I ODONTOGENIC LESIONS
Case 1: Maxillary Sinus Keratocystic Odontogenic Tumour
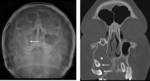
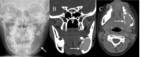
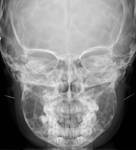
13-year old boy with pain and lump over the right maxillary region (Figure 1).
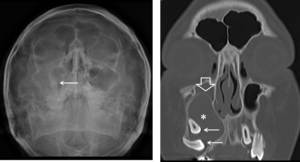
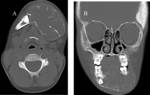
Fig. 1: Plain radiograph of the face shows opacification of the right maxillary sinus with the presence of a tooth (arrow).
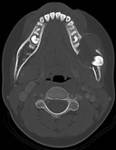
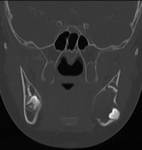
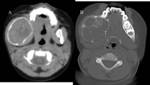
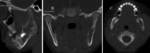
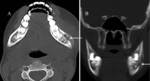
Coronal CT image shows the presence of a cyst in the right maxillary sinus (*). The upper border of the cyst within the right maxillary sinus can be seen (open arrow). 2 teeth can be seen projecting into the cystic lesion (arrows).
This lesion is a common cyst of the mandible. Some cases occur in the maxillary sinus and may be mistaken for mucous retention cysts. Patients may present with a painful mass. Lesions may be single or multiple and when multiple are often associated with Gorlin's syndrome.
Imaging features
The lesion appears as a well-defined, unilocular,
well-corticated radiolucent lesion that have a tendency to grow in an antero-posterior direction. Cortical expansion may occur. Tooth displacement,
root resorption and extrusion may be seen in some more aggressive cases. Differentiation with other odontogenic cysts may be difficult on imaging.
Treatment
The treatment of choice is complete removal of the entire cyst but recurrence rates are high.
Case 2: Dentigerous Cyst
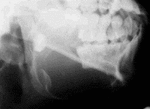
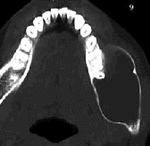
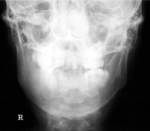
11-year-old boy with swelling of the left side of the jaw of several months duration. Plain radiograph (Figure 2) and Axial CT image (Figure 3) show a cystic lesion causing bony expansion in the body of the mandible.
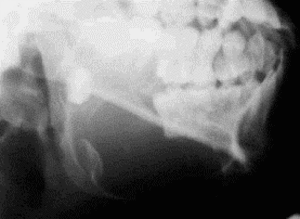
Fig. 2: Lateral plain radiograph of the mandible shows a large cystic lesion causing bony expansion associated with the crown of a tooth which appears dysplastic
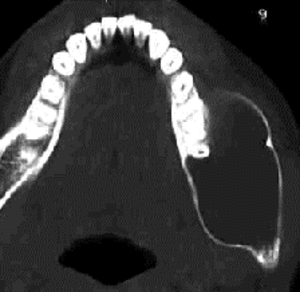
Fig. 3: Axial CT image shows the lesion to be cystic and causing bony expansion with cortical thinning.
This is a common developmental cyst. It forms around the crown of an unerupted tooth due to fluid accumulating between the follicular epithelium and the crown of a developing or unerupted tooth4. Identifying the crown of an unerupted tooth is very common.
Imaging features
The lesion appears as a well-defined radiolucent lesion associated with an unerupted tooth.
Treatment
The treatment of choice is complete removal of the entire cyst and the affected tooth.
Case 3: Ameloblastoma
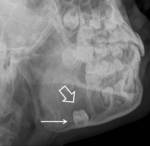
9-year old boy with pain and left mandibular swelling. Plain radiograph and CT show the presence of a radiolucent lesion seen in the left mandible associated with an unerupted tooth (Figures 4-6).
