INTRODUCTION
The imaging findings of some tropical diseases are fairly characteristic.
Because of increased migration and frequent traveling,
some patients with such infections may be encountered in non-endemic areas and the diagnosis may be delayed or difficult.
Therefore knowledge of the most important features of these diseases is important.
SCHISTOSOMIASIS MANSONI
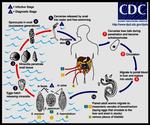
Schistosomiasis mansoni is caused by the trematode Schistosoma mansoni,
which is endemic in the Middle East,
Africa,
Atlantic coast of South America,
Caribbean and Asia (1).
It represents the second cause of mortality among parasitic infections after malaria,
affecting aproximately 150 million people and causing 500 thousand deaths per year around the globe (2).
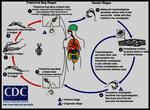
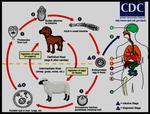
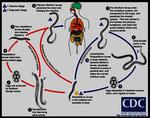
Infection typically occurs through direct contact with contaminated water,
either through the skin or ingestion (Fig.
2).
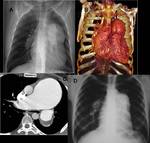
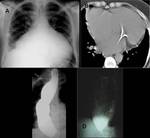
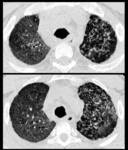
The pulmonary manifestations may be acute (fever,
cough with mucoid sputum or hemoptysis, dyspnea) or chronic (pulmonary hypertension and cor pulmonale) (Fig.3).
Imaging Features
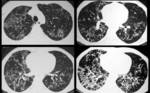
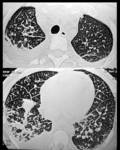
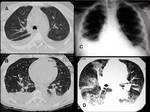
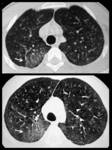
Acute form (Fig.4):
Migratory multifocal consolidations and ground glass opacities
Miliary nodules
Nodular opacities with ill-defined margins and multiple nodules with halo sign on CT
Diffuse or sparse ground-glass opacities
bilateral reticulonodular pattern
Irregularly thickened interlobular septa
Chronic form:
Central pulmonary artery enlargement
Cardiomegaly
Lung calcifications
Localized mass (pseudoneoplastic form)
AMEBIASIS
Amebiasis is caused by the protozoan parasite Entamoeba histolytica and is endemic in Central and South Americas,
Africa,
and India.
Approximately 1% of the world’s population is thought to be infected,
with approximately 70 thousand deaths reported annually.
It represents the third cause of mortality amongst parasitic diseases,
after malaria and schistosomiasis (2-4).
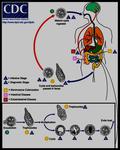
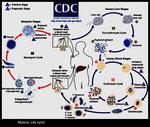
The infection is acquired by ingestion of cysts that become trophozoites in the colon and may invade the bowel wall (Fig.
5) (4).
Pulmonary involvement may present clinically as cough and pleuritic chest pain.
Patients may develop pleuropulmonary abscesses,
hepatobronchial fistulas and rupture of liver abscesses to pericardium (5).
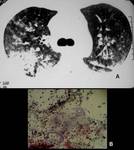
Imaging Features
Elevation of the right hemidiaphragm
Pleural effusion/empyema
Consolidation and excavation
Pericardial effusion and pericarditis
Invasion of the inferior vena cava
CHAGA’S DISEASE
Chagas disease is caused by a flagellate protozoan parasite,
Trypanosoma cruzi, which is acquired through the bite of an insect from the Reduviidae family (genera Triatoma,
Rhodnius,
and Panstrongylus) (Fig.
6) (2).
It is endemic in areas of Central and South America,
where nearly 24 million people are infected and results in approximately 60.000 deaths per year (2).
Imaging Features:
Chronic heart failure (septal lines,
pulmonary edema,
pleural effusion)
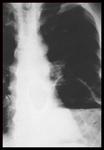
Cardiomegaly (Fig.
