PLANTAR FASCIA:
Anatomy:
- Multilayered,
fibrous aponeurosis with medial,
central,
and lateral components.
- In the midsole,
it splits into five bands,
one for each toe,
that insert on the proximal phalanges.
The normal fascia appears as a thin (2–4-mm) band with low signal intensity on all pulse sequences
1) Plantar fasciitis
- Classically present as heel pain,
which is worse when weight bearing after a prolonged rest and eases with walking. Exacerbated by passive dorsiflextion.
- Low grade inflammatory process involving the plantar aponeurosis caused by:
- Degenerative
- Mechanical: repetitive injury
- Systemic: seronegative spondyloarthropathies (Ankylosing spondylitis,
Reiter syndrome,
psoriatic arthritis).
Image findings:
- Fusiform thickening of the calcaneal end of planter fascia and increased signal intensity of the proximal plantar fascia.
- T1/PD: Intermediate signal.
- T2/STIR: High signal.
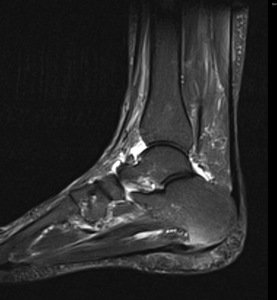
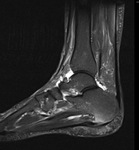
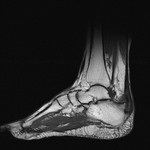
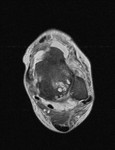
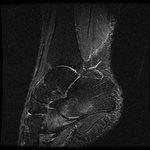
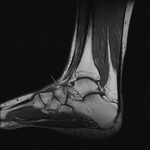
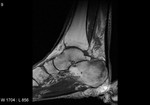
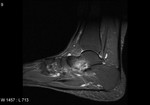
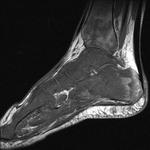
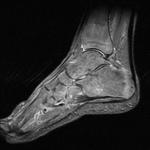
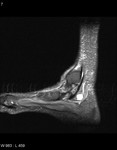
Fig. 1: Plantar fasciitis: STIR sagittal image showing thickening and hyperintensity of calcaneal insertion of plantar fascia with adjacent reactive bone marrow oedema in calcaneus .
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
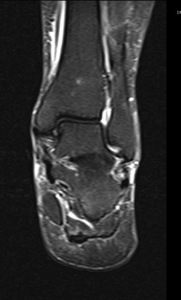
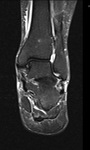
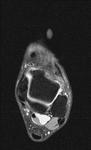
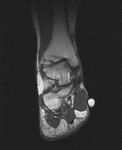
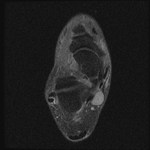
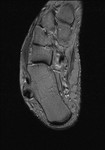
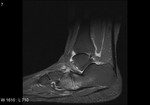
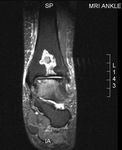
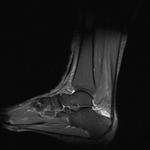
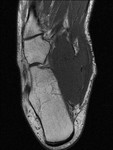
Fig. 2: Plantar fasciitis: STIR coronal image showing marked thickening of central band of plantar fascia with hyperintensity in underlying flexor digitorum brevis muscle .
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
2) Plantar fascia rupture
- Tear can occur in those with long standing plantar fasciitis and those treated with steroid injections.
Image findings:
- The plantar fascia is usually of low signal.
- Partial or complete discontinuity of the fascia demonstrate areas of T2 and STIR hyperintensity,
which represent haemorrhage and oedema.