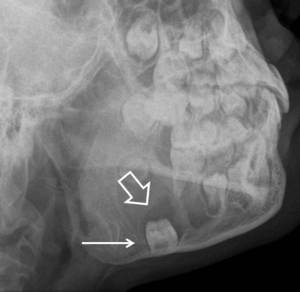
Fig. 4: Plain oblique radiograph of the mandible shows the presence of a well-defined radiolucent lesion (open arrow) in the body of the mandible associated with an unerupted tooth (arrow).
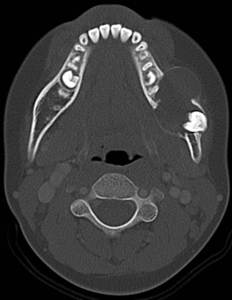
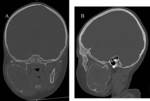
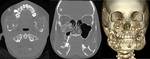
Fig. 5: Axial CT image shows similar findings to the plain radiograph
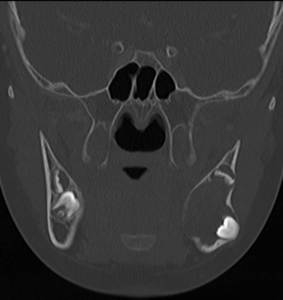
Fig. 6: Coronal CT image shows similar findings to the plain radiograph
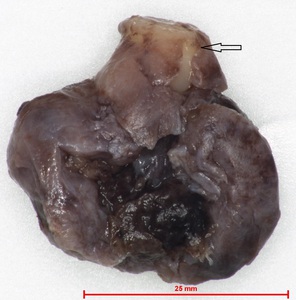
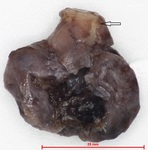
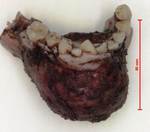
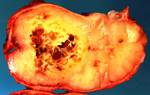
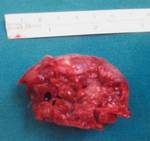
Fig. 7: Gross specimen of the resected lesion shows a collapsed cyst measuring 2.5 x 2 x 1 cm, enclosing a tooth within (arrow).
Image courtesy of Dr Derrick Lian, Department of Pathology and Laboratory Medicine, KK Hospital.
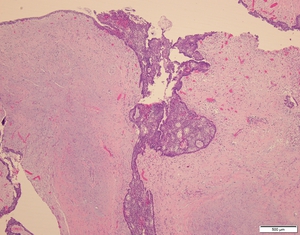
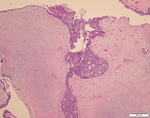
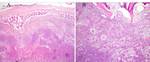
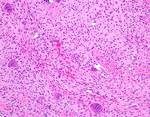
Fig. 8: The cyst wall is lined by basaloid epithelium with a plexiform and anastomosing pattern of extension deep into the fibrous wall. The lining epithelium varies in thickness, and in many areas forms polypoid projections into the cyst lumen.
Image courtesy of Dr Derrick Lian, Department of Pathology and Laboratory Medicine, KK Hospital.
These are invasive neoplasms that may occasionally metastasize. Less than 1% are malignant. They arise from the enamel-forming cells of the odontogenic epithelium that have failed to regress during embryonic development. 3 types have been described: Intra-osseus (solid or cystic),
well-circumbscribed unilocular,
and peripheral (extraosseus).
Imaging features
This lesion has variable radiographic appearances appearing as either unilocular or multilocular cystic lesions. Slight marginal sclerosis,
scalloped margins,
cortical expansion,
loss of lamina dura,
root resorption and tooth displacement may be present. They may appear identical to the Dentigerous cysts but erosion of the roots of the adjacent teeth are unique to ameloblastomas2,5.
Treatment
The treatment of choice is complete removal of the entire lesion with at least 1.5cm of surrounding normal bone to prevent recurrence.
Case 4: Odontogenic Myxoma
9-year old boy with painless mass over the left side of the mandible.
Plain radiograph shows a lucent lesion with aggressive margins in the body of the left side of the mandible. CT shows a lesion with an attenuation slightly higher than soft tissue in this region. MRI shows the lesion to be heterogenous in echotexture with heterogenous enhancement post contrast.
