexor-pronator mass. Some fibers are still attached to the medial epicondyle (arrow): partial tear. The MCL has a normal insertion on the medial epicondyle (curved arrow).
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
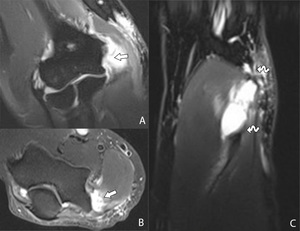
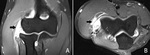
Fig. 24: Coronal (A), axial (B) and sagittal (C) T2-WI showing a complete tear of the flexor-pronator mass (arrow). The degree of retraction should be evaluated on sagittal images (distance between the curved arrows).
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
Following a valgus trauma in children,
avulsion of the medial epicondyle is more frequent than tearing of the flexor-pronator mass ( Fig. 25 )
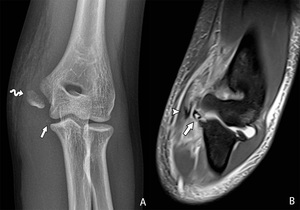
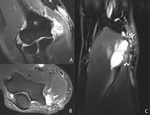
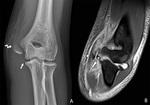
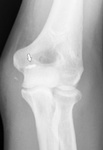
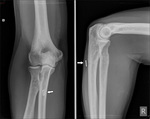
Fig. 25: Avulsion fracture of the medial epicondyle after a valgus trauma in a 15-year-old patient with a preexisting Little League elbow. Plain films (A) show the avulsion fragment (arrow) and a traumatic separation of the medial epicondyle apophysis (curved arrow) with accompanying soft tissue swelling. A subsequent MRI of the elbow reveals an avulsion fragment (arrow) on the pd T2-WI with FS (B). The tendons of the flexor-pronator mass do not seem to be ruptured (arrowhead).
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
Ulnar neuropathy should always be excluded in medial epicondylitis ( Fig. 26 ).
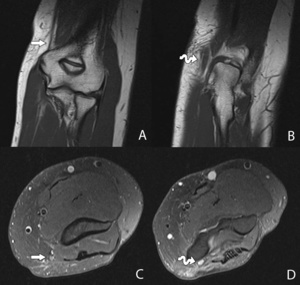
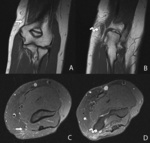
Fig. 26: Coronal T1-WI of the elbow showing the ulnar nerve in the cubital tunnel (B) and more proximally (A). Corresponding T2-WI in the axial plane at the level of the cubital tunnel (D) and more proximally (C). The ulnar nerve in the cubital fossa is thickened and hyperintense on the T2-WI compared to the images more proximally: ulnar neuropathy.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
On plain films,
anchor material can be seen after tendon or ligament reinsertion ( Fig. 27 ).
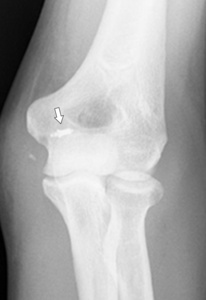
Fig. 27: Plain film of the elbow showing a Mitek-anchor (arrow) after repair of the MCL and the flexor-pronator mass.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
C) The anterior compartment
Plain films have usually no added value caused by superposition.
CT-scan can be useful to reveal bone spur formation in the distal biceps tendon ( Fig. 28 ).
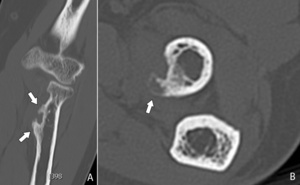
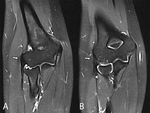
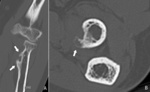
Fig. 28: Coronal (A) and axial (B) CT-image in bone window of the elbow revealing a bone spur formation at the radial tuberosity (arrows). This can be misinterpreted as a tumor. The key to the diagnosis is the location at the insertion of the biceps tendon and the absence of a soft tissue mass.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
Ultrasound of the distal biceps tendon is performed with the elbow in extension.
Evaluation of this tendon is difficult in unexperienced hands because of the deep insertion of the tendon on the radial tuberosity.
Ultrasound can be used for evaluation of tendinosis and (partial) tearing of the distal biceps tendon ( Fig. 29 ).
The insertion site at the radial tuberosity can also be seen from posteriorly with the arm in pronation and flexion.
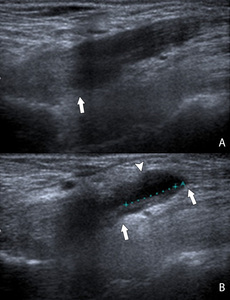
Fig. 29: Longitudinal ultrasound image of the distal biceps tendon revealing a partial tear. The fibers of the tendon are interrupted (arrow) and a soft tissue collection is seen (arrowhead).
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
The FABS-position (flexion,
abduction and supination) ( Fig. 30 ) is used for assessment of the distal biceps tendon on MRI.
In this position,
the tendon loses its oblique course seen in the standard imaging position.
The tendon is now straight in a coronal and sagittal plane,
resulting in an easier interpretation of the distal biceps tendon ( Fig. 31 ,
Fig. 32 ).
A full thickness tear of the distal biceps tendon with more than 8 cm of retraction indicates an accompanying tear of the lacertus fibrosis.

Fig. 30: The FABS position is used to obtain a straight distal biceps tendon in a sagittal and coronal plane on MRI. The elbow is flexed with the arm in abduction and the forearm in supination.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
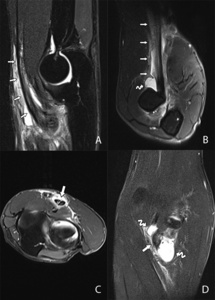
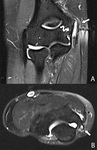
Fig. 31: Sagittal (A), axial (C) and coronal (D) T2-WI with FS and T2-WI with FS in FABS position (B). The distal tendon of the biceps muscle is hyperintense (arrows) on the sagittal image and on the image in FABS position with fluid signal intensity around the tendon (arrows): tendinosis of the distal biceps tendon with peritendinosis. Notice the better visualization of the distal portion of the biceps tendon in FABS position compared to the standard position in extension. On the axial images, a hyperintense longitudinal cleft (arrow) can be seen: partial longitudinal tear. Along the biceps tendon, a hyperintense, sharply delineated structure is seen (curved arrows): bicipitoradial bursitis.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
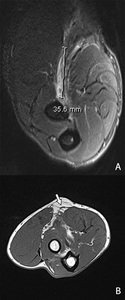
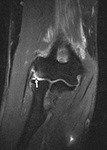
Fig. 32: Dixon T2-WI with FS in FABS position at the level of the radial tuberosity (A) and an axial T1-WI at the level of the lacertus fibrosis (B). There is a full thickness tear at the radial tuberosity seen with retraction of 3,5 cm. The lacertus fibrosis is still intact (arrow), causing the biceps tendon not to retract any further. Retraction of more than 8 cm indicates rupture of the lacertus fibrosis.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
Placement of an anchor at the dorsal aspect of the proximal radius or ulna indicates distal biceps tendon repair ( Fig. 33 ).
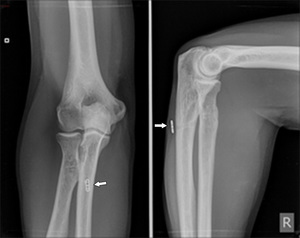
Fig. 33: Plain films of the elbow showing anchor placement (arrow) after distal biceps tendon repair.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
D) The posterior compartment
Plain films can show bone spur formation or soft tissue calcifications near the olecranon in advanced cases ( Fig. 34 ).
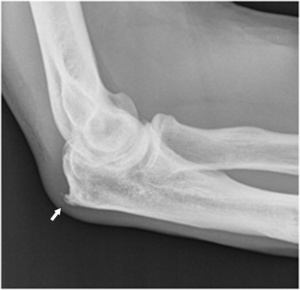
Fig. 34: Plain films showing spur formation (arrow) at the olecranon.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
Ultrasound of the distal triceps tendon is performed with the elbow in flexion ( Fig. 35 ).
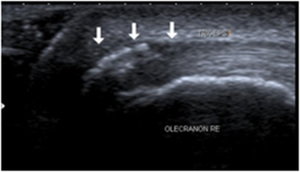
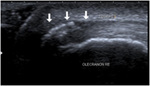
Fig. 35: Ultrasound of the distal triceps tendon showing thickening of the tendon, calcifications and adjacent hypoechogenicity in the tendon (arrows): calcifying tendinosis of the distal triceps tendon.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
MRI shows the same imaging features as in the other compartments.
The triceps tendon is best evaluated in the sagittal and axial plane ( Fig. 36 ).
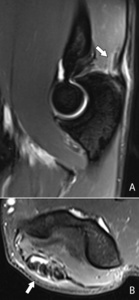
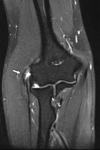
Fig. 36: Sagittal (A) and axial (B) T2-WI with FS showing hyperintensity at the distal portion of the triceps tendon (arrow) and peritendinous hyperintensity: tendinosis of the distal triceps tendon with peritendinosis.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
After trauma or repetitive stress,
avulsion fracture of the olecranon can occur ( Fig. 37 ).
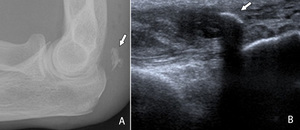
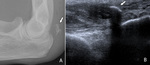
Fig. 37: Plain films (A) of the elbow and ultrasound (B) of the distal triceps tendon showing an avulsion fragment of the olecranon (arrow).
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium
Olecranon bursitis is usually a straightforward diagnosis on ultrasound due to its location at the olecranon and in the subcutaneous soft tissue ( Fig. 38 ).
It shows a fluid collection with usually hyperaemia.
There may be some debris in the collection.
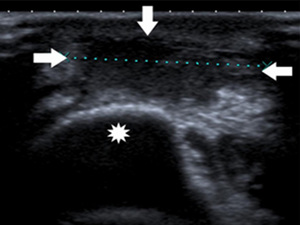
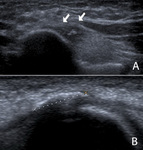
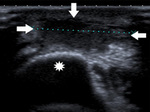
Fig. 38: Ultrasound of the posterior elbow showing a fluid collection (arrows) in the subcutaneous soft tissue at the olecranon (star): olecranon bursitis.
References: Department of Radiology, AZ Sint-Maarten, Mechelen-Duffel, Belgium