EPIDEMIOLOGY
- Paget's disease has a characteristic geographical distribution:
- It presents high prevalence in United Kingdom,
North America,
Australia,
New Zealand and Germany.
- It is unusal to find cases in Africa or Asia.
- 3 – 4 % of people over 40 year old are affected.
- It is more frequent in men than in women (3:2) and prevalence increases in both sexes with age.
- Only 10 – 30 % presents monostotic form.
ETIOLOGY
Despite the fact that 140 years have passed since it was first described,
the etiology of Paget’s disease remains unknown.
Various theories have been postulated throughout these years,
such as:
- Viral origin: intranuclear and intracytoplasmatic inclusion bodies which can be seen in osteoclasts of bones affected by Paget’s disease are similar to the nucleocapsid of the Paramyxovirus of the RNA virus family).
- Genetic component:
- SQSTM1/p62 gene confers hyperactivity to osteoclasts precursors producing multinucleated osteoclasts.
5 – 10 % of patients with Paget’s disease present this gene mutation.
- There is also a locus of susceptibility in 18q chromosome.
It causes increased osteoclastic activity,
explaining the increased bone remodelling of this disorder.
- An increased IL-6 in bone marrow and blood in patients with Paget’s disease has been observed in recent studies.
Apparently,
IL-6 produces an increase in osteoclasts formation.
DIAGNOSTIC IMAGING:
Radiographic findings:
Simple radiography is the method of choice in the diagnosis and monitoring of Paget’s disease.
Reserving CT and MRI for cases of diagnostic doubt and those requiring assessment of possible complications.
Bone lesions of destructive nature are observed,
followed by repair with deposit of excess neoformed bone.
There are three stages:
- Active or destructive: Lylic phase where osteoclastic reabsorption predominates.
- Mixed: Persistence of active disease in which osteoblastic and osteoclastic hyperplasia coexist with predominance of osteoblastic activity.
- Inactive or sclerotic: Blastic phase in which activity is gradually lost until it becomes inactive.
We must remember that despite having reached the inactivity phase,
the disease can be reactivated.
Although bone expansion has been the classical image of the Paget’s disease,
due to the disorganized bone remodelling it undergoes,
during the different phases we can see an increased and decresed bone edge,
and bone marrow of different densities.
Not all bones are affected with the same frequency,
presenting the folowing descending order in the pelvis,
the lumbar spine,
the sacrum,
the femur,
the skull and the dorsal column.
Characteristics of the imaging according to its location:
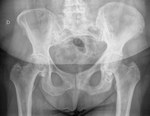
Pelvic affection in X-ray imaging:
The most frequent is to see mixed or sclerotic changes,
showing a marked trabecular thckening.
The ilion usually shows irregular islets of high density and radiolucent areas.
However,
the iliopubic and ilioischiatic branches usually have a greater bone widening which is really deforming.
Fig. 1
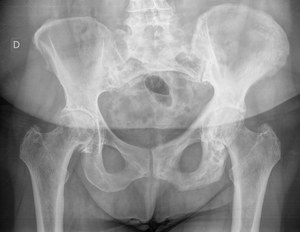
Fig. 1: 68 year old woman. Thickening of the bone cortical and coarsening of the trabecular pattern of the left iliopubic and ischiopubic branches, characteristic of Paget's disease.
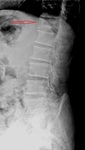
Vertebral involvement in X-ray imaging:
There is an increased and disorganization in the bone trabecular pattern in the mixed stage.
In addition,
it has a cortical thickening,
remarking the edges of the vertebral body and producing an image of ‟ picture frame vertebral body” or “bone within a bone”.
Fig. 2
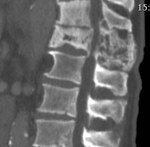
In the sclerotic stage there is a loss of height with increased anteroposterior diameter,
as well as increased size of the posterior vertebral elements.
Fig. 3
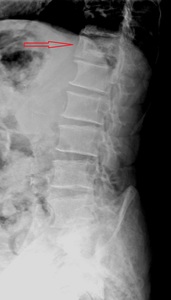
Fig. 2: 79 year old man. Image of ‟picture frame vertebral body” or “bone within a bone”.
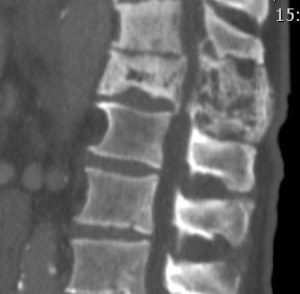
Fig. 3: Same patient in figure 2 three years after. CT image showing loss of height with increased anteroposterior diameter and coarsening of the posterior elements.
X-ray imaging of long bones:
In the osteolytic phase we can see a radiolucent area that begins in the metaphysis of the bone and extends towards the diaphysis showing a characteristic image of “blade of grass”
In more advanced stages,
successive layers of neoformed bone accumulate in the periostium,
evolving to sclerosis that ends up merging with the cortex.
Cortical proliferation on the external surface together with endosteal destruction causes an increase in the transversal diameter of the bone,
but a thin cortical bone.
In surfaces subjected to tension the bone responds by depositing periosteal bone,
and on those under compression reabsorbing it,
which causes deforming bowing of the bone.
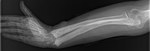
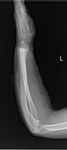
The most common is the lateral femur bowing and the anterior tibia bowing. Fig. 4 ,
Fig. 5
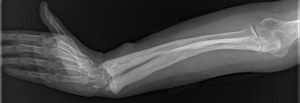
Fig. 4: 64 year old woman. Coarsening of the trabecular pattern of the ulna and radius, together with bowing specially of the radius.
Skull affection in X-ray imaging:
Abnormal radiolucent areas are seen in osteolytic phase:
- Circumscribed osteoporosis: First destructive stage.
It is a desossification of the frontal or occipital area,
well-defined, which spreads slowly to cover the main portion of the calotte.
Progressive sclerosis or mixed phase affects de inner table of the calvarial ang diploe,
leaving smooth bone in the outer table.
We can observe large round areas of sclerosis surrounded by demineralization,
showing a characteristic appearance in “cotton ball”.
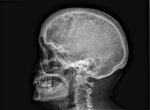
Fig. 6
When diffuse sclerosis is reached,
there is a significant thickening of the inner table which results in an increase in the diploe producing a skull image in ‟tam-o-shanter″ (typical broad,
flattened Scottish beret).
In addition,
a softening of the base of skull wih basilar invagination can occur,
which can cause a cranial nerve entrapment.
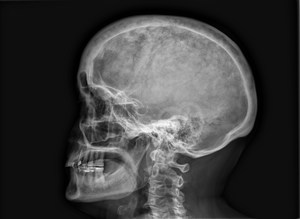
Fig. 6: 69 year old woman diagnosed with Paget's disease. Characteristic skull appearance in “cotton ball”.
Affection other less common bones: Fig. 7 ,
Fig. 8
- In the ribs there is an increase in bone density with bone widening.
- When clavicles,
hands and feet bones are affected,
wthey are seen larger and denser.
- Finally,
if we have a small bone affectation,
a “bubble destruction” occurs.
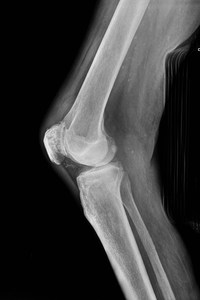
Fig. 7: 89 year old man. Increased trabecular pattern and coarseness of the right patella.
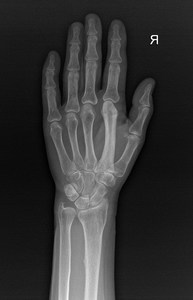
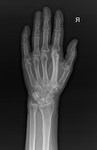
Fig. 8: 64 year old woman. Marked increase in size and sclerosis of the second right-hand metacarpal.
DIFFERENTIAL DIAGNOSIS:
•Blastic metastases in the pelvis:
- Prostate metastases usually affect the pelvis in a diffuse manner,
unlike Paget's disease which only alters the bone structure of a hemipelvis.
- In addition,
they neither show a coarsened trabecular pattern,
nor increase in the bone size,
which is characteristic of the Paget.
•Fibrous dysplasia:
- It presents an image in "blade of grass" similar to that shown in initial stages of Paget's disease.
- However,
unlike Paget's disease,
it is characteristic of dysplasia to affect the facial mass,
rather than the growth of the calotte.
- There is usually no trabecular or cortical thickening,
and it has a higher prevalence in the young population.
•Multiple myeloma:
- Myeloma has similar lytic lesions,
but does not thicken bone or coarsen the trabecular pattern.
•Myelofibrosis:
- Myelofibrosis produces sclerosis without increasing bone size.
•Frontal hyperostosis:
- Unlike Paget's disease,
frontal hyperostosis usually only affects the inner table of the frontal bone and sometimes the parietal.
TREATMENT
•Treatment is not always indicated in Paget's disease,
it is only contemplated in the following situations:
- Symptomatic disease: Pain in affected bone.
- Presurgical treatment of the Pagetic lesion to decrease high vascular flow and the risk of hemorrhage.
- Treatment to reduce the risk of hypercalcemia in patients requiring prolonged immobilization.
- The treatment of the disease in order to slow down the progression and future complications is currently considered a dubious indication.
•Treatment can be divided into pharmacological,
considering bisphosphonates as standard drug,
or,
non-pharmacological,
which includes orthopedic and surgical measures.
DEGENERATION OF PAGET’S DISEASE INTO SARCOMA
Among the complications of Paget's disease,
the most frequent is osteoarthrosis secondary to biomechanical alteration that supposes changes in bone structures caused by Paget's disease.
As well as,
fractures and entrapment of cranial pairs secondary to the growth of the skull base are not rare complications.
However,
sarcomatous degeneration implies the most serious complication of the disease,
despite having a very low incidence,
less than 10%.
It is more common in generalized Paget's disease.
In addition,
like the disease itself,
it is more common in men and increases its incidence with age.
Paget’s disease can degenerate to different types of sarcoma:
- Osteosarcoma (the most common)
- Fibrosarcoma
- Condrosarcoma
We must suspect this complication when the patient presents a pain of new appearance and resistant to treatment,
accompanied by a soft tissue mass.
Occasionally,
degeneration debuts with a pathological fracture.
In addition,
it is mandatory to rule out this complication in the face of an increase in erythrocyte sedimentation rate (ESR) and alkaline phosphatase.
Sarcomas seem to reflect a distribution similar to that of Paget's disease,
showing a clear predilection for the femur,
humerus and pelvis.
In image diagnosis it can be used radiography,
as well as CT or the MRI:
– In radiography we can find:
- Lytic Lesions
- Cortical destruction
- Spiculated periosteal reaction and/or fractures without signs of consolidation
- Soft-tissue mass
– In CT bone destruction with soft-tissue increase is determined with greater precision.
–In MRI it can be seen an hypointense Pagetic bone in T1-weighted sequences,
with significant enhancement after intravenous gadolinium administration.
Sarcomatous degeneration has a very poor prognosis with a 5-year overall survival of 11%.