CONGENITAL TARSAL COALITION
Background
This is the abnormal fusion of two or more tarsal bones,
which most likely results from abnormal differentiation and segmentation of primitive mesenchyme with resultant lack of joint formation.
The estimated prevalence is less than 1% of the population.
50% of cases are bilateral.
90% of coalitions are talocalcaneal or calcaneonavicular.
In talocalcaneal coalition all three facets of the subtalar joint may be affected,
however the middle facet is the most commonly involved.
The coalition is most commonly intra-articular,
although extra-articular coalition can also occur. Other,
reported (rarer) coalitions include talonavicular,
calcaneocuboid and cubonavicular.
Tarsal coalitions can be subclassified according to the type of abnormal bridging:
- Fibrous (syndesmosis)
- Cartilaginous (synchondrosis)
- Osseous (synostosis)
Clinical presentation:
Some patients are asymptomatic.
However,
others present in late childhood or adolescence, with hindfoot/tarsal pain or stiffness.
Patients with calcaneonavicular coalition present earlier than those with talocalcaneal coalition (8-12 years versus 12-16 years).
In order to adapt to the hindfoot valgus,
there is secondary peroneal shortening leading to flat foot,
allowing the subtalar joint to be held in the least painful position.
Clinically,
there is reduced hindfoot motion,
pes planus and calcaneus valgus.
Imaging findings:
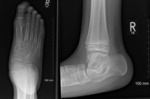
Plain radiographs
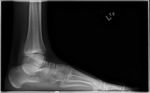
Talocalcaneal coalition
- May demonstrate direct continuity between the two tarsal bones.
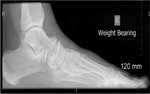
- Talar beak sign - seen on lateral radiographs and represents a prominent beak at the anterior aspect of the talus,
which extends superiorly and away from the talonavicular joint.
This can be seen in talocalcaneal and calcaneonavicular coalitions,
but is seen more commonly in the former.
It is said to occur because the presence of a coalition limits motion at the hindfoot,
leading to compensatory increased motion at the talonavicular joint and the formation of a traction osteophyte at the talar insertion of the dorsal talonavicular ligament.
The sensitivity and specificity of the talar beak sign in detecting talocalcaneal coalition are 48% and 91% respectively,
making it a helpful sign if present. Fig. 8
- 'C' sign - also best seen on lateral radiographs,
this represents posterior continuity between the inferomedial border of the talus and sustenuculum tali.
The sensitivity and specificity of this sign are 88% and 87% respectively.
It is more of a sign of pes planus than of coalition. Fig. 10
- 'Drunken waiter' sign - occurs as a result of a dysmorphic sustenuculum tali,
the inferior border of which becomes enlarged and rounded with a convex undersurface.
(It is normally rectangular on a lateral radiograph and has a flat contour).
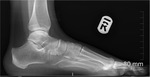
- Absent middle facet sign - this requires a true lateral radiograph.
The non-osseous or osseous coalition obscures the middle facet.
Calcaneonavicular coalition
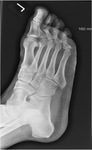
- The internal oblique view best demonstrates the calcaneonavicular interface,
allowing coalition to be diagnosed. Fig. 9 Depending on the type of coalition,
the bones may be in close proximity with irregular articular surfaces as in fibrous and cartilaginous coalition,
or a bony bar may be present as in osseous coalition.
- The talar beak sign may also be seen.
- The 'anteater' sign has a specificity of 94% and a sensitivity of 72% in calcaneonavicular coalition.
The normal anterior process of the calcaneus becomes elongated and squared distally,
resembling the snout of an anteater. Fig. 11
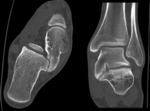
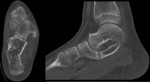
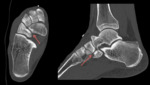
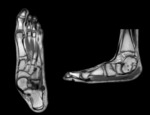
Computed tomography (CT)
- Non osseous coalitions (fibrous and cartilaginous) are subtle.
There may be abnormal narrowing of the joint space with associated minimal reactive osseous changes.
May appear similar to osteoarthritis with sclerosis and subchondral cystic change at a tarsal joint in an otherwise normal non-arthritic foot. Fig. 12 Fig. 13 Fig. 14
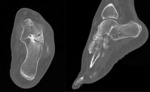
- Osseous coalitions appear as an abnormal osseous continuity of two bones. Fig. 15
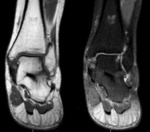
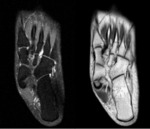
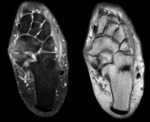
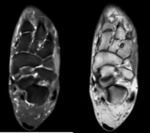
Magnetic resonance imaging (MRI)
- Non-osseous coalitions - demonstrate narrowing of the joint space and irregularity of the bone interface.
There may be bone marrow oedema at the syndesmosis or synchondrosis.
Cartilaginous coalitions demonstrate signal intensity similar to that of cartilage which is of intermediate signal intensity on T1-weighted images and is hyperintense on T2-weighted images.
Fig. 17 Fig. 18 Fibrous coalitions demonstrate low signal intensity at the joint on all sequences. Fig. 19
- Osseous coalition - bone marrow signal continues across the fused articulation,
reflecting the signal or normal marrow. Fig. 20
ACCESSORY NAVICULAR
A relatively common anatomical and radiographic normal variant,
which affects 4-14% of the population and is often bilateral.
