Anatomy
Although the groin lacks formal anatomical limits,
for practical purposes it can be considered as the area that covers the inguinal region and the pubic symphysis,
it extends inferiorly to involve the proximal aspect of the adductor compartment of both thighs and superiorly to the rectus abdominis muscles.
The pubic symphysis is an amphyarthrodial joint,
composed of a pair of pubic bones and an interposed articular disc offers an ovoid articular face covered with articular cartilage and a fibrocartilaginous disc interposed,
it´s function is absorbing the forces created in the movements.
The superior and inferior ligaments (arcuato),
are more important than the anterior and posterior to stabilize the joint.
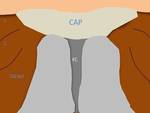
The pubis is the place of insertion of numerous muscle groups.
The most important are the anterior rectus and the long adductor,
both are inserted through the aponeurosis forming an anatomical unit but its function is antagonistic.
Additionally other tendinous structures such as gracilis,
adductor breve,
pectineus,
external obturator as well as the parasinfisial ligaments and elements of the external inguinal canal (transverse and internal oblique muscle through the joint tendon and the external oblique through the inguinal ligament),
are inserted in the pubis creating a continuous fibrocartilaginous component with the pubic ligaments and the articular fibrocartilaginous disc,
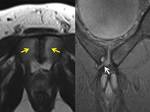
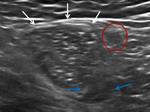
known as the prepubic aponeurotic complex (fig 1) that should be considered as an anatomical and functional unit,
and crucial to verify its integrity in imaging studies to reach the diagnosis.
(3)
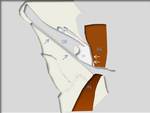
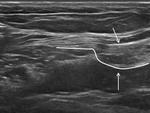
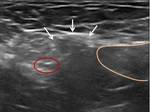
Another basic structure to understand inguinal pathology is the superficial inguinal ring (fig2).
The external oblique muscle fascia inferiorly forms the inguinal ligament.
The medial aponeurotic fibers are thin and are divided into two fascicles in their insertion in the pubic tubercle to form the superficial inguinal ring,
which allows the passage of the spermatic cord.
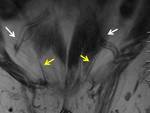
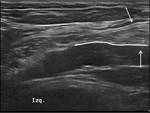
The posterior wall is formed by the weak transversalis fascia,
reinforced by fibers of the abdominal oblique internal and transverse muscles.
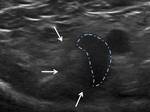
Their medial fibers converge,
giving rise to the classically known joint tendon, inserted predominantly in the anterior rectus sheath (fig3).
(4).
Image tests
Simple Rx (Rx)
The X-ray examination includes the following projections
1.
Anteroposterior projection in decubitus
2.
Anteroposterior view in standing and alternately in one foot (Flamenco view)
3.
Dunn view (45 ° hip flexion)
Radiographic evaluation is essential to evaluate macro-instability or chronic changes secondary to micro-instability in the pubic symphysis and the anatomy of the hips.
1.
Presence of a crossed sign (overlap between the anterior and the posterior wall of the acetabulum)
2.
Enlargement and / or erosion and / or sclerosis of the symphysis
3.
Instability of symphysis> 2 mm
4.
Calculation of the angle α
Ultrasound
Ultrasound is an excellent technique to assess inguinal pain.
It is an accessible,
fast and cheap technique.
With adequate protocol and training the visualization of both anatomy and pathology and therefore the diagnostic performance is excellent.
In addition,
the possibility of performing dynamic ultrasound with the provocative maneuver of Valsalva or standing can allow a quick and accurate diagnosis of most hernias that would not be possible with the static or sectoral image of other techniques.
Another advantage is the "sonopalpación",
being able to direct the patient the exploration to the exact zone where the clinic is generated,
fundamental in patients with ruptures of the insertion of the anterior rectus,
long adductor or injuries of the joint tendon.
