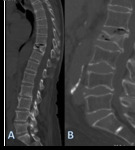
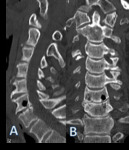
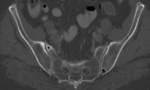
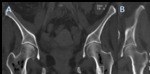
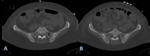
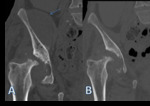
Plain film radiography has just a limited role in detecting the presence of intraosseous air.
CT is the most useful imaging method to characterize the presence of intraosseous air and to characterize its extension.
MRI can also detect the presence of gas,
although evidence in its performance in comparison to CT is still lacking.
In the appropriate clinical setting,
presence of intramedullary bone air in the absence of prior surgery,
other invasive procedures or trauma,
raises serious concern for emphysematous osteomyelitis.
Besides excluding these diseases,
the radiologist must be aware of the existence of pneumatocysts,
which are more common in the illium and sacrum,
near the sacro-iliac joints and in the vertebrae and usually present a sclerotic rim.
Kummel disease and lymphangiomiomatosis of the bone must also be excluded,
but the clinical context usually makes its diagnosis straightforward.
Pelvis,
femur,
tibia and thoracolumbar vertebrae have been described as the most common sites of involvement by emphysematous osteomyelitis.
In the appendicular skeleton,
the presence of gas in the absence of invasive procedures or compound fracture is considerered pathognomonic of emphysematous osteomyielitis.
In the vertebrae,
differentiation between osteonecrosis (Kummel disease),
pneumatocyst and emphysematous osteomyelitis is paramount:
- In non-infective conditions,
the distribution of gas is linear,
well demarcated,
band-like or triangular.
- In infective conditions,
the distribution of gas is uneven,
bubbly and eventually with extension into adjacent soft tissue.
Although the high number of differential diagnosis,
the presence of extensive intraosseous gas,
bone marrow edema and adjacent fluid collections increase the possibility of emphysematous osteomyelitis in the adequate clinical setting.