7)
Megaesophagus
Bronchiectasis and tracheomegaly are rarely seen
MALARIA
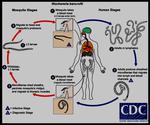
Malaria is an infectious disease caused by protozoan parasites of the genus Plasmodium,
transmitted by the bite of the female Anopheles mosquito (Fig.
8) (6).
It is endemic in South America,
Africa,
and southernAsia,
and is responsible for 2.2 to 2.5 million deaths annually (2).
It represents the first cause of mortality related to parasitic infections (2).
Pulmonary involvement is a relatively common manifestation of malaria and is usually benign,
occurring in approximately 1% to 40% of cases in some series (6).
Pulmonary manifestations range from subclinical lung disease to hypoxia, bronchitis,
interstitial or alveolar infiltrates (Fig.
9),
pleural effusion and pulmonary edema (6).
Imaging Features
Pleural effusion
Diffuse interstitial edema
Lobar consolidation
Bronchiolitis obliterans organizing pneumonia (BOOP)
Eosinophilic pneumonia with bilateral patchy consolidation (association with the use of pyrimethamine)
DENGUE
Dengue is an arboviral disease transmitted usually by female mosquitoes of the genus Aedes (7).
There are 2.5 billion people at risk worldwide and 50 million new infections per year,
mostly in Southeast Asia,
Western Pacific,
and Americas (7).
It can present a diverse clinical spectrum,
ranging from asymptomatic illness to dengue shock syndrome,
as well as presenting with unusual manifestations,
such as hepatitis,
encephalitis,
myocarditis,
Reye's syndrome,
hemolytic uremic syndrome and thrombocytopenic purpura (8).
Imaging Features:
Ascites and pleural effusion (Fig.
10)
Bilateral areas of consolidation with air bronchograms and ground-glass opacities
HYDATIDOSIS
Hydatidosis is an infection caused by the taenia Echinococcus granulosus,
whose larval form accidentally affects men by forming hydatic cysts preferably in the lungs and liver (9).
E granulosus is the most common causative parasite and may be seen in the Mediterranean region,
Eastern Europe,
Africa,
South America,Middle East,Australia,
andNew Zealand (2).
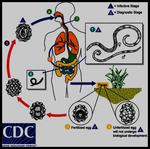
Figure 11 shows E.
granulosus life cycle.
Pulmonary involvement occurs in 10-30% of cases,
being second only to the hepatic involvement.
However,
in children the lungs may be the commonest site of cyst formation (10).
Pulmonary involvement may present clinically in a variety of ways,
ranging from subclinic disease to cough,
expectoration,
fever and hemoptysis;
Lung abscess,
pneumothorax,
pleural effusion and pulmonary embolism are also described complications.
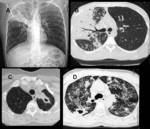
Imaging Features
Well circumscribed spherical opacities with sizes ranging from 1-20 cm
Solitary in 70-80% of cases and usually located in the lower lobes
“Crescent sign” can be seen in ruptured cysts
Transdiaphragmatic extension of hepatic cysts can result in elevation of the hemidiaphragm,
pleural effusion,
atelectasis,
cysts and pleural empyema (Fig.
12)
Air-bubble sign (strong indicator of infected hydatid cysts)
LYMPHATIC FILARIASIS
Lymphatic filariasis is caused by the nematodes Wuchereria bancrofti and Brugia malayi,
which are endemic to tropical regions inAfricaand southeast Asia,
respectively.
Typically,
individuals become infected in early childhood through the bite of an infective mosquito (Fig.
13) (12);
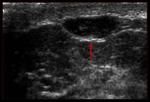
Filariasis is the most commonly reported parasitic infection of the breast.
In acute lymphatic filariasis,
the larvae cause local inflammation and granulomatous lymphangitