The general REQUIREMENTS for interventional procedures are common for the most of them:
- Informed consent: we must inform the patient or his representative about the purpose of the procedure,
explain the technique and possible complications.
The patient must accept the procedure and sign the document whenever possible.
- Adequate coagulation values to avoid bleeding.
-
- Accessible compression point
- Enough coagulation
- INR <1.5
- Platelets> 60000
- Prothrombin time
- Suspend anticoagulant or antiaggregant treatments under medical supervision.
- Procedure planning:
-
- Assess other examinations provided by the patient.
- Correct choice of the most suitable transducer: High resolution linear transducers (>12MHZ) are ideal for performing interventions in the musculoskeletal system.
However,
in deep and intra-abdominal lesions it is necessary to use convex probes more frequently,
with the inconvenience of the anisotropy that makes difficult the visualization of the needle.
- Identify,
characterize and locate the lesion on ultrasound.
- Accessibility through an acoustic window with the possibility of real time imaging control.
- Do not go through important vessels (using power Doppler to properly identify) or structures that can be damaged (tendons)
- In general,
the shortest route to the injury is the most appropriate and the ideal path is the most parallel to the surface of the transducer.
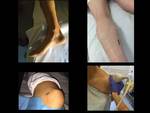
- Draw the entrance site with a marker Fig. 1
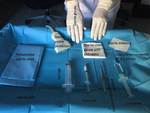
- Asepsis Fig. 2
-
- Maintain strict asepsis of the puncture site.
-
- Antiseptic (5% alcoholic chlorhexidine)
- Fenestrated cloth over the skin
- Sterile gloves
- Sterile probe protectors
- Sterile biopsy/ drainage material
- Analgesia (1% lidocaine)
-
- Local anesthesia at the puncture site and path.
- Truncal anesthesia,
in the case of procedures over peripheral nerves.
- Conscious sedation (pediatric patients)
- ATB coverage is mandatory in case we leave a drain.
TECHNIQUE:
We propose free hand technique: keeping the transducer on one hand and the procedure material on the other one.
The technique involves introducing the needle or catheter through the plane of the US imaging. The advance of the needle is controlled in real time.
The ideal path of the needle is the most parallel to the surface of the transducer.
This orientation will increase the echogenicity of the needle and allow better visualization appearing as a bright.
echogenic line,
sometimes with associated reverb artefacts.
If the orientation is oblique,
the echogenicity of the needle decreases,
to the point of seeing just the tip as a bright echogenic point in case of high the obliquity.
To avoid artifacts it is convenient to select a single focal area.
To keep the needle parallel to the surface of the transducer,
it is better to insert it far away from the transducer and press the probe through the skin trying to correct orientation.
Lateral approach is preferred to entire visualization of the needle.
Incomplete visualization of the needle is secondary to misalignment with the transducer.
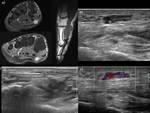
PROCEDURES: Fig. 3
Biopsies:
Indicated: in any musculoskeletal injury of unknown nature,
in metastatic lesions to obtain information about its possible origin,
to rule out tumor recurrence after surgery,
in fat tumors to rule out sarcomas,
and in infectious lesions,
to diagnose its specific etiology.
After considering the general requirements we can go on.
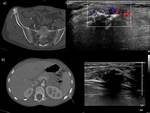
Technique: We usually use automatic guns.
- For the majority of the injuries we use a frontal cut 18 G needles,
which allows different length samples to be taken.
Fig. 4
- In fat or soft consistency lesions we have found more useful “tru-cut” type 14 G needles (lateral cut).
Get at least 3 specimens from different areas of the lesion to obtain representative specimens of the whole lesion to avoid sampling errors.
Bone lesions with cortical disruption or with soft tissue mass can also be biopsied under US guidance.Fig. 5 Fig. 6
Beware of:
- Not passing through compartments if a malignant lesion is suspected.
- Avoiding cystic /necrotic areas.