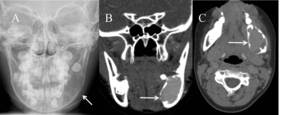
Fig. 9: (A)Plain radiograph shows a lucent lesion with cortical erosion in the body of the left side of the mandible (arrow). (B and C) Coronal and Axial CT images show the lesion to be slightly higher in attenuation when compared to surrounding soft tissue. Areas of cortical erosion and thinning can be seen indicating that the lesion is aggressive.
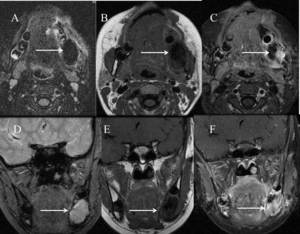
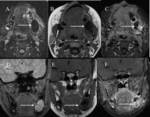
Fig. 10: (A) Axial T2, (B) Axial T1, (C) Axial T1 fat-saturated post contrast, (D) Coronal Gradient echo, (E) Coronal T1 and (F)Coronal T1 fat-saturated post-contrast images shows a lesion of heterogeneous signal intensity in the body of the left side of the mandible showing areas of enhancement post contrast.
Odontogenic myxomas are benign lesions that are locally aggressive without metastatic potential. They occur in the posterior portion of the mandible and usually present as painless masses. This tumour arises from embryonic connective tissue and histologically it consists mainly of spindle shaped cells and scattered collagen fibres distributed through a loose,
mucoid material6.
Imaging Features
Radiographically these lesions appear as lucent,
aggressive lesions with fine trabeculations resembling a 'soap-bubble' appearance. They are indistinguishable from Ameloblastomas.
Treatment
These lesions are usually resected with a generous portion of surrounding bone to prevent recurrence.
Case 5: Mixed Odontogenic Tumour
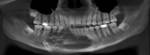
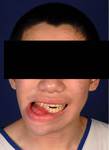
15-year-old boy with 6-month history of swelling of the right side of the jaw that was occasionally painful (Figure 11). Imaging shows the presence of a multiloculated expansile lesion just to the right of midline in the body of the mandible (Figures 12-14).
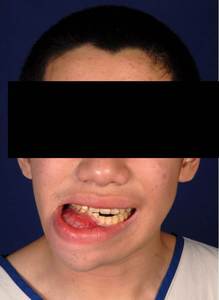
Fig. 11: Frontal photograph of the patient shows a swelling of the right side of the jaw.
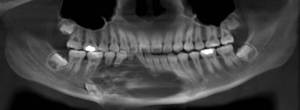
Fig. 12: Orthopantomogram of the mandible shows a multiloculated lucent lesion just to the right of midline causing surrounding erosion that involve the teeth.
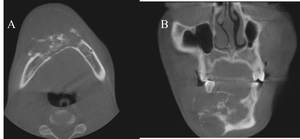
Fig. 13: (A) Axial and (B) Coronal CT images show a destructive, multiloculated lucent lesion in the right side of the body of the mandible.
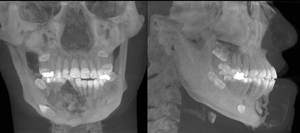
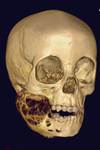
Fig. 14: 3D reconstructed image shows the expansile radiolucent lesion just to the right of midline in the body of the mandible with aggressive features distorting the teeth
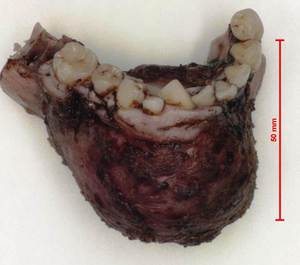
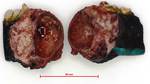
Fig. 15: Gross specimen of the resected portion of the mandible shows the lesion measuring about 6cm in size expanding the involved part of the mandible.
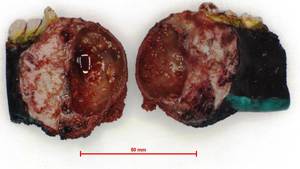
Fig. 16: Internal appearance of the lesion shows a cystic part and a solid posterior part.
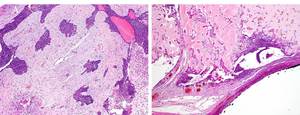
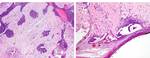
Fig. 17: (A) HE stain of the solid component show islands and nests of epithelial cells with peripheral palisading, within a fibrous stroma. (B) The cyst wall lining shows ameloblastomatous cells with ghost cells.
