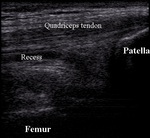
Suprapatellar recess is localized deep to the quadriceps tendon,
between the suprapatellar and prefemoral fat pad.
There is a physiological,
small amount of anechoic fluid within the recess in normal knee (Fig.1).
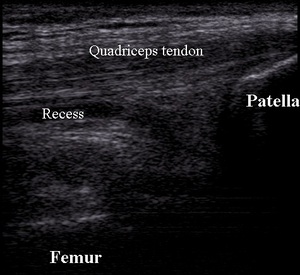
Fig. 1: Normal quadriceps tendon and suprapatellar recess
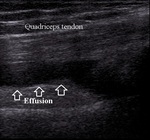
Ultrasound is sensitive in detecting very small amount of effusion in suprapatellar and parapatellar recesses.
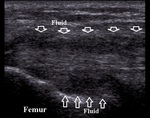
Quantity of the effusion can be a predictor of the degree of trauma (Fig.2).
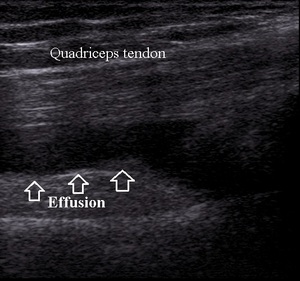
Fig. 2: Moderate effusion in suprapatellar recess
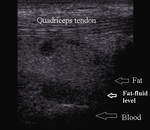
Quality of the effusion is also important.
Hemarthrosis could be an accurate sign for severe intra-articular trauma of the knee,
while lipohemarthrosis can be a reliable sign for an intra-articular fracture (Fig.3).
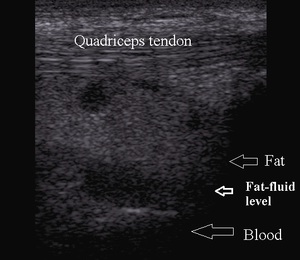
Fig. 3: Suprapatellar recess lipohemarthrosis
Quadriceps tendon inserts on the proximal patellar pole.
On sonography it appears as linear,
homogenous fibrillar structure in longitudinal plane (Fig.1,
2,
3).
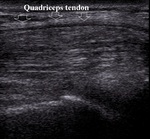
The main traumatic changes of the ligament include partial and full-thickness tear being very rare,
and more common tendinitis (Fig.4).
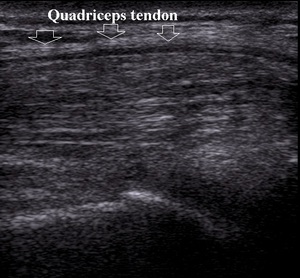
Fig. 4: Quadriceps tendon tendinitis
Patellar ligament (tendon) is easily visualized on ultrasound,
because it’s thick and has superficial location.
Normal patellar tendon is a hiperechoic,
fibrillar,
clearly demarcated structure in longitudinal plane,
oval in transverse plane inserting on lower patellar pole proximally and tibial tuberosity distally.
Its thickness is 4-5 millimeters and it’s widening at both insertions (Fig.5).
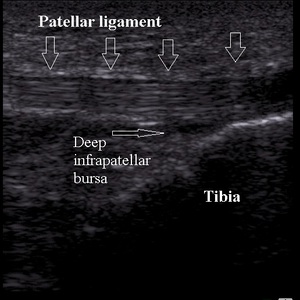
Fig. 5: Normal patellar ligament
Most common patellar ligament traumatic lesions are patellar tendonitis,
partial or full thickness tear and bursitis.
Inflammation of the patellar tendon (tendinopathy,
tendonitis,
tendinosis,
Jumper’s knee) is the most common type of patellar tendon pathology.
It’s an overuse syndrome usually affecting athletes with repetitive quadriceps muscle contractions,
including jumping and running.
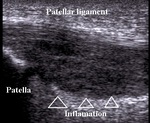
Inflamed patellar tendon is partially or totally thickened,
swollen-hipoechoic,
with disruption of normal fibrillar pattern and increased vascularization on Doppler (Fig.6).