- Directing to the peripheral and more solid area.
- Not going through infected areas.
Histological analysis:
We send the specimens to the pathology service in formaldehyde. The pathological may pose difficulties to subtype the tumors and determine the tumor grade since the musculoskeletal tumors are usually heterogeneous and the sample may not be representative of the whole tumor.
In general the technique is very reliable to distinguish between benign and malignant lesions with a sensitivity of 90 to 97% and specificity of 98 to 100%
Complications:
|
|
SOLUTIONS
|
|
Pain
|
Analgesia
Sedation
|
|
Insufficient sample:
|
Sufficient sample
Solid areas
|
|
Hemorrhage (1%):
|
Hemorrhagic Diathesis Correction
Avoid going through thick vessels
Compress biopsy area after procedure
|
|
Planting implants (infrequent)
|
Include in surgery resection of the biopsy pathway
Avoid crossing compartments
|
Arthrocentesis
Indication: It can be done with 2 different purposes: therapeutic or diagnostic.
US guided arthrocentesis increases the success of intraarticular location of the injection to 97%.
It can be especially useful in obese patients,
small or loculated effusions,
or in poorly accessible joints,
such as hip.
Technique: the technic is the one described in the general section.
Once reached the articular cavity with the tip of the needle you can both,
aspire or inject.
In case of aspiration, frequently,
we will need to use 14-18G needle due to thick joint fluid.
When the high density of the liquid or the existence of septa fibrin or clots make impossible to drain the joint effusions using needles,
the Use of catheters of size 7-8F may allow drain the joint.
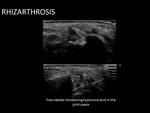
For therapeutic injection we will try to use as fine as possible needle,
the spinal ones are really usefull.
We can introduce different components.
- Corticosteroids for the treatment of scarce arthritis.
Only used in selected cases due to the association with damage and loss of elasticity in the cartilage in joints that support weight.
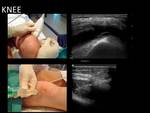
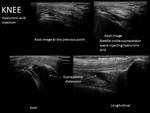
- Hyaluronic acid.
To promote joint lubrication in osteoarthritis.
Usually in the hip,
knee and trapeziometacarpal joint.
Note that the injection through a spinal needle is slightly difficult due to its high density.
- Urokinase.
In very dense effusion with partitions of fibrin or in hemarthros,
it allows lysing fibrin and emptying the effusion.
In the knee,
for example,
100,000 UI of urokinase dissolved in 30 cc of serum are injected and after waiting 1-2 h,
the liquid is aspirated.
- Gadolinium dilution to perform arthro-MRI.
Specific instructions for different joints:
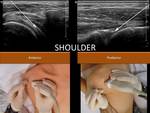
- Shoulder: The anterior access is made with the patient in supine and the arm rotated externally.
The needle penetrates the axial plane from the outside to the inside,
crossing the subscapularis tendon.
Posteriorly, the puncture is made with the arm in forced approach and externally rotated,
following an axial plane,
from outside inward,
crossing the infraspinatus muscle,
in the direction of the posterior labrum.
Fig. 7
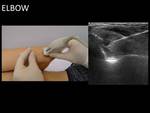
- Elbow: The access is made with the articulation flexed,
from the posterior side of the elbow,
following a longitudinal plane,
and directing the needle towards the olecranian fossa of humerus.
Fig. 8
- Wrist: Usually the access between the first ans second extensor compartment directing the needle to the radius.
Fig. 9
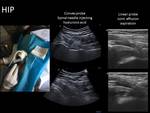
- Hip: The puncture should be made in the existing concavity between the head of the femur and the anterior surface of the surgical neck,
with the patient in the supine and the hip in external rotation,
with the needle aligned with the axis of the surgical neck of the femur.
Fig. 10
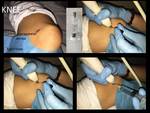
- Knee: The easiest access is in the suprapatellar bag,
with patient in supine and the knee slightly flexed.
Fig. 11 Fig. 12 Fig. 13
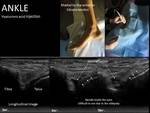
- Ankle.
The simplest access is on the front of the ankle,
directing the tip towards the tibiotalar articulation,
from a distal level.
Fig. 14
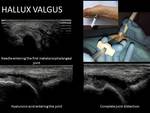
- Nearly all joints are accessible by US.
For example the first metatarsophalangeal joint. Fig. 15
Beware of:
- Being extremely aseptic.
- In septic arthritis,
it is convenient to avoid manipulation and Injection of corticosteroids is contraindicated.
- Avoiding puncture of the articular cartilage.
- Avoiding exercise in the joint for two weeks and load weights for six after corticosteroid injection.
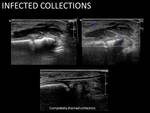
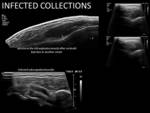
Drainage of infected collections: Fig. 16 Fig. 17 Fig. 18
Muscle abscesses can be caused by surgical interventions,
local injections,
trauma,
foreign bodies or the extension of infectious processes.
Bursitis is inflammatory processes of the periarticular bursae that can become infected.
Technique: is the one described in the general section.
In case of intramuscular abscesses we usually use 8F-10F drainage connected to a bag until no evident drainage during 24h.
In bursitis we can aspire with 18G needle or try a 14G abbocath .
In 80% of cases,
percutaneous drainage manages to cure the abscess and avoid surgery.
In the rest allows controlling the infection and decreases its size,
facilitating the surgery and allowing it to be carried out in an elective way.
Consider as cause of failure: the presence of intracavitary bodies (foreign bodies,
foci of myositis ossificans,
bone fragments) in which germs can be cantoned and cause recurrence of infection,
and association with infectious foci in the adjacent bone (osteomyelitis).
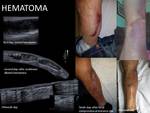
Drainage of hematic collections:
Musculoskeletal hematomas are usually secondary to trauma or sports,
although they can be facilitated in patients with hemorrhagic diathesis or anticoagulated.
When they are asymptomatic they only require conservative treatment waiting for his spontaneous reabsorption.
However,
if they are symptomatic, their drainage can alleviate their symptoms and reduce the necessary healing time.
In hematomas caused by trauma or muscle fibers tear the evacuation allows accelerate the healing of the injury and shorten the inactivity time.
Technique:
Hematoma: the technique is similar to that described for abscesses.
The content of the hematoma varies from liquids collection to coagulated hematomas.
Fig. 19
- If the collection is purely liquid a fine catheter (7-8 F) will be enough.
- But if the content is coagulated,
thick catheters (10-12 F) eider with or without fibrinolytic substances.
We recommend to use urokinase in clotted hematoma (100,000-250,000 IU,
depending on the volume of the hematoma) every 8 hours until the hematoma is completely drained or if no volume decrease is appreciated (usually happens in 1-3 days)
Small muscle tear: Rapid evacuation of collections formed in the areas of rupture accelerates their healing.
The objective is not to diminish the bruise,
but to avoid the pseudocysts and accelerate healing.
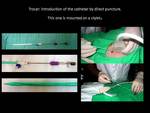
The evacuation of these collections can be done by direct puncture and aspiration with 18-20 G needle.
You may repeat puncture if the collection returns
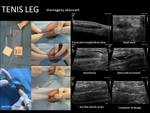
Tennis leg: It is the muscular tear at the distal myotendinous junction of the medial gastrocnemius.
In severe cases a hematic collection is formed between the gastrecnemious and the soleus that produces a remarkable functional impotence that can last for months.
In these patients the evacuation allows rapid recovery of the patient.
You will need to place a fine catheter (6-7 F) inside the collection and keep it until it stops draining for 48 h.
