Keywords:
Extremities, Musculoskeletal bone, Professional issues, Plain radiographic studies, Education, Education and training
Authors:
L. Nelson1, P. Smalley1, J. Harris2; 1Salford/UK, 2Manchester/UK
DOI:
10.1594/essr2017/P-0198
Conclusion
There is very little,
if at all,
in the literature about artefact caused by dressings on X-ray and its significance,
except in the education of radiographers,
where key texts reccommend removal of dressings.8 Many instruction leaflets for silver containing dressings advise a patient to remove these prior to MRI for safety reasons,9 but this fear has been allayed in a recent study stating this is not necessary.10
Dressings containing silver compounds particularly seem to obscure X-ray imaging in our study and this has implications for clinical practice.
Although initially we felt that only those dressings containing such radio-opaque compounds would obscure the images,
it appears that any dressing has the ability to do this,
with the most likely ones being those containing silver,
those with densely packed fibres designed to sit inside ulcers and those impregnated with antimicrobial fluids.
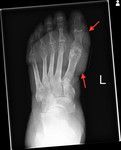
As can be seen in figure 17,
an anterior view of the left foot,
the dressing here obscures the bone of the left 1st metastarsal and proximal phalanx.
The arrows delineate the boundaries of the dressing.
In a foot with pathological bone changes such as osteoporosis,
such as this one,
it can be appreciated how the subtle early changes of osteomyelitis may be missed,
especially between dressing changes between surveillance.
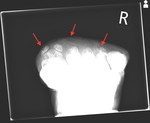
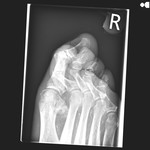
On plantar oblique imaging of the right foot the dressing overlying in figure 18 is clearly seen superiorly delineated by the arrows in this windowed view.
Our study was limited in certain ways.
First of all,
we used a hand to model our patients' feet which had none of the associated bone pathology mentioned and also the bones were not osteopenic nor osteoporotic.
The normal density could make it difficult to appreciate any problem created by a dressing obscurring the imaging.
Secondly,
we were not able to mimic clinical conditions such as blood products or wound exudate soaking the dressing,
adding to the artefact.
In conclusion,
we have shown how artefact caused by a simple dressing on a diabetic foot ulcer may have implications for the correct diagnosis and surveillance of bone pathology and in particular osteomyelitis.
We have shown pictorially the effect this can have on real life cases and in our model with suggestions of certain dressings causing this.
Since there does not appear to be a particular quality to a dressing which predicts this effect,
we recommend all dressings are temporarily removed during X-ray in such patients and suggest this should also be described in the instruction leaflets for such dressings.