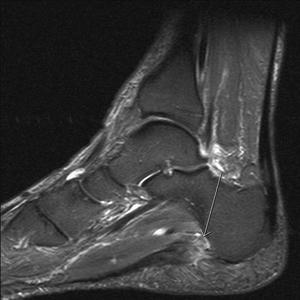
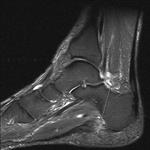
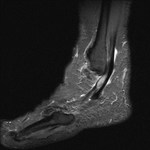
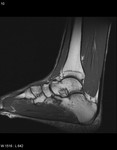
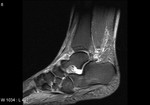
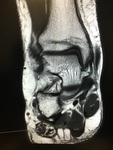
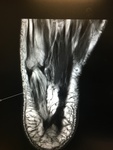
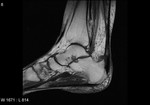
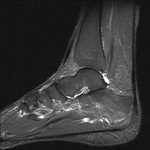
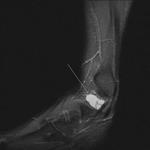
Fig. 3: Plantar fascia rupture: STIR sagittal image demonstrating almost complete discontinuity of the plantar fascia with associated hyperintensity suggestive of oedema and granulation tissue.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
3) Plantar fibromatosis.
- Nodules commonly located at the medial aspect of the plantar arch.
- Causes symptoms due to mass effect or invasion of the local structures such as muscles and neurovascular structures.
- Occurs in both paediatric and adult population with male predilection (2:1).
Learning point: It is associated with other fibroproliferative conditions such as Dupuytren disease.
In contrast with Dupuytren disease,
flexion deformity is not a common finding.
Image findings:
USS:
- Mixed echogenic,
nodular thickening of the plantar fascia,
separate from the calcaneal insertion.
MRI:
- T1/T2: Low-to-intermediate signal due to fibrous nature.
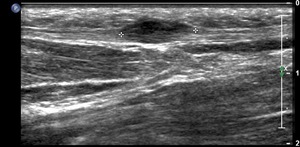
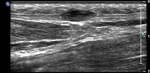
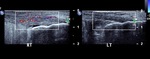
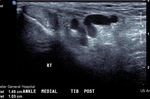
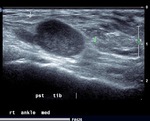
Fig. 4: Plantar fibroma: Ultrasound image demonstrating a hypoechoic nodular lesion in central band of plantar fascia
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
MUSCULAR,
TENDINOUS AND LIGAMENTOUS:
Anatomy:
- The Achilles tendon is formed by the tendons of the gastrocnemius and soleus muscles and inserts on the posterior aspect of the calcaneus.
- It is surrounded by loose connective tissue paratendon.
- Normal Achilles tendon has uniformly low signal intensity on MRI and a flattened or slightly concave anteriorly and measures less than 1cm in thickness.
Learning point: Atrophy of the soleus muscle is a more sensitive indicator of atrophy due to complete tear or denervation than gastrocnemius.
1) Insertional Achilles Tendinitis
- Common in runners and leads to development of enthesophyte.
Image findings:
- Thickened Achilles tendon distally.
- Ill-defined longitudinal high signal,
which can mimic partial tears.
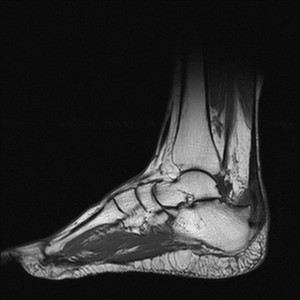
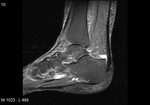
Fig. 5: Insertional Achilles tendinitis: T1 sagittal MRI Image shows thickening of the tendon at its insertion with intratendinous areas of increased signal intensity. Enthesopathic changes with osseous spur is seen at calcaneal bone tendon interphase.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
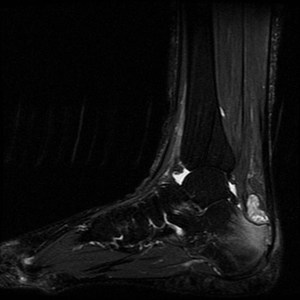
Fig. 6: Insertional Achilles tendinitis: T2 fat suppressed sagittal MRI demonstrates additional features of bone marrow oedema in calcaneus and high signal intensity in Kager's fat pad suggestive of inflammation. There is also evidence of retro calcaneal bursitis .