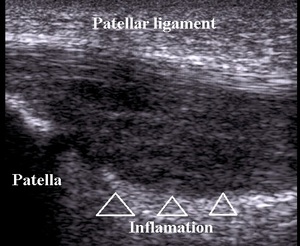
Fig. 6: Patellar ligament inflamation
Calcifications suggest chronic tendonitis.
Total tear of the patellar ligament is rare.
It could be a result of acute trauma in athletes,
local corticosteroid injections or more often consequence of chronic microtrauma causing tendon degeneration and tear.
There is a discontinuity between the ruptured fragments,
tendon is swollen,
thickened,
fluid-blood is often visualized near the rupture.
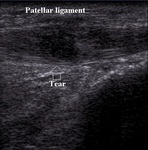
Focal hipoechoic lesion within tendon is visible in partial thickness tear (Fig.7).
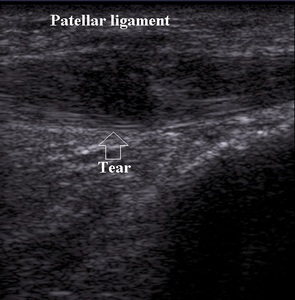
Fig. 7: Partial thickness tear of patellar ligament
Common pathology of patellar tendon in adolescence are Osgood-Schlater disease and Sinding-Larsen-Johansson disease,
both connected to sport activities,
traction trauma,
affecting distal and proximal tendon insertion.
Usually there are signs of bone fragmentation and irregularity at the insertion spot as well as signs of tendonitis.
There are several bursae around the patellar ligament.
Prepatellar bursa is a tricompartmental structure.
It lies between the patellar surface and the subcutaneous fat.
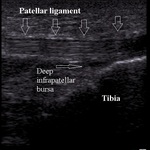
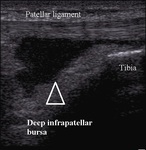
Deep infrapatellar bursa is localized between the distal patellar insertion and tibial surface,
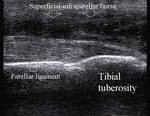
and superficial infrapatellar bursa lies superficially to the tibial tubercle.
Most common ultrasound signs for bursitis are enlarged bursa,
filled with anechoic or hypoechoic fluid and bursal wall synovial hypertrophy.
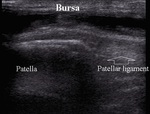
Prepatellar bursitis,
also known as housemaid’s knee is a result of chronic microtrauma-friction usually as a result of kneeling or rarely arauma (Fig.8).
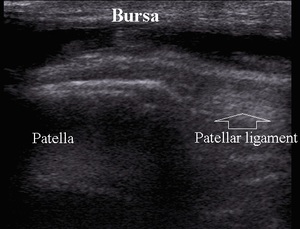
Fig. 8: Prepatellar bursitis
Deep infrapatellar bursitis occurs as a consequence of repetitive,
excessive knee extension in jumping,
running (Fig.9).
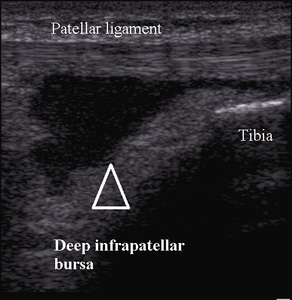
Fig. 9: Deep infrapatellar bursitis
Superficial infrapatellar bursitis can occur in direct trauma or extended kneeling (Clergyman’s knee) but also in other conditions (Fig.10)
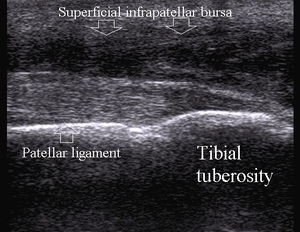
Fig. 10: Superficial infrapatellar bursitis
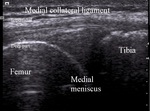
Medial collateral ligament spreads from the femoral epicondyle proximally to the medial tibia distally.
It consists of 2 hipoechoic longitudinal prats,
superficial and deep part,
later forming a part of the joint capsule.
