The physical background,
correct instrumentation and technical procedures for basic and innovative Ultrasound (US) imaging are described below,
subdivided into several topics.
US Imaging:
· B-Mode.
· Elastosonography.
· Bi-dimensional Panoramic Imaging.
· Three-dimensional Panoramic imaging.
· Volumetric imaging.
· Low Mechanical Index (MI) Contrast Enhanced Ultrasound (CEUS).
Doppler hemodynamics evaluation modalities:
· Pulsed Wave Doppler.
· Color Doppler.
· Power Doppler.
The details of insonation and advanced imaging technologies (harmonic imaging,
speckle reduction and compound imaging techniques) are also described below.
Ultrasound physical principles and their application: IMAGING
Ultrasound definition
Ultrasound is made up of mechanical sound waves.
Typical ultrasound frequencies are higher than those generally audible by the human ear: 20 kHz is the conventional frequency value applied to discriminate standard sound frequencies from ultrasound.
In Diagnostic Ultrasonography,
mechanical sound waves are produced by a piezo-ceramic crystal inserted into a probe,
kept in direct contact with the patient’s skin by an acoustic coupling gel.
This probe generates the ultrasound waves,
then receives the acoustic return signal (commonly referred to as “echo”).
The ultrasound used in sonography usually has a frequency of between 1 and 22 MHz.
Ultrasound interaction and phenomenology
Like any other wave phenomenon,
ultrasound is subject to:
• Reflection - reflection can be specular (single direction) or diffuse (several directions).
Diffused echoes are the ones which do not return to the probe,
usually occurring where tissue has complex interfacing surfaces.
• Refraction - deviation of a wave passing from one physical medium to another,
changing its propagation velocity.
• Scattering - deflection/dispersion due to the change of direction of an incident wave,
when colliding with a surface.
• Absorption - reduction of wave intensity with increasing distance from the source; refraction it depends on the type and thickness of a single tissue and on transmission frequency.
• Attenuation - attenuation proportionally increases with longer distances and higher frequencies.
Ultrasound can be defined through parameters such as frequency,
wavelength,
propagation velocity,
intensity (measured in dB) and attenuation (due to the acoustic impedance of the medium the ultrasound wave travels through).
Acoustic impedance
When an acoustic wave reaches the point where acoustic impedance changes,
the wave can be reflected,
refracted,
diffused or damped.
The reflected portion provides information on the different impedances of the two tissues and is given by the following formula:
R = (Z1 – Z2)2 / (Z1 + Z2)2
Where: Z = acoustic impedance factor
As bone impedance (high Z) is very different from tissue impedance,
sonography does not allow us to see what is behind a bone structure.
Air and gas filled regions (low Z) produce a “shadow” effect,
due to the total reflection of ultrasound.
Acoustic impedance (Z) is the property that lets us distinguish between the different tissues of the body area examined.
No reflection is produced within a perfectly homogenous medium.
Ultrasound velocity
The propagation velocity (V) of ultrasound depends on the density and stiffness of the medium the acoustic wave passes through.
V = λ x F
Where:
V= velocity (m/sec)
λ = wavelength = distance covered by a wave in a cycle
F = frequency = number of oscillations within a time unit (T=1/F) expressed in Hz
In biological tissue,
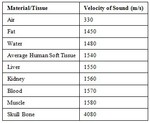
ultrasound velocity (V) is about 1540 m/s,
except in the bone,
where ν = 4000 m/s.
The average propagation velocity within human body soft tissue is considered to be 1540 m/s (see Table 1).
Sonography
Sonography is a medical diagnostic method which does not use ionizing radiation.
It is based on the transmission of ultrasound waves and the emission of echoes by the detected targets.
Sonography is an operator-dependent and patient-dependent diagnostic technique.
