1.
IMAGING
PLAIN RADIOGRAPHS
Plain radiographs are the modality dedicated for evaluation of the hip bones (developmental dysplasia) and the joint spaces (osseous intra-articular loose bodies).
Plain radiographs in internal SHS tend to be normal.
[3]
ULTRASOUND (US) EXAMINATION
US is performed with a 5–12-MHz linear transducer.
In some patients with larger body habitus,
the use of a 3–5-MHz curvilinear transducer may be indicated.
Static US evaluation
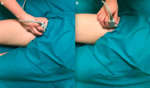
The patient lies supine on the examination bed with the hip in neutral position (extension and adduction).
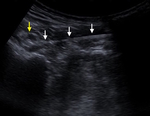
Place the transducer in the longitudinal and transverse planes in the anterior region of the hip. Fig. 1 Although infrequent in the presence of internal SHS,
anomalies such as iliopsoas bursitis (synovial thickening or hypoechoic fluid collection in a typical location,
which is lateral to the femoral vessels,
posteromedial to the iliopsoas muscle and tendon and anterior to the capsule of the hip joint),
paralabral cyst (paraarticular hypoechoic fluid collection),
iliopsoas tendinitis (thickening of the tendon,
hypoechogenicity,
loss of fibrillary pattern) and iliopsoas tendon tears (well-defined hypoechoic or anechoic intratendinous defects) should be systematically sought.
Do not mistake artifactual hypoechoic appearance of the tendon due to anisotropy for tendon pathology.
Use Colour or Power Doppler sonography to detect inflammation.
[3-6]
Dynamic US evaluation
Closely observe the movement of the PT and the medial iliac muscle.
1.
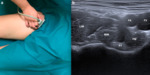
Neutral position: Place he transducer in an oblique plane just above the hip joint parallel to the pubic bone with the lateral end of the probe scanning the antero-inferior iliac spine.
In this neutral position the iliac muscle is located more laterally than the PT,
which lies anterior to the superior pubic ramus and posterior to the medial iliac muscle. Fig. 2
2.
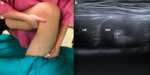
Flexion: Maintain the transducer in an oblique plane and fully flex the patients’ hip.
For optimal dynamic evaluation extreme flexion of the hip is needed.
During flexion the PT moves superficially along the medial side of the medial iliac muscle. Fig. 3
3.
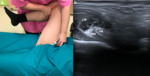
Frog leg position: Abduct and externally rotate the patient’s hip.
The PT and the medial iliac muscle rotate (counterclockwise on the right side and clockwise on the left side). Fig. 4 In this position the PT lies on the superior part of the medial iliac muscle,
which is now caught between the tendon and the superior pubic ramus. Fig. 5
4.
Return to neutral position: Adduct,
internally rotate and extend the patient’s hip.
In healthy individuals the PT glides back smoothly medially over the medial iliac muscle and ends its course on the pubic bone without a snap.
In patients with internal SHS the PT abruptly returns to its previous position with snapping against the superior pubic ramus,
producing an audible snap.
This snap usually occurs about midway to neutral position. Fig. 8 It is essential to correlate the timing of tendon snapping visible at US with the snapping sensation and,
even more importantly,
with the referred pain.
[3,
4,
6]
Tips
If the dynamic evaluation fails to produce a snap,
simply ask the patient to generate the hip movement that produces the snapping sensation.
In doubtful cases compare with the unaffected contralateral side.
[4,
5]
MAGNETIC RESOCANCE IMAGING (MRI)
Internal SHS is a dynamic phenomenon; therefore a static image cannot reliably identify the tendon as the etiology.
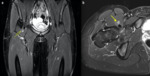
MRI can detect tendinopathy (tendon thickening,
high signal intensity on fluid-sensitive sequences) Fig. 6 and bursitis (enlarged bursa,
high signal intensity on fluid-sensitive sequences).
The additional value of MRI,
especially MR-arthrography is in detecting intra-articular pathology.
A negative US examination should always be followed by an MRI.
[6,
7]
2.
TREATMENT
When pain is not present,
treatment is not warranted.
When pain is present upon snapping,
treatment is conservative (activity modification,
rest,
stretching,
steroid injections,
oral anti-inflammatory medications,
physical therapy).
Most of the time,
patients experience relief with these measures.
If pain persists surgery (open or arthroscopic loosening or complete release of the tendon) can be considered.
[3,
4]
Ultrasound-guided local anesthetic and corticosteroid injection of the inflamed PT sheath or the iliopsoas bursa can provide quick symptomatic improvement in the professional dancers for who ‘time is money’.
The injection is performed using a freehand technique with the patient supine with the lower limb slightly extra-rotated.
The PT is localized in short-axis or long-axis using a linear transducer.
A 20-22 G needle is inserted next to the tendon using a lateral in-plane approach.
If there is preexisting fluid distention of the iliopsoas bursa,
then the needle is directed into the bursa.
A therapeutic mixture consisting of 5 mL 1% lidocaine,
1 mL of bupivacaine and 1 ml of triamcinolone is administered in the peritendinous soft tissue or into the bursa under sterile conditions.
When a bursa is present,
the steroid should be preferably injected therein.
The end point of the injection is direct distention of the iliopsoas bursa and/or the presence of microbubbles in a peritendinous distribution. Fig. 7 [3,
4,
8,
9]