Ultrasound,
in addition,
can serve as a guide for the practice of interventional techniques,
whether for therapeutic or diagnostic purposes.
Limitations include the inability to assess bone structures,
particularly bone marrow edema,
limited hip assessment and operator dependence on the technique.
You must provide the following information
1.
Evaluation of the muscular tendon unit of the abdominal and adductor muscles.
2.
Dynamic evaluation of inguinal canal structures.
3.
Evaluation of internal organs.
4.
Evaluation of the urinary tract and genitals
Magnetic Resonance (MR)
Undoubtedly,
the MR is a modality of image with everything necessary to assess this entity.
Among its strengths,
it includes sensitivity to fluids,
being the only technique capable of detecting edema in bone marrow,
it also has a high spatial resolution and multiplanar capacity.
It can include adjacent areas in the study,
such as the hip and even abdominal organs,
detecting anomalies that can produce symptoms that simulate inguinopubic pain.
The limited availability and incapacity to carry out studies with dynamic maneuvers are the main limitations of this technique.
It is essential to establish an adequate protocol of study,
including sequences T1 and STIR coronal,
T2 and DPfs axial and oblique
The hips should be included in the study.
Athletic pubalgia
A general term for all causes of inguinal pain is '' Athletic pubalgia ''.
It refers to a spectrum of lesions of the musculoskeletal system that are located in and around the symphysis pubis and that share similar mechanisms of injury as well as common clinical manifestations.
The most common causes of athletic pubalgia originate in the symphysis pubis (osteitis pubis),
in the muscles and tendons of the adductor and rectus abdominis group,
and inguinal wall.
The pain in the groin in athletes can be acute (secondary to a single event),
chronic (secondary to biomechanical alteration and repetitive microtrauma) or mixed.
It can be postulated that a lesion in a structure (typically insertion of a long adductor or rectus abdominis) may secondarily affect the rest of the structures that depend on the aponeurotic complex,
leading to a dynamic muscular imbalance with the consequent dysfunction or joint instability,
which may lead to to a vicious circle that perpetuates itself in time.
Four major radiological findings appear in patients with pubalgia of the athlete
1.- Degenerative changes in the synovial joint
2.- Pathology in adductor muscle insertions
3.- Bone marrow edema
4.- Secondary cleft sign
Symphysitis
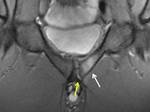
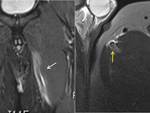
The edema that is the main sign of pubic osteitis and MRI is the best technique to detect it.
It may be due to direct trauma or more frequently to micro-instability (fig 4).
It can be classified in different degrees depending on the signal strength and its extension (<1 cm is classified as grade I, more than 1 cm but <2 cm is grade II,
more than 3 cm It is classified as grade III).
In cases of chronic evolution,
fatty changes in bone marrow,
erosions and osteophytes can be identified (fig 5).
Tendon insertions (CAP)
The characteristic finding is a rupture of the long adductor insertion.
It causes pain in up to 40-60% of cases.
The most frequent mechanisms of injury are rapid adduction of the hip,
forced abduction and sudden acceleration.
Both ultrasound and MRI can be used for diagnosis.
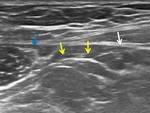
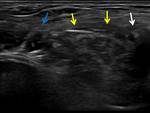
The ultrasound study demonstrates the insertion of the anterior rectus muscle that continues along the pubic fascia.
The findings of tendinopathy include thickening or hypoechogenicity of the tendon,
as well as the loss of the fibrillar pattern.
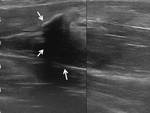
In cases of tendon tear,
the discontinuity of the tendon can be seen as an anechoic defect (fig 6).
In MRI,
most lesions can be visualized directly.
