Case report:
A 88-year-old woman was admitted in the emergency orthopaedic department (ED) of our hospital for persistent pain at the left lower extremity.
The pain initially started suddenly two months before and the family orthopaedic doctor diagnosed greater trochanteric bursitis.
She underwent a corticosteroid injection in the trochanteric bursa with no improvement of the clinical outcome.
There was no history of trauma,
fever,
weight loss or family history of skeletal disorders.
She had undergone partial mastectomy after having diagnosed breast cancer four years ago.
She received treatment against osteoporosis (weekly 70 mg alendronate,
calcium supplement and vitamin D daily) for four years.
In terms of activity,
previously the patient could be self-serviced and went through her daily activities without any discomfort or use of any type of walking aids.
During the physical examination,
the patient presented an analgesic gait that was improved by using a cane on the opposite side of the painful limb.
Except of tenderness in the left femur,
there were no other specific clinical findings or neurological deficits.
Laboratory examination results including complete blood count,
erythrocyte sedimentation rate,
C-reactive protein value,
alkaline phosphatase levels,
blood biochemistry,
liver and kidney function tests,
rheumatoid factor,
tumor markers and serum protein electrophoresis were within normal limits.
Radiograph of the femurs showed asymmetrical endosteal mid-diaphyseal hyperostosis with partial obliteration of the medullary cavity and mild expansion of bone mostly in the left femur.There was no periosteal reaction or soft- tissue abnormalities.
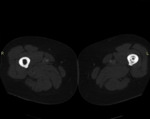
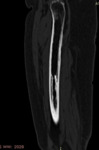
CT of the femurs confirmed the endosteal new bone formation and narrowing of the medullary canal.
No cortical irregularities were noticed.
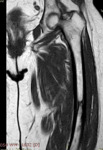
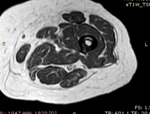
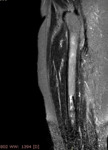
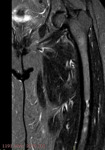
MRI demonstrated low signal intensity in all pulse sequences at the site of osteosclesosis.
Minimal enhancement was noted at fat-supressed contrast enhanced T1-sequence.Neither increase signal intensity or enhancement was noted at the adjacent soft tissue.
Isolated radiological findings are not diagnostic; hence,
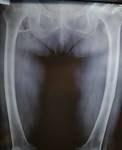
the role of triphasic bone scan in ruling out other differentials is valuable.Initial vascular phase and blood pool images show no evidence of increased vascularity or soft tissue tracer pooling.
Delayed anterior and posterior planar images showed fusiform‑shaped intense area of tracer uptake mostly in the diaphysis of left femur corresponding to the site of pain.
Abnormal tracer uptake was seen in 3 thoracic vertebrae (T8,T10,
T12),
which were attribute to osteoporotic vertebral fractures and to the anterior edge of the 7th rib.
Follow up radiographs and CT performed 4 months later showed that the lesions remained stable.