1.
Congenital lesion
A.
Spinal dysraphism
Types (by defect in the overlying skin)
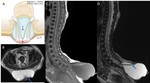
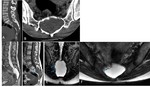
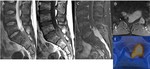
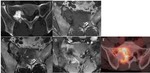
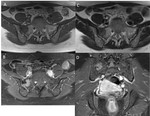
- Open: Myelomeningocele (Fig.
1),
Myelocele
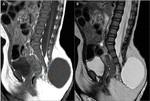
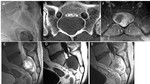
- Close: Lipomyelomeningocele (Fig.
2),
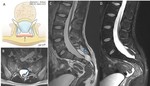
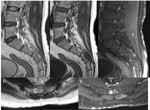
Lipomyelocele (Fig.
3),
Meningocele
B.
Tumorous condition
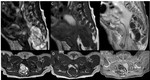
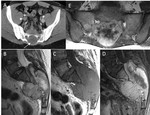
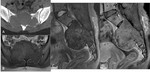
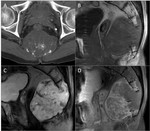
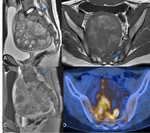
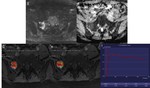
Sacoccygeal teratoma (Fig.
4)
Meningeal cyst (perineural cyst,
Tarlov cyst) (Fig.
5)
- Common developmental lesions (5%)
- Abnormal dilatations of the meninges within the sacral canal or
foramina by sliding of the meninges from a defective dura mater
- Classification of meningeal cysts
Type 1 – Extradural meningeal cysts (no neural tissue)
1A – Arachnoid cyst
1B – Sacromeningocele
Type 2 – Extradural meningeal cysts containing neural tissue
Perineural cyst or Tarlov cyst
Type 3 – Intradural meningeal cysts
2. Sacrococcygeal canal tumors
A.
Schwannoma (Fig.
6) / Neurofibroma (Fig.
7)
- Benign,
slowly-growing tumors that arise from myelin sheath of lower
lumbar and sacral dorsal sensor nerve roots
- Multiple neurofibromas are characteristic of von Recklinghausen’s
neurofibromatosis with potential for malignant transformation.
- CT: circumscribed osteolysis,
enlargement of a sacral foramen,
fine
sclerotic rim
- MRI: characteristic on T2 (target sign),
contrast enhancement
B. Ependymoma (Fig.
8)
- Arise from ependymal cells within the central canal of the spinal cord or
ependymal glia within the filum terminale
- Intramedullary type – most often in the cervical spine
- Myxopapillary type – conus medullaris or filum terminale
- Vascular soft-tissue masses with areas of hemorrhage and mucinous
degeneration
- Bony destruction but rarely metastasizes
- CT: Neural foramen widening
- MRI: Iso-SI to spinal cord on T1/T2WI,
Contrast enhancement
C.
Myeloid sarcoma (granulocytic sarcoma) (Fig.
9)
- Also known as chloroma or extramedullary myeloblastoma
- Rare malignant extramedullary solid tumor composed of primitive
precursor cells of the granulocytic series of WBC
- Associated with AML,
CML and other myeloproliferative disorders
- Thoracic (73%) > Lumbar (34%) > Sacral (23%) > Cervical (5%)
3. Sacrococcygeal bone tumors
- Metastasis far more common than primary tumors
- Evaluation according to epidermiology,
topographic features and other characteristic features
A.
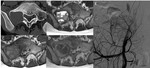
Primary benign tumor – Giant cell tumor (Fig.
10)
- Second most common primary sacral tumor after chordoma
- 2nd- 4th decades of life,
Male : Female = 1 : 2
- Locally aggressive
- Often eccentrically located.
- May extend across the sacroiliac joint.
- Very vascular neoplasm
- CT: Lytic,
expansile and destructive mass,
thin sclerostic rim,
low
attenuation areas (necrosis)
- MRI: Intermediate SI on both T1 and T2WI,
may contain hemorrhage
or necrosis
B.
Primary benign tumor – Aneurysmal bone cyst (Fig.11)
- Expansile lesions with blood-filled cystic areas
- Detected by the 2nd decades (80%)
- Not actual neoplasms,
but reactive lesions
results from trauma or coexist with other bone lesions
- Fluid-fluid level with internal hemorrhage
- Lack of mineralization
- May involvement of adjacent vertebra
- MRI: Low/intermediate SI on T2WI
C.
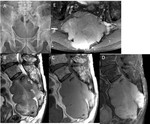
Primary malignant tumor – Chordoma (Fig.
12)
- Originate from embryonic remnants of the primitive notochord
- Remnants persist within the cranial and caudal area of the spine
(sacrum 60%)
- Always occur in a midline or paramedian location
- Most commonly found 4th-7th decades
- Locally aggressive,
but uncommon metastasis (7-14%)
- may involve adjacent vertebra and SI joint
- Osteolytic,
destructive soft tissue mass with internal calcifications
- Collar-button or mushroom appearance
- Fluid,
gelatinous mucoid materials → heterogeneous high SI on T2WI
D.
Primary malignant tumor – Osteosarcoma (Fig.
13)
- M/C nonlymphoproliferative primary malignant bone tumor
- But,
rarely affects the spine
- 5th common primary malignant tumor of the sacrum (4%)
- Primary (3rd-4th decades)
- Secondary (7th decades) to Paget’s disease,
osteonecrosis,
chronic osteomyelitis and radiation therapy.
- Arises in the posterior elements (79%),
may involve adjacent vertebra
- MRI: Low SI on T1 & T2 d/t mineralized/osteoid matrix
E.
Primary malignant tumor – Chondrosarcoma (Fig.
14)
- 2nd common nonlymphoproliferative primary malignant tumor of spine
- But,
rarely affects sacrum
- M > F (4 :1),
common at 4th-8th decades
- Arises in the posterior elements (85%),
may involve adjacent vertebra
- MRI: High SI on T2WI,
Rings and arcs enhancement pattern
F.
Hematologic malignancy – Ewing sarcoma (Fig.
15)
- Primary vertebral Ewing sarcoma,
rare(3.5-15%)
- Sacrum is most frequently involved (55%) / sacral ala (69%)
- Metastatic involvement is more common
- M/C nonlymphoproliferative primary malignant tumor of the spine in
children
- Small round cell sarcoma
- M/C – 2nd decade,
M > F (1.5 :1)
- Soft-tissue mass usually larger than intra-osseous component
G.
Hematologic malignancy – Plasmacytoma (Fig.
16)
- Multiple myeloma
- The second common primary malignant neoplasm of the sacrum.
- Malignant monoclonal proliferation of plasma cells of the bone marrow
- M/C – 6th and 7th decades,
M > F (2 :1)
- Solitary,
larger,
osteolytic form in younger patients
H.
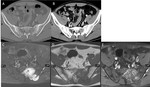
Metastasis (Fig.
17-18)
- Most common sacral neoplasm
(25 times more common than primary bone tumors)
- Primary site
Breast > prostate > lung > kidney > uterus > thyroid > stomach
- By hematogenous,
lymphatic spread,
direct extension
- Osteolytic lesion : lung cancer,
breast cancer
- Osteoblastic lesion : prostate cancer,
medulloblastoma
- DWI and quantitative evaluation with ADC maps
-provide important information about vertebral bone marrow lesions
for differentiating malignant lesion,
particularly in oncological patients