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
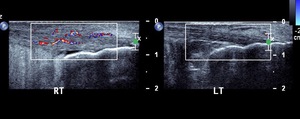
Fig. 7: Insertional Achilles tendinitis with retrocalcaneal bursitis:
Ultrasound image demonstrates heterogeneity of right Achilles tendon with intratendinous neovascularity .Fluid is seen in retro calcaneal bursa . Comparison with normal left side shown .
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
2) Tenosynovitis
- Inflammation of the synovial membrane surrounding the tendon.
- Causes:
- Injury
- Rheumatoid arthritis
- Infection
- Compartment syndrome
- Gout/pseudogout
- Diabetes.
Image findings:
MRI:
- T1: Low-to-intermediate signal
- T2: High signal
- Contrast enhancement of the tendon sheath thickening.
Learning point: Synovial membrane usually not seen unless there is pathology,
which present as increased fluid collection around the tendon,
thickening of the synovial sheath with increased colour flow.
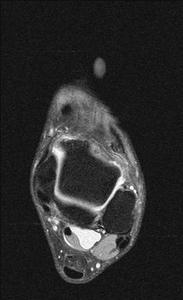
Fig. 8: Tenosynovitis of FHL :STIR axial MRI demonstrates fluid in the sheath of flexor hallucis longus disproportionate to ankle joint effusion.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
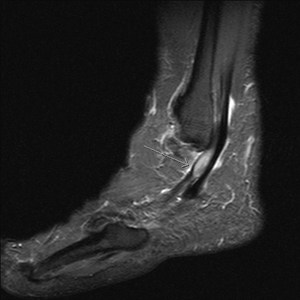
Fig. 9: Peroneal tenosynovitis: STIR sagittal MRI image shows thickened hyperintense peroneal tendons with fluid in common peroneal sheath.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
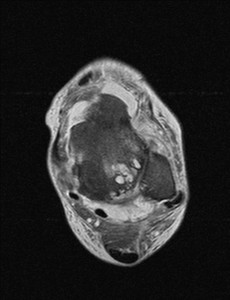
Fig. 10: Peroneal tendon dislocation: T2 Axial MRI image shows lateral dislocation of peroneal tendons over the lateral malleolus.There are also degenerative changes at the ankle joint .
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
3) Hypertrophic and accessory muscles
- Although accessory muscles are usually incidental findings,
they can cause symptoms as a result of local mass effect.
- Patients can present with local swelling or due to secondary compression of blood vessels,
nerves and tendons.
- Hypertrophic and accessory muscles can cause heel pain by nerve compression and are known cause of tarsal tunnel syndrome.
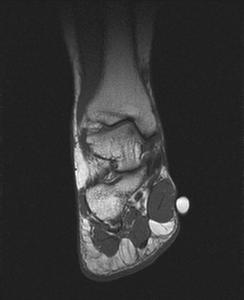
Fig. 11: Hypertrophic Abductor hallucis Muscle :T1 coronal image with a skin marker at site of discomfomt demonstrates hypertyrophic abductor hallucis muscle .
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
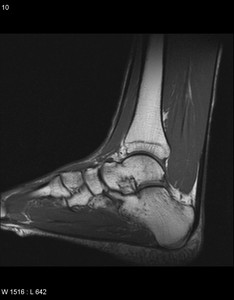
Fig. 12: Accessory Soleus with a fleshy insertion: Sagittal T1-weighted MR images shows accessory soleus with a fleshy insertion on the medial calcaneus .
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
4) Ligament strain (Sinus tarsi syndrome)
- Sinus tarsi syndrome - Instability of the subtalar joint due to significant ligamentous injury (talocrural interosseous and cervical ligaments) causing synovitis and scar formation within the sinus tarsi.
- Pain upon palpation of the sinus tarsi,
exacerbated by supination and adduction of the foot.
Image findings:
- Inflammatory,
scar and ligamentous injury within the sinus tarsi.
- T1 hyperintese fat replaced by scar tissue,
fluid and ligamentous disruption.
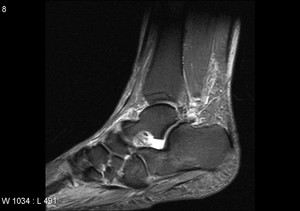
Fig. 14: Sinus tarsi syndrome: It is a clinical finding that mainly consists of pain and tenderness of the lateral side of the hindfoot, between the ankle and the heel.
