Several clinical cases from our Department were selected in order to illustrate the typical aspect of osteoid osteoma and its treatment with RFA guided by CT.
Relative contraindications to RFA include a lesion located in the hand or in the spine (<1cm from vital structures such as nerves),
pregnancy,
cellulitis,
sepsis and coagulopathy.
Lesions that have a nidus bigger than 1 cm generally need multiple applications of the electrode in several positions (6).
The procedure has several steps and is performed under aseptic conditions with general anesthesia in a CT room (Fig.
10).
Lesion localization is achieved with multiple thin-section CT images acquisition at the level of the osteoid osteoma (Fig.
11).
Multiplanar reformatted images may help in preprocedure planning (Fig.
12).
For lesions less than 1 cm in diameter,
a single skin entry point is made,
otherwise multiple skin entry points are necessary to obtain the 1-cm-wide ablated margin required for treatment success.
After confirming the precise lesion localization with CT imaging,
entry point is marked on the skin overlying the lesion (Fig.
13).
The preferred approach is a perpendicular angle to the cortical surface of the involved bone,
avoiding any adjacent neurovascular structures.

Fig. 13: Axial CT image of the left femural head demonstrates the preferred angle of approach, nearly perpendicular to the cortical surface. A radiopaque mark is placed on the skin overlying the lesion.
The cannula with stylet is inserted and advanced through the soft tissues to the bone surface and a localizing scan is done to confirm its correct position.
After that,
the stylet is exchanged for the done drill that is advanced through the cannula to penetrate the outer bone cortex (Fig.
14).
With the done drill positioned at the cortical edge of the nidus,
CT images are obtained to verify appropriate position.

Fig. 14: Spot CT image obtained after insertion of the cannula. The stylet is removed and the drill advanced through the cannula. The drill is right positioned at the cortical edge of the lesion
The drill is removed,
and electrode is placed through the cannula with its tip directed toward the center of the nidus (Fig.
15).
More CT images are acquired to confirm a satisfactory position of the electrode (Fig.
16).

Fig. 15: Spot CT image show the needle extending beyond the cannula and penetrating the osteoid osteoma nidus.
Ablation is done during a total of approximately 6 minutes at a targeted temperature of 90 degrees Celsius and,
after that,
the electrode is removed.
Postprocedural CT is performed to exclude soft tissue swelling and hematoma (Fig.
17).
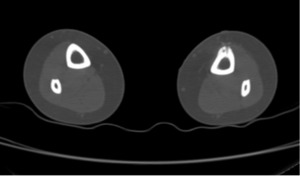
Fig. 17: Axial CT postprocedural in order to exclude potential complications as soft tissue swelling and hematoma.













