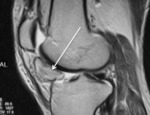
Fat pad impingement syndromes are frequently the result of an acute trauma or repetitive micro-trauma that may cause hemorrhage or inflammation of the respectively injured fat pad.
Generally hemorrhage and inflammation result in swelling and hypertrophy of the adipose structure leading to compression of adjacent structures which consequently cause more inflammation and the outcome is an injure cycle.
The method of choice for the diagnosis of these lesions is MR.
This imaging technic can show inflammation of anterior fat pads of the knee,
which manifest as areas of increased signal intensity on fluid sensitive sequences.
In anterior suprapatellar fat pad impingement syndrome the cause is usually due to either a developmental cause related to the anatomy of the extensor mechanism,
direct trauma,
overuse or to abnormal mechanics (high knee flexion angles).
In this syndrome the posterior border of the fat pad is convex with mass effect upon the suprapatellar recess and therefore a cause for anterior knee pain.
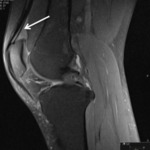
The most significant imaging finding is an increased signal of anterior suprapatellar fat pad (quadriceps fat pad) on fluid sensitive sequences.
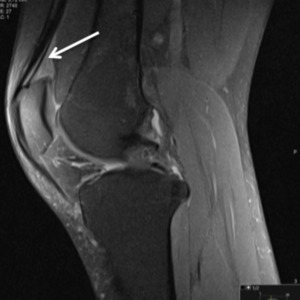
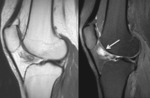
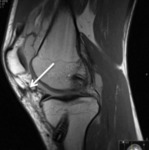
Fig. 3: Sagittal PD fat sat; Anterior suprapatellar impingement syndrome
In Hoffa’s disease (infrapatellar fat pad impingement syndrome) the cause is usually due to a forceful direct impact to the patella that could be single or repetitive.
The inflamed fat pad becomes hypertrophied with predisposition to impingement between the tibia and femur.
As described previously,
the hemorrhage and edema will occur with mass effect of the surrounded structures (acute phase),
with continuous aggression of Hoffa’s fat pad a fibroblastic response will follow and the result will be fibrocartilaginous tissue that rarely can undergo ossification (chronic phase).
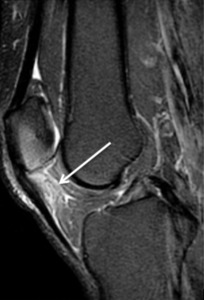
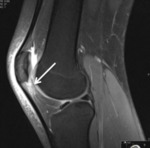
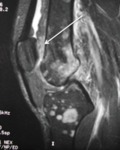
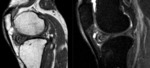
Fig. 5: Sagittal T2 fat sat; Hoffa disease
- Imaging features of the acute phase – High signal intensity on T2-weighted MR images and GAD enhancement
- Imaging features of the chronic phase – Low signal intensity on both T1 and T2 weighted MR images.
There were described three types of inflammatory alterations in Hoffa’s fat pad:
- Hoffa’s disease with inflammatory changes occurring homogenously and affecting the entire infrapatellar fat pad (described above)
- Impingement of the superolateral aspect of the infrapatellar fat pad
- Infrapatellar plica syndrome
Impingement of the superolateral aspect of the infrapatellar fat pad (clinically more common but radiologically more subtle than the previous one) occurs at the superolateral portion of the fat pad between the patellar tendon and lateral femoral condyle as a secondary sign of patellofemoral maltracking,
occurring between the patellar tendon and the lateral femoral condyle and causing a friction syndrome.
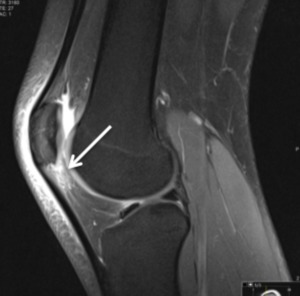
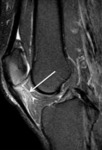
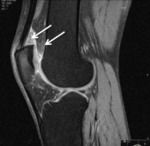
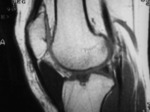
Fig. 6: Sagittal PD fat sat; Impingement of the superolateral aspect of the infrapatellar fat pad
Imaging features of this pathology are high T2 signal intensity related to edema of the superolateral portion of the fat pad and occasionally high signal cartilage of the lateral condyle.
Infrapatellar plica syndrome may be difficult to differentiate from Hoffa’s disease.
Edema and fibrotic thickening of the Hoffa’s fat pad is also characteristic and the clue to diagnosis consists in the locations of these alterations.
If these features follow the anatomy of the plica then infrapatellar plica syndrome is the most probable diagnosis.
The plica or ligamentum mucosum is a ligament formed between eighth and twelfth weeks of gestation from synovial mesenchyme that normally is later resorbed but can persist giving rise to the plica.
The infrapatellar plica is slightly more common in males.
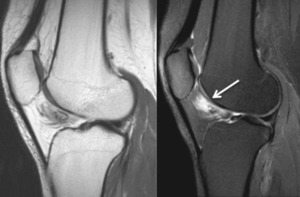
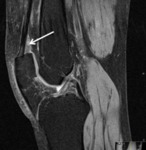
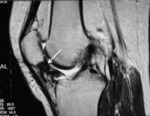
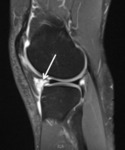
Fig. 7: Sagittal T1 fse and T2 fat sat; Infrapatellar plica syndrome
Posterior suprapatellar fat pad impingement (prefemoral fat pad) can occur between the patellar under surface and the anterior surface of the distal femur.
