Keywords:
Musculoskeletal spine, MR, Imaging sequences, Congenital
Authors:
V. A. Mutafchiyski, B. Milev; Sofia/BG
DOI:
10.26044/essr2019/P-0061
Background
Klippel-Feil syndrome is a complex heterogeneous entity that results in cervical vertebral fusion.
Two or more non-segmented cervical vertebrae are usually sufficient for diagnosis.[1] There is a recognised female predilection.
Klippel-Feil syndrome has an incidence of 1:40,000-42,000.
The classic clinical triad of a short neck,
low hairline,
and restricted neck motion is considered to be present in <50% of patients with this syndrome.
[2] It is believed to result from faulty segmentation along the embryo’s developing axis during the third to eight weeks of gestation.
Klippel-Feil syndrome occurs as the result of a sporadic mutation or as an inherited disorder,
with variable expression.
Presumed causative factors include teratogens and maternal alcoholism.
SGMI is the first KFS gene identified,
found on chromosome 8.
[4] There are two classifications.
Original classification (described by Maurice Klippel and Andre Feil): three types grouped depending on the extent and location of vertebral fusion as well as associated vertebral abnormalities.
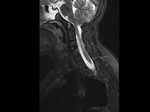
Type I: fusion of many cervical and upper thoracic vertebra.
[Fig.1] Type II: fusion of two or three vertebrae with associated hemivertebrae,
occipito-atlantal fusion or other cervical spine abnormalities.
Type III: cervical fusion with lower thoracic or lumbar vertebral fusion.
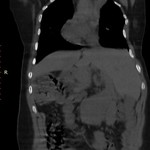
[2] Updated classification (by Clarke et al ) grouped by patterns of inheritance,
associated anomalies and the axial level of the most anterior fusion.
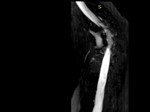
[Fig.2] [3] Neurologic symptoms developing later in life are due to development of degenerative disc disease,
instability and spinal stenosis at adjacent segments.[ Fig.3] [4] Patients may present with neck or radicular pain,
slowly progressive or acute myelopathy,
ataxia,
hyperreflexia,
and upper and lower motor neuron dysfunction.
[5] Mirror movements may occur in patients with KFS who have associated cervicomedullary neuroschisis.
This phenomenon is characterized by voluntary movements in one extremity mimicked by involuntary movements in the other with a central plane of symmetry.
[6] Brainstem compression from basilar invagination may result in obstructive hydrocephalus,
autonomic dysfunction,
with labile blood pressure,
arrhythmias,
respiratory depression and sudden death,
and vascular compromise,
with resultant neurologic deficits,
vertebrobasilar insufficiency or transient ischemic attacks.
[7]