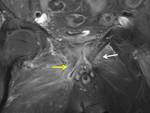
The tear in the insertion of the aponeurosis manifests as areas of increased signal in the lower aspect of the pubis and 1-2 cm lateral to the symphysis,
giving rise to the classic sign of the "secondary cleft" (fig 4)(6).
The sign of the superior cleft refers to a rupture in the insertion of the tendon of the anterior rectus (6).
There may be edema in bone marrow adjacent to the area of insertion,
which should not be confused with pubic osteitis.
In many patients,
this affectation precedes the clinical and radiological appearance of changes in pubic osteitis.
Sometimes other alterations are identified as asymmetries in the abdominal muscles,
and tendinosis at the level of others tendon insertions in the pubis,
Athlete's hernia
Also called prehernia complex,
Gilmore groin,
athlete's hernia
Currently they are understood as a group of lesions involving the abdominopelvic musculature causing weakness of the posterior wall of the inguinal canal,
in the triangle of Hesselbach. The patients respond to the surgical restoration of the inguinal anatomy.
(7)
The ultrasound exam is especially useful in this entity,
manifested as a convex bulge of the posterior wall of the inguinal canal,
evident in the effort (Valsalva) but spontaneously reduced when the abdominal wall is relaxed (fig 7 and 8) The images obtained in MRI or CT in the Valsalva maneuver also show the bulging of the posterior wall (8)
The Valsalva conditions tension of the joint tendon and descent of the roof of the inguinal canal,
to prevent the herniation of structures through the transversalis fascia.
In the dynamic sonographic study the inferior displacement of the cord can be followed,
in case of insufficiency of the posterior wall,
on the other hand,
the cord is displaced anteriorly (fig 9 and 10) (9)
Differential diagnosis
Hockey Syndrome Goalie Base-ball Pitcher
The groin pain in this unusual syndrome is the result of a myofascial hernia of the adductor muscle long,
several centimeters from its pubic insertion.
An etiological link with chronic repetitive stress at sites of neurovascular penetration has been suggested.
Patients often experience acute onset pain,
which may be persistent.
The complete clinical history and physical examination often identify pain distal to the symphysis pubis,
on the herniated muscle.
The most common finding is long adductor muscle belly edema and a muscular lump (fig11).
Septic arthritis
The clinical and radiological appearance of pubic osteitis and osteomyelitis may be indistinguishable.
Osteomyelitis is very uncommon in athletic patients without risk factors such as surgery or pelvic neoplasms.
The infection is usually due to Staphylococcus aureus.
Patients present with fever and acute onset of pain in the pubis that may radiate to the groin.
Radiographic and MR images of septic arthritis-osteomyelitis and pubic osteitis may be similar,
although soft tissue edema and sometimes abscesses may appear in the infection (fig 12).
Inguinocrural hernias
Inguinal hernias (Direct,
indirect and femoral).
Can be associated with significant morbidity and even mortality.
Although they are traditionally diagnosed clinically,
some may be difficult to identify and even more difficult to classify.
Ultrasound is an excellent technique to detect,
differentiate and classify inguinal hernias.
The Valsalva maneuver is a critical component of the examination,
because in many patients the hernia can be completely reduced at rest.
There are several locations in which the internal abdominal wall shows weakness,
being prone to hernia.
An indirect inguinal hernia is produced the deep inguinal ring.
Here,
structures enter the inguinal canal lateral to the inferior epigastric artery and superior to the inguinal ligament,
and extend for a variable distance through the inguinal canal (fig 13).
A second location of parietal weakness is found in the inferior aspect of the Hesselbach triangle,
where direct inguinal hernia is produced.
This weakened area is lateral to the joint tendon and medial to the inferior epigastric artery (fig 14).
A third weakened area is inferior in relation to the inguinal ligament and lateral to the lacunar ligament,
where femoral hernia is produced,
typically medial and adjacent to the femoral vessels.
During the Valsalva maneuver,
the vein will usually expand and must be differentiated from a femoral hernia,
in which case there is an imprint on its medial side (fig 15) (10)