Cysts of the knee joint
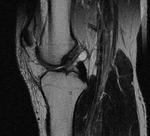
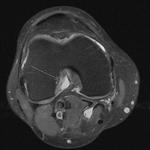
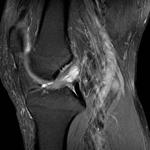
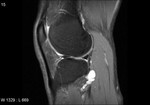
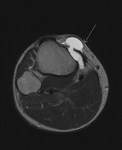
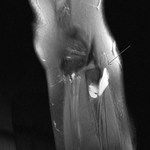
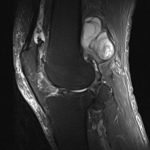
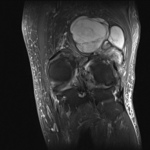
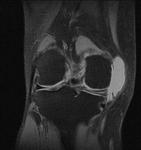
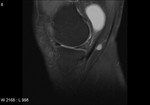
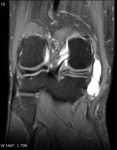
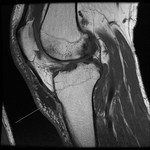
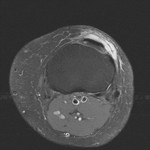
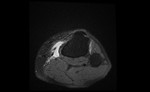
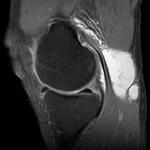
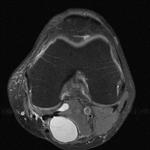
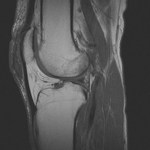
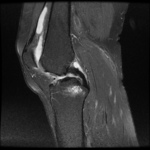
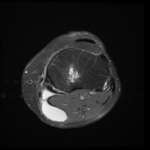
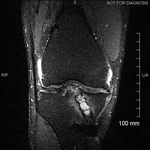
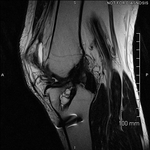
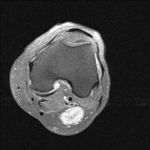
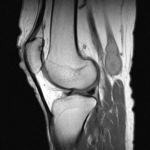
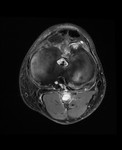
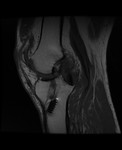
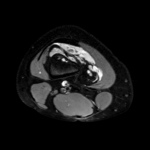
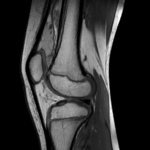
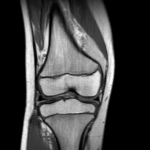
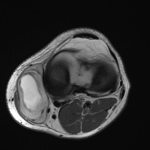
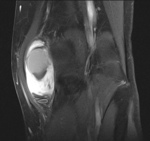
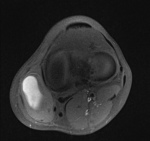
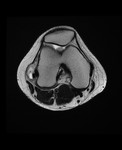
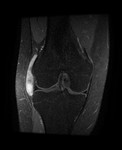
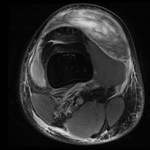
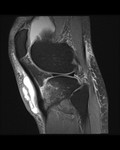
Ganglion cyst (Figures 1 - 8)
Ganglion cyst is a non-malignant cystic lesion commonly associated with musculoskeletal structures. Histology demonstrates thin connective tissue capsule with no synovial lining and contains gelatinous fluid that is rich in hyaluronic acid and other mucopolysaccharides (1).
Although its exact aetiology is unknown,
it is thought to be secondary to mxyoid degeneration of connective tissue and can be broadly divided into intra-articular and extra-articular ganglion cysts.
Intra-articular cyst: Commonly associated with the anterior cruciate ligament,
which is an intra-articular/extra-synovial structure. However,
can be found in the Hoffa’s fatpad attached to meniscotibial and coronary ligaments. They can also present outside the knee joint but within the joint capsule.
Extra-articular cyst: Associated with tendons,
ligaments,
muscles and nerves. These may also represent extension of intra-articular ganglion cyst.
Image findings:
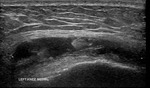
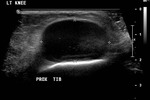
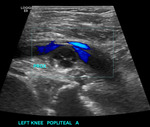
USS:
- Well-defined anechoic lesion with posterior acoustic enhancement
- May contain few internal septations with no neovascularity
- No associated soft tissue component
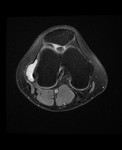
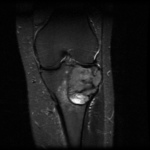
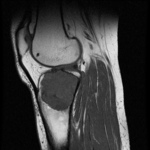
MRI:
- T1: Typically,
hypointense although high proteinaceous content or internal haemorrhage can cause hyperintensity
- T2: Usually hyperintense
- No contrast enhancement
Key learning point: Large,
complex ganglion cyst can often mimic a more aggressive lesion. It is therefore important to find a ‘tail’ that communicates the cystic lesion with the adjacent tendon,
joint or ligament.
