KNEE JOINT
- Joints: two condylar joints between femur and tibia; saddle joint between patella and femur
- Blood supply: main supply are the genicular branches of the popliteal artery
- Nerve supply: branches from the femoral,
tibial,
common peroneal and obturator nerves
- Movements: flexion to 150°,
extension to 5-10° hyperextension; rotation while in the flexed position to 10° actively and 60° passively
1. DISTAL FEMORAL FRACTURE
- ≈ 10% of all femoral fractures
- Bimodal distribution: high energy blunt trauma in young people; fall in elderly people
1.1 IMAGING
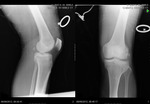
1.1.1 CONVENTIONAL RADIOGRAPHY
- Two imaging planes (antero-posterior and lateral)
- Fractures can be difficult to identify
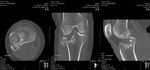
1.1.2 COMPUTED TOMOGRAPHY
- Evaluate for radiographically occult fractures or if the fracture is intra-articular and complex
- 3D volumetric reconstructions: useful when dealing with comminuted fractures
- Identify vascular or neurologic involvement: very important (injury to the popliteal artery and sciatic nerve are common; in doubt,
consider angiography)
1.2 AO/OTA CLASSIFICATION (2018)
Three types,
according to their relationship to the joint:
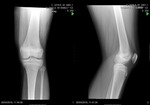
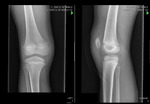
- 33A – Extra-articular fracture (Fig. 1)
o 33A1: avulsion fracture
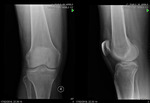
o 33A2: simple fracture (Fig. 4, Fig. 5)
o 33A3: wedge or multifragmentary fracture
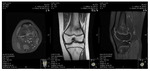
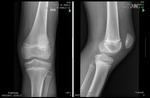
- 33B - Partial articular fracture (Fig. 2)
o 33B1 lateral condyle,
sagittal fracture
o 33B2 medial condyle,
sagittal fracture
o 33B3 frontal/coronal fracture
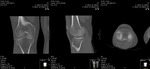
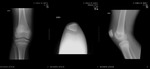
- 33C - Complete articular fracture (Fig. 3)
o 33C1 simple articular,
simple metaphyseal fracture
o 33C2 simple articular,
wedge or multifragmentary metaphyseal fracture
o 33C3 multifragmentary articular fracture,
simple,
wedge or multifragmentary metaphyseal fracture
2.
PROXIMAL TIBIAL FRACTURES
2.1 TIBIAL PLATEAU FRACTURES
- Bimodal distribution: males in 40s (high-energy trauma); females in 70s (falls)
- Trauma usually with the knee in valgus position
- Lateral plateau involvement: ≈ 80%
- Meniscal lesions: ≈ 50%
- Ligament lesions (cruciate and collateral ligaments): ≈10-25%
- Lipohemarthrosis may be present
2.1.1 IMAGING
2.1.1.1 CONVENTIONAL RADIOGRAPHY
- Severity is often underestimated
- Fractures may be radiographically occult
- Lateral oblique view makes evaluation easier
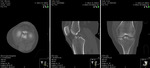
2.1.1.2 COMPUTED TOMOGRAPHY
- Identification of radiographically occult fractures,
better characterization of the degree of tibial plateau depression and definition of the fracture plane
- Pre-operative evaluation
- Hemarthrosis: fat (marrow)-fluid (blood) level on cross-table lateral view is usually visualized
2.1.1.3 ANGIO-CT,
ANGIOGRAPHY OR DOPPLER IMAGING
- If popliteal vein or popliteal artery damage is suspected
2.1.1.4 MAGNETIC RESONANCE IMAGING
- Imaging modality of choice to evaluate tibial plateau fractures (fracture line,
ligaments,
meniscus)
2.1.2 SCHATZKER CLASSIFICATION (Fig. 6)
- Type I – lateral femoral condyle is driven into articular surface of tibial plateau
- Type II – split wedge depression of the lateral tibial plateau (Fig. 9, Fig. 10, Fig. 11)
- Type III – pure central depression of the lateral tibial plateau; no lateral wedge and lateral cortex is intact
o IIIa: with lateral depression
o IIIb: with central depression
- Type IV – split wedge of the medial tibial plateau (Fig. 12)
- Type V – bicondylar tibial plateau fracture; may have an associated fracture of the intercondylar eminence (metaphysis and diaphysis retain continuity) ( Fig. 13)
- Type VI – tibial plateau fracture with dissociation of the tibial metaphysis and diaphysis (transverse or oblique fracture of proximal tibia resulting in dissociation of the metaphysis from the diaphysis)
2.2 TIBIAL EMINENCE FRACTURE
- Intra-articular fracture of the bony attachment of the anterior cruciate ligament on the tibia (in young people,
the ligaments are stronger than their bony attachaments)
- More common in children during athletic activity (usually caused by forceful hyperextension of the knee or by a direct blow over distal end of femur with the knee flexed)
