Embryology:
Human spine development commences during embryogenesis and lasts until the age of thirty.
It occurs in four overlapping stages:
1.
Mesenchymal stage: The notochord forms in the 3rd gestational week and its role is to induce ectodermal and mesodermal differentiation resulting in formation of the neural plate,
which folds to form the neural tube.
It determines the spinal axis and contributes to the formation of the nucleus pulposus of the intervertebral disks.
Notochord cell remnants have been described in the cranial and caudal portions of the spinal axis,
which explains the high prevalence of chordomas in these locations.
The paraxial mesoderm will be segmented in 42-44 somites by the end of the 5th gestational week.
Each somite consists of three cell elements: the sclerotome or future vertebra,
the myotome,
and the dermatome.
The adjacent halves of two contiguous somites contribute to one vertebra during formation of the membranous vertebral column
2.
Chondrification is initiated in the 5th gestational week and results in a cartilaginous vertebral column.
3.
Primary or enchondral ossification occurs in three primary ossification centers:
a. Central: forms the midportion of the vertebral body.
b.
Bilateral neural ossification centers contribute to the neural arch and the posterolateral vertebral.
c. Costal ossification centers form a portion of the lateral mass.
A total of six centers produce the sacral alae.
4.
With secondary ossification, two epiphyseal plates provide accessory ossification to the superior and inferior portions of each sacral vertebral body.
Disks separate the sacral vertebrae during childhood,
fusing progressively until the 3rd decade of life.
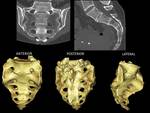
Anatomy: Fig. 32
The sacrum is a large inverted triangular shaped bone and has a concave anterior or pelvic surface and a convex posterior outer surface.
It is located in the caudal aspect of the spinal axis between articulating superiorly with L5,
inferiorly with the coccyx,
and bilaterally with the iliac bones at the sacroiliac joints.
It consists of five vertebrae (named S1,
S2,
S3,
S4 and S5) fused both anteriorly and posteriorly.
Posteriorly,
the fused spinous processes form the median sacral crest,
which extends caudally to the sacral hiatus.
The sacral hiatus is a defect in the posterior wall of the sacrum at the S5 level.
The sacral canal is the caudal continuation of the lumbar spinal canal containing the meninges,
the lower portion of the cauda equina (sacral and coccygeal nerve roots),
the filum terminale,
and fibrous and fatty tissue.
The epidural space terminates at the sacral hiatus.
S1 is the largest and the strongest of the sacral vertebral bodies which contains the greatest density of trabeculae arranged in a cruciate pattern designed to provide support during axial loading.
The prominent anterosuperior lip of bone is the sacral promontory.
The sacral ala is the wing-shaped bone found lateral to this vertebral body with decreased trabecular density; that is why sacral insufficiency fractures occur in this location.
Four pairs of foramina with openings on the anterior and posterior surfaces of the sacrum transmit the ventral and dorsal rami of the sacral nerve roots (S1–S4),
respectively.
The lateral masses are paired blocks of bone located lateral to the sacral foramina.
Due to its anatomy,
relationships with other bones or cavities and the variety of components a wide range of disease processes can involve the sacrum.
We are going to focus on tumoral sacral bone disease.
NEOPLASTIC LESIONS
The most common sacral neoplasm is metastatic disease,
followed by multiple myeloma and lymphoma.
Primary neoplasms of the sacrum are infrequent and account for fewer than 7% of all intraspinal primary tumors.
|
Benign
|
Malignant
|
|
Giant cell tumor
Aneurysmal bone cyst
Hemangioma/vascular lesions
Osteoid osteoma /Osteoblastoma
Osteochondroma
Lipoma
Chondromyxoid fibroma
Bone island/
Teratoma
Benign notochordal cell tumor
|
Metastases
Multiple myeloma
Lymphoma
Leukemia
Chordoma
Chondrosarcoma
Ewing sarcoma
Fibrosarcoma
Osteosarcoma
Primitive neuroectodermal tumor
|
Sacral tumors diagnosis is often delayed due to its capability to accommodate large masses before becoming symptomatic.
Only when compress adjacent structures as neural roots or pelvic organs clinical manifestations appear.
Symptoms are nonspecific,
including low back pain,
palpable mass and neurological deficits.
Plain radiographs,
are usually insensitive for the evaluation of this complex region,
should always be carefully scrutinized by all radiologists to minimize diagnostic delays.
The purpose of cross-sectional imaging (CT and MR) is to define the anatomical localization,
extent,
and radiologic features contributing to the correct diagnosis and facilitating treatment planning.
Although the differential diagnosis for a sacral tumor is extensive,
various primary neoplasms have characteristic features on CT scans and MR imaging that may aid in making a diagnosis.
However image guided biopsy is often required.