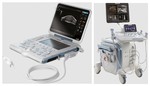
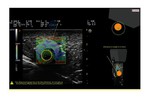
Ultrasound system
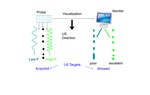
A Diagnostic Ultrasound system (Figure 1) includes three main functional blocks:
1) a probe transmitting and receiving the signal
2) a central electronic system which:
• generates the transmission pulse
• receives the return signal (echo) from the probe
• processes the received signal
3) a visualization system (monitor) displaying the image in grayscale,
obtained by the conversion of the ultrasound return signal
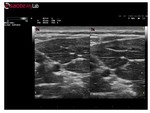
Axial Resolution and Lateral Resolution
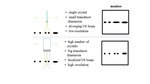
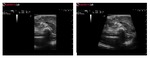
Ultrasound axial resolution can be defined as the minimum distance at which a double target can be distinguished as two separate targets along the ultrasound beam axis.
The axial resolution is determined by emission frequency: a high frequency wave with a corresponding short pulse length will yield better axial resolution than a low frequency wave (Figure 4).
Ultrasound lateral resolution is the minimum distance at which a double target can be distinguished as two separate targets (Figure 5) along a direction perpendicular to the ultrasound beam axis.
Lateral resolution depends on the focal zone area and increases:
• when the frequency increases
• decreasing the size of the elements of the transducer
• increasing the number of elements in the transducer
The frequency adjustments for improved Spatial (Axial and Lateral) Resolution in ultrasound beam penetration capabilities can be summarized as follows:
• High frequency enables High Spatial Resolution but Low Penetration
• Low frequency enables High Penetration but Low Spatial Resolution
Temporal and Contrast Resolution
Temporal Resolution indicates the system capacity to represent rapid movement of structures; it is quantified by calculating the number of images in each time unit (Frame Rate) and it depends on:
• Field of view dimensions
• Number of focal points
• Scan depth
• Line density
Contrast Resolution indicates the distribution of black and white levels on the US image; it specifies the ultrasound system ability to discriminate between two structures with different acoustic impedance.
It depends on:
• Intensity of the echoes (Gain and TGC)
• Dynamic range
• Gray Maps
• Pre and post-processing (e.g.
Spatial Compound techniques and Speckle Reduction Algorithms)
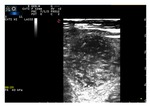
B-Mode Parameters
B-Mode is the primary method of ultrasound imaging and its most important parameters are:
• Dynamic Range
• Enhancement
• Density
• Gray Map
• General Gain intensity: regulates the strength of the echoes received (amplification)
• TGC – Time Gain Compensation: adjusts the sensitivity at each depth to allow compensation for signal attenuation from the deepest tissues and structures (amplification)
• Scan Depth
• Scan Width
• Transmission Frequency
• Zoom factor
• Ultrasound beam focus and number of focal points
Pre-Processing Parameters
The group of so-called pre-processing parameters is made up of:
• Dynamic Range – related to the number of gray levels available during acquisition to represent the return echoes (measured in decibels,
dB)
• Enhancement - emphasizes the differences in density between two adjacent structures by amplifying the higher frequencies of the received echo
• Density – characterized by the number of lines making up the transmitted ultrasound beam (an increase reduces the frame rate)
Dynamic Range
The dynamic range in signal processing is the range between the minimum and maximum intensity signals that a system can display.
Changing the Dynamic Range generates the following outcomes:
• Higher Dynamic Range value - the image tends more toward Black (used to discriminate two levels of gray close to White)
• Lower Dynamic Range value - the image tends more toward White (used to discriminate two levels of gray close to Black).
See Figure 6.
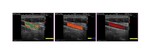
Post-Processing Parameters
Gray Map (called also Gray-scale) is a post-processing parameter for changing the gray level representation of the echo image on the monitor.
This is why there are usually pre-set curves (customizable by the operator) that represent various combinations of grayscale and echo amplitude.
Each gray map allows users to display US images with different patterns of contrast (Figure 7).
