- The literature review of acute musculoskeletal pathology reveals that many of the acute musculoskeletal pathology ultrasound images may resemble the ultrasound images of other abnormalities.
- Acute musculoskeletal pathologies and their common misdiagnoses,
along with recommended solutions and precautions,
are presented and discussed below.
1. Cellulitis versus necrotizing fasciitis
Cellulitis refers to edema and hyperemia of subcutaneous tissue and skin which is primarily clinical diagnosis.
However,
in case of failed antibiotic treatment or suspected complication or inconclusive diagnosis,
imaging can provide a crucial information for conclusive diagnosis and appropriate treatment decision [1].
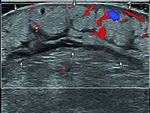
Ultrasound shows different images of cellulitis depending on the location and the severity of the pathogens.
The difference ranges from increased echogenicity with thickened skin and subcutaneous tissues to cobblestone appearance accompanying with hyperemia of the involved area on Doppler imaging (Fig. 1) [2,
3].
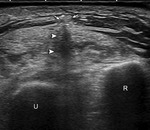
Necrotizing fasciitis is severe deep soft tissue infection leading to necrosis of the tissue [1],
usually as the result of group A streptococci [2].
Although necrotizing fasciitis may appear as cellulitis as soft tissue edema,
the presence of soft tissue gas with comet tail artifact or dirty shadowing provides sufficient evidence to conclude necrotizing fasciitis (Fig. 2) [2,
4].
Since ultrasound is more effective in detecting gas within soft tissues than plain radiographs [4],
it is an excellent imaging tool for providing a conclusive diagnosis between cellulitis and necrotizing fasciitis.
2. Tenosynovitis versus extensor retinaculum or pulley injury
Tenosynovitis may occur as the result of infectious or noninfectious process.
Infective tenosynovitis generally results from Staphylococcus aureus or Streptococcus pyogenes [2] after penetrating injury especially at hand and wrist.
Ultrasound can reveal visual clues of pathology within tendon sheath or intraarticular locations that are useful for deciding appropriate treatment.
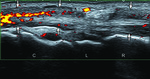
Tenosynovitis appear as distended tendon sheath with an-/hypoechoic fluid or synovial hypertrophy (Fig. 3) [5,
6].
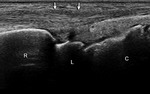
Extensor tenosynovitis of the wrist may simulate a normal structure known as extensor retinaculum as a hypoechoic band if the sound beam is not positioned perpendicular to the retinaculum while performing ultrasound (Fig. 4) [5].
In addition,
digital flexor tenosynovitis of the hand is also sometimes confused with pulley injury as thickened hypoechoic band (Fig. 5) [6].
Knowledge of anatomical location and bowstring deformity in pulley injury can help in differentiating between these two entities.
3. Synovitis versus fluid distention of a joint recess
In general,
synovitis results in hypoechoic synovial proliferation with articular distention that may resemble complex fluid distention of a joint recess [7].
However,
synovitis is minimally compressible,
whereas the fluid distention joint recess is redistributable during dynamic ultrasound.
Doppler imaging can aid in differentiating between these two entities with hyperemia in synovitis,
whereas no hyperemia is visible for the complex fluid (Fig. 6) [7].
4. Fracture versus other bone irregularities
Normal osseous cortex shows a uniform and smooth hyperechoic line with posterior shadowing.
Although ultrasound has limitation in assessing osseous pathology,
it can assess fracture with high accuracy [8].
Thus,
ultrasound can be used to diagnose osseous by observing surface discontinuity,
surface irregularity,
double line cortex,
avulsion fracture and disrupted alignment (Fig. 7) [9,
10].
Moreover,
ultrasound can reveal other associated abnormality such as hemothorax from rib fracture and other important characteristics such as osteophytes in osteoarthritis etc.
(Fig. 8) [5] For confirmation,
correlation with plain radiographs can be used for verification.
5. Osteomyelitis and pitfalls
Osteomyelitis has bimodal predisposing age groups with different predisposing pathogens [2].
Plain radiograph is the primary modality for evaluation,
however it has low sensitivity in diagnosing osteomyelitis.
Magnetic resonance imaging (MRI) is the imaging of choice in assessment of this entity,
however,
MRI is not always accessible and expensive [2].
On ultrasound,
the presence of juxtacortical fluid collection in adults or subperiosteal exudate in children accompanying with surrounding hyperemia may indicate acute osteomyelitis (Fig. 9) [11,
12].
Moreover,
ultrasound can provide details about the area of the infection and predisposing factors such as foreign body and fistula etc.
On the other hand,
normal ultrasound appearance cannot exclude osteomyelitis according to the major drawbacks of ultrasound in evaluation of intramedullary abnormality [11].
6. Detection of foreign bodies retention
The retained foreign bodies can be classified as radiopaque or non-radiopaque (wood and plastic,
etc.) which might have been undetected.
Ultrasound has high accuracy in determining the size,
the contour and the location of the foreign body [13].
On ultrasound,
all foreign bodies have hyperechoic characteristics with associated sonographic artifact such as posterior shadowing and surrounding soft tissue changes as the result of edema,
hemorrhage and granulation.
(Fig. 10) [13,
14] Such features could help in identifying the foreign bodies.
Moreover,
ultrasound can detect potential complication including infection and soft tissue injuries,
as well as assist in removal of the foreign bodies (ultrasound-guided) [13].