PD FAT SAT sagittal image shows bright(fluid) signal intensity in sinus tarsi fat .
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
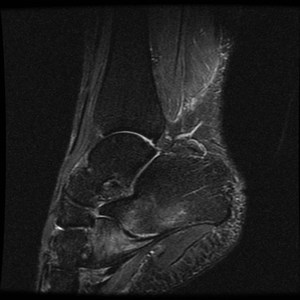
Fig. 13: Short Planter ligament sprain:
STIR sagittal image shows the sprain injury of the ligament.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
NEUROGENIC:
1) Neurogenic tumour
- Tumour that occurs along the path of the peripheral nerves.
Image findings:
USS: Oval,
homogenous,
hypoechoic mass in connection with the nerve.
Requires detailed knowledge of the course of the peripheral nerves.
Key learning point:
- Anterior tibial artery can be used as a landmark to find the deep peroneal nerve.
- Cortex of the distal fibula used to identify superficial peroneal nerve.
- Short saphenous vein that runs lateral to the Achilles tendon to identify sural nerve.
- Posterior tibial artery,
flexor digitorum/hallucis longus used to identify tibial nerve.
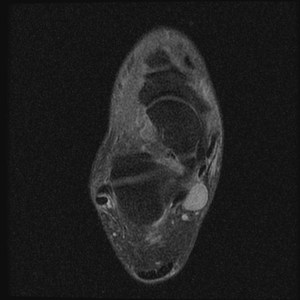
Fig. 15: Neurogenic tumour of posterior tibial nerve:STIR axial MRI iamge shows an ovoid well defined high signal mass lesion suggestive of neurogenic tumour arising from posterior tibial nerve .
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
2) Baxter's neuropathy
- Nerve entrapment syndrome that results from the compression of the inferior calcaneal nerve.
- The causes include altered foot biomechanics such as flatfoot,
plantar calcaneal enthesophytes and plantar fasciitis.
Image findings:
- Amyotrophy or fatty degeneration of the abductor digiti minimi muscle and less commonly of the flexor digitorum brevis and the quadratus plantae muscles.
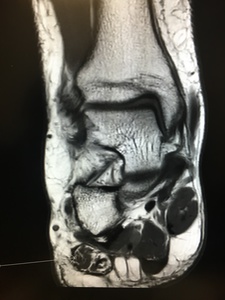
Fig. 16: Baxter's Neuropathy :In a 53 year old female with heel pain, T1 coronal and axial mri images show fatty changes within abductor digiti minimi muscle, suggestive of chronic denervation changes , in this case compression of inferior calcaneal nerve (Baxter nerve)was caused by plantar calcaneal spur and plantar fasciitis.
References: Radiology,NHS Trust, Heartland hospital ,Birmingham uk
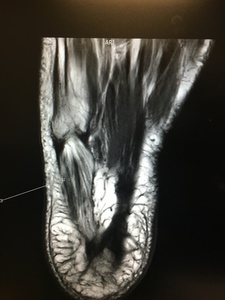
Fig. 17: Baxter's Neuropathy :In a 53 year old female with heel pain, T1 coronal and axial mri images show fatty changes within abductor digiti minimi muscle, suggestive of chronic denervation changes , in this case compression of inferior calcaneal nerve (Baxter nerve)was caused by planter calcaneal spur and planter fasciitis.
References: Radiology,NHS Trust, Heartland hospital Birmingham /UK
3) Tarsal tunnel syndrome
- Entrapment neuropathy of the posterior tibial nerve and/or its branches as it passes through the flexor retinaculum (the tarsal tunnel). This condition is similar to carpal tunnel syndrome of the wrist.
- Any space-occupying lesion within the tarsal tunnel can cause symptoms of pain and paresthesia of the toe,
sole and heel.
(50% are idiopathic).
- Ganglion cyst
- Tenosynovitis of flexor tendons
- Tumours (lipoma,
neurogenic)
- Os trigonum
- Hypetrophic and accessory muscles
- Vascular malformations
Image findings:
- Gives bone and soft tissue anatomy to delineate the cause of the tarsal tunnel syndrome.
