The transosseous approach typically involves using a bone needle to create a channel and co-axially advancing a soft tissue biopsy gun to sample the underlying soft tissue mass.
Such an approach allow for access to lesions that may have otherwise required open surgical biopsy.
Our procedures were performed using an Aquilion ONE Toshiba 320 slice CT scanner.
Local anesthetic was administered to the skin at the level of the lesion and also infiltrated to the periosteum.
Following this,
a 13-gauge bone biopsy needle was advanced under CT fluoroscopy guidance to the cortex of the targeted bone.
The bone biopsy needle would then be advanced through the proximal cortex,
through the bone to be traversed until positioned adjacent the distal cortex.
At this location an additional 2–5 ml of local anesthetic would be infused.
Once the bone biopsy needle had passed through the targeted bone,
the central trochar would be withdrawn.
An 18- or 20-gauge soft tissue biopsy needle would then be advanced co-axially through the bone biopsy needle into the distal soft tissue.
A number of bones can be safely traversed en route to underlying soft tissue lesions.
These would include the vertebral body.
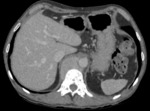
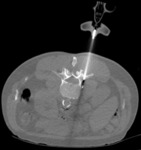
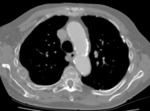
Figure 1 demonstrates a large retrocrural soft tissue mass immediately anterior to the vertebral body.
In order to avoid traversing the pleura,
a transvertebral body approach was taken.
With this approach,
care must be taken to avoid breaching the medial wall of the pedicle to avoid injury to the epidural space.
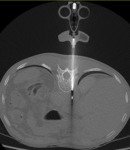
The 13 gauge bone biopsy needle was carefully advanced through the pedicle and vertebral body,
extending through the anterior cortex and a soft tissue biopsy of the retrocrural mass was taken using an 18 gauge needle (Figure 2).
Histopathology revealed a diagnosis of extra-osseous myeloma.
A transtransverse process approach can be useful to access paraspinal lesions.
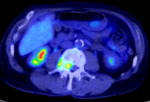
Figure 3 demonstrates an axial fused PET-CT image of an FDG avid mass in the right spinal canal with paravertebral extension,
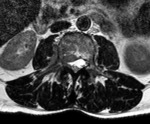
deep to the right psoas (SUVmax 4.8). The axial T2-weighted image (Figure 4) demonstrates a small paraspinal soft tissue mass,
deep to the L3 transverse process and a soft tissue mass is also evident within the spinal canal.
The mass encased the exiting nerve root,
making biopsy of this area hazardous.
Therefore a transtransverse process approach was taken using a 13 gauge bone biopsy needle and co-axial 18 gauge soft tissue biopsy needle (Figure 5).
Histopathology revealed a diagnosis of mantle cell lymphoma.
Transscapular biopsy may be useful for accessing lesions in the lung apex or posterior rib lesions.
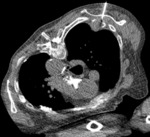
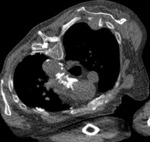
Figure 6 demonstrates an expansile lytic mass within the posterior aspect of the right 5th rib.
The patient was not able to tolerate moving his arm into a position to allow direct biopsy of this lesion so a transosseous approach was taken.
A 16 gauge 40mm white needle was passed through the blade of the scapula (Figure 7) and an 18 gauge soft tissue biopsy needle was then co-axially advanced into the lytic 5th rib lesion (Figure 8).
Histopathology revealed a plasmacytoma.
Key tips for transosseous biopsies include:
1.
Use sufficient local anaesthetic to the proximal and distal cortex and conscious sedation with fentanyl and midazolam when required.
Keeping the patient comfortable,
calm and still are essential for complex image-guided biopsies.
2.
Transosseous biopsies are best suited to lesions close to the bone being traversed and is not well suited for targeting mobile lesions.
This is because the trajectory of your biopsy needle is constrained by the position of the bone biopsy needle.
3.
Plan your route in advance and go in a straight line! Using the CT scanner laser light and ensuring that this passes through both the hub of the needle and the skin entry point may be helpful to stay in the plane of the scan.
Beam hardening artefact from the bone biopsy needle may be useful to demonstrate the course of the needle and to confirm that advancing in this plane will traverse the bone safely and pass through the target lesion.
As the bone biopsy needle will be fixed in position,
repositioning would require repeat ostetomy.
As such,
careful planning beforehand is advised to prevent needle malpositioning.