Normal Variants of the Shoulder:
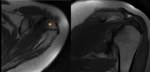
Os Acromiale (Fig.
1)
- Resulting from failure of fusion of the ossification centers at the acromial apophysis and base of the acromion
- Present in 7-15% of the population and bilateral in ~ 60% of cases
- Often asymptomatic,
though can lead to pain,
instability,
or rotator cuff impingement,
best diagnosed on shoulder MR
- In symptomatic patients marrow edema and irregularity of the surface interface at the synchondrosis suggest motion
- Mimics an acromion fracture
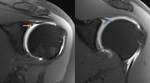
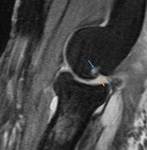
Sublabral Recess (Fig.
2)
- Recess between the superior portion of the glenoid fossa and biceps-labral complex
- Located superiorly between the 11-1 o'clock position at the insertion of the biceps tendon
- Increased signal intensity curves medially following the contour of the superior glenoid rim
- If high signal is seen extending posterior to the biceps anchor or laterally-indicative of SLAP tear
- Mimics a SLAP-type labral tear
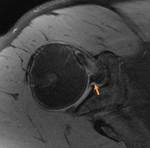
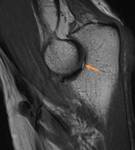
Sublabral Foramen (Figs.
3)
- Focally detached portion of the anterosuperior labrum at the 1-3 o'clock position from the underlying glenoid rim
- Occurs anterior to the biceps anchor
- Present in ~ 11-12% of the population
- Delineated from a sublabral recess and SLAP tear by origin,
extent of involvement,
and morphology
- Mimics a labral tear
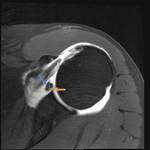
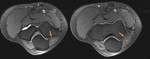
Buford Complex (Fig.
4)
- Congenital anatomic variant with a cord like,
thickened middle glenohumeral ligament and absence of the anterosuperior labrum,
generally from the 1-3 o'clock position
- Present in 1.5-2% of the population
- Remaining portion of the labrum is unaffected
- Be warry of a labral variant anytime high signal intensity is seen along the superior glenoid rim
- Mimics a displaced labral tear
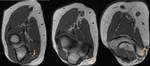
Cystic Change of the Bare Area (Fig.
5)
- Dorsal humeral head cysts located dorsally at the bare bone area of the anatomic neck
- Common incidental finding present in 10-35% of the population
- No association with rotator cuff pathology or osteoarthritis
- Not to be confused with cysts involving the greater and lesser tuberosities,
underlying the supraspinatus and subscapularis tendon attachment sites respectively,
which are associated with rotator cuff pathology
Glenoid Bare Area (Fig.
6)
- Normal physiologic bare area devoid of articular cartilage
- Most frequently involves the central glenoid fossa
- Commonly used anatomic landmark arthroscopically
- Incidence of 88% in cadaveric specimens
- Mimics a focal,
full-thickness articular cartilage defect
Normal Variants of the Elbow:
Capitellar Pseudodefect (Fig.
7 & 8)
- Frequent finding depicted by a change in contour of the posterior aspect of the distal humerus with a trough-like indentation at the junction of capitellum and lateral epicondyle posterolaterally
- Nonarticulating structure devoid of cartilage
- Best visualized on sagittal and posterior coronal MR images
- Mimics an osteochondral defect,
though these generally occur anterolaterally and demonstrate marrow edema
Olecranon Pseudodefect (Fig.
9)
- Created by inward tapering of the trochlear groove at the junction of the coronoid process and olecranon resulting in small cortical notches
- Characteristic location typically with absence of surrounding signal abnormality
- Small in size measuring up to 7 mm
- Mimics an osteochondral defect or loose body
Anconeus Epitrochlearis (Fig.
10)
- Accessory muscle extending from the medial cortex of the olecranon to the inferior surface of the medial epicondyle,
superficial to the ulnar nerve
- Present in ~ 11% of the population from cadaveric studies
- Believed that the cubital tunnel retinaculum represents the remnant anconeus epitrochlearis
- Most frequently incidentally discovered in asymptomatic individuals,
however can be a cause of cubital tunnel syndrome due to compression of the ulnar nerve
- Must be closely distinguished from the flexor carpi ulnaris
Ulnar Transposition (Fig.
11)
- Ulnar nerve transposition surgery is performed for relief from a variety of causes leading to cubital tunnel syndrome
- Submuscular: ulnar nerve runs anterior to the medial epicondyle in the fat between the brachialis and flexor-pronator muscle
- Intramuscular: ulnar nerve runs within the flexor-pronator muscle mass
- Subcutaneous: ulnar nerve runs superficial to the flexor-pronator muscle mass within the subcutaneous fat
- In the absence of appropriate clinically history,
can mimic ulnar nerve subluxation or dislocation which can be seen with various etiologies including laxity or congential absence of the arcuate ligament
Normal Variants of the Hip:
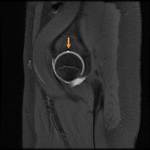
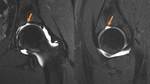
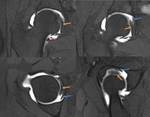
Pseudodefect of acetabular cartilage (supraacetabular fossa) (Fig.
12, 13,
& 15)
- Variant of the acetabular roof representing a focal subchondral bone defect
- Present in ~ 10% of the population
- Located at the 12 o'clock position on coronal and sagittal imaging,
entirely separated from the acetabular notch
- Always covered with articular hyaline cartilage
- Two types: Type 1 fills with contrast on MR arthrogram; Type 2 is filled with cartilage
- Mimics an osteochondral defect
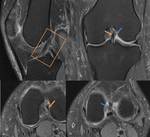
Stellate Crease (Fig.
14 & 15)
- Stellate shaped,
hence the name,
deficient area of hyaline cartilage within the acetabular articular surface
- Located at the anterosuperior acetabulum in continuity with the acetabular notch,
medial to the supraacetabular fossa
- Can appear irregular mimicking an osteochondral defect or mistaken for early chondromalacia
- Clean margins and lack of adjacent marrow signal abnormality help distinguish this entity
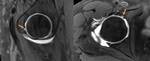
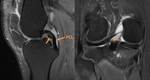
Ligamentum Teres (Fig.
16,
17,
& 19)
- Ligament of the hip which can appear striated,
multi-bundled,
and/or bilobed
- Attaches distally and medially to the transverse ligament of the acetabulum and proximally and laterally to the fovea capitis
- Thought to provide some intrinsic stability to the hip joint
- When torn can be a cause of hip pain and locking
- Delineation of normal vs.
partially torn ligamentum teres is difficult in many cases,
often with poor arthroscopic correlation
- Presence of a medial plica can be confused for ligamentum teres pathology
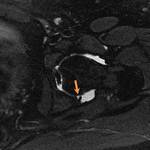
Pectinofoveal Fold (Fig.
18 & 19)
- Normal intra-articular structure of the hip
- Present in ~95% of MR hip arthrogram patients
- Can vary in its appearance and attachment site
- Inserts onto the hip capsule in ~75% and proximal femur in remaining cases
- No symptomatic potential in contrast to hip plica which can become trapped between adjacent structures
- Mimics other normal synovial reflections/hip plica,
however distinction is determined solely upon its classic location
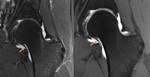
Sublabral Sulcus (Fig. 20 & 21)
- Smoothly marginated cleft of increased signal formed where a partially separated labrum meets the adjacent articular cartilage
- Present in ~ 25% of the population
- If 3 o'clock is used as anterior in position these are located at the 4 o'clock position
- Posterosuperior and anterosuperior are most common occurring with a similar incidence (44-48%),
posteroinferior and anteroinferior are far less common (< 5% each)
- Mimics a labral tear requiring careful differentiation,
particularly when located anteriorly where labral tears are most common
Normal Variants of the Knee:
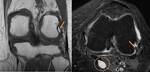
Two Discrete Bands of Normal ACL (Fig.
