The bone marrow is a large organ that is responsible for normal hematopoiesis.
The cellular structure of bone marrow is complex,
containing stem cells responsible for the production of erythrocytes,
granulocytes,
monocytes,
lymphocytes,
and platelets.
Bone marrow can be divided into two types:
- - yellow (fatty) marrow: contains more fat,
approximately 80%,
and is less cellular.
- - and red (hematopoietic) marrow: about 70% is composed of cellular elements,
that contain mostly water,
and about 30% consists of fatty elements.
Red marrow contains the hematopoietic stem cells and blood cell progenitors.
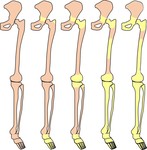
At birth almost the whole skeleton is occupied by red marrow,
which progressively converts into yellow one by a predictable pattern: from distal to proximal,
from the appendicular to the axial skeleton and from the diaphysis of the long bones toward the metaphysis,
in a bilateral and symmetric way.
Marrow in the spine is typically the last to become inactive.
Fig 1.
Under normal conditions,
in adults,
red marrow can be found in the skull,
scapulae,
sternum,
ribs,
hip bones,
vertebrae and proximal long bones.
This hematopoietic marrow may be replaced by fatty marrow with age.
But marrow composition may change also due to other factors such as obesity,
running,
anemia or other hematologic disorders,
chemotherapy or radiation therapy.
Reconversion from yellow to red marrow refers to the reverse sequence of marrow maturation in response to increased hematopoietic demand.
It can occur during the whole life,
following this process the same predictable pattern as the normal conversion,
but in the reverse direction.
MRI is an ideal noninvasive imaging technique that can be used to study the level of bone marrow cellularity at any skeletal location.
MRI is very sensitive to early detect cellular infiltration confined to the bone marrow space prior to the development of trabecular destruction.
However,
the specificity of the MRI signal characteristics is limited,
due to overlapping in the presentation of both neoplastic and non-neoplastic lesions on conventional T1-W,
T2-W,
and fluid-sensitive images.
Furthermore,
morphological sequences do not provide quantitative information.
For example,
the cellular proliferation of malignant lesions,
the so-called “bone marrow replacement lesions”,
replaces normal bone marrow,
leading to the disappearance of fat signal inside the lesion.
This has been established as a key diagnostic criterion to differentiate neoplastic tissue from normal marrow.
The predominant contribution of fat to bone marrow signal explains the importance of unenhanced T1-W sequences for the evaluation of bone marrow,
as normal bone marrow or benign lesions have a depictable fat content,
as areas of high signal intensity on T1-W sequences.
Conversely,
malignant lesions usually show decreased signal on T1-W images,
with variable appearance on fluid-sensitive images.
But,
sometimes focal areas of low T1-W signal within bone marrow provide a diagnostic dilemma.
Normal red marrow contains intermixed fat,
and typically show higher signal intensity than muscle on T1-W sequences.
However,
in cases of profound red marrow reconversion,
red marrow may be difficult to differentiate from malignancy,
as bone marrow infiltration or replacement with malignant cells tends to produce focal or diffuse areas with equal to lower signal intensity than muscle on T1-W images.
DIXON MRI is a water-fat separation method that helps to:
- - identify pathology hidden by fat,
- - assess bone marrow disease,
- - allows tissue characterization of neoplasms and
- - quantify the fat percentage of a tissue.
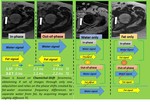
It is based on chemical shift phenomena and in one acquisition can provide a set of four images:
- - in phase (equivalent to standard non-fat-suppressed images)/out of phase images: typical chemical shift imaging
- - water-only image: equivalent to fat-suppressed images,
and
- - fat-only image: water-suppressed signal intensity image.
Dixon technique can be acquired with two,
three or multiple echo times.
The more the echo time (TE),
the lesser the phase error.
It can be used with T1-W and T2-W images,
with spin echo or gradient echo sequences,
and water-only images may be also used after gadolinium injection,
providing a very homogeneous fat-suppression.
Dixon method relies on the phase shifts created by fat-water resonance frequency differences to separate water from fat.
Phase information is encoded by acquiring images at slightly different TE,
exploiting the difference in resonance frequency between water and fat.
Fig 2.
Recently,
Maeder et al proposed Dixon SE T2-weighted sequences with fat-only and water-only reconstructions as an alternative to the standard combination of morphologic sequences (T1-W and fat-suppressed fluid sensitive sequences) for the detection of spinal bone marrow lesions.
In their study,
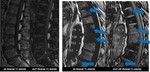
metastasis was defined as an area of replacement of the fatty signal of bone marrow,
hypointense compared with skeletal muscle on T1-W images,
and without detectable signal intensity on Dixon fat-only T2-W images. Fig 3.
Because Dixon fat-only T2-W images are specific to fat signal,
their interpretation is more straightforward: bone marrow replacement lesions show almost no intralesional signal relative to adjacent bone marrow because of the disappearance of fat,
and therefore,
there is no need to compare the signal intensity to that of adjacent muscle.
On the other hand,
chemical shift imaging (CSI) from in phase (IP) and opposed phase (OP) Dixon images,
can demonstrate the relationship between the amount of fat and water that coexist in the same voxel,
being useful to assess bone marrow lesions.
CSI is based on the principle that protons attached to water and fat precess with slightly different frequencies.
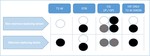
When a voxel contains fat and water,
there is an additive effect on the signal in the IP image with loss of signal on the OP image.
Marrow infiltrative processes tend to replace the fatty marrow components completely.
Thus,
as a marrow infiltrative process completely replaces normal fatty marrow,
there is only water within the voxel and there is no significant drop in signal on the OP image compared with the IP image.
Signal drop can be assessed qualitatively or may be expressed quantitatively as the signal intensity ratio (SIR).
The relative SIR is calculated with the formula: SI (OP)/SI (IP) and can also be expressed as a percentage signal drop using: [(SI (IP) - SI (OP))/ (SI (IP)] x 100.
Thus,
processes that replace or displace marrow will have a SIR cut-off value > 0.8 or a percentage of signal drop <20%.
Conversely,
non-marrow-replacing processes will show a SIR <0.8 or a percentage of >20% signal loss,
with a 95% sensitivity and an 89% specificity.
Fig 4,
5.