Gray Map adjustment is a function that links the input represented by the ultrasound echo amplitude to the output represented by the gray tones of the points corresponding to the ultrasound echo image displayed on the monitor.
Gain (Signal Amplification)
The received echoes have less amplitude than the transmitted ultrasound waves,
therefore amplification of the received echoes and the depth of compensation (Time Gain Compensation - TGC) is fundamental for accurate echo image representation.
If the return echo signal is very low,
it must be amplified before being sent for processing and display.
There are two different gain controls on the US scanner:
• A dedicated control (General Gain) which defines the overall signal level (general control).
• A certain number of TGC cursors that control signal amplification at a certain depth (relative control).
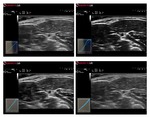
General Gain for ultrasound echoes refers to the degree of amplification applied to all return echo signals.
If it is too low there will be under-amplification of the echo signal and the image will be very dark.
If it is too high there will be over-amplification of the displayed echo image,
introduction of artifactual noise and a reduction in contrast resolution,
with all echoes getting progressively brighter (Figure 8).
Due to the attenuation of ultrasound in the human body (1dB/cm/MHz),
echoes from structures far away from the transducer have lower intensity/amplitude than for similar structures closer to the transducer.
The TGC control compensates this effect by progressively increasing the amount of amplification applied to signals/echoes with a higher return time,
a function of penetration depth (Figure 9).
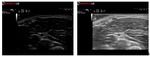
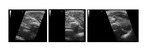
B-Mode Advanced Technologies: XView
XView is a real-time algorithm that provides speckle reduction.
It does this during each of the stages that constitute the ultrasound image formation process.
XView enables configuration of the different image characteristics in terms of smoothing (image homogeneity),
detail (reintroduction of the original speckle for each pixel) and enhancement (highlighting hyper-echoic structures).
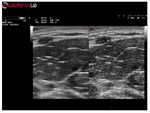
B-Mode Advanced Technologies: MView
MView Technology consists of an ultrasound technique that uses electronic beam steering of a transducer array to acquire several co-planar scans of an object from different view angles: pulses are transmitted both perpendicular to the transducer array and in oblique directions (Figure 10).
Different pulses from different angles are correlated to form one final image.
MView Technology has many advantages:
• structures with curved and irregular borders are more readily visualized
• tissue margins are more clearly visible
• image homogeneity is increased
The use of XView and MView technologies at the same time significantly increases image quality (Figure 11).
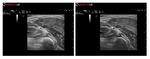
B-Mode Advanced Technologies: TPView
TPView enables the trapezoidal imaging format of the echo viewing angle for the linear transducer (Figure 12).
B-Mode Advanced Technologies: BSteer
The BSteer function performs lateral steering of the B-Mode echo image.
This tool is especially useful when limited access does not allow optimal probe positioning for detailed examination of an internal body area (Figure 13).
Harmonic Imaging
Harmonic Imaging is an ultrasound technique that analyzes the harmonic component of the reflected echo.
The ultrasound signal generated by the probe is usually a sine wave; the returned echo is no longer sinusoidal and contains many frequencies that are integer multiples of the fundamental transmitted frequency.
Most of the distortions and the "noise" present in the return echo are related to the fundamental frequency.
In Harmonic Imaging,
the fundamental frequency component of the return echo is eliminated,
maintaining only the second harmonic echo signal components.
It is completely detached from the second harmonic (twice the transmitted frequency) of the return echo.
Greater amplification of the received signal is therefore needed,
because the echo amplitude in the second harmonic is much lower than the one at the fundamental frequency (Figure 14).
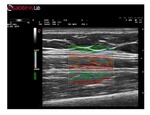
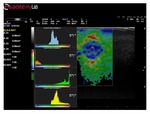
Elastosonography
Elastosonography is a non-invasive method that supports the physician in assessing tissue elasticity.
This technology provides additional information to standard B-Mode and a better definition of a potential lesion area,
making it suitable for diagnosis and follow-up.