22)
- ACL is an intraarticular extrasynovial ligament consisting of two synergistic fiber bundles coursing obliquely within the intercondylar fossa
- Originates from the posteromedial corner of the medial aspect of the lateral femoral condyle
- Attaches to a fossa anterior and lateral to the anterior tibial spine
- Bundles are named according to their respective tibial attachment
- Smaller anteromedial bundle originates more medial and superior on the lateral femoral condyle
- Larger posterolateral bundle originates more lateral and distal on the lateral femoral condyle
ACL Reconstruction (Fig.
23)
- Two most common ACL reconstructions performed: autologous bone-patella tendon-bone graft & the autologous four-strand hamstring graft consisting of the semitendinosus and gracilis tendons
- These primary techniques replace only the anteromedial bundle,
whereas the newer double bundle technique replaces both anteromedial and posterolateral bundles
- May demonstrate intermediate signal intensity on short-TE sequences up to 12 months with normal low signal intensity > 12 months
- Thorough evaluation of the femoral and tibial tunnels is crucial in assessing for graft isometry and possible impingement,
best demonstrated on sagittal and coronal imaging
- Susceptibility to injury is greatest during the remodeling process (4-8 months post-op)
- Typical complications include graft laxity/tear,
impingement,
arthrofibrosis,
cystic degeneration,
ganglion formation,
and intraarticular loose bodies
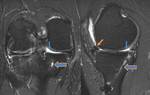
Ligaments of Humphrey and Wrisberg (Fig.
24 & 25)
- Discrepancy exists in the literature as to whether the meniscofemoral ligament is one ligament with two discrete bands vs two distinct ligaments
- They arise from the posterior horn of the lateral meniscus and attach to the lateral aspect of the medial femoral condyle
- The anterior meniscofemoral ligament (Humphrey) is located anterior to the PCL with the posterior meniscofemoral ligament (Wrisberg) posterior to the PCL
- Incidence of at least one meniscofemoral ligament ranges in anatomic studies from 65-95%,
with the ligament of Wrisberg most frequently present
- Mimics a posterior horn lateral meniscal tear at its meniscal attachment
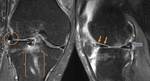
Meniscal Transplant/Allograft (Fig.
26 & 27)
- Accurate sizing is key for graft survival and cartilage protection/preservation
- Peripheral allograft is sutured to the joint capsule and meniscal horns are transfixed either with small bone plugs or soft tissue fixation with sutures
- Allograft demonstrates signal characteristics mirroring the native meniscus,
though focal high-signal intensity foci are commonly visualized and considered normal
- Surgically related micrometallic artifacts are visualized along the meniscocapsular junction,
a distinguishing feature of a meniscal allograft
- Meniscal allograft body can frequently demonstrate some degree of minor radial displacement to frank dislocation into the peripheral gutters
- > radial displacement is seen with medial allograft transplants compared with lateral
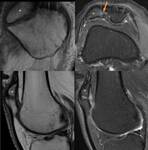
Cyamella (Fig.
28)
- Sesamoid bone (accessory ossicle) located within the popliteus tendon at lateral aspect of the distal femur
- Rare is humans ~ 2-3% in cadaveric studies, much more common in primates
- Vary considerably in size
- Can be confused with a fabella which is a sesamoid located with the lateral head of the gastrocnemius muscle
- Can also be mistaken for sequela of a posterolateral corner injury,
detached osteophyte,
or osteochondromatosis
Bipartite Patella (Fig.
29)
- Results from failure of fusion of secondary ossification centers
- Present in 2-3% of the population
- Frequently seen bilaterally; 3 Subtypes
- Type 1: 1% of cases located at the inferior patellar pole
- Type 2: 20% of cases located at lateral margin of the patella
- Type 3: 75% of cases located superolaterally
- Marrow edema and abnormal signal across the synchondrosis is frequently demonstrated in symptomatic cases
- Mimics an acute fracture