Introduction
Osteoid osteoma is a small and benign painful osteoblastic lesion with specific imaging findings and symptoms.
It represents 10% of all skeletal lesions (1).
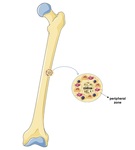
The lesion is characterized by two zones (Fig.
1):
- Central zone: composed of atypical bone known as the nidus;
- Peripheral zone: sclerotic bone that contains osteoclasts,
osteoblasts and dilated capillaries.

Fig. 1: Illustration of the central and peripheral zone of osteoid osteoma
References: Figure adapted from a template produced by Servier Medical Art (http://smart.servier.com) under the Creative Commons License
It usually affects children and young adults between the ages of 10 to 35 years-old,
with a male predominance.
Osteoid osteoma has a higher incidence in long bones (Fig.
2),
mostly affecting the diaphysis of the femur or tibia (Fig.
3).
Other less common sites include the spine,
hands and feet (Fig.
4).
However,
the osteoma osteoid may occur in any bone.

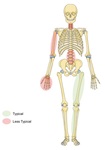
Fig. 2: Illustration representing the predilection sites of osteoid osteoma
References: Figure adapted from a template produced by Servier Medical Art (http://smart.servier.com) under the Creative Commons License
Clinically,
the characteristic symptom is bone pain wich often worsens at night and is considerably relieved by aspirin or other non-steroidal anti-inflammatory drugs.
This is due to the high levels of prostaglandins existent in the nidus and the reason why aspirin reduces the pain (2).
Pain initially may be described as a sensitive discomfort wich may progress to severe localized pain over the site of the lesion.
Less commonly,
the symptoms might be growth disturbance,
bone deformity,
and painful scoliosis in spinal lesions.
If it affects a joint capsule it can cause joint swelling,
synovitis,
effusion and restricted motility.
Even with medical therapy implementation,
several patients persist with residual discomfort related to the lesion.
Radiologic Imaging Characteristics
Osteoid osteoma can be of three types according to the location of the nidus at radiologic imaging: cortical,
medullary and subperiosteal.
Those with cortical location are the most common and are characterized by a reactive sclerotic cortical thickening that surrounds a central radiolucent nidus.
The other two types are less common and are usually intra our peri-articular with less osteosclerosis.
1. Radiographic Findings
Osteoid osteoma characteristically demonstrate a circular or ovoid lucency,
representing the nidus (usually less than 10mm in diameter),
with a variable degree of surrounding sclerosis (Fig.
5).
In situations with wide sclerosis,
it may interfere with visualization of the radiolucent nidus.

Fig. 5: Radiographic appearance of osteoid osteoma on tibial diaphysis (A) and humeral diaphysis (B). Both radiographs show a faded tibial diaphyseal circular lucent defect with a diameter less than 1 cm (arrow) and surrounding sclerosis.
2. Scintigraphic Findings
Bone scintigraphy may be useful to localize lesions,
principally in cases with clinical suspicious and nearly normal radiographic findings.
It usually shows an intense activity at the nidus and with decreased activity in the surrounding reactive zone,
a pattern known as the double-density sign (Fig.
6).

Fig. 6: Radionuclide skeletal scintigraphy demonstrates intense activity in the nidus in the left distal tibia (arrow) with surrounding mild activity (double-density sign)
3. Computed Tomographic Findings
Computed tomography (CT) is the best modality to localize and identify this benign lesion (Fig.
7).
It provides the best characterization of the nidus and the surrounding cortical sclerosis (3).
The nidus appears as a radiolucent region with different degrees of central mineralization in about 50% of the cases (Fig.
8).
Around the nidus is common to see a marked reactive sclerosis.
Although,
some lesions may show no exuberant reactive sclerosis.

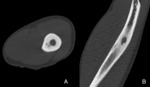
Fig. 7: Axial (A) and coronal reformatted (B) CT images of the humeral diaphysis revealing a radiolucent nidus with faint internal mineralization and some surrounding sclerosis

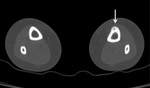
Fig. 8: Axial (A) and sagital (B) CT images of the distal tibia, in the tibialotarsal component, demonstrating a focal cortical lucency with central calcification (arrow) and surrounding sclerosis in association with an osteoid osteoma.
4. Magnetic Ressonance Imaging (MRI) Findings
Other imaging techniques,
as Magnetic Resonance Imaging,
may help distinguishing osteoid osteoma from a suspected infection.
This imaging modality shows the surrounding marrow and soft tissue changes associated with the lesion.
The nidus usually has an isointense sign to that of the muscle on T1-weighted images and is variable on T2-weighted images.
The surrounding reactive zone shows a hyperintense signal on T2-weighted images (Fig.
9).
Dynamic MRI demonstrate early enhancement in arterial phase with subsequent early partial washout,
in contrast to osteomyelitis slow enhancement,
without any arterial peak enhancement (4).

Fig. 9: Axial (A) and coronal (B) T2-weighted show in the outer edge of the tibial shaft of the right leg show the nidus with marked surrounding marrow edema, the typical MR imaging appearance of osteoid osteoma.
Treatment Options
There are different options to treat this condition,
including medical management with non-steroidal anti-inflammatory drugs,
open surgical resection and percutaneous techniques.
As the long-term medical therapy can be associated with refractory pain and surgical resection requires significant bone resection,
CT-guided RFA has been proposed as a safe,
minimally invasive and cost-effective treatment for osteoid osteoma.
RFA is an electrosurgical technique wich uses hight frequency alternating current heating the lesion with consequent coagulation necrosis.
A recent study has demonstrated up to 96% technical success with this procedure (5).