The elastosonography ultrasound image is computed in real-time by coding information related to tissue strain,
since regions of different stiffness are differently compressed.
In order to perform the elastosonography examination,
users must apply perpendicular pressure through rhythmic movements on the tissue.
The pressure applied by that action allows us to evaluate the modification of the echo signal and thus compute how the different tissues distort (if they are soft) or move (if they are hard) compared to the probe position.
The result of this calculation,
computed in real time,
is shown by a color image overlapping the B-Mode image.
The degree of deformation is given by a chromatic scale.
Strain elastosonography is a qualitative analysis where the estimation of strain information is computed in relation to the surrounding tissue (Figure 15).
Common strain elastosonography workflow tools are:
• Real-time acquisition feedback - real-time feedback on the acquisition quality is displayed to allow adjustments of the probe movement,
thus improving the elastosonography image quality,
and giving information on the quality of the acquisition,
correlated to the compression applied by the probe.
• Dual View - allows real-time comparison between the B-Mode and elastosonography imaging methods to facilitate image interpretation.
• Motion Graph – the trace can be visualized relative to the probe motion during elastosonography application.
This is intended for measurement of compression or release of the tissue being examined.
Elastosonography Measurements
• Ratio – semi-quantitative measurement that enables relative measurement of the stiffness of a Region of Interest (ROI) compared to another reference ROI
• Hardness/Softness Percentage – indicates how many pixels of the elastosonography echo image are below or above a fixed threshold on the color palette
• Histogram: available for all the measurement regions (Hard to Soft,
Mean,
SD,
0-100 scale) to assess the hardness or softness homogeneity of one or more elastosonography echo image areas (Figure 16).
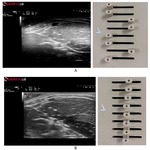
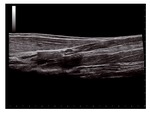
Bi-dimensional Panoramic Imaging
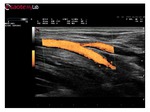
Panoramic imaging technology merges multiple B-Mode images into one complete panoramic image,
theoretically extending the echographic image field of view to the entire muscle (Figure 17).
The scanning is performed manually and graphical feedback indications give indirect qualitative information about the scan velocity needed to reconstruct the desired field of view and muscle portion.
Multiple options are usually available in Bi-Dimensional Panoramic Imaging,
such as:
• Auto fit of composite image
• Image Zoom
• Merge levels/realignment (in case of scanning mismatches)
• Frame markers
• Colorize
• Distance measurement
• Image saving
• Color Doppler capability
• Rotation/Pan/Zoom
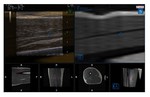
Volumetric imaging
Muscle echographic volumes can be automatically acquired with volumetric probes (also enabling 4D representations; i.e.
live continuous visualization of 3D real-time volumes),
which are useful for volumetric reconstructions of large muscle lesions (for diagnosis and follow up) and complex biopsy procedure guidance.
Simpler,
but also less geometrically precise,
volumetric acquisitions can be performed with traditional 2D transducers with 3D Freehand software reconstruction tools.
In this case,
similar to Bi-Dimensional Panoramic Imaging,
the third dimension is provided by slow movement of the transducer in the transverse direction (to the scanning plane).
Artifacts may be generated by inconstant speed of the probe movement.
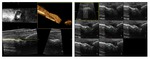
Additional management tools (Figure 18) for the acquired volume are Thick Slice Imaging (where a thick portion of the entire volume is visualized and managed separately) and Tomographic Mode Imaging (where multiple tomographic views can be selected within the acquired volume,
and visualized and managed separately).
Three-dimensional panoramic imaging
3D Panoramic imaging enables the acquisition of electromagnetically tracked Free hand muscle volumes with common 2D transducers.
Multiple volumes can be acquired and merged (Figure 19).
