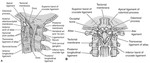
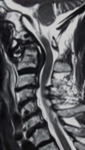
Three characteristic patterns of subluxation have been described :
• Atlanto axial subluxation
• Cranial settling
• Subaxial subluxation
Atlanto axial subluxation is the most common deformity.
It results from laxity of the primary and secondary ligamentous restraints.
Cranial settling results from occipito atlanto axial erosion and may lead to brainstem compression.
Subaxial cervical subluxation occurs secondary to combined destruction of disco vertebral complex and facet joints.
It may appear as an isolated deformity or affect multiple levels
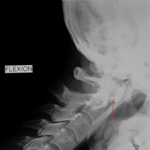
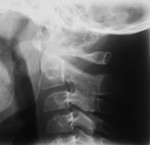
Radiographs (lateral flexion / extension dynamic views) should be performed routinely to establish whether instability is fixed or reducible
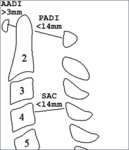
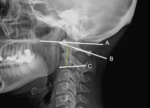
Extent of atlanto axoidal subluxation is assessed by the anterior or posterior atlanto dental interval (AADI,
PADI) (Fig 2,
Fig 3,
Fig 4)
•AADI is the distance from the posterior margin of the ring of C1 to the anterior surface of the odontoïd.
Normal value in an adult is less than 3 mm
The AADI poorly correlates with risk of neurological deficit
•PADI is the distance from the posterior aspect of the odontoïd to the anterior edge of the posterior ring of the atlas
•PADI is a more reliable predictor of neurologic deficit
CRANIAL SETTLING
Several measurements are used to quantify the extent of cranial settling,
the most commonest are: Mc Rae,
Mc Gregor,
Chamberlain,
Redlund,
Johnell
No single measure has a high sensitivity or specificity.
A combination of measurements has the greatest predictive power ( Fig 5)
SUBAXIAL SUBLUXATION : Subaxial subluxation may be measured in mm
A sagittal diameter of 14 mm or less better correlates with the presence of myelopathy
Evaluation of plain radiographs is often difficult.
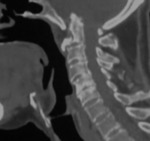
CT is particularly useful to determine the amount of cranial settling and to measure PADI and AADI values ( Fig 6,Fig 7,
Fig 8)
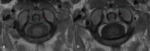
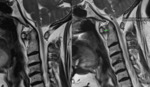
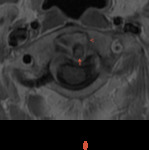
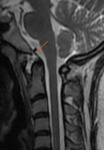
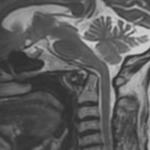
MRI provides explicit information of soft tissue lesions,
the neuraxis and epidural tissues (Fig 9- 15) .
It is a modality of choice in determining neural compression
Anatomical structures can be visualised in all planes,
without bone artifacts
MRI can demonstrate cord compression due to bone as well as soft tissue mass. A cord diameter of 6 mm in flexion is consistent with neurological deficits
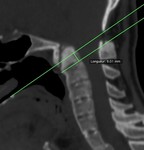
The cervicomedullary angle is the angle between a line drawn along the anterior aspect of the cervical cord and another line along the medulla (Normal angle: 135° - 175°)
IMAGING PREDICTORS OF PARALYSIS
•PADI of less than 14 mm
•Combination of AAS with cranial settling
•Subaxial cranial diameter of less than 14 mm
•Cervicomdullary angle of less than 135°
•Cord diameter in flexion of less than 6 mm
•Subaxial anterior subluxation