Churg-Strauss syndrome
Named after American pathologists Jacob Churg and Lotte Strauss.
They presented the histological criteria of the syndrome in the American Journal of Pathology in 1951,
based on 13 cases originally diagnosed with polyarteritis nodosa.
Clinical features
- Autoimmune condition affecting asthmatics.
Characterised by hypereosinophilia in the blood and tissues and is therefore now known as eosinophilic granulomatosis with polyangiitis.
- Small to medium vessel necrotising pulmonary vasculitis.
- Other features include sinusitis,
diarrhoea,
purpura,
and joint pains.
- Association with pANCA.
Imaging characteristics
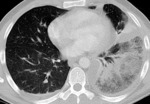
- Parenchymal consolidation/ground glass.
Pulmonary haemorrhage and effusions.
Fig. 1
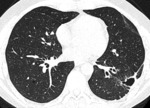
- Centrilobular nodules,
interlobular septal and bronchial wall thickening.
- Can cavitate,
often if complicated with infection.
Fig. 2
Granulomatosis with polyangiitis (Wegener's granulomatosis)
Named after German pathologist Freidrich Wegener who presented the condition in two reports during the 1930s.
It remained so until the year 2000,
when his previous affiliations with the Nazi party came to light.
Following on from this it is now known as granulomatosis with polyangiitis.
Clinical features
- Multi-system necrotising non-caseating granulomatous vasculitis.
- Affects small to medium sized vessels.
- Present with cough,
haemoptysis,
airway and sinus mucosal disease leading to osseous and cartilaginous destruction.
Patients may also get proteinuria,
haematuria and renal failure.
- Strong association with cANCA.
Also may diagnosed by renal biopsy and seen on CT sinus studies.
Imaging characteristics
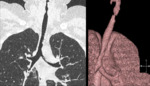
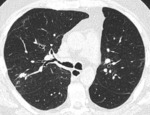
- Nodules are random in distribution and size,
which commonly cavitate.
Fig. 3
- Pulmonary haemorrhage.
- Basal reticulonodular pattern.
- Peripheral wedge like consolidation and pleural effusions.
- Thickening of the airways,
leading to cartilage destruction and airway stenosis.
Fig. 4 and Fig. 5
Sjögren’s syndrome
Named after Swedish opthalmologist Henrik Samuel Conrad Sjögren who described the syndrome in his thesis “Zur kenntis deer keratoconjunctivitis sicca”.
However this was not deemed high enough standard to be awarded the title of “docent” at the time (later achieving this).
When it was translated into English in 1943 that the term Sjögren syndrome became common place.
Clinical features
- Autoimmune disorder involving hyperactivity of B-lymphocytes,
with autoantibody and immune complex production leading to inflammation.
- Clinical features include keratoconjunctivitis sicca,
dryness of the mouth,
bilateral parotid enlargement,
dry cough and dyspnoea.
- Association with anti SSa(Ro),
anti SSb(La),
sjögren A and sjögren B antibodies.
Imaging characteristics
- Most commonly non-specific interstitial pneumonia (NSIP) picture.
- Also can present as lymphocytic interstitial pneumonia (LIP) cryptogenic organising pneumonia (COP) or usual interstitial pneumonia (UIP).
Fig. 6
- Bronchitis,
with a tree in bud pattern and mosaic attenuation secondary to obstructive bronchiolotis also seen.
- Witihin the parotid and submandibular glands patients can develop multiple cysts. Fig. 7 and Fig. 8
Pancoast lung tumour
Named after American radiologist Henry Khunrath Pancoast,
the first ever American professor of roenterology.
He reported 3 cases of Pancoast syndrome in 1924 (see below) before describing its association with superior pulmonary sulcus tumours in 1932.
Clinical features
- Apical lung cancer arising in the superior pulmonary sulcus.
- Usually non-small cell lung cancer.
- Classically can lead to Pancoast syndrome due to local invasion - Ipsilateral chest/shoulder pain,
C8-T2 radiculopathy and Horner’s syndrome.
Imaging characteristics
- Apical mass with local invasion into the surrounding tissues and adjacent ribs.
Fig. 9
- In addition to PET-CT (Fig. 10),
MRI (Fig. 11) is often used for local assessment of the tumour and the involvement neurovascular structures.
Swyer-James / Macleod Syndrome
Described by Canadian chest physicians Paul Robert Swyer and George James and simultaneously by English chest physician William Macleod in their papers in Thorax in 1953 and 1954.
As a result the two eponyms are often used interchangeably.
Clinical features
- Post infective obliterative bronchiolitis leading to impaired growth in the affected lung.
This occurs in childhood following recurrent infections and is frequently seen in respiratory viruses,
such as adenovirus and RSV or mycoplasma pneumoniae infection.
- Whole lung usually involved rather than lobar involvement.
Imaging characteristics
- Hyperlucent hemithorax Fig. 12.
- Bronchiectasis.
- Volume loss and reduction of pulmonary markings.
Small ipsilateral hilum.
- "Pruned tree" appearance on CT and radiographs.
Fig. 13
- May have air trapping in expiration.
Birt-Hogg-Dubé syndrome
Named after Canadian physicians Arthur Birt,
Georgina Hogg and William Dubé who examined a family with hereditary thyroid cancer and cutaneous manifestations,
publishing their work in the Archives of Dermatology in 1977.
Pulmonary and renal associations were subsequently described over the following two decades.
Clinical features
- Autosomal dominant genetic disorder secondary to deletion mutation in the folliculin (FLCN) gene,
a tumour suppression gene restricting cell growth and division.