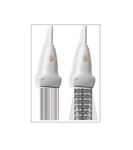
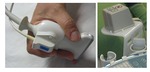
Real-time fusion of 3D and 2D US image data can be carried out during the US with an electromagnetic tracking system,
consisting of a transmitter in a fixed position and a small receiver attached to the US probe with a specific connector (Figure 20).
The scanning velocity during 3D panoramic acquisitions does not affect reconstruction,
as in conventional Free hand volumetric imaging (not electromagnetically tracked),
where the quality and dimension – length - of the final merged image is related to the acquisition scanning velocity.
CEUS – Contrast Enhanced Ultrasound Imaging
Ultrasound medium contrast imaging representation is related to the use of ultrasound contrast agents during diagnostic ultrasound.
Ultrasound contrast agents consist of microbubbles filled with a liquid containing gas which are injected through the vein into the system circulation.
The microbubbles contained in the contrast medium have high echogenicity: the difference in echogenicity between the microbubbles and the surrounding tissue is very high.
The technique of using contrast media to study the perfusion of an organ is performed at a low mechanical index (low MI) in order not to destroy the microbubbles,
even if intercepted by the ultrasound beam to examine the echo reflection.
High mechanical index imaging is used to deliberately break the bubbles in order to obtain an enhancement of the echo signal (Figure 21).
CEUS can be used for tissue perfusion examination,
as well as for pre-post treatment comparisons (regarding intervention procedures) and biopsy support in needle guidance for target detection.
Ultrasound physical principles and how to use them: DOPPLER
Doppler principles
In Diagnostic Ultrasonography,
Doppler indicates a technique used to measure blood flow,
based on the natural phenomenon studied by the Austrian physicist Christian Johann Doppler (1803-1853).
Doppler effect
The Doppler effect (or Doppler shift) is an apparent change in wave frequency perceived by a fixed observer with respect to a moving source of sound waves.
This effect is commonly heard when a vehicle sounding a siren or horn approaches,
passes,
and recedes from an observer: the frequency perceived is higher (than the actual frequency) during the approach,
it is accurate at the crossing point,
and lower as the vehicle recedes.
Apparent acoustic wave frequency modifications are related to the speed and direction of the vehicle.
Doppler effect in Diagnostic Ultrasound
In Diagnostic Ultrasound,
the wave is transmitted not by a moving object but by a fixed object (ultrasound probe).
In Diagnostic Ultrasound,
the echoes received from fixed tissues are at the same frequency as the transmitted beam.
If the echoes are generated by moving targets such as blood cells,
then the output and input frequencies will not be the same,
and the generated echo frequency will vary directly with the velocity and direction of the target movement.
The shift in frequency is used to determine the relative velocity and direction of the moving structures (blood cells).
The greater the frequency shift,
the higher the velocity of the moving object.
Movement toward the transducer results in a higher received frequency while movement away from the transducer will mean a lower received frequency.
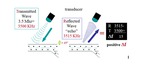
Doppler frequency (fd) formula (Figure 22):
fd= [2 * ft * V * cos (q)] * c
Where:
fd = Doppler frequency (called also Doppler shift)
ft = transmitted frequency
c = speed of sound in tissue
V = blood velocity
q = angle of incidence between ultrasound beam and direction of flow
A higher Doppler frequency is obtained if:
• the velocity is increased.
• the beam is more aligned to flow direction.
• a higher frequency is used.
The transmission and reception frequencies are in the ultrasound frequency range and therefore not audible (by a human being),
but the difference between them (fd = Doppler shift) is commonly in the kHz-domain range of acoustic frequencies,
which is within the audible range of sounds.
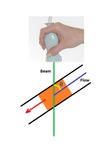
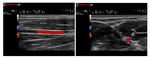
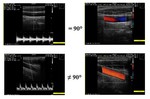
The ultrasound beam must never be perpendicular to the targeted flow,
otherwise no Doppler shift will be generated by the moving targets (Figure 23).