Meniscal Cyst (Figures 9 - 11)
Also termed parameniscal cyst,
when it extends beyond the margin of the meniscus. It is a common condition found in approximately 5% of MR Knee examinations and are often associated with meniscal tear,
where the synovial fluid become encysted (2). However,
parameniscal cyst near the anterior horn of the lateral meniscus is thought to occur without any evidence of meniscal tear (3).
Medial meniscus: Usually found adjacent to the posterior horn as meniscal tears commonly occur in this location.
Lateral meniscus: As the lateral meniscus is not bound tightly by the joint capsule,
the meniscal cyst can protrude superficial to the lateral collateral ligamentous complex (ITB,
fibular collateral ligament and biceps femoris tendon) mimicking a palpable soft tissue lesion on clinical examination.
Image findings:
USS:
- Anechoic cystic lesion located adjacent to the meniscus
- Associated degenerate or torn meniscus can sometimes also be visualised
MRI:
- This is the investigation of choice as it can accurate assess the meniscus for tears or other internal derangement of the knee.
- Communication with torn meniscus is important to definitively term the cyst a ‘meniscal cyst’
- T1: Hypointense
- T2: Hyperintense
- No contrast enhancement
Key learning point: Visualisation of the posterior margins of the knee joint can be limited on arthroscopy,
therefore MRI becomes important in assessing for the presence of meniscal cyst in these locations.
Bursal disease (Figures 12 - 18)
Also known as synovial cyst is a juxta-articular cyst that is lined by synovium that may or may not communicate with the joint itself. It always smooth,
frictionless movement of muscle and tendon around a joint. It can become inflamed secondary to repetitive trauma or systemic inflammatory process. Recurrent inflammation causes fluid to accumulate within the bursa,
which can present as soft tissue swelling.
Association:
- Commonly degenerative changes of the knee
- Trauma
- Inflammatory arthropathy e.g.
Rheumatoid arthritis,
SLE,
JRA
- Crystal arthropathy e.g.
Gout
Popliteal cyst (Baker’cyst):
- Cyst represents fluid distended bursa that arises between the medial head of the gastrocnemius and semimembranosus. It commonly communicates with the knee joint and loose bodies can be found in the distended bursa when there is associated osteoarthritis of the knee or osteochondromatosis.
Infrapatellar/prepatellar bursa:
Prepatellar bursa as the name suggests is a bursa found anterior to the patella and infrapatellar bursa found anterior to the patellar tendon. Its inflammation is secondary to repetitive pressure classically in patients’ who do a lot of kneeling (e.g.
plumbers and gardeners). It presents as anterior knee pain with associated soft tissue swelling. Although diagnosis can usually be made with history and examination,
imaging maybe needed in atypical or unusual presentations. Cystic,
well-defined lesion in classic locations in conjunction with appropriate clinical history is required for the diagnosis.
Subchondral cyst/geode (Figures 19 - 20)
These well-defined cystic lesions arise from the subchondral bone plate and is a common finding in the presence of degenerative joint. There are two hypotheses to its formation;
1. Synovial fluid intrusion theory - increased synovial pressure causes the adjacent bone erosion,
which in turns becomes encapsulated by fibrous tissue causing the intraosseous cyst (4).
2. Bone contusion theory – loss of overlying cartilage predispose the subchondral bone to increased microtrauma leading to focal osteonecrosis and resultant fluid accumulation giving arise to the subchondral cyst (5).
It is most commonly seen in degenerative joint disease,
rheumatoid arthritis,
crystal deposition disease and avascular necrosis. It is the most common differential diagnosis to a lytic lesion of the epiphysis and there is usually concurrent joint disease and overlying cartilage loss.
ACL reconstruction tibial tunnel cyst (Figures 21 - 23)
Small amount of fluid can develop within the tibial tunnel component of ACL reconstruction. The fluid is generally thought to be reabsorbed within 18 months,
however can persist. These may sometimes extrude through the tibia into the adjacent subcutaneous tissue leading to pretibial cyst,
which can be palpable clinically. It is thought to be secondary to incomplete incorporation of allograft leading to tissue necrosis and leakage of synovial fluid through the tunnel (6).
Key leaning point:It is important to note that this does not lead to tunnel expansion,
graft failure or screw instability.
Cyst-like lesions of the knee joint
Neurovascular lesions
Peripheral nerve sheath tumour (Figures 24 - 26)
Peripheral nerve sheath tumours (PNST) are benign neurogenic tumours that arises from the nerve sheaths. They can undergo malignant transformation (MPNST) commonly closer to nerve trunks,
such as sciatic nerve,
brachial and sacral plexus (7). MPNST account for 10% of soft tissue sarcomas and 40-60% of MPNST arise from patients with NF1 (8). Patients with MPNST classically present with pain or focal neurological deficit along the nerve that is affected due to impingement or mass effect.
