A 71-year-old woman came to our observation after suffering from right shoulder pain for about 2 years.
Pain started worsening in the last 4 months with sudden onset of global functional limitation,
in particular considering abduction (limited to 90°) and intrarotation (limited to “hand on side”) movements.
The patient has never experienced joint loking episodes.
No significant traumatic events have been reported in the anamnestic reconstruction.
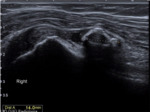
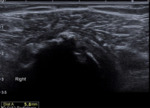
After performing the ultrasound evaluation,
we demonstrated thickening of both walls of subacromial bursa with fluid distension and a partially calcified loose body of about 14 mm in diameter (Fig.
1-2).
As a collateral finding we demonstrated a lenticular 6 mm long calcification in the context of the subscapular tendon fibers in pre-insertional location (Fig.3).
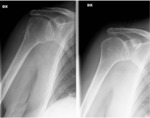
To better evaluate the shoulder structures and confirm our ecographic evaluation we performed an X-ray exam which demonstrated: sub-cortical bone sclerosis of the humeral trochitis,
as a sign of rotators cuff’s chronic sufferance; humeral head sopraelevation and a faint round calcification projectively localized near the bicipital groove (Fig.
4).
The last finding confirmed the ultrasound evidence with a preliminary diagnosis of osteo-chondromatosic loose body.
After discussing with the patient the ultrasound and radiological iconographic findings and obtaining informed consent,
the patient agreed with the proposed procedure of minimally invasive ultrasound-guided loose body removal.
The patient was prepared with skin disinfection and set up of sterile field around the operation site.
The procedure was performed using sterile probe cover,
sterile gloves and mask.
We reached the loose body with a 22-25 G needle with echo-guided technique (Fig.5 - video 1).
Local anesthesia was performed with 2-3 ml of Lidocaine Hydrochloride at 2% and 2-3 ml of Naropin.
A scalpel was used to create a subcentimetric skin incision at the level of the sub-acromial bursa anterior recess.
The loose body was then extracted using Halsted-mosquito straight surgical forceps.
No complications occurred during and after the procedure.
The cutaneous access was medicated with Steri-strip.
NSAIDs were prescribed if needed and the patient was told to take antibiotic prophylaxis with Amoxicillin and clavulanic acid 1g one tablet every 12 hours for six days,
refraining from manual labor for 5-6 days.
To complete the procedure,
we performed an US-guided infiltration of the glenohumeral joint with lateral access and a 23G needle,
injecting an 8 cc solution of lidocaine,
naropine,
triacort and medium-low molecular weight ialuronic acid (0.8%).
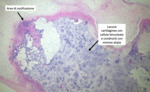
The removed loose body was macroscopically compatible with an osteochondral nodule of synovial origin and was sent to the Department of Pathological Anatomy for histological examination.
The latter confirmed the presence of hyaline cartilage tissue with proliferation of small blood vessels and inflammatory infiltrate with a central calcific matrix,
findings consistent for type II osteochondromatosis body (Fig.
6).