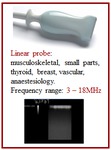
The linear probes allow electronic ultrasound beam steering during longitudinal scans (Figure 24).
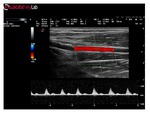
Pulsed Wave Doppler
In Pulsed Wave Doppler (PW),
Doppler shift data are selectively provided from a small segment of the ultrasound beam called the Sample Volume (SV).
PW performs an analysis of all the frequency variations,
giving a (quantitative) real-time representation of all velocities over time,
present in the blood flow detected by the SV (Figure 25): peak velocities can thus be differentiated from average and minimum velocities.
PW is enabled by positioning the SV on the vessel to be examined: a pulse is sent out from the transducer and the frequency shift in the reflected pulse is measured after a certain time.
Using the Doppler equation,
the echo information obtained within the SV is analyzed in terms of frequency shift and related amplitude,
enabling the blood flow velocity to be determined.
This process is repeated alternately through many transmit-receive cycles each second,
in order to obtain enough data to calculate the frequency components of the sampled volume.
The frequency data are converted to velocity and displayed in a scrolling text format on the monitor (spectrum).
The time interval between pulse emission and the receipt of its echo reflected from a moving blood cell determines the value of the Pulse Repetition Frequency (PRF; also known as Scale)
PW has the benefit of providing Doppler shift data,
for a selective SV,
along the ultrasound beam.
PW’s main limitation in terms of detectable Doppler shift is that the maximum Doppler shift (and therefore the related blood flow velocity) measurable in PW is limited to one half the sampling rate defined by the PRF (Nyquist limit),
which is mainly determined by the sampling depth
Color Doppler
Color Doppler combines the B-Mode image format and a bi-dimensional (qualitative) representation of blood flow in real time.
Color Doppler detects the velocity and direction of a flow in a similar manner to PW,
but the detection does not take place within a single SV,
but in several sample volumes at once.
The number of Color Doppler “sample volumes” depends on the number of lines where the measurements take place and the number of sample volumes along each line.
The number of lines,
limited by the transducer array width,
depends on the size of the sampled area (Color Box),
which is operator adjustable.
A color (within a selected Color Map) is assigned to the calculated velocity data to represent a certain velocity and direction,
then displayed in a Color Box that is super-imposed on the B-Mode image (Figure 26).
Color Doppler enables a visual overview of the blood flow distribution to be obtained,
in terms of direction and speed.
Color Doppler limitations are mainly related to the fact that it gives only qualitative information for the average velocity at a certain point in the Color Box.
PW & Color Doppler Conventions (Sign,
Color)
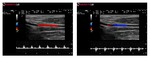
Due to a convention in Doppler signal representation,
Blood flows moving toward the transducer are shown as Positive in PW Doppler and Red in Color Doppler; flows moving away from the probe are shown as Negative in PW Doppler and Blue in Color Doppler (Figure 27; Figure 28).
Power Doppler
Power Doppler is a blood flow detection modality based on a concept similar to that of Color Doppler,
but instead of measuring the frequency difference between the emitted and received waves,
it considers the energy of the Doppler frequency.
Power Doppler is theoretically more sensitive than Color Doppler but it cannot distinguish the direction of movement of blood cells (Figure 29).
To overcome this limitation,
the Directional Power Doppler modality has been introduced,
which combines the sensitivity of Power Doppler with the typical flow direction discrimination of Color Doppler.
The color intensity of the Power Doppler signal corresponds to the number of detected moving red blood cells,
regardless of the direction and velocity of their flow.
Power Doppler is mainly used to study smaller and deeper vessels,
and vessels characterized by slow blood flow which cannot be well identified with Color Doppler.
Power Doppler is more sensitive than Color Doppler to movement artifacts.
Main Doppler Control Parameters
The main operator-dependent parameters that act directly on PW and the Color Doppler signal quality are as follows:
• Frequency - Doppler transmission frequency.