The final diagnosis is an Odontogenic tumour combining features of:
1. Calcifying cystic odontogenic tumour
2. Adenomatoid odontogenic tumour
3. Ameloblastoma fibrodentinoma
Odontogenic tumours may arise from the epithelial part of the tooth,
the ectomesenchymal part or both. This case illustrates a lesion that arises from all these components. (1) and (2) have epithelial origins and (3) has mixed origins.
Treatment
The patient underwent a radical en-bloc excision followed by reconstruction of the mandible with satisfactory result.
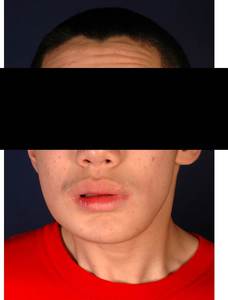
Fig. 18: Post-operation and reconstruction photograph shows satisfactory result.
II NON-ODONTOGENIC LESIONS: BONE-RELATED
Case 6: Ossifying Fibroma - Juvenile trabecular sub-type
A 2-year old boy presented with right jaw swelling that was gradually increasing in size over a period of 1 year. Plain radiographs were not available and the CT shows the presence of an expansile,
multiloculated,
radiolucent lesion in the right side of the mandible.
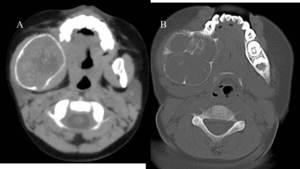
Fig. 19: (A) Axial CT image in soft tissue window and (B) bone window shows the presence of an expansile multiloculated lesion situated in the body of the right side of the mandible.
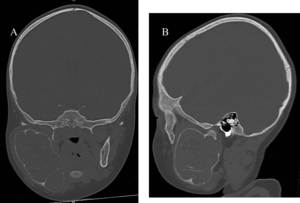
Fig. 20: (A) Coronal and (B) Sagittal CT images show the expansile, multiloculated within the right side of the mandible.
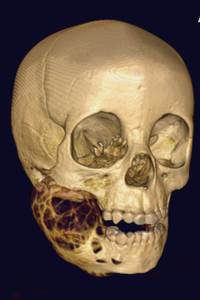
Fig. 21: 3D reconstructed CT image shows the multiloculated lesion with bubbly features in the right side of the mandible.
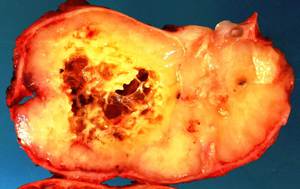
Fig. 22: Gross photograph of mandibular resection specimen showing a well-circumscribed pale yellow tumour with focal cystic degeneration
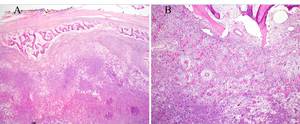
Fig. 23: (A)Photomicrograph: H&E-stained photomicrograph (magnification x20) showing thin rim of remnant mandibular cortical bone (top) and subjacent predominantly fibrous tumour with variable cellularity. (B) Photomicrograph: H&E-stained photomicrograph (magnification x100) showing fibrocellular tumour with osteoid and irregular lamellar bone formation. There is no merging of preexisting bony trabeculae (top) with lesional bone.
The ossifying fibroma is a primary non-odontogenic tumour that is a well-defined lesion composed of fibrocellular tissue and mineralized material of varying appearance7. The case being presented is the Juvenile Trabecular sub-type which consists of cell-rich fibrous tissue with bands of cellular osteoid together with slender trabeculae of plexiform bone lined by a dense rim of enlarged osteoblasts. Mitoses,
multinucleated giant cells,
pseudocystic degeneration and haemorrhages may be present.
Treatment
Complete excision of the lesion usually yields a permanent cure.
Case 7: Giant Cell Reparative Granuloma
7-year old boy with past history of left temporoparietal Ewing's sarcoma that was resected when he was 4.5 years old with cranioplasty done. Presented at 7-years old with a mass in the floor of the mouth measuring about 2cm in size and fixed. CT shows a multiloculated lesion in the left side of the body of the mandible. MRI shows the lesion to be low in signal intensity on T1-weighted imaging and isointense on T2-weighted imaging. The tumour enhanced post-contrast.