A scar will form on the bed; the quicker it is solved the smaller the scar will be.
Fig. 20 Fig. 21
Beware of:
- The evacuation of a hematoma is contraindicated in active bleeding.
- In case of bleeding during the procedure the drain should be closed until it stops.
- Computed tomography and angiography are useful to assess the existence of active bleeding and even treat it.
- Patients in treatment with oral dicoumarins should change anticoagulation to low molecular weight heparin before the evacuation.
- Broad-spectrum antibiotic treatment should always be associated with the drainage.
We use amoxicillin with clavulanic or cloxacillin.
- In tennis leg: Low-molecular-weight heparin should be prescribed at a prophylactic dose while maintaining drainage,
given the risk of intramuscular venous thrombosis.
- Comprehensive bandage is necessary to avoid re-bleeding and favor cicatrization.
- Not using urokinase in case of active bleeding in the previous 4 days.
Therapeutic infiltrations:
Local corticosteroid injection is a common procedure in musculoskeletal inflammatory processes or trauma.
The ultrasound guide allows directing the injection precisely,
increasing its effectiveness and reducing its complications.
Drugs:
Several types of corticosteroids can be used; we usually use 40 mg/mL of triamcinolone acetonide.
Sometimes,
the Injection causes discomfort during the first 48 h.
The result of the infiltration usually is appreciated in the first 15 days. In patients without known pathology,
the infiltration can solve the painful problem,
but if there is an underlying cause is expected a recurrence in the medium term.
Technique:
After performing the asepsis measures,
the puncture is performed directing the needle to the target; it is possible to follow the dispersion of the liquid in the tissue.
Fine needles (23-25G) are preferred because they are less painful and can avoid local anesthesia.
The injection into inflamed joint bursae should be done inside.
If you want to infiltrate a structure not covered by a sheath or a bursa,
the injection must go to the surface of the structure.
Fig. 22
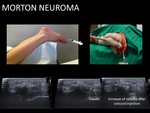
- Treatment of Morton's neuromas. It consists of direct injecting into the neuroma.
We prefer plantar access.
Usually a 23G needle is enough.
The procedure can be repeated three times with 6 week space. Fig. 23
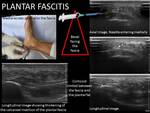
- Treatment of plantar fasciitis. The Injection should be done on the surface of the fascia,
without penetrating inside or injecting into the fat. We use medial access,
entering a 21G needle to the lateral site,
facing the bevel to the fascia and injecting corticoid while retiring the needle.Check that the injected liquid spreads through the surface of the fascia. Fig. 24
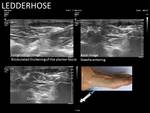
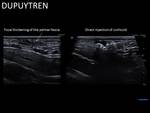
- Treatment of Ledderhose's and Dupuytren disease. Direct injection into the lesion with a 23G needle.
The nodule diminishes and improves pain and retraction.
Fig. 25 Fig. 26
Beware of:
- Intradermal or subcutaneous corticosteroids can produce skin atrophy and local hypopigmentation.
- Not injecting into tendon,
fascia or ligament,
to avoid damaging and weakening.
- Resting for two weeks is indicated and carrying weights for 6 weeks should be avoid after peritendinous injections.
- Corticosteroids should be used with caution,
especially when the adjacent tendon supports load (patellar,
Achilles) or is injured.
- Corticosteroids are not indicated for the treatment of chronic tendon injuries.
- Spacing the injections time enough to check its effects; usually a minimum of 6 weeks.
- Do not use more than 3 injections in the same place in each treatment,
and you should not repeat the injection if at least 4 weeks of symptomatic relief is not achieved after 2 injections.
- If the patient is diabetic,
you should consider hyperglycaemia after corticosteroids.
In insulinodependant patient they should increase the injected dose.
In case of oral antidiabetic drug,
you should recommend eating less carbohydrate the following 48 hours.
Ganglion cyst treatment (also valid for parameniscal cyst)
Most are asymptomatic and do not require treatment or they even resolve spontaneously.
Some can cause symptoms by compression of the adjacent structures and they need to be treated.
On other occasions it requires its treatment for cosmetic reasons.
Surgery presents recurrence rates of up to 34%.
The puncture of these lesions under ultrasound control has results similar to those of surgical treatment.
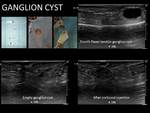
Technique: Fig. 27
- Aseptic procedure.
- Local anesthesia (lidocaine 1%) with a 23G needle.
- Thick needles (18G) or abbocath (14G): the content of the ganglion is extremely dense.
- Useful to perform lavages with serum to compete evacuation.
- We always completed Injection of corticosteroids in the lesion in order to decrease the recurrence rate.
- The technique is very effective in short term.
However,
the possibility of recurrence is significant.
The treatment can be repeated.
- The use of absolute alcohol must only be used by experienced interventional radiologist.
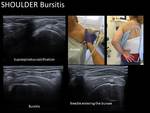
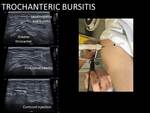
Bursitis treatment
Bursitis can manifest as wall thickening of the joint bursae,
fluid collections or in case of infection,
the formation of pus inside the collection.
In inflammatory bursitis,
direct injection of corticosteroids (40mg/mL of triamcinolone acetonide) in the bursa is the indicated treatment.
40mg/mL of triamcinolone acetonide
When there are Intra-bursal liquid collections,
they should be emptied before the injection.
We can use 23 G or 21 G needle usually depending on the distance.
Fig. 28 Fig. 29
Infectious bursal infections should be treated as described for the treatment of abscesses.
Corticosteroids are contraindicated.
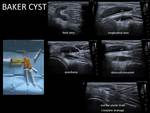
Baker's cysts treatment:
They can cause symptoms due to inflammation,
rupture,
intracystic hemorrhage,
increased internal pressure or compression to adjacent structures even can simulate a thrombophlebitis of the leg.
In these cases,
percutaneous treatment by puncture and aspiration with ecographic control is indicated.
Technique:
- Asepsis
- Local anesthesia (lidocaine 1%) with a 23G needle (25 mm length) or 21G (40 mm length)
- 14G abbocath,
introducing both the catheter and the sear,
retire the last one and leave the catheter inside the cyst.
- Aspire the content to the final end.
- Injection of corticosteroid (40mg of triamcinolone acetonide) Fig. 30
The treatment is very effective in the short term,
over all in patients with pseudothrombophlebitis.
Although the recurrence is frequent if there is an underlying cause,
at least the objective of improving symptomatology is achieved almost always.
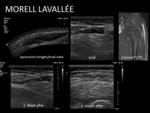
Morel- Lavallée treatment: Fig. 31
Occur when the skin and subcutaneous fatty tissue traumatically and abruptly separate from the underlying fascia opening a potential space superficial to the fascia filled by various types of fluid.
Once these lesions become established and encapsulated then conservative management is rarely successful so we should try to intervene before.
Technique:
- Asepsis
- Local anesthesia
- Fine needle: Spinal (20G) or abocath (18G)
- Aspire the content to the final end.
- Compressive bandage
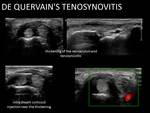
De Quervain´s tenosynovitis treatment: Fig. 32
Painful stenosing tenosynovitis involving the first extensor tendon compartment of the wrist.
Technique:
- Asepsis.
- Direct injection of corticoid (40mg of triamcinolone acetate) with a 23G needle inside tendon sheath next to the retinaculum.
Beware of possible septa separating both tendons,
ensure that you are injecting in the damage one.
- After 3 weeks,
direct injection of hyaluronic acid for better lubrication.
Treatment of Triger Finger,
calcifying tendinitis and tendinosis requires the development of interventional skills beyond the purpose of this poster