RATIONALE OF REPAIR:
To achieve intrinsic stability,
the anteroinferior glenoid labrum and the glenoid bone distribute forces across the glenolabral complex when subjected to compressive loads.
With progressive labral and bone loss,
the articular contact is reduced which in turn increases the pressure across the joint when subjected to stress.
.
As a result,
an isolated soft tissue / Bankart repair,
without simultaneous bone graft,
in the setting of shoulder dislocations with glenoid bone loss,
will lead to an overload of forces at the overload at the bone-soft tissue repair interface,
eventually increasing the likelihood of failure of such repair.
.
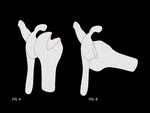
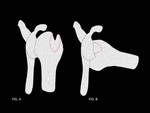
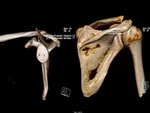
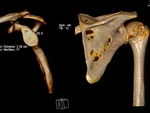
CONCEPT OF ENGAGING LESIONS: (Fig. 2 , Fig. 3)
Burkhart and De Beer described the concept of “engaging Hill-Sachs lesions” as an osseous injury that occurs secondary to anterior shoulder dislocation and predisposes to the failure of arthroscopic repair. Engagement of lesions was defined as the reproduction of symptoms of instability,
such as increased apprehension or a catching/popping sensation when the shoulder was placed in a functional position of abduction and external rotation (defined as 90° of abduction and between 0° and 135° of extension).
.
Symptomatology was thought to be a result of the geometry of Hill-Sachs lesions with a horizontal orientation relative to the humeral shaft in the non-abducted position that becomes parallel to the anterior margin of the glenoid in the abducted and externally rotated (ABER) position,
which predisposes to engagement.
Alternatively,
Hill-Sachs lesions oriented more vertically relative to the humerus in the non-abducted position and extending diagonally to the anterior glenoid in the ABER position result in continuous,
uninterrupted contact between these two surfaces without engagement.
.
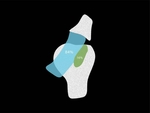
THE GLENOID TRACK: (Fig. 4 ,
Fig. 5)
In order to identify patients requiring bone grafts,
Ito et al introduced the concept of ‘glenoid track’.
This concept was based on the interaction of the humeral head and the glenoid when the arm was placed in abduction and external rotation (ABER).
They demonstrated that as the arm was abducted,
the contact area of the glenoid shifted from the inferomedial to the superolateral portion of the posterior articular surface of the humeral head.
This creates a zone of contact between the glenoid and the humeral head defined as the ‘glenoid track’.
This track if intact (i.e.
no significant bone loss),
under the circumstance of glenohumeral instability,
guarantees bone stability.
.
In their publication,
they described the distance from the medial margin of the contact area to the medial margin of the rotator cuff attachment onto the humerus was 18.4 ± 2.5 mm or 84 % ± 14 % of the glenoid width with the arm at 60° of abduction to the scapula or 90° of abduction to the trunk.
Omori et al,
in an independent research measuring the width of the glenoid track in live shoulders,
using a semi-dynamic method,
reported the width of the glenoid track the arm abducted at 90° was 85 % ± 12 % of the glenoid width.
.
COMPARISON OF THE CONCEPTS:
Both these concepts (i.e.
glenoid tracks and engaging Hill Sachs lesions) are complementary concepts that evaluate the interaction of bipolar bone loss during dynamic shoulder function. Dynamic intraoperative assessment,
for engagement,
is always performed before repairing the Bankart lesion.
However,
this more often than not leads to over-diagnosis of as ligamentous insufficiency usually permits the HH to translate anteriorly,
thus facilitating engagement of the humeral defect with the glenoid rim.
On the other hand,
arthroscopic evaluation after the completion of a Bankart repair can put the repair at risk by overstressing the newly repaired capsulolabral complex in abduction and external rotation,
thus,
compromising the repair itself.
.
In summary,
arthroscopic techniques, provide qualitative information about Hill-Sachs engagement.