It is subdivided into three types,
according to the Geist classification:
- Type I - this represents a small sesamoid bone within the substance of the tibialis posterior tendon and is also known as os tibiale externum'.
This accounts for 30% of accessory navicular.
- Type II - this is a triangular shaped ossicle which is united with the navicular via a synchondrosis and measures 8-12mm in size.
This is considered to be a secondary ossification centre of the navicular and accounts for 50-60% of accessory navicular and 70% of symptomatic cases.
It is also known as a 'prehallux'. Fig. 22
- Type III - this represents a cornuate acessory ossicle which is fused to the navicular via a bony bridge. Fig. 22 Fig. 23
Clinical presentation:
- Type II (and to a lesser extent type III) accessory navicular can be associated with medial foot pain and tenderness,
which is exacerbated by weight bearing,
walking and wearing narrow shoes.
In symptomatic type II accessory navicular this is due to repetitive stress and shear forces across the synchondrosis due to the pull of the tibialis posterior tendon (the bulk of which inserts into the tendon).
- There may be secondary tibialis posterior tendon dysfunction.
Imaging findings:
- Plain radiograph/CT: confirm the presence and type of accessory navicular.
Not usually helpful in identifying abnormality in symptomatic cases.
- MRI: also confirms the presence and type of accessory navicular.
MRI is also able to detect bone marrow oedema within the navicular and synchondrosis and cartilage irregularity/fraying in painful type II accessory navicular.
Fig. 24 Secondary tibialis posterior tendon abnormalities such as tendinosis,
tenosynovitis and tear may also be detected.
Fig. 25
CONGENITAL VERTICAL TALUS
This is also known as rocker bottom foot or congenital convex pes valgus.
It is a severe form of congenital rigid flat foot,
that has an incidence of 1 in 10,000 and affects male and females equally.
50% of cases are idiopathic,
and 50% are associated with aneuploidic syndromes (trisomy 13,
trisomy 18,
18q deletion) and non-aneuploidic syndromes (spina bifida and arthrogryposis).
Congenital vertical talus results from dorsal and lateral subluxation of the talonavicular joint.
This causes the navicular to lie dorsally on the neck of the talus,
the talus lies in a plantar and medial position (vertically directed).
The head of the talus produces a prominence on the medial side and the calcaneus produces a rocker bottom on the sole of the foot.
The forefoot is dorsiflexed,
abducted and everted.
The hindfoot is fixed in plantarflexion.
Soft tissue contractures can result and with displacement of the peroneal longus and tibialis posterior tendons and contracture of the Achilles tendon.
Imaging findings:
Plain radiograph
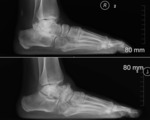
- Lateral - vertically positioned talus,
dorsal dislocation of navicular. Fig. 26
- AP - widened talocalcaneal angle. Fig. 26
- Forced plantarflexion lateral radiograph is diagnostic and demonstrates persistent dislocation of the talonavicular joint.
- Forced dorsiflexion lateral radiograph demonstrates fixed equinus.
CONGENITAL TALIPES EQUINOVARUS
This has an unknown aetiology and is commonly referred to as clubfoot.
It has an incidence of 1 in 1000 births,
is more common in males and may be unilateral or bilateral.
It may be syndromic (when in association with other conditions e.g.
spina bifida) or may occur in isolation (idiopathic).
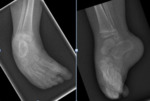
Features of talipes equinovarus: Fig. 28
- Severe hindfoot varus
- Adduction or inversion of the forefoot and midfoot
- The entire foot is held in equinus position,
the heel is high and the fibula is prominent.
- The foot cannot therefore be placed flat on the ground in the standing position.
It may be seen in association with congenital disorders such as cerebral palsy or spina bifida.
Non-surgical treatment is the gold standard (Ponseti method or the French functional method).
Surgical treatment may be considered in fixed deformity,
a known complication of this is early degenerative change involving the ankle,
subtalar and midtarsal joints. Fig. 29
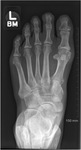
METATARSUS ADDUCTUS
This is the most common congenital abnormality of the foot with an incidence of 1-3/1000 births.
There is medial displacement of the forefoot relative to the hindfoot,
which may be flexible or rigid.
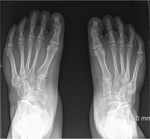
The following features may be present:
- The first metatarsal is medially displaced with or without medial displacement of the metatarsals on the cuneiforms. Fig. 30
- Prominence of the fifth metatarsal base.
- Neutral/slightly valgus hindfoot.
- Supinated forefoot.
- In some cases,
there may be widening of the space between the first and second toes.
In many cases,
imaging is not required as they are mild,
flexible and self correcting.
With persistent deformity i.e.
in rigid cases,
weight bearing radiographs may demonstrate medial deviation of the metatarsals and a trapezoidal shape to the medial cuneiform.
Note there may be increased risk of developmental dysplasia of the hip in these patients.
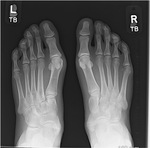
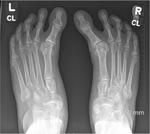
CONGENITAL HALLUX VARUS
This is a very rare condition where the big toe is is angled medially at the metatarsophalangeal joint,
resulting in a large cleft between the first and second toe. Fig. 31