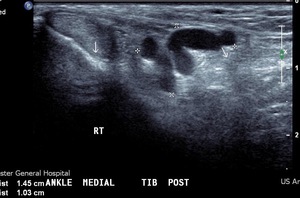
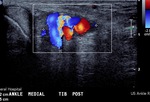
Fig. 40: Vascular malformation of tarsal tunnel: Ultrasound with colour doppler imaging shows vascular malformation in tarsal tunnel adjacent to posterior tibial nerve.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
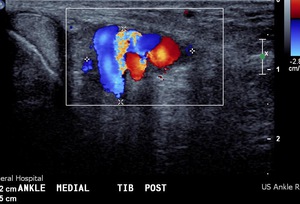
Fig. 41: Vascular malformation in tarsal tunnel: Ultrasound with colour doppler imaging shows vascular malformation in tarsal tunnel adjacent to posterior tibial nerve.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
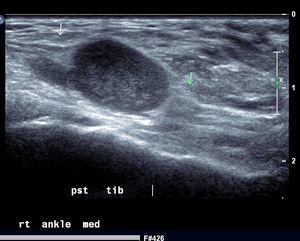
Fig. 42: Neurogenic tumour of posterior tibial nerve : Ultrasound image of a neurogenic tumour of posterior tibial nerve seen as well defined ovoid hypo echoic lesion arising from the nerve.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
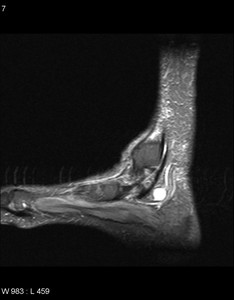
Fig. 43: Tarsal tunnel syndrome due to ganglion cyst: STIR sagittal iamge of hinfoot shows well circumscibed ganglion cyst in the course of posterior tibial nerve in tarsal tunnel.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
OSSEOUS:
1) Developmental/congenital
- Tarsal coalition is defined as partial or complete union of two or more bones of the mid/hindfoot.
- Occurs in up to 6% of the population with male predilection (4:1). It is bilateral in 50% of the cases.
- Present with pain,
tarsal tunnel syndrome,
perineal muscle spasms,
pes planus with increased incidence of osteoarthritis.
Learning point: Tarsal coalition refers to developmental anomaly rather than secondary causes such as rheumatoid arthritis.
Image findings:
- Calcaneonavicular (45%) -
- Involves anterior process of the calcaneus.
- Anteater nose sign.
- Talocalcaneal (45%) -
- C-sign
- Talar beak sign
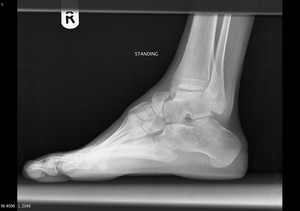
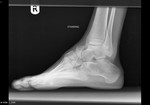
Fig. 18: Tarsal coalition: Plain radiograph showing calcaneocuboid coalition.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
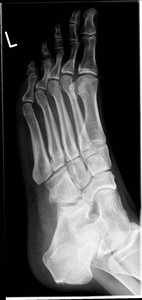
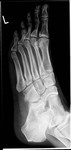
Fig. 19: Tarsal coalition : Plain radiograph showing Calcaneonavicular coalition
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
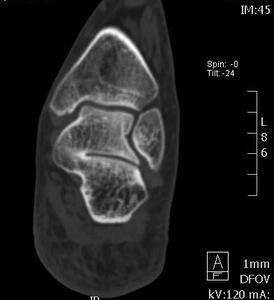
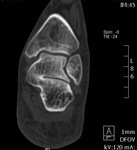
Fig. 20: Tarsal coalition: Coronal reconstruction of multi-slice CT demostrates osseous talocalcaneal coalition
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
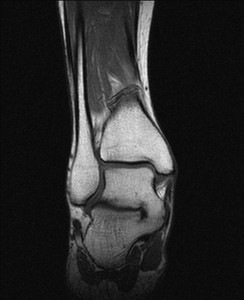
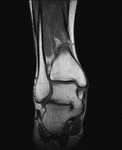
Fig. 21: Tarsal coalition: T1 Coronal MRI image showing osseous talocalcaneal coalition.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
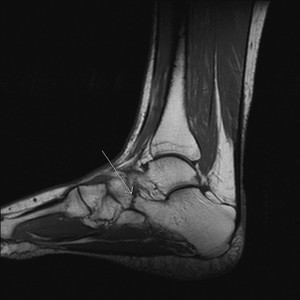
Fig. 22: Tarsal coalition: T1 sagittal MRI shows fibrous calcaneonavicular coalition
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
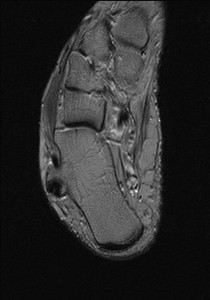
