The common peroneal nerve (CPN) is a frequent site of focal neuropathy of the lower limbs.
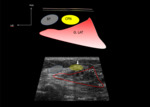
ANATOMY (Fig. 1
CPN is the lateral branch of division of the sciatic nerve at the level of the popliteal fossa.
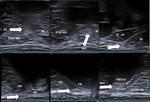
Main landmarks used for ultrasound are (Fig. 2):
- medially: the lateral head of the gastrocnemius muscle
- laterally: biceps femoris tendon
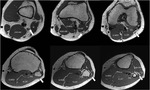
The CPN then courses around the neck of the fibula just beneath the proximal aspect of the peroneus longus tendon: this is the fibular tunnel (Fig. 3 .
and Fig. 4)
The superficial and deep peroneal nerve innerve the lateral and anterior muscles of the leg (tibialis anterior,
extensor digitorum longus,
extensor hallucis longus,
peroneus brevis and peroneus longus) and are responsible of eversion and dorsiflexion of the foot.
The corresponding sensory area is the antoerolateral aspect of the leg and foot,
the deep peroneal nerve providing cutaneous innervation to the webbing between the first and second digits.
AETIOLOGY
Causes of CPN neuropathy can be divided in 3 main catergories:
A/ Postural,
microtraumatic or conflictual
- Prolonged compression following loss of consciousness (coma,
alcohol or drug abuse)
- Prolonged or repetitive position at work or during sport with flexed knees or crossed legs (yoga,
strawberry pickers palsy,
prolonged squatting...)
- Intraoperative malposition during colorectal,
gynecologic,
urologic,
and joint surgery.
- Fabella: small sesamoïd bone embedded in the tendon of the lateral head of the gastrocnemius muscle, reportedly occur in up to 30% patients.
Depending on the size and the topography of the fabella,
it can be in close contact with the nerve.
- Fibular tunnel syndrome: In 1989,
Leach et al.,
have described eight patients presenting with CPN palsy during running activity.
Surgery releasing the nerve around the fibula solved the symptoms.
- Other anatomic variations that can interfere with CPN have been described.
B/ Traumatic
- Direct: weapon wound,
postoperative after knee surgery,
hit
- Secondary to fibula neck fractures,
knee luxation...
- Repetitive ankle sprain or ankle instability
C/ Tumoral
- The main tumoral cause are ganglion cysts secondary to degenerative proximal tibiofibular joint.
These cysts are more frequently extrinsec to the nerve and are responsible of the compression.
Although relatively rare,
ganglia originating from the proximal tibiofibular might be intraneural (coursing along the articular branch of the nerve to pass from a joint capsular defect into the nerve).
- Other extrinsec compression causes may be variable: tug lesions,
exostosis,
lipoma...
- Intraneural: Post-traumatic nevroma,
schwannoma and neurofibromas
Electrodiagnostic tests are useful to confirm the diagnosis,
they might provide localizing information to the region of the fibular head and are posssibly useful tin providing prognostic information with regard to recovery of nerve function.