Image findings:
USS:
- Hypoechoic,
well defined mass along the course of the peripheral nerve
CT:
- Usually low attenuation due to fat content of myelin
MRI:
- The lesion is well-defined and is fusiform-shaped,
which tapers towards the normal nerve on either side of the lesion
- A peripheral rim of fat,
also known as ‘Split-fat sign’ is a classic finding where the neurogenic lesion is surrounded by a normal adjacent subcutaneous fat
- There can also be denervation oedema (acutely) or fatty atrophy (chronically) of the nerve supplied by the affected nerve
- T1: Usually isointense to muscle
- T2: Hyperintense
Key learning point: MPNST is also found to be more heterogeneous compared to other neurogenic tumours. Contrast enhancement is also variable in both benign and MPNST,
although more contrast enhancement is apparent in MPNST (9). PET-CT can isolate the area of increased tracer activity indicative of malignant transformation,
which can be targeted for image-guided biopsy.
Cystic adventitial disease (Figures 27 - 29)
This is an uncommon vascular malformation usually affecting the peripheral vasculature.
It affects middle-aged patients without any history of atherosclerosis or other forms of systemic vasculitides. Popliteal artery is the most commonly site of disease affecting up to 85% of cases (10). Patients classically present with calf claudication and lower leg pain.
Histology demonstrates collection of mucinous cysts along the adventitial layer of the affected vessel.
Image findings:
USS:
- Multiple anechoic cystic lesions scattered throughout the wall of the affected vessel.
- There is no Doppler flow through the lesions.
- The lesions may cause mass effect of the artery with associated Doppler waveform and velocity indicative of arterial stenosis.
MRI:
- Aggregation of small cysts or multiloculated appearance of large cyst along the wall of the popliteal artery giving a concentric or hour-glass appearance to the stenotic segment
- The mass effect caused by the lesion can displace the affected artery to one side giving it the classic ‘scimitar sign’
- T1: Usually hypointense,
although determined by the mucinous content of the lesions
- T2: Hyperintense
Synovial haemangioma (Figures 30 - 32)
It is a rare,
benign vascular malformation arising from the joint and is categorised as a subtype of soft tissue haemangioma. Patient present at a young age with history of recurrent haemarthrosis,
pain and knee swelling and commonly affect the knee joint.
Image findings:
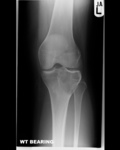
Plain radiograph:
- Non-specific knee joint effusion
- Sometimes can identify intra-lesional phlebolith or soft tissue density mass lesion
MRI:
- Lobulated intra-articular mass within the synovial recesses. Aberrant vascular communication can be seen extending to the muscles and adjacent bone (11)
- T1: Isointense.
Low signal fibrous septations can be seen
- T2: Markedly hyperintense with fluid-fluid level
- Can cause blooming artefact on gradient echo sequences due to recurrent chronic haemorrhage
Tumours mimicking cyst
Malignant soft tissue lesions (Figures 33 - 38)
There is wide array of soft tissue lesions that can mimic cysts on MRI. Undifferentiated pleomorphic sarcomas,
myxofibrosarcomas,
myxoid liposarcomas,
synovial sarcomas,
extraskeletal myxoid chondrosarcomas and rarely soft-tissue metastases can present as T2 hyperintense lesions as seen in cysts (12). It is therefore imperative to give contrast to discern if there is any intra-lesional contrast enhancement seen in malignant soft tissue lesions.
Image findings:
- Wall thickening
- Heterogenous internal signal
- Thick septation
- Intra-lesional nodule
Giant Cell Tumour (Figures 39 - 41)
Relatively common,
benign bone tumour arising from the metaphysis and extending into the epiphysis. This lesion is commonly seen around the knee joint affecting distal femur or proximal femur in approximately 50-65% of cases (13). Although usually benign,
sarcomatous transformation can occur especially in inoperable cases that have been treated with radiotherapy. Lung metastases are also known to occur although have an excellent prognosis (13). There is often co-existence with aneurysmal bone cyst (ACB).
Image findings:
The classic findings include:
- Occurs in patients with closed growth plates
- Well-defined,
non-sclerotic rim
- Eccentric lesion
- Abuts the articular surface (or within 1cm of the articular surface)
MRI:
- T1: Low to intermediate solid components
- T2: Heterogeneously high signal with areas of low signal due to haemosiderin and fibrosis
- T1 C+: The solid components will enhance
- Fluid-fluid level can be seen when there is co-existence with ABC.
Miscellaneous
Morel-Lavellee lesion
Lesion that arises secondary to a degloving injury as a result of severe trauma. The overlying skin and subcutaneous tissue is abruptly sheared away from the underlying fascia causing a potential space in between that is filled with serious fluid and haematoma. These may spontaneously resolve or become encapsulated and present as a palpable mass.
Image findings:
Hypo- or anechoic,
well-defined lesion,
which may contain areas of internal debris depending on the consistency of the lesion. On both USS and MRI,
the lesion can be identified arising between the fascia and the overlying subcutaneous lesion. Internal fluid-fluid level can also be appreciated in some cases.