-
Typically involves separation of the tibial attachment of the anterior cruciate ligament (separation at the femoral attachment is rare)
-
Occur in 40% of tibial eminence fractures (meniscal injury,
collateral ligament injury,
capsular damage,
osteochondral fracture)
2.2.1 IMAGING
2.2.1.1 CONVENTIONAL RADIOGRAPHY
- Anteroposterior,
lateral (most useful for determining fracture displacement),
intercondylar and oblique (helpful in determining the extent of tibial plateau involvement) views
2.2.1.2 COMPUTED TOMOGRAPHY
- Useful for pre-operative planning
- Used when fracture displacement cannot be determined by plain radiographs
2.2.1.3 MAGNETIC RESONANCE IMAGING
- To determine associated ligamentous/meniscal damage
- Majority of fractures show no additional internal derangement (meniscal injuries)
- 15-37% of cases have associated intra-articular pathology
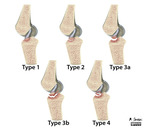
2.2.1.4 MODIFIED MEYERS AND MCKEEVER CLASSIFICATION (Fig. 14)
- Type I: minimally/nondisplaced fragment (< 3mm)
- Type II: minimally displaced with intact posterior hinge
- Type III: completely displaced:
o IIIa: involves small portion of the eminence
o IIIb: involves the majority of the eminence
- Type IV: comminuted avulsion or rotation of the fracture fragment (Fig. 15, Fig. 16)
3. PATELLAR FRACTURES
- 1% of all fractures
- Most common in 20-50 year-old patients
- Two-thirds of cases occur in males
- Usually post direct trauma to the patella or sudden forceful contraction of the quadriceps muscles in the context of a sports injury
3.1 IMAGING
3.1.1 CONVENTIONAL RADIOGRAPHY
- The best imaging study is a lateral view radiograph,
but it does not detect vertical or osteochondral fracture
- The axial projection of the patella allows better visualization of vertical fractures. Differential diagnosis with bipartite patella must be done
- Incomplete fractures could be difficult to detect because fracture line may not be obvious
3.1.2 COMPUTED TOMOGRAPHY
- Useful in comminuted fractures.
3.1.3 MAGNETIC RESONANCE IMAGING
- If there is high suspicion for an incomplete fracture (radiographically occult)
- To evaluate osteochondral fracture,
periosteal sleeve avulsion and if there is associated tendon and/or retinacular rupture
3.1.4 CLASSIFICATION (Fig. 17)
Patellar fractures are commonly classified according to their morphologic pattern and degree of displacement:
3.2 BIPARTITE/MULTIPARTITE PATELLA
- An important differential diagnosis of patellar fracture.
- Results from non-fusion of the accessory patellar ossification centre.
o Type I: at the inferior pole (5% of all lesions)
o Type II: at the lateral patellar margin (20%) (Fig. 26, Fig. 27)
o Type III: at the superolateral pole (75%) (Fig. 25)
3. AVULSION FRACTURES
3.1 STIEDA FRACTURES
- Bony avulsion injury of the medial femoral collateral ligament at the medial femoral condyle
3.2 PELLEGRINI-STIEDA LESION (Fig. 28)
- Ossified post-traumatic lesions at (or near) the medial femoral collateral ligament adjacent to the margin of the medial femoral condyle
- Stieda fracture is a presumed mechanism of injury
- Plain radiograph shows a calcification (few weeks after the initial injury) adjacent to the medial femoral condyle,
often linear or curvilinear and paralleling the femoral cortex
3.1 SEGOND FRACTURE
- Small avulsion fracture involving the superolateral surface of the proximal tibia
- Characteristic radiographic finding: small,
curvilinear or elliptic bone fragment projected parallel to the lateral aspect of the tibial plateau,
best seen on the anteroposterior view of the knee - lateral capsular sign
- Frequently associated with anterior cruciate ligament and meniscal tears
- Magnetic resonance imaging should be performed in all cases to evaluate associated ligamentous injury
3.1 REVERSE SEGOND FRACTURE (Fig. 29)
- Small avulsion fracture involving the superomedial surface of the proximal tibia
- Characteristic radiograph finding: small,
curvilinear or elliptic bone fragment projected parallel to the medial aspect of the tibial plateau,
best seen on the anteroposterior view of the knee
- Represents avulsion of the deep capsular component of the medial collateral ligament
- Associated with tears and avulsions of the posterior cruciate ligament from the posterior tibial plateau and tear of the medial meniscus
- Magnetic resonance imaging should be performed to evaluate associated ligamentous injury