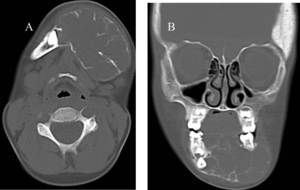
Fig. 24: (A)Axial and (B) Coronal CT images show the presence of a multiloculated cystic lesion in the left side of the body of the mandible.
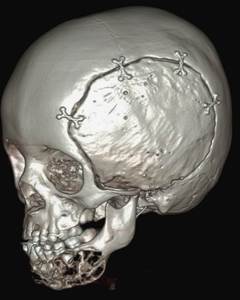
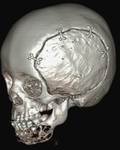
Fig. 25: 3D reconstructed CT images shows the multiloculated lesion in the left side of the body of the mandible. The previous cranioplasty on the left side of the skull vault can be seen.
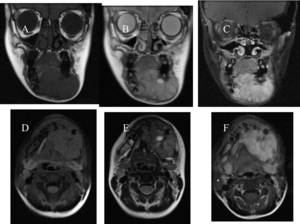
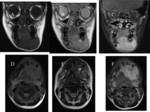
Fig. 26: (A) Coronal T1, (B)Coronal T2, (C)Coronal T1 post-contrast, (D)Axial T1 fat-saturated, (E) Axial T2, (F)Axial t1 post-contrast MRI images shows the lesion in the left side of the mandible to be low in signal intensity on T1-weighted imaging, intermediate in signal intensity on T2-weighted imaging and demonstrating contrast enhancement.
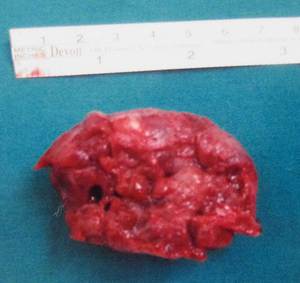
Fig. 27: The resected specimen is an irregular hard brown piece of tissue measuring 5.5 x 3.2 x 2.6 cm with a tooth on one surface, along with multiple irregular hard brown pieces of tissue with a few teeth on the other surface.
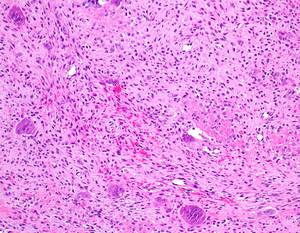
Fig. 28: H&E stained photomicrograph shows a section of bone with a central area characterised by diffuse clusters of osteoclastic-type giant cells within a fibroblastic, spindled cell and collagenous stroma. The stroma displays extensive haemorrhage and haemosiderin-laden macrophages. A prominent feature in much of the tumour is the presence of irregular spicules of bone with reactive osteoid formation and osteoblastic rimming. The squamous mucosa and submucosal stroma are unremarkable. The histological features and tumour site are compatible with giant cell reparative granuloma.
The giant cell reparative granuloma is usually seen in adults and children before the age of 30 years. It is believed to be a single lesion in a spectrum of altered vascular and reactive responses within bone. They present as localized jaw swellings and initially may appear radiographically as simple cystic lesions that eventually become multilocular. There is also evidence of expansion,
root resorption and erosion/remodelling of the cortex. Differential diagnosis include brown tumours of hyperparathyroidism. Laboratory tests should be able to distinguish the two entities.
Treatment
Complete removal is the treatment of choice but because these lesions are not encapsulated,
they may recur and brown tumour should be excluded.
Case 8: Cherubism
10-year old boy presented with 5-year history of bilateral cheek swelling. Plain radiograph and CT shows bilateral,
symmetrical,
multiloculated lucencies causing expansion of the mandible and maxilla bones.
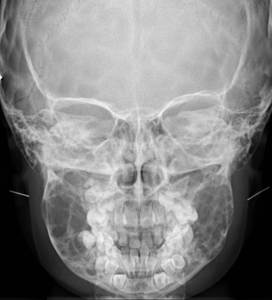
Fig. 29: Plain frontal radiograph shows the presence of bilateral, symmetrical, multiloculated lucent expanded regions in the mandible and maxilla diagnostic of cherubism.
