Introduction
The calcaneus may be affected by acquired and congenital disorders.
Multiple pathologies may arise in the calcaneus and include traumatic,
infectious,
haematological,
neoplastic and other secondary disorders which affect the calcaneus indirectly.
In some cases,
the location of certain pathologies within the calcaneus and their radiographic may be diagnostic [1].
A review of 66 cases of tumour and tumour-like calcaneal lesions was performed together with a review of the literature in order to develop a diagnostic algorithm for the more commonly encountered calcaneal lesions.
Anatomy
The calcaneus is the first tarsal bone to ossify and is the only tarsal bone to have a secondary epiphysis [2].
The development of the calcaneus parallels the osteogenesis seen in long bones [3].
The calcaneus may be divided into epiphyseal,
metaphyseal and diaphyseal equivalents [4].
The calcaneus has six surfaces and is roughly cuboidal in shape [1]:
- Superior surface: has anterior,
middle,
and posterior facets for articulation with the talus
- Plantar surface: tuberosity along its posterior aspect
- Lateral surface: bony prominence for attachment of the calcaneofibular ligament
- Medial surface: extends anteriorly as the sustentaculum tali
- Anterior surface: articulates with the cuboid
- Posterior surface: for insertion of the Achilles tendon
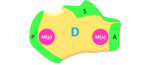
These surfaces correspond to the different epiphyses [5] (Figure 1):
The superior epiphysis - corresponds to the superior surface of the calcaneus
The anterior epiphysis- confluent with the anterior surface of the calcaneus and articulates with the cuboid
The posterior epiphysis – equivalent of the posterior surface where the Achilles tendon inserts

Fig. 1: Schematic diagram of the calcaneus demonstrating the three epiphyses (green): posterior (P), superior (S), anterior (S), diaphysis (D) and anterior (a) and posterior (p) metaphyses (M) (pink)
References: A. Vidoni
The diaphysis comprises the body of the calcaneus and the anterior and posterior metaphyses bridge the anterior and posterior epiphyses to the diaphysis respectively.
Vascular supply
The blood supply of calcaneus is derived from medial and lateral calcaneal arteries [3].
The posterior aspect of the calcaneus near the cartilage plate has an extensive blood supply and is considered comparable to the metaphysis in long bones [4].
Location
The existing literature is limited with only two location-specific small case series of the calcaneus.
The majority comprise individual case reports describing specific osseous lesions and their treatment [6].
The evaluation of lesions in the calcaneus can be considered analogous to the evaluation of lesions in long bones with an epiphysis,
metaphysis and diaphysis.
The calcaneus may be considered to have three epiphyses: superior,
anterior and posterior.
Patients and method:
We retrospectively reviewed the imaging of all 66 patients with tumours or tumour-like conditions of the calcaneus from the database of a tertiary referral Orthopaedic centre excluding those patients before 2007 due to lack of availability of imaging on PACS.
This cohort of patients was obtained after filtering through a search for calcaneal lesions which resulted in 174 cases.
Only 66 of these were true calcaneal lesions.
All primary tumours of the calcaneus were included together with non neoplastic conditions such as infection.
The imaging reviewed was based on plain radiographs with MRI correlation in some cases.
Results:
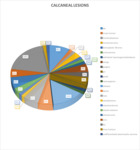
23 different pathologies were identified and ranged from common pathologies such as intra-osseous lipomas and simple bone cysts to more esoteric lesions such as epithelioid haemangioma (Figure 2).

Fig. 2: Pie chart demonstrating the percentage of different calcaneal lesions in our patient group
References: C. Azzopardi
Some of these lesions showed a predilection for certain locations within the calcaneus.
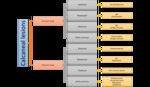
Based on a review of the literature and the cases from a tertiary orthopaedic centre a flowchart demonstrating the frequency of certain lesions within different parts of the calcaneus was formulated (Figure 3).

Fig. 3: Flow chart suggesting the diagnosis of calcaneal lesions based on patient age and location of the lesion within the calcaneus
References: C. Azzopardi
Lesions with an unpredictable location were not included in the diagnostic flowchart.
Discussion:
Epiphyseal lesions
Chondroblastoma (Figure 4)
Chondroblastoma occurs in tarsal bones in 6 to 7% of cases and is observed more commonly in the calcaneus [4,
7].
It generally arises in the superior epiphysis adjacent to the talocalcaneal articulation.
The epiphyseal location of chondroblastoma is however quite typical,
joint involvement,
however,
is rare.
It is typically a lucent lesion with marginal sclerosis.
Internal calcifications can be seen in 40-60% of cases [8,
9].
Adjacent periosteal reaction,
erosion or soft tissue mass is a cause for concern and indicates possible malignancy.
A differential diagnosis based on plain radiographs includes giant cell tumour and aneurysmal bone cyst [7].
MR signal characteristics are typical of cartilage.
MR is also helpful to evaluate spread across the physis or transcortical extension.
Surrounding bone marrow and soft tissue oedema is often observed [9,10].
Chondroblastomas may be difficult to eradicate surgically in view of their epiphyseal location and proximity to the articular cartilage which may result in growth disturbances.
An alternative primary treatment for chondroblastoma is focused radio-frequency heat ablation [9].

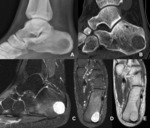
Fig. 4: Image A: Plain radiograph demonstrates a well defined lytic lesion in the posterior epiphysis
Image B: Sagittal CT reconstruction confirms a well defined osteolytic lesion in the posterior epiphysis
Image C: Sagittal STIR
Image D: Axial STIR
Image E: Axial T1
MR images show a lesion with an epiphyseal location and typical surrounding inflammatory oedema
Osteoid osteoma:
10% of osteoid osteomas occur in the bones of the foot,
with 2% to 3% of them occurring in the calcaneus [11].
The talus is the most common site for osteoid osteoma comprising 30% of lesions occurring in the foot.
Most of the lesions in the calcaneus occur adjacent to the talocalcaneal articulation and are epiphyseal in nature [4].
Plain radiographs often show sclerotic thickening of the bone with a radiolucent nidus.
The nidus may,
however,
not appear on x-ray.
In a juxta-articular location osteoid osteoma may cause reactive synovitis and simulate arthritis without periostitis [12].
A bone scan can be performed to verify the diagnosis in those patients with a high index of suspicion.
Computerized tomography is done to confirm the location of the lesion and aid the surgical approach [11].
Computed tomography-guided percutaneous techniques have been used to achieve ablation of the nidus with minimal tissue invasion especially in areas which may be hard to access surgically such as the calcaneus [12].
Metaphyseal lesions
Aneurysmal bone cyst (Figure 5):
The calcaneus is a rare location for an aneurysmal bone cyst (ABC),
comprising only 1.6% of the cases [13].
In long bones 60% percent originate from metaphyses,
while 28% originate from the meta-epiphyseal and subchondral parts.
ABC arising secondary to chondroblastoma typically affects the epiphysis [14]. ABCs may sometimes extend throughout the entire calcaneus or extend to the epiphysis across an open cartilage plate [15].
In view of this variability there is no specific location pattern for ABC in the calcaneus although most appear in the posterior half and in our cohort of patients they appeared to be mainly epiphyseal or meta-epiphyseal.
MR imaging typically shows a well-defined lesion with internal septations.
Multiple fluid-fluid levels may be seen [16].
Osteomyelitis (Figure 6):
The calcaneus has an apophysis,
the equivalent to the metaphyseal region of long bones.
This region is vulnerable to haematogenous infection [17].
The calcaneus may be involved by infection via various routes [4]:
· haematogenous route
· penetrating injury
· secondary to soft tissue infection
Most cases of haematogenous osteomyelitis begin in the posterior meta-epiphyseal region.
Infection may spread across the cartilage plate to involve the nearby apophyses [4].
This therefore means that prompt treatment in calcaneal osteomyelitis is essential as it may lead to growth plate disturbances,
with secondary growth arrest and deformity.
It may also spread into the body of the calcaneus and occasionally may involve the whole of the calcaneus [4].