However,
by general consensus,
it is now believed that engagement must be quantified with the help of imaging.
.
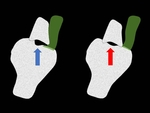
QUANTIFYING BIPOLAR BONE LOSS: (Fig. 6 ,
Fig. 7)
Currently evaluation of the GT,
in an attempt to quantify bone loss,
is employed in the preoperative evaluation of patients.
The evaluation of the GT can be performed using 3D CT scans of MRI.
The rationale of this evaluation is based on the fact that the width of the GT decreases in the presence of a glenoid bone defect.
.
At our institution,
CT scans are routinely prescribed for the evaluation of glenoid bone loss.
In all our patients,
we ensure imaging of both shoulders using bone algorithms to ensure comparison between normal and pathological sides.
After obtaining a scan of the shoulder,
post-processing techniques with volume rendering of the joints is performed at the workstation.
The glenoid and the humerus are separated to ensure individual visualization of these structures.
.
An en face image of the glenoid is assessed first,
with the contralateral glenoid serving as a reference.
The greatest horizontal width of the glenoid is established and the difference is calculated (d).
.
The posterior view of the humerus is assessed next.
The medial margin of the footprint of the rotator cuff and the Hill-Sachs lesion is identified. A straight line,
measuring 83 % of the glenoid width,
is placed from the medial margin of the rotator cuff footprint.
.
In the absence of a bony glenoid defect,
this line represents the medial margin of the glenoid track.
In case of a glenoid defect,
the distance "d" is subtracted from the 83 % line to obtain the medial margin of the true glenoid track.
If the HSL is located within the glenoid track,
it is referred to as a “non-engaging” Hill-Sachs lesion; while if it extends medially over the medial margin of the glenoid track,
it is referred to as an “engaging” HSL.
.
A bony bridge is usually observed between the rotator cuff attachments and the medial margin of the HSL.
The width of this bridge together with the width of the HSL amounts to the Hill-Sachs Interval (HSI).
The medial margin of the HSI is the critical point in determining if a Hill-Sachs lesion is non-engaging or engaging.
.
TREATMENT OPTIONS
It is believed that anterior instability with glenoid bone loss of ≥ 25 % (of the inferior glenoid diameter),
regardless of the dimension of the Hill-Sachs lesion,
needs treatment with a bone graft to the glenoid.
The bone graft widens the glenoid track significantly in all cases,
to an extent that in virtually all cases,
the Hill-Sachs lesion cannot go off the glenoid track.
In rare cases where the Hill-Sachs still goes off the glenoid track post-grafting,
the surgeon would consider concomitant bone-grafting of the Hill-Sachs lesion or “remplissage” of the Hill-Sachs.
.
Most authors prefer the Latarjet procedure in cases of bipolar bone loss.
In this procedure,
a coracoid bone graft is used which provides stability from the sling effect of the conjoined tendon.
Thus the combination of glenoid track enlargement and the sling effect,
the Latarjet procedure proves effective even in large degrees of bipolar bone loss,
without having to resort to additional humeral-sided procedures (humeral bone graft or “remplissage).
.
In cases with glenoid bone loss <25 % of the inferior glenoid diameter,
the Hill-Sachs lesion is usually small or absent.
In such cases,
an arthroscopic Bankart repair is performed.
.
Occasionally,
a large Hill-Sachs defect may be associated with a glenoid that has a minimal bone loss.
In such cases,
the width of the Hill-Sachs Interval (Hill-Sachs lesion plus bone bridge) must be determined.
If the HSI width is >83 % of the inferior glenoid diameter,
arthroscopic remplissage is added to the arthroscopic Bankart repair.
With remplissage,
the humeral bone defect is filled with the infraspinatus tendon,
arthroscopically.
In certain high-risk collision athletes,
the surgeon may choose to do a Latarjet procedure,
even with lesser degrees of bone loss,
to reduce the chance of recurrent instability