Now often referred to as folliculin gene-associated syndrome.
- Lung cysts with spontaneous pneumothoraces.
- Patients may also develop bilateral renal tumours and cutaneous lesions.
Imaging characteristics
- Multiple lung cysts often in a lower zone distribution,
which lead to secondary pneumothorces. Fig. 14
- Often round,
ovoid or septated,
especially if large.
- Renal masses may be seen and therefore patients undergo regular surveillance. Fig. 15
Kawasaki’s disease
Named after Japanese paediatrician Tomisaku Kawasaki who published his observations on 50 patients in a Japanese journal in 1967.
The exact aetiology of this complex condition is still unknown,
with Kawasaki founding the Japan Kawasaki Disease Research Center in 1990.
Clinical features
- Although unclear current theories point to an infective cause coupled with genetic susceptibility and an autoimmune response.
- Small to medium vessel vasculitis in childhood causing coronary artery aneurysms and myocarditis in the subacute phase.
- Other features include fever,
conjunctivitis,
anterior uveitis,
lymphadenitis,
strawberry tongue,
desquamation of digits and thrombocytosis.
Imaging characteristics
- CT,
MRI and catheter angiography shows ectatic,
aneurysmal and stenosed coronary arteries. Fig. 16
- Occasionally calcified coronary artery aneurysms may be appreciated on chest radiographs and CT. Fig. 17
Kaposi’s sarcoma
Named after Hungarian physician and dermatologist Moria Kohn Kaposi who described a skin cancer in elderly male subjects in 1872 in the journal “archiv für dermatologie und syphyllis’.
Initially called “idiopathic multiple pigmented sarcoma”.
Over a century later in San Francisco the disease rose to prominence,
identified in young gay men as one of the earliest indications of AIDS.
Clinical features
- Mesenchymal tumour that involving the lymphovascular system.
Lesions are positive for human herpesvirus 8.
- Affects those who are immunosuppressed,
post transplant and in those with HIV as an AIDS defining illness.
- Endemic form in Sub-Saharan Africa and is one of the most prevalent tumour in this region.
- Lung involvement initially followed by multiple purple coloured skin lesions and widespread organ involvement.
Imaging characteristics
- Ill defined ‘flame’ shaped nodules in a peribronchovascular distribution. Fig. 18
- Can have patchy ground glass changes and interlobular septal thickening.
- Lymphadenopathy is a late feature of disease. Fig. 19
Kartagener’s syndrome
Named after Swiss internist Manes Kartagener.
Although it was initially described in a case by Ukrainian physician Alfons Karlovich Zivert in 1904,
Kartagener later reported a group of cases of the condition in 1933.
He later received plaudits for his dissertation into bronchiectasis and became a professor in 1950 and so the condition bears his name.
Clinical features
- Kartagener's syndrome is a subtype of primary ciliary dyskinesia with situs inversus.
Passed on by autosomal recessive inheritence.
- Ciliary dysfunction causes chronic sinusitis and bronchiectasis.
Patients may also suffer from infertility in males and sub fertility in females.
Imaging characteristics
- Situs inversus. Fig. 20
- Consolidation and Bronchiectasis,
which can be cylindrical or cystic - less severe than cystic fibrosis.
- Mucous plugging and resultant atelectasis. Fig. 21
- May see tree in bud pattern/centrilobular nodules with mucous impaction.
Morgagni’s hernia and Bochdalek’s hernia
Congenital diaphragmatic herniae.
These where described by Italian anatomist and pathologist Giovanni Battista Morgagni and Czech anatomist Vincent Alexander Bochdalek who lived and worked in the 18th and 19th centuries respectively.
Clinical features
- Morgagni’s hernia - Anteromedial,
right sided,
small congenital hernia between the pars sternalis and pars costalis.
Low risk of prolapse of abdominal organs.
- Bochdalek’s hernia - Posteromedial,
left sided,
often large congenital hernia secondary to failure of closure of pleuroperitoneal hiatus.
Abdominal organs more commonly prolapse. Fig. 22
- Both may present with respiratory distress in infancy and can lead to pulmonary hypoplasia,
which is more common in Bochdalek hernias.
- Surgical repair is sometimes necessary,
but is not without complication.
Fig. 23
Imaging characteristics
- Soft tissue densities,
which can obscure the anterior or posterior silhouette sign.
- May mimic pulmonary pathology on chest radiographs (Fig. 24 and Fig. 26).
- CT shows the defect (Fig. 25 and Fig. 27) and may show herniated visceral contents into the thorax.
Lemierre’s syndrome
Named after French bacteriologist Andre Alfred Lemierre,
who reported the syndrome in 1936 in a case series of 20 patients,
in which throat infections were followed by anaerobic sepsis.
Clinical features
- Infectious thrombophlebitis of the internal jugular vein with haematogenous spread to other organs.
- Occurs following upper respiratory infections,
such as tonsillitis and pharyngitis,
which may also be complicated by retro/parapharyngeal abscesses.
- Gram negative bacterium fusobacterium necrophorum the most common pathogen.
- Lungs most common site of embolic disease.
Less commonly septic arthritis and meningitis.
Imaging characteristics
- Contrast enhanced CT shows a jugular filling defect (which may also be appreciated on ultrasound) and oropharyngeal infective changes.
Fig. 28
- In the lungs septic emboli are seen as multiple,
predominantly lower zone,
cavitating nodules.
Fig. 29
- May also see cavitating pulmonary infarcts.
- Pleural effusions are common,
which can develop into empyema.