Fig. 6: Image A: Radiograph demonstrating a mixed lytic/sclerotic lesion arising from the posterior aspect of the calcaneus typical of osteomyelitis
Image B: Sagittal CT reconstruction
Image C: Axial CT
Images confirm the X-ray findings
Metastases (Figure 7):
Metastases to the tarsal bones occurs most frequently from colon,
kidney or lung primaries with the genitourinary system and the colon accounting for more than half of the reported metastases to the foot [18].
28% of metastases occur in the posterior calcaneus since the posterior aspect of the calcaneus is richly vascularised [18,
4]. Metastases tend to occur in the metaphyseal region but may extend into the diaphysis.
All the cases in our cohort of patients who presented with calcaneal metastases were above the age of 20.
Giant Cell Tumour:
The prevalence of giant cell tumour (GCT) of the calcaneus is less than 2% [19].
It occurs in patients with a closed physis and in our group of patients all the patients with a GCT were above the age of 20.
It is metaphyseal in location in tubular bones with extension into the epiphysis or diaphysis.
In the calcaneus GCT tends to occur more commonly in the posterior metaphysis with extension into the epiphysis or diaphysis.
It may also occur anteriorly [4].
Radiographically GCT presents as a well defined lesion with a non sclerotic margin.
Diaphyseal lesions
SBC (Figure 8):
The typical location of simple bone cysts in the calcaneus is diaphyseal,
specifically in the inferolateral aspect of the anterior third of the calcaneus [20].
This area is called the pseudocystic triangle [3].
The diagnosis is made based on radiographic findings which are often diagnostic when in the typical location.
Findings are of a lytic,
well defined lesion with a sclerotic margin [21].
The main differential diagnosis is lipoma which also typically occurs in the anterior third to mid-portion of the calcaneus.
MR imaging demonstrates homogenous low signal intensity on T1 weighted images and high signal intensity on T2 weighted images.
A lipoma on the other hand is isointense to fat on all sequences [22].

Fig. 8: Simple bone cyst. Typical site and MRI appearances for this benign lesion.
Intra-osseous lipoma (Figure 9,10):
Intra-osseous lipomas involve the calcaneus in 30% of cases.
In our cases the patient age group was older than 20 years of age.
Their location is typically in the antero-inferior aspect of the calcaneal diaphysis.
The radiographic appearances consist of a well circumscribed radiolucent lesion with a rim of sclerosis.
Intra-lesional calcification may be present this represents areas of fat necrosis.
MRI confirms the fat component of the lesion [23].

Fig. 9: Intraosseous lipoma of the calcaneus. The central dystrophic calcification is typical and, if present, helps to distinguish this lesion from a bone cyst.
Ewing’s sarcoma:
Ewing’s sarcoma of the foot is rare and occurs most commonly in the calcaneus.
It may be misdiagnosed as osteomyelitis in the foot as it may have a similarly aggressive appearance [24].
In the calcaneus,
however,
osteomyelitis usually develops posteriorly near the cartilage plate whilst Ewing’s may occur anywhere but is mainly diaphyseal and may involve the whole of the calcaneus [4].
Entire calcaneus
Chondrosarcoma (Figure 11):
Chondrosarcoma of the calcaneus is rare accounting for 0.5–2.97% of all chondrosarcomas of other sites [25].
Whilst chondrosarcoma is usually centrally placed in tubular bones,
there is no typical location pattern for chondrosarcoma in the calcaneus.
In the two cases we observed,
the tumour was seen to involve the whole of the calcaneus.
Chondrosarcoma is usually slow growing but generally appears as an aggressive osteolytic lesion radiographically.
Punctate calcification may be seen in the tumour matrix [4].

Fig. 11: Axial and coronal T1 weighted MR images of the calcaneus involving most of the calcaneal diaphysis. Hypointense foci correspond to punctate calcifications in the tumour matrix. Histologically proven chondrosarcoma.
Osteosarcoma (Figure 12):
The most commonly involved tarsal bone is the calcaneus,
however,
overall osteosarcoma of the foot is rare with an incidence of 0.2-2% of all osteosarcomas.
Osteosarcoma in the foot tends to have a predilection for older patients.
This observation was made by Biscaglia et al.
(1998) [26].
The reported subtypes of calcaneus osteosarcomas include conventional osteosarcoma,
low-grade central osteosarcoma,
telangiectatic osteosarcoma,
periosteal osteosarcoma and small- cell osteosarcoma.
There is no specific location for osteosarcoma in the calcaneus,
however,
in the four cases we present the tumour is seen to involve the whole of the calcaneus.
Lymphoma:
Primary Non-Hodgkin’s lymphoma of the bone is rare and accounts for less than 2% of all lymphomas in adults.
In 92% of cases patients are over the age of thirty.
Involvement of the calcaneus is rare.
It does not have a specific location and tends to involve all of the calcaneus [27].
Radiographically an osteolytic lesion with ill-defined margins is often present with cortical breaks and soft tissue components.
Alternatively,
the lesion may be completely sclerotic.
Overall imaging findings are those of an aggressive lesion,
although a periosteal reaction is uncommon [1].