• PRF (Scale) - Pulse Repetition Frequency - repetition frequency of the transmitted ultrasound signal.
• θ - Doppler angle correction between the transmitted ultrasound beam and the targeted blood flow direction.
• Doppler insonation angle - in order to have a Doppler shift different to zero,
the insonation angle must not be perpendicular (90°).
• Doppler Gain - Gain of the received Doppler signal.
Transmission Frequency
High ultrasound transmission frequency increases sensitivity to small vessels and slow blood flows on superficial structures; while low ultrasound transmission frequency increases sensitivity to high velocity flows and to large and deep vessels.
PRF (Scale)
PRF is the number of times per second that the transducer transmits a pulse.
It is directly dependent on the transmission depth.
A sufficiently high PRF is a prerequisite for the detection of high velocities and superficial vessels.
The detection of slow flows and deeper vessels should preferably be performed with lower PRF.
The PRF should be as high as possible for the examination of elevated blood flow velocities; the maximum measurable velocity can be calculated by the following equation (Nyquist limit):
Vmax = PRF / 2
PRF Changes and related effects and detection characteristics
PW with Color Doppler elevated PRF generates a Doppler signal characterized by:
• Higher measurable velocities
• Lower sampling depth
• Higher Frame Rate
• Reduced aliasing
PW with Color Doppler low PRF generates a Doppler signal characterized by:
• Lower measurable velocities
• Deeper sampling depth
• Lower Frame Rate
• Increased aliasing (Figures 30 and 31)
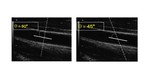
Doppler angle correction
The transmitted beam should be as parallel as possible to the examined blood flow,
in order to obtain the most accurate velocity.
The q Doppler angle correction is an angle value introduced within the Doppler shift formula to align the transmitted ultrasound signal with the direction of the examined blood flow as much as possible.
To obtain a reliable and repeatable Doppler signal detection result,
q needs to be between 15° and 60°.
q must never be equal to 90 ° in order to avoid the so-called “ Zero Doppler Effect”,
which means the PW Doppler spectrum is almost null or very disturbed,
and Color Doppler has very low representation (even in the presence of a technically detectable blood flow signal).
See Figure 32.
Doppler insonation angle
The Doppler insonation angle refers to the angle between the transmitted ultrasound signal and the direction of the examined blood flow.
For linear probes,
in a longitudinal scan,
an electronic beam steering function can be used to avoid perpendicular Doppler insonation angles (Figure 33).
Doppler Gain
If Doppler Gain is set too low,
it generates an under-estimate of the intensity of flows,
with a consequent loss of valuable information.
Conversely,
if it set too high,
it generates a noisy PW Doppler spectrum signal and a Color Doppler with an unreal color signal,
including in areas of the Color Box where no vessels are present (Figure 34).
Advanced Technologies
The following section describes some advanced imaging tools for guidance,
visualization and multimodal real-time fusion,
to show how to achieve an accurate real-time MUS using innovative practices.
Needle Enhancement
The safe and successful performance of ultrasound-guided procedures requires detailed knowledge of anatomy and an understanding of where the needle tip is at all times.
This relies on needle and transducer manipulation,
which can be a challenge,
especially for beginners.
Visualization of the needle tip requires alignment with the ultrasound beam,
which is not always achieved.
Even when it is,
the physical characteristics of the needle and technology limitations can obstruct visibility.
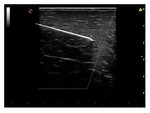
Needle Enhancement Technology makes the needle especially visible during angled needle insertions for various clinical procedures.
This technology is based on advanced imaging processing techniques,
together with optimized beam steering.
This combination makes the needle more clearly distinguishable from the surrounding tissue,
while maintaining the image quality of the target (Figure 35).