Fig. 23: Peroneal tubercle syndrome : T2 axial image shows elongated peroneal tubercle with irritation of peroneal tendons.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
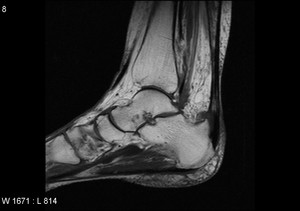
Fig. 24: Haglund deformity :T1 and STIR sagittal MRI shows bony prominence is seen on postero-superior aspect of calcaneal tuberosity. The soft tissue near the Achilles tendon becomes irritated when the bony enlargement rubs against shoes. This often leads to painful bursitis.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
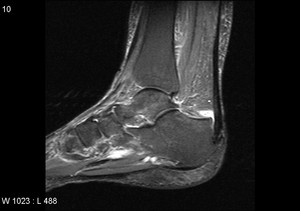
Fig. 25: Haglund deformity :T1 and STIR sagittal MRI shows bony prominence is seen on postero-superior aspect of calcaneal tuberosity. The soft tissue near the Achilles tendon becomes irritated when the bony enlargement rubs against shoes. This often leads to painful bursitis.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
2) Posterior impingement /Os trigonum
- Impingement syndome of the ankle,
described commonly in ballet dancers.
- Due to repetitive ankle plantar flexion.
- Presence of os trigonum is one of the predisposing factors.
- Other factors include: Stieda process (elongated lateral tubercle of talus),
fracture of the lateral tubercle of talus,
abnormal calcification of the posterior ankle,
superior slope of the calcaneal tuberosity and inferior slope of posterior tibial articular surface.
Image findings:
- Os trigonum and presence of other predisposing anatomical variants.
- Posterior capsular thickening and synovitis of posterior talofibular ligament.
- Tenosynovitis of flexor hallucis longus.
- Bone contusion of lateral tubercle of taus.
- T1: Low signal,
T2/STIR: High signal (bone contusion)
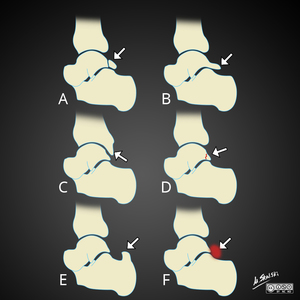
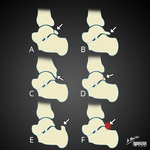
Fig. 26: Different causes of posterior impingement syndrome of ankle.
A) Os trigonum, B) Stieda syndrome C) Down-sloping posterior tibia D) Fracture through lateral tubercle of posterior process of talus E) Prominent superior calcaneus F) Inflammatory soft tissue.
References: Case courtesy of Dr Matt Skalski, Radiopaedia.org, rID: 35398
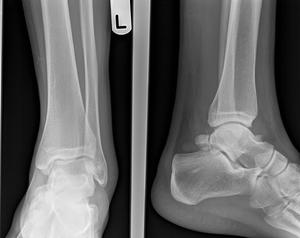
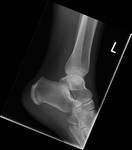
Fig. 27: Os trigonum : Lateral radiograph of ankle shows large well corticated ossicle around the posteriro margin of talus and calcaneum.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
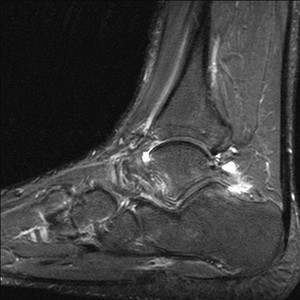
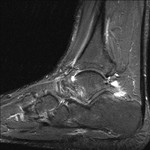
Fig. 28: Posterior ankle impingement: Sagittal STIR image of the ankle shows focal fluid collection and infalmmatory changes around the elongated posterior process of talus and mild bone marrow oedema.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
3) Fractures
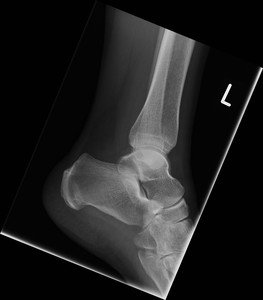
Fig. 29: Stress fracture of calcaneum : Plain radiograph showing linear sclerotic line in calcaneus suggestive of stress fracture .
