Keywords:
Arthritides, Education, Conventional radiography, Musculoskeletal system, Musculoskeletal joint, Musculoskeletal bone
Authors:
H. D. Peiris, C. Lord, V. T. Skiadas, M. Sampson; Southampton/UK
DOI:
10.1594/essr2017/P-0276
Imaging findings OR Procedure Details
IMAGING FINDINGS
Alignment
1. Joint deformities
- Subluxation or dislocation e.g.
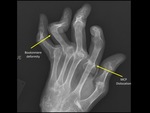
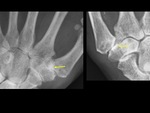
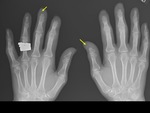
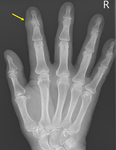
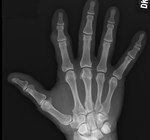
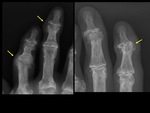
Boutonniere deformity - RA (Fig. 1),
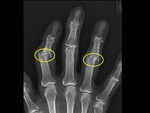
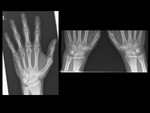
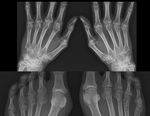
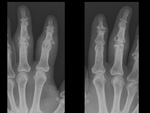
lateral subluxation ( Fig. 2 ) in OA,
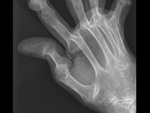
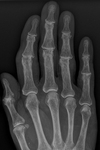
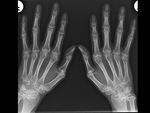
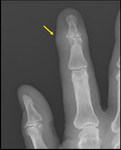
Z-deformity in RA ( Fig. 3 ),
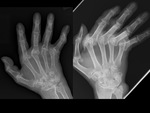
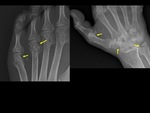
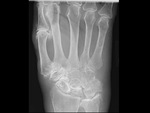
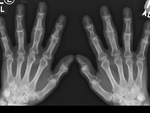
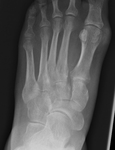
ulnar deviation ( mainly MCP joints) ( Fig. 4 ) in inflammatory arthritis,
swan-neck deformity with PIP hyperextension and DIP flexion (fig.5)
- In patients with SLE joint MCP joints ulnar deviation is not associated with erosive changes,
as in rheumatoid arthritis (fig 37)
Bone changes
1. Mineralisation
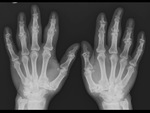
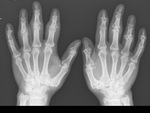
- Normal mineralisation in all arthritides apart from RA ( Fig. 5 )
- Regional/diffuse osteoporosis – RA ( Fig. 6 )
- Periarticular osteoporosis – RA.
Please note that this feature is depended strongly on technical factors and it can be subjective.
2. Bone formation
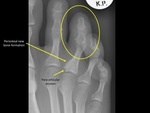
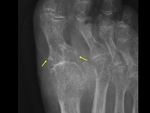
- Periosteal new bone formation ( Fig. 7 ) – seronegative spondyloarthropathies like psoriatic arthritis.
- Diffuse increased osteopenia,
not commom in psoriatic arthritis.
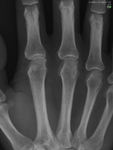
- Marginal osteophytosis ( Fig. 8 ) – OA
- Subchondral sclerosis ( Fig. 9 ) – OA
- Periarticular overhanging edges ( Fig. 10 ) – Gout
- Syndesmophytes – ankylosing spondylitis and other inflammatory arthropathies
3. Bone destruction/erosions
a. Active vs Non-active
- Rheumatoid arthritis,
psoriatic arthropathy,
gout,
CPPD – non-aggressive with sclerotic borders ( Fig. 11 ) or aggressive with no sclerosis ( Fig. 12 )
- Osteoarthritis – non-aggressive,
subchondral cysts (fig.16)
b. Location of erosions
- Joint margins (para-articular) – inflammatory erosions e.g.
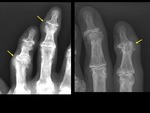
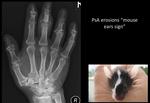
psoriatic arthropathy (‘mouse ears’) ( Fig. 13 ),
- Long standing erosive changes in psoriatic arthritis giving a “pencil-in-cup” deformity of a joint ( Fig. 14 )
- Central – erosive osteoarthritis (‘sea-gull/gull-wing’) ( Fig. 15 )
- Peri-articular erosions in gout ( Fig. 16 )
- Acro-osteolysis in scleroderma ( Fig. 17 )
Cartilage (Joint space changes)
- Preserved joint space ( Fig. 18 ) – early RA,
gout
- Joint space narrowing
- Symmetrical ( Fig. 19 ) – early inflammatory arthropathies
- Asymmetrical ( Fig. 20 ) – OA
- Joint space widening – early infective/inflammatory arthropathies due to the joint effusion at the early stages.
Distribution
1. Monoarticular/Polyarticular
a. Monoarticular ( Fig. 21 )
- Septic arthritis
- Post-traumatic secondary OA
- Crystal deposition – e.g.
gout
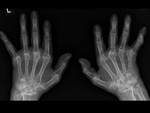
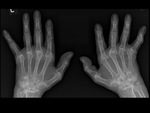
b. Polyarticular ( Fig. 22 )
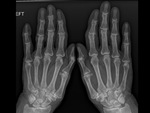
- Rheumatoid arthritis
- Psoriatic arthritis
- OA
2. Proximal/Distal
a. Proximal joints affected in:
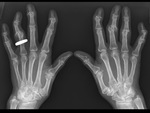
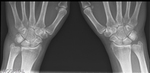
- Rheumatoid arthritis ( Fig. 23 )
- CPPD ( Fig. 24 )
- Ankylosing spondylitis
b. Distal joints affected in:
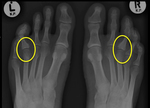
- Psoriatic arthropathy ( Fig. 25 )
- Reiter’s syndrome
- Osteoarthritis ( Fig. 26 )
3. Asymmetrical/Symmetrical
a. Asymmetrical
b. Symmetrical4
Soft tissues
1. Soft tissue swelling
- Soft tissue swelling around joints or tendons– early RA ( Fig. 32 )
- Asymmetrical soft tissue swelling – OA (due to asymmetrical osteophytosis) ( Fig. 33 )
- Diffuse swelling – e.g.
of a whole digit – psoriatic arthropathy (‘sausage-shaped’ digit) ( Fig. 34 ),
Reiter’s syndrome
- Lobulated,
bumpy soft tissue swelling – Gout ( Fig. 35 )
2. Calcification
Soft tissue calcifications
- Gout – calcified tophus ( Fig. 36 )
- Scleroderma ( Fig. 37 )
- CPPD – calcification of the triangular fibrocartilage complex (TFCC),
chondrocalcinosis,
periarticular calcification ( Fig. 38 )