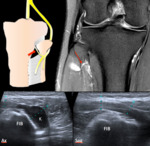
Standard knee x-ray must be performed before any ultrasound procedure:
Proximal tibiofibular joint osteoarthritis,
tumor of the fibular head and presence of fabella must be assessed.
Prior to the ultrasound exam,
it is also essential to get full medical history of the patient to look for occupationnal or microtraumatic causes,
prior trauma or surgery.
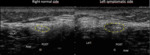
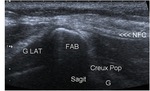
NORMAL ULTRASOUND FINDINGS (Fig. 5 and Fig. 6)
For an optimal resolution,
a high-end ultrasound unit equipped with a high-resolution broadband linear-array probe and corresponding soft-tissue software are necessary.
CPN is similar to other peripheral nerves on ultrasound exam:
- On short-axis planes,
US demonstrates CPN as honeycomb-like structure composed of hypoechoic spots embedded in a hyperechoic background in which the hypoechoic structures correspond to the fascicles that run longitudinally within the nerve,
and the hyperechoic background relates to the interfascicular epineurium.
- On long-axis planes,
nerves typically assume an elongated appearance with multiple hypoechoic parallel linear areas,
which correspond to the neuronal fascicles that run longitudinally within the nerve,
separated by hyperechoic bands
Measurements in healthy volunteers reported a mean cross-sectional of the nerve from 11 to 12 mm2 but in everyday practice comparison with controlateral asymptomatic nerve is more useful.
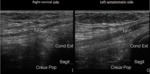
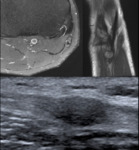
PATHOLOGICAL ULTRASOUND FINDINGS (Fig. 5 and Fig. 6
- Nerve swelling on short- and long axis planes compared to asymptomatic side although it might be more difficulte on long-axis plane (tortuous course of the nerve).
- Loss of fascicular echotexture and global hypoechogenicity of the nerve on axial and longitudinal planes,
compared to asymptomatic side.
As the the findings might be subtle,
the exam must be bilateral to increase confidence in the diagnosis.
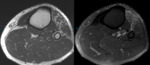
At chronic phase,
there might be an increased echogenicity of innervated muscles of anterior and lateral side of the leg secondary to fatty degeneration in chronic denervated muscles (Fig. 7 and Fig. 8).
It must be kept in mind that a normal ultrasound exam does not exclude the diagnosis and that a CPN neuropathy confirmed with electrodiagnostic tests can look normal on ultrasound; some authors stated that it might be of good prognosis value with regards to recovery.
ETIOLOGY
The second step of the ultrasound exam is to look for the cause.
Ultrasound is especially useful for tumoral causes.
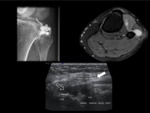
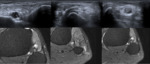
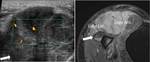
Extrinsec ganglion cysts (Fig. 9) originating from the proximal tibiofibular joint,
(the most frequent tumoral cause),
are frequently easily recognised as well-circumscribed anechoic masses.
Demonstrating a stalk connecting the ganglion with the superior tibiofibular joint might increase confidence in the diagnosis when the cyst does not have the typical appearance (thick and irregular echogenic wall or septations).
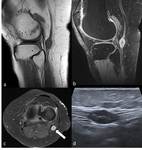
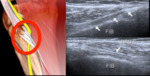
Intraneural ganglion cysts: They appear as intraneural cystic masses causing displacement of the fascicles and fusiform thickening of the nerve. The ganglions have a long tubular process reflecting the articular branch,
which joins the peroneal nerve on the posterolateral
aspect of the fibula (Fig. 10 and Fig. 11).
Traumatic neuromas and benign nerve sheath tumors (schwannomas and neurofibromas) appear as fusiform swelling of the nerve with both ends connected to proximal and distal normal nerve.
Eccentric location of the swelling and cystic changes are indicative of schwannoma; other subtle ultrasound features have been reported to help differentiate between schwannomas and neurofibromas but it still might be difficult in everyday practice (Fig. 12 and Fig. 13 .
Relationship of the nerve to adjacent bony structures must be studied carefully with comparison to controlateral asymptomatic side to detect a conflict with an exostosis,
a bone callus or a fabella.
Some authors stressed the importance of manual palpation of the nerve or palpation with the US transducer to reproduce the patient's pain and irradiation when the nerve exhibes a normal sonographic appearance (Fig. 14).
There is a wide variety of possible other compressive tumors and,
correlated to the MR exam,
ultrasound can help to describe close contact between the mass and the tumor,
sometimes on dynamic studies.
It might also demonstrate subtle changes in the size and echostructure of the nerve.
In any dubious situation,
histologic correlation with be helpful and ultrasound will help to guide the needle during biopsy (Fig. 15).
Other causes,
microtraumatic or conflictual might be more difficult to detect. The diagnosis must be suggested when nerve swelling is located at the level of the fibular tunnel (Fig. 16) without tumoral cause,
or if comparative ultrasound show asymetry between the symptomatic and asymptomatic side (muscle hypertrophy or anatomic variant) .
DIFFERENTIAL DIAGNOSIS
Every patient with pain of anterolateral side of the leg and foot drop does not have CPN neuropathy.
DOMS (Delayed Onset Muscular Soreness) lesion: Patients presenting with pain and stiffness in muscles from hours to to days after unaccustomed or strenuous exercise.
Hyperechogenicty of the muscle can mimic fatty degeneration in chronic denervated muscle but muscle hypertrophy,
the recent onset of symptoms and quick recovery help to make the correct diagnosis (Fig. 18.
Chronic compartment syndrome: It might be difficult to differentiate these two entities ,
especially in young athletic patients.
Concomittent CPN neuropathy and compartment syndrome has even been reported.
Compartment pressure measurement is the gold standard for the diagnosis.
US-GUIDED INJECTION
Ultrasound might also be helpful to guide local anesthetic or corticosteroid injection at the site of neuropathy, the relief of symptoms after injection being another argument to confirm the initial diagnosis.