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
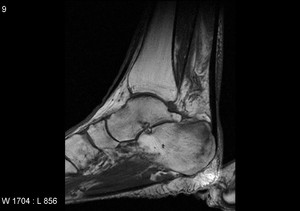
Fig. 30: Calcaneal stress fracture: T1 sagittal image demonstrates irregular linear low signal intensity line in posterior superior calcaneus in keeping with the stress fracture.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
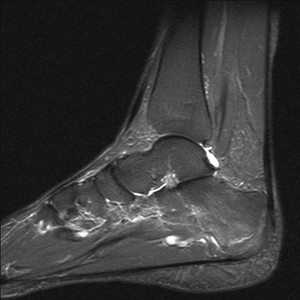
Fig. 31: Calcaneal Stress fracture: STIR sagittal image demonstrates high signal intensity fracture line in calcaneus with mild bone marrow oedema.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
4) Osteomyelitis
- Calcaneus is a common place for osteomyelitis in both children and adult population.
- In children,
it is usually from haematogenous spread whereas in adults,
it is from local soft tissue infection.
- Haematogenous osteomyelitis leads to metaphyseal predilection in children.
Osteomyelitis in adults occur in pressure points and sores.
Image findings:
- T1: decreased bone marrow signal.
- T2/STIR: Increased signal.
- Contrast enhancement clearly defines the border of infection than STIR
- Oedematous soft tissue involvement with loss of low signal cortex.
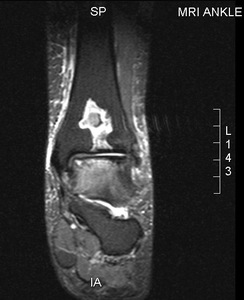
Fig. 36: Broadie's abscess: T2 fat suppressed coronal image shows well circumscibed abscess cavity with surrounding granualtion tissue in subarticualr distal tibia. Secondary arthrpathy of ankle joint with bone marrow oedema in talus.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
5) Bone Tumours
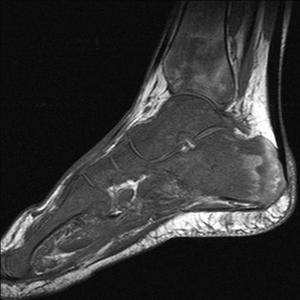
Fig. 37: Lymphoma of foot: T1 and STIR sagittal views show repalcement of bone marrow of foot and ankle bones with lymphoid tissue in a known patient of lymphoma.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
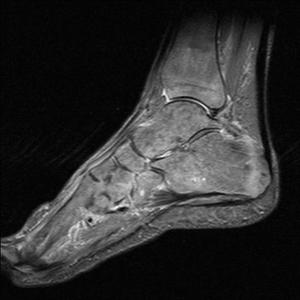
Fig. 38: Lymphoma of foot: T1 and STIR sagittal views show repalcement of bone marrow of foot and ankle bones with lymphoid tissue in a known patient of lymphoma.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
ARTHRITIS:
1) Inflammatory arthritis
- Encompasses wide range of pathology including septic arthritis,
rheumatoid arthritis and seronegative spondyloarthropathy.
- Characterised by bone erosions and uniform joint space narrowing.
- Monoarticular involvement requires infection to be considered.
- Bilateral,
symmetrical deforming arthropathies of hands in proximal distribution suggest rheumatoid arthritis.
- Multiple joint involvements in distal distribution with bone proliferation suggest seronegative spondyloarthropathy.
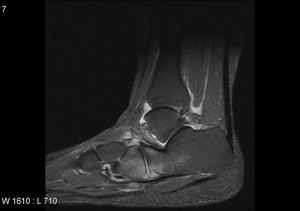
Fig. 32: Inflammatory arthritis: STIR sagittal image of hind foot shows calcaneo-cuboid joint subarticular bone marrow oedema with synovits. Further synovitis in ankle joint also demonstated.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
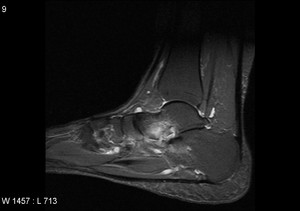
Fig. 33: Inflammatory arthritis: STIR sagittal image shows subarticular inflammatory changes in anterior subtalar joint with fluid and inflammation in sinus tarsi.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
2) Neuropathic joint
- Progressive degeneration and destruction of the joint,
secondary to abnormal pain sensation and proprioception.
- Occurs in patient with peripheral neuropathy (commonly diabetes).
- Six Ds of neuropathic joint:
- Dense bone
- Degeneration
- Destruction of articular cartilage
- Deformity
- Debris
- Dislocation
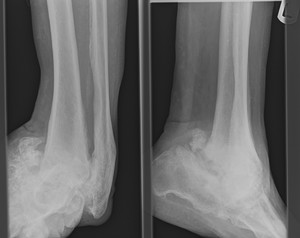
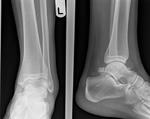
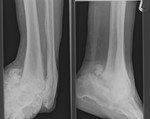
Fig. 34: Charcots arthropathy: AP and lateral radiographs of ankle shows marked disorganisation, destruction and bony debris involving ankle and subtalar joints.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
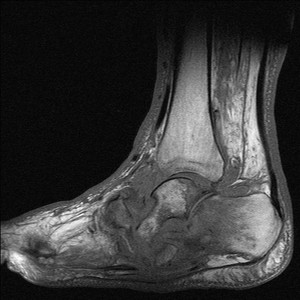
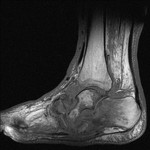
Fig. 35: Neuropathic arthropathy of mid and hind foot joints: T1 sagittal image of mid and hindfoot shows destruction and disoganisation of joints with rockerbottom deformity in a patient with known Diabetes.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
BURSAL:
- Inflammation of the retrocalcaneal bursa located between the posterosuperior calcaenus and anteroinferior calcaneal tendon.
- It is a component of Haglund syndrome (Figure 24).
- Patient present with painful ankle,
exacerbated by ankle dorsiflexion.
- Causes include,
injury,
inflammatory arthropathies and fracture.
Image findings:
USS:
MRI:
- T1: Low signal
- T2/STIR: HIgh signal
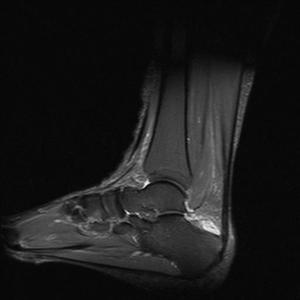
Fig. 39: Retrocalcaneal buristis
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
MISCELLANEOUS - SOFT TISSUE ABNORMALITIES:
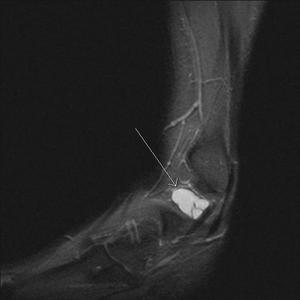
Fig. 44: Ganglion cyst: STIR sagittal image shows loculated ganglion cyst on lateral aspect of hindfoot just anterior to peroneal tendon and inferior to lateral malleolus.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK
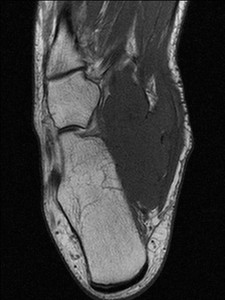
Fig. 45: Sarcoma of hinfoot: T1 axial image shows large medium signal intensity soft tissue mass on medial aspect of the hindfoot and involving muscles.
References: Radiology,NHS Trust, university hospital Leicester-Leicester/UK