Virtual Biopsy
Virtual Biopsy is a technology developed to increase the operator confidence during Ultrasound Real-time biopsy procedures: the real needle is highlighted by the Virtual needle indication directly on the Real-time Ultrasound image with a proper 3D representation of the probe,
scanning plane,
needle in plane and off plane and path to the target (Figure 36).
Colored target over imposed on the area to be biopsied,
can be shown as well.
The needle path is visualized also before the insertion of the real needle in order to plan in advance the best path of insertion to avoid vessels and structures.
Virtual Biopsy technology is particularly useful for deep biopsies,
for complicated biopsies with difficult approach due to target location and during the biopsy learning curve of a novice operator.
Usual imaging and Doppler modalities (for instance Elastosonography,
Color Doppler,
Power Doppler) can be activated also when within the Virtual Biopsy environment.
A proper electromagnetic technology (same used for the 3D Panoramic tool) enables the real-time tracking of probe and needle.
Virtual Navigator for Multimodality Real-time Fusion Imaging
Virtual Navigator is a multimodality real-time fusion imaging technology that can be used to enhance real-time MUS with MRI acquisitions,
thereby supplementing MRI data with Diagnostic Ultrasound morphological (B-Mode) data,
hemodynamic (Color,
Power and Pulsed Wave Doppler) data and stiffness (Elastosonography) data.
These real-time ultrasound diagnostics and the highly detailed anatomical mages offered by MRI can be displayed in real time in a virtual space where the different imaging modes are merged and the ultrasound scanning plane spatial data is correlated with three-dimensional MRI volumes (Figure 37).
A proper electromagnetic tracking technology (same used for the 3D Panoramic tool ) enables Fusion Imaging Virtual Navigation between the ultrasound probe,
the second imaging modality and the needle/treatment instruments.
Visual comparison
Visual comparison tools enable side-by-side visualization of saved images and clips with real-time scanning.
This tool simplifies the repositioning of the probe in the target area during follow up scans.
It simplifies the monitoring of disease progression/treatment effects and can also be a valuable teaching tool.
Tips and Tricks
Procedural details are illustrated in the following section in order to avoid the most common pitfalls and allow data from different studies to be compared.
Excessive compression
Excessive muscle compression by the probe while scanning can create image distortions in terms of geometrical relationships between the tissue and possible lesions.
The correct amount of gel is necessary to ensure effective coupling between the transducer and the patient’s skin (Figure 38).
Using an adequate amount of gel
A sufficient amount of gel use ensures effective probe-skin matching.
This avoids echo image black cones and image homogeneity throughout the whole field of view (Figure 39).
The presence of air bubbles in the gel placed on the patient’s skin can create artifacts which may be visible locally as potential calcifications (Figure 40).
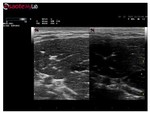
Insonation angle
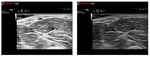
The insonation angle is of paramount importance for accurate and repeatable MUS scanning.
MUS echo images are dramatically altered when the probe insonation angle varies,
simply by tilting the probe over the examined muscle,
both for diagnosis and follow up.
The inter and intra MUS operator variability for scanning techniques and probe handling/positioning is of major importance and must be standardized to ensure repeatability (Figure 41).
Correct system set up (Imaging parameters,
General Gain and TGC)
A good technical understanding of ultrasound physics is vital for accurate MUS imaging.
Particularly for the purpose of follow-up activities,
the system must always be configured in the same way,
with particular attention paid to both system parameters and scanning technique.
Automatic Adjustment
An automatic adjustment tool enables automated and operator-independent image and PW Doppler signal optimization.
Regarding B-Mode imaging,
the tool optimizes image quality through adjustments of the image histogram,
based on an optimized image database present within the system,
as well as setting general gain and Time Gain Compensation in order to ensure image homogeneity and readability.
Automatic adjustment of PW optimizes gain,
baseline and PRF (scale) in order to accurately visualize the full Doppler trace for the examined vessel.