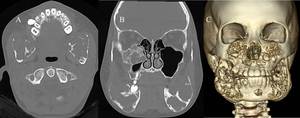
Fig. 30: (A)Axial, (B)Coronal (C)3D reconstructed CT images show similar findings to the plain radiograph with better demonstration of the bony expansion and cortical thinning.
Cherubism is a conditon where there is bilateral and symmetrical bony expansion of the mandible and maxilla due to lesions which are histologically identical to giant cell granuloma7. The disease begins in young children and other family members are also often affected. The condition is inherited as an autosomal dominant manner with variable penetrance. As the disease progresses,
the lesions evolve from a multiloculated,
soap-bubble appearance to a more sclerotic appearance with a decrease in size. Thus the disease often stabilizes and regresses without a need for treatment.
Case 9: Fibrous Dysplasis of the mandible
18-year old male presented for dental treatment. The plain radiographs shows asymmetric thickening,
expansion and sclerosis of the right side of the mandible with a 'ground-glass' density diagnostic of fibrous dypslasia.
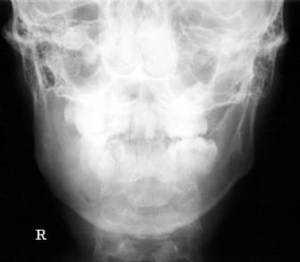
Fig. 31: The right side of the mandible is larger than the left and the bony matrix has been replaced by bone of 'ground-glass' density diagnostic of fibrous dysplasia.
Fibrous dysplasia is a condition characterized by patchy replacement of bone by fibrous tissue.
It is associated with bone deformities and pathological fractures.
There are two distinct forms of involvement - the monostotic (one bone) and polyostotic (multiple bones) forms. Craniofacial fibrous dysplasia is usually of the monostotic form. Histologically,
fibrous dysplasia shows replacement of normal bone by moderately cellular fibrous tissue containing irregularly shaped trabeculae consisting of woven bone without rimming osteoblasts that fuse with adjacent bone7. It is a self-limiting disease and treatment is required only if there are complications that arise due to local increase in the size of the involved bone.
Case 9: Metastasis
3 year 2 month old boy,
a known leukaemic patient presented with left sided jaw pain. CT shows a lucency in the left ramus of the mandible with involvement of the left side of the body of the mandible.
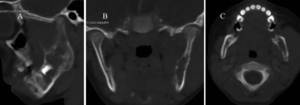
Fig. 32: Known leukaemic patient with bony infiltration of the left side of the mandible. (A)Sagittal oblique, (B) Coronal (C) Axial CT images show a lucency with irregular margins involving the left ramus and body of the mandible. Histological diagnosis revealed leukaemic involvement.
Metastatic disease may occasionally involve the mandible. In adults,
the most common sites are the kidneys,
lungs and breasts. Mandibular involvement is rare in children but should always be considered in the diagnosis,
especially if there is a known primary. Note that 30% of metastases originate from an unknown primary2.
Case 10: Osteomyelitis
12- year old girl presented with pain,
swelling,
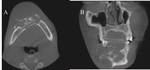
fever and soft tissue swelling over the left jaw. CT shows a lucent lesion with a cloaca and overlying periosteal reaction. These findings are consistent with osteomyelitis.
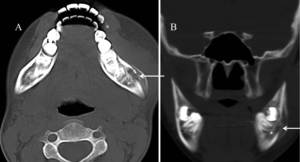
Fig. 33: (A)Axial (B)Coronal CT images shows a lucent lesion within the left side of the body of the mandible (*) with a cloaca (arrow) and overlying periosteal reaction. Overlying soft tissue swelling is also noted.
Osteomyelitis of mandible may give rise to various radiological appearances depending on whether it is acute or chronic. Acute lesions may not have any radiological findings in the early stage but chronic lesions demonstrate findings ranging from radiolucent to radioopaque. Low grade infections can cause sclerosing osteomyelitis a.ka.
Garre's sclerosing osteomyeltis in which periosteal new bone is deposited along the cortex and trabeculae2.