Keywords:
Outcomes, Education and training, Imaging sequences, Education, MR, Conventional radiography, Musculoskeletal system, Musculoskeletal spine, Musculoskeletal joint
Authors:
M. Haris1, H. Gupta2; 1Halifax/UK, 2Leeds/UK
DOI:
10.26044/essr2019/P-0080
Background
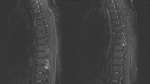
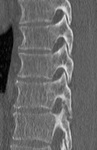
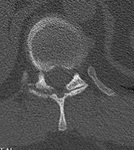
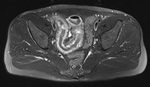
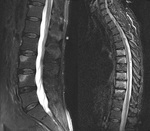
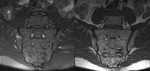
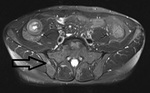
Spondyloarthritis encompasses a number of inflammatory conditions with some shared common features.
Spondyloarthropathies are broadly divided into those predominantly affecting the axial skeleton,
which will be our focus for this exhibit and those with a peripheral skeletal predominance.
Spondyloarthritis has a reported prevalance of 0.8%-1.7% in Western Europe and is more common than rheumatoid arthritis (1).
Despite this,
prompt diagnosis of spondyloarthritis remains an ongoing challenge.
Several studies have demonstrated a mean diagnostic dealy of axial spondyloarthropathy ranging from 2-8 years,
with one study showing only around 15% of cases recieving a diagnosis within three months of initial presentation (2).
Several reasons have been hypothesised for this delay,
including misdiagnosis of low back pain as mechanical rather than inflammatory especially in a non-specialist clinical setting.
Other causes for diagnostic delay include atypical clinical presentation and missed radiographic or MR findings.
This delay can increase patient anxiety and often results in the use of unnecessary resources to try and reach a diagnosis and delay treatment in cases with active inflammation.
We include examples where patients did not present with the typical history and symptoms of spondyloparthropathy and therefore had non sacroiliac joint protocol imaging on first presentation and how findings seen led to raising the posssibility and allow for further conclusive imaging and diagnosis.