The result will be an enlargement and high signal intensity on fluid-sensitive sequences of this fat pad.
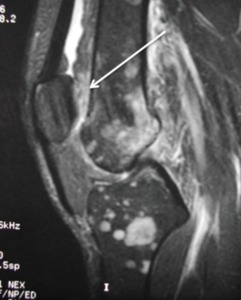
Fig. 8: Sagittal T2 fat sat; Posterior suprapatellar fat pad impingement in a patient with leukemia
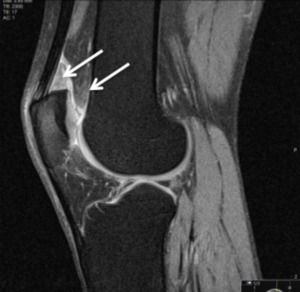
Fig. 9: Sagittal T2 fat sat; Edema of the anterior and part of the posterior suprapatellar fat pad.
Another type of fat pad alterations are post-operative related changes in which the major consequent imaging feature is fibrosis resulting in areas of low signal intensity on MR in T1 and T2 weighted images.
They can be divided in post-surgical,
post-arthroscopic and Cyclops lesion in anterior cruciate ligament (ACL) reconstruction.
In post-arthroscopic the alterations are seen in portal site and are typically linear and horizontal lesions with the post-operative alterations more extensive.
The cyclops lesion (localized anterior arthrofibrosis) is a complication of ACL reconstruction and the imaging feature is a soft-tissue mass within the Hoffa’s fat pad located anteriorly or anterolaterally in the intercondylar notch near the tibial insertion of the reconstructed ACL and as in the previous entities it is mainly composed of fibrous tissue so it has low intensity on T1 and T2 weighted images.
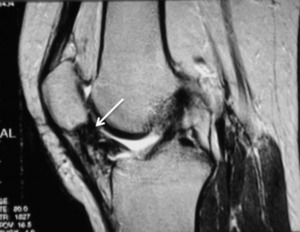
Fig. 10: Sagittal T2 FSE; Arthrofibrosis
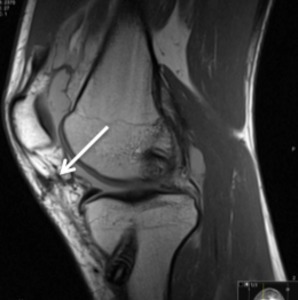
Fig. 11: Sagittal PD; Linear fibrosis post-arthrocopy
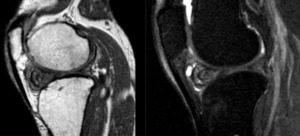
Fig. 12: Sagittal T1 and T2 fat sat; Cyclops lesion in a patient with ACL reconstruction
Another intrinsic alteration of the Hoffa’s fat pad is the presence of an intracapsular chondroma,
a benign cartilaginous soft tissue tumor that results from extrasynovial metaplasia of the capsule or adjacent connective tissue.
It is a rare form of chondroma characteristically located inferior to the patella.
Imaging features of intracapsular chodromas can show a calcified lesion (low signal on MR) with areas of high signal intensity on T2 weighted images as a result of chondroid matrix and edema.
Fat pad abnormalities can however be caused by extrinsic factors as joint effusion,
meniscal cysts,
ganglion cysts and localized nodular synovitis.
Joint effusion is a usual finding in the knee,
however if it is of great volume it will compress the adjacent structures.
In infrapatellar fat pad the normal clefts previously described are normal structures and should not be mistakenly identified as injuries.
Meniscal cysts are extrusions of synovial fluid through a meniscal tear (horizontal or complex).
If they occur anterior and medially they project themselves into the infrapatellar fat pad.
Deep infrapatellar bursitis is an abnormal distention of deep infrapatellar bursa due to inflammatory conditions.
Ganglion cysts are formed from synovial herniation or tissue degeneration developing from the joint capsule,
ligaments,
bursa,
tendon sheaths or subchoncral bone.
They can be unilocular or multilocular.
Unlike meniscal cysts,
ganglion cysts are not associated with meniscal tears.
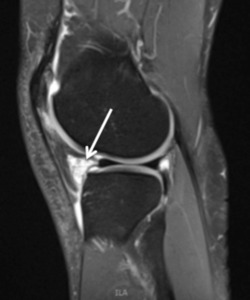
Fig. 14: Sagittal PD fat sat; Ganglionic cyst (no meniscal tear)
Localized Nodular Synovitis (villonodular synovitis) is a benign proliferative disorder that can affect fat pads.
On MR it appears as a well-defined
mass.
The signal intensity are variable and include high signal intensity on T2 images from edema and low signal intensity in all sequences due to hemosiderin (iron content).
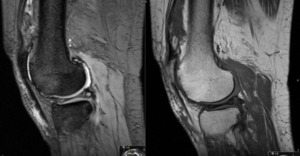
Fig. 15: Sagittal T2 * and T1 SE; Suprapatellar villonodular synovitis
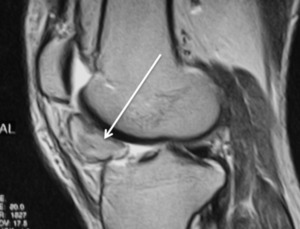
Fig. 16: Sagittal T2 FSE - Infrapatellar villonodular synovitis