Both parts are divided by a thin hiperechoic part representing fatty tissue and ligament bursa (Fig.11).
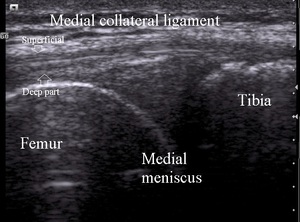
Fig. 11: Medial knee normal anatomy
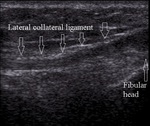
Lateral collateral ligament is a thin cord spreading from the lateral femoral epicondyle to the fibular head (Fig.12).
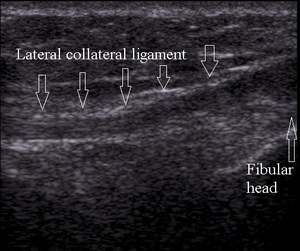
Fig. 12: Normal lateral collateral ligament
Collateral ligament trauma is common,
especially the medial collateral ligament,
which is the commonest ligament injury of the knee (Fig.14).
When the ligament is torn partially,
in acute period it is thickened,
heterogeneously hipoechoic,
its normal structure is disrupted,
with various amount of fluid,
edema and blood around the ligament (Fig.13).
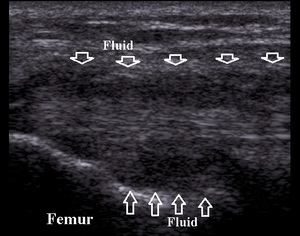
Fig. 13: Lateral collateral ligament partial thickness tear
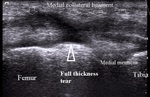
In full thickness tear the ligament is separated in two parts,
with hemorrhage or granulose tissue between the fragments (Fig.14).
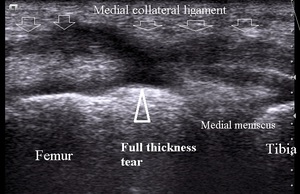
Fig. 14: Medial collateral ligament full thickness tear
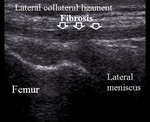
In chronic ligament tear hipoechoic thickened part of the ligament can be visualized,
representing fibrous scarring tissue,
also calcifications are sometimes seen.
Bone avulsion injuries are also common (Fig.15).
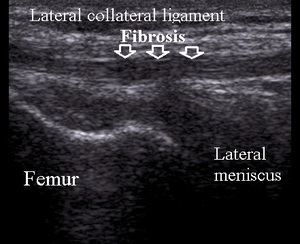
Fig. 15: Lateral collateral ligament chronic tear
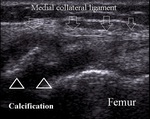
Pellegrini-Stieda lesion is a chronic medial collateral ligament tear with calcification forming near the proximal ligament insertion (Fig.16).
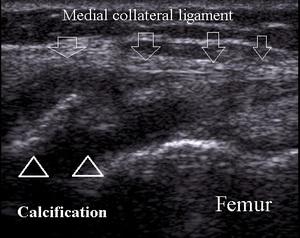
Fig. 16: Pellegrini-Stieda lesion
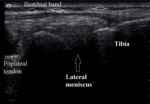
Iliotibial tract (band) inserts on Gerdy tubercle,
on the anterolateral tibial surface.
It’s clearly visible on ultrasound because of its superficial localization (Fig.17,
18).
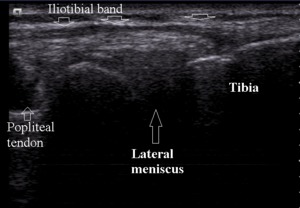
Fig. 17: Lateral knee normal anatomy
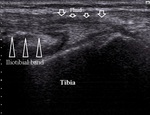
The most common traumatic disorder is iliotibial tract friction syndrome,
appearing in long-distance runners and cyclers.
It’s usually moderate hipoechoic and thickened,
with soft tissue edema around it (Fig.19).
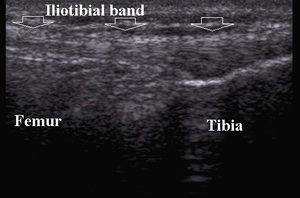
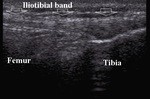
Fig. 18: Normal iliotibial band
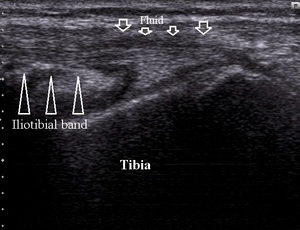
Fig. 19: Iliotibial band friction syndrome
Avulsion fractures of small bony fragments,
sometimes overlooked on initial radiography can be identified on ultrasound.
Stieda fracture is avulsion of bony fragment at the proximal insertion of medial collateral ligament.
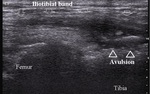
Segond fracture is bony avulsion from the tibial insertion of the lateral capsular ligament.
It can be clearly demarcated on ultrasound (Fig.20).
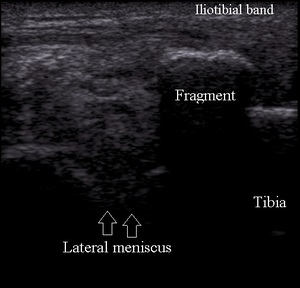
Fig. 20: Segond avulsion fracture
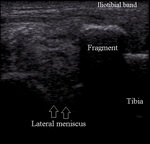
Avulsion fracture of iliotibial band insertion on Gerdy tubercle is very rare (Fig.21).
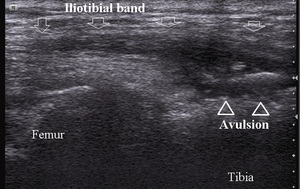
Fig. 21: Iliotibial band avulsion fracture
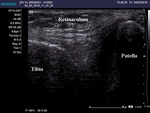
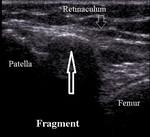
More common is avulsion of small osteochondral fragments originating from medial patellar facet or fracture of small lateral femoral condyle fragment (Fig.22) in lateral patellar dislocation (Fig.23).
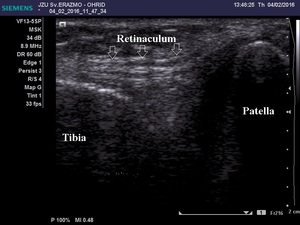
Fig. 22: Normal medial patellar retinaculum
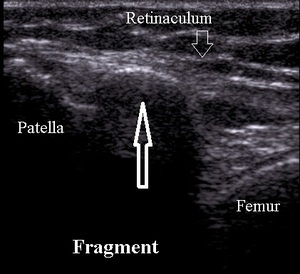
Fig. 23: Medial patellar facet osteochondral fracture
Meniscal tears,
especially in superficial parts can be adequately examined with ultrasound.
Normal meniscus is a triangular,
hiperechoic structure with smooth surface between the femoral and tibial articular surface (Fig.11,
17).
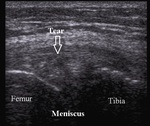
The main sonographic signs for meniscal ruptures are linear hiperechoic defect within the meniscus or spreading to the meniscal articular margins (Fig.24),
meniscal irregular surface,
change of meniscal shape compared to contralateral knee,
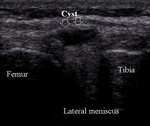
presence of meniscal cysts (Fig.25).
Medial meniscus is more commonly injured.
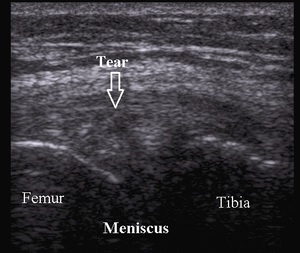
Fig. 24: Medial meniscus tear
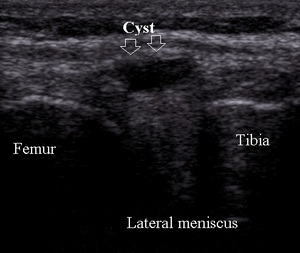
Fig. 25: Lateral meniscal small cyst