Imaging Review:
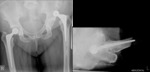
The pre-reduction plain radiographic films demonstrated a posteriorly dislocated left prosthetic femoral head (Fig. 1)
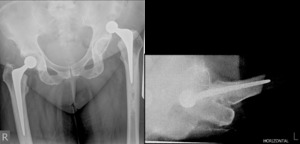
Fig. 1: AP and lateral plain radiographs demonstrating the posteriorly dislocated left hip prosthesis.
Although most metallic implants can be safely imaged with MRI,
their presence can cause significant artifacts that result in non-diagnostic images.
This is due to the consequential local field disturbances and large resonant frequency shifts.
Aside from the fact that metal has no signal on MRI and appears black,
these additional artifacts include signal voids (black areas) and signal pile-ups (bright areas),
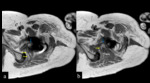
failure of adjacent fat suppression, and geometric distortion10 (Fig. 2).
Metal artefact reduction sequences (MARS) are used to reduce these artifacts on MRI.
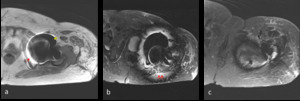
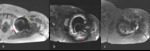
Fig. 2: Non metal-artifact suppression MRI demonstrating peri-prosthetic artifacts: (a) signal void (yellow arrow) and signal pile-up (red arrow) (b) failure of adjacent fat suppression on STIR sequence (red arrow) (c) peri-prosthetic geometric distortion.
For the purpose of identifying a suspected neurological pathology and to reduce metal induced artifacts from the hip prosthesis, axial and coronal T1-weighted and fat suppressed sequence with MARS,
were obtained.
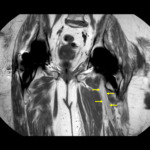
The images demonstrated an anteriorly displaced left sciatic nerve,
which was particularly evident when reviewed in conjuction with the coronal plane (Fig. 3).
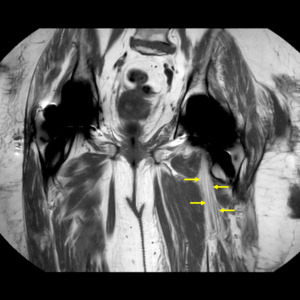
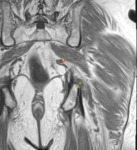
Fig. 3: Coronal T1-weighted MARS, demonstrating the anteriorly displaced left sciatic nerve (yellow arrows) as reflected by it's positional plane adjacent to the left lesser trochanter.
On further review,
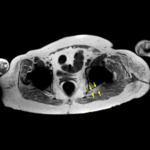
it was noticed that the left sciatic nerve had exited the greater sciatic foramen more horizontally and anteriorly than normal,
with it's projection towards the prosthetic femoral neck (Fig. 4).
This is thought to be secondary to the displacement of the nerve that was being pulled anteriorly and upwards by the prothesis.
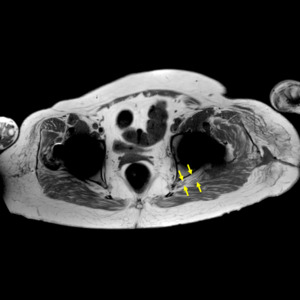
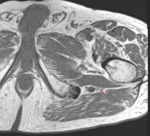
Fig. 4: Axial T1-weighted MARS demonstrating the left sciatic nerve (yellow arrows) exiting the greater sciatic foramen in a relatively horizontal and anterior course compared to the right side. This reflects the tension the nerve is subjected to by the entwinement.
At the level just superior to the ischial tuberosity,
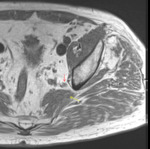
axial T1w MARS demonstrated a large anterior nerve bundle emerging on the medial aspect of the metal artefact (Fig. 5 a).
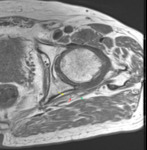
This is then rejoined with another posterior nerve bundle distally (Fig. 5 b).
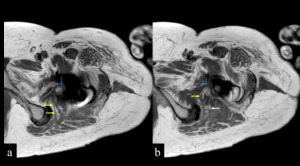
Fig. 5: Axial T1w MARS - (a) at the level of the inferior border of the left prosthetic femoral neck, demonstrating an anteriorly displaced nerve bundle (blue arrow) emerging medial to the metal artifact.
(b) A posterior nerve bundle (yellow arrows) is shown to course anteriorly to rejoin the thicker anterior bundle. The posterior femoral cutaneous nerve (white arrow) is identified.
These findings raised a high suspicion of splitting of the sciatic nerve and entwinement of the split anterior branch around the prosthetic femoral neck with subsequent rejoining of the nerve fibres distally.
Subsequent surgery confirmed that the anterior half of the sciatic nerve was entwined around the femoral neck prosthesis and displaced anteriorly,
confirming the MRI findings.
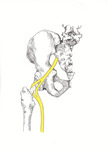
The anterior component was found to be under tension around the femoral neck while the remaining sciatic nerve was lying posteriorly (see illustrative diagram - Fig. 6).
Post-operatively,
the patient continued to experience sensory deficits,
dense motor palsy of the left foot and was discharged with a foot drop splint.
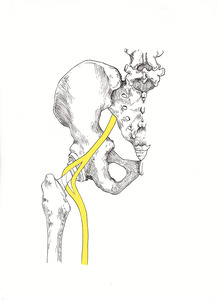
Fig. 6: Illustrative diagram by Caryn Koh - Posterior view of the left hip demonstrating splitting and entwinement of the left sciatic nerve around the femoral neck prosthesis.
The Sciatic Nerve :
The sciatic nerve is the largest nerve in the body measuring up to 2cm in thickness and is derived from the ventral rami of L4 - S3 spinal nerves,
containing both sensory and motor fibres.
It provides sensory innervations to the majority of the lower leg (with the exception of the medial margins of the leg and foot) and motor innervations to the posterior compartment of the thigh,
and anterior and posterior compartments of the leg and foot11.
Course :
The sciatic nerve exits the pelvis through the greater sciatic foramen,
and normally passes anteriorly across the inferior border of the piriformis muscle (Fig. 7) and then posteriorly across the superior border of the superior gemellus muscle (Fig. 8,
Fig. 9).
It descends in the gluteal region between the greater trochanter of the femur and the ischial tuberosity along the posterior thigh,
in which it subsequently divides into its branches; the larger tibial nerve and smaller common peroneal nerve.
This division occurs at any point between the sacral plexus and the popliteal fossa,
although in 85 - 89% of cases,
it occurs near the apex of the popliteal fossa12.
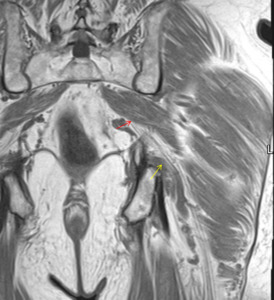
Fig. 9: Coronal T1w MRI of the left hip - demonstrating the left sciatic nerve passing the inferior border of the piriformis muscle (red arrow) and coursing over the superior gemellus muscle (yellow arrow) posteriorly.
Incidence of anatomical variants and detection with MRI :
Although it was not demonstrated in our case,
the initial hypothesis of a high bifurcation resulting in a split nerve entwinement was considered.
There are multiple cadaveric studies13,14,15 in the literature that have noted the incidence of variations in the course and bifurcation of the sciatic nerve,
the first of which was classified by Beaton and Anson15 in 1937.
With the advancement of imaging techniques,
Varenika et al16 demonstrated that it is possible to detect these variants with MRI in 2017.
They proposed that an axial T1-weighted non fat saturation sequence is ideal for delineating muscle anatomy and initial identification of the nerve,
surrounded by a plane of fat.
Furthermore,
a greater sensitive assessment can be achieved using a triplanar approach.
In their large scale study of 755 consecutive MRI scan reviews,
12 - 20% had anatomical variants,
with almost all being type II variants16.
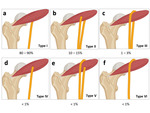
There are 6 anatomic variants described in the literature (Fig. 10):
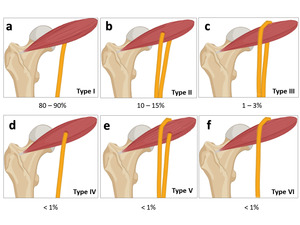
Fig. 10: Illustrative diagram - demonstrating the classification of the variants of the course and branching of the sciatic nerve in relation to the piriformis muscle and their incidences as described in the literature.
- Type I (normal course) : Sciatic nerve exits inferior to the piriformis undivided.
- Type II : Sciatic nerve divides above the piriformis,
where the superior branch exits through the piriformis and the other inferior to it.
- Type III : Sciatic nerve divides above the piriformis,
one branch courses superior to the piriformis,
the other inferior to it.
- Type IV : Sciatic nerve exits through the piriformis,
undivided.
- Type V : Sciatic nerve divides above the piriformis,
one branch courses superior to the piriformis,
the other through it.
- Type VI : Sciatic nerve courses superior to the piriformis,
undivided.
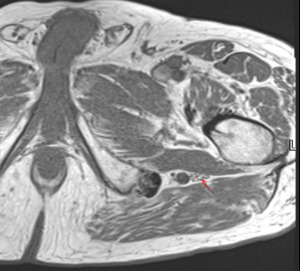
Fig. 11: Axial T1w MRI of the left hip - demonstrating a Type I left sciatic nerve (red arrow) as one bundle at the level of the ischial tuberosity.
Most split variant cases were associated with a split sciatic nerve at the level of the ischial tuberosity and rarely appear as a single combined nerve by then (normal non-split appearance as shown in Fig. 11).
Hence,
identifying splits at the level of the ischial tuberosity can be a useful diagnostic approach in identifying high splitting normal variants16.
Clinically,
this may also help with the diagnostic workup of unclear cases with extra-spinal sciatica.
Although,
the definite relation between anatomical variants of the sciatic nerve and compression of the sciatic nerve by the piriformis muscle (also known as piriformis syndrome) still remains unclear.