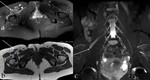
MR neurography allows the localization of the nerve abnormality,
as well as the evaluation of the extent,
the character and the possible causes of the pathology.
Occasionally It may exclude the possibility of neuropathy and it may indicate a different diagnosis mimicking peripheral nerve abnormality.
Furthermore it provides anatomic information,
which is valuable,
especially in pre-operative cases,
or in planning therapeutic injections.
Thus,
knowledge of the anatomy of the peripheral nerve system is of paramount importance.
The anatomy of the peripheral nerves is complex.
Peripheral nerves are comprised by neuron axons.
Each neuron axon is enveloped by “endoneurium”,
which is a myelin stealth composed of Schwann cells.
“Fascicle” is a group of neuron axons enveloped in a tissue layer,
called “perineurium”.
Many fascicles together,
enveloped in another one tissue layer (“epineurium”) comprise the peripheral nerve (Fig1).
Suggested MR protocol for the evaluation of peripheral nerves includes 2D high resolution T1 weighted,
T2 weighted combined with fat suppression and 3D isotropic STIR sequences.
Post gadolinium T1 weighted with fat suppression images may contribute in diagnosis in several cases.
Diffusion Tensor Imaging (DTI) is also used in several institutions,
in order to perform fiber tractography.
Findings suggestive of nerve abnormalitiy are nerve enlargement,
deviation,
or discontinuity,
disruption of fascicular pattern,
T2 hyperintesnities.
Enchantment post contrast medium administration may be present due to the blood-nerve barrier breakdown.
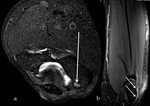
MRI can also depict acute and chronic skeletal muscle denervation,
adding clues for the localization of the level of the nerve abnormality.
Acute denervation is characterized by muscle edema,
subacute denervation by both edema and fatty infiltration and chronic denervation by fatty infiltration and atrophy.
Edema due to muscle denervation should be diffuse,
without any involvement of the adjacent fascia (Fig 2).
Most usual causes of peripheral nerve abnormalities are nerve entrapment/compression,
trauma,
tumor,
and inflammation.
Entrapment occurs when a nerve is compressed by adjacent structures.
T2 hyperintensity is noticed on the affected nerve.
Maximum signal intensity is seen at the level of the compression and just proximal to it.
Fascicular pattern abnormalities and nerve enlargement may occur in more severe cases,
usually proximal to the compression site.
Skeletal muscle denervation may indicate the level of the impingement.
Causes include fascia thickening,
accessory muscles,
hematomas,
synovitis,
tenontitis,
masses,
synovial cysts,
aneurysms and varicose veins.
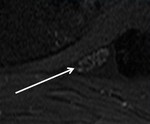
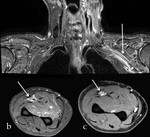
Common locations of nerve impingement are anatomical tunnels (ex.
the carpal tunnel Fig3,
the cubital tunnel Fig4).
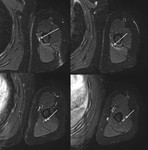
MR neurography may aid the assesment of nerve injury grade.
Nerve injuries include neuroapraxia,
axonotmesis and neurotmesis.
Neuoapraxia is attributed to focal damage at the myelin stealth without axons disruption.
Signal abnormalities (T2 hyperintensity) occurs at the level of the abnormality and proximal to it (mild T2 hyperintensity).
It is the least severe injury and it resolves within weeks to months,
because the axons are not damaged (Fig 5).
Axonotmesis is characterized by loss of axonal and perineurium continuity (Fig 6).
Neuroma in continuity may occur.
Axonal injuriy with disruption of the perineurium and epineurial layers,
with complete transaction of the nerve,
or end bulb neuroma formation (Fig 7),
are depicted in neurotmesis,
which requires surgical treatment.
Valerian degeneration may occur in neurotmesis and axonotmesis.
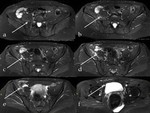
Tumors of the peripheral nerves are usually benign.
They include schwannomas (Fig 8),
neurofibromas,
perineuromas,
neuromas.
Malignant transformation,
as well as infiltration from other neoplasms may also occur.
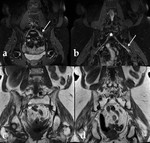
Occasionally peripheral nerves can be infiltrated by lymphoma (Fig 9) or leukemia.
Systemic and inflammatory disorders that may involve the peripheral nerves include chronic inflammatory demyelinating polyneuropathy (CIDP),
inflammatory neuritis,
ischemia,
metabolic disorders,
vasculitis,
radiation neuropathy and connective tissue disorders.
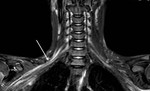
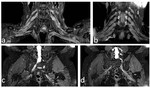
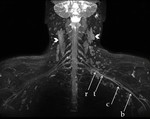
Patients with CIDP may have mild to moderate abnormalities in multiple nerves or plexuses (Fig 10).
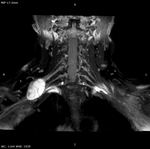
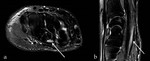
Inflammatory neuritis/plexitis post vaccination or infection affect most commonly the brachial plexus (Fig 11) and may regress after weeks or months.
Parsonage Turner Syndrome (Brachial plexitis) is characterized by acute onset of shoulder pain followed by weakness or sensory loss of the upper extremity (Fig 12).
The etiology is unknown but the condition is associated with recent viral infection,
or vaccination.
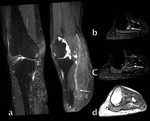
Radiation induced neuropathy may appear several years after radiotherapy.
Symptoms are progressive and nerve damage is irreversible.
Pathophysiology is poorly understood,
but it seems to involve ischeamia because of capillary network failure and direct compression due to radiation induced fibrosis.
Apart from the nerve/plexus abnormalities,
findings include bone (fatty replacement of bone marrow) and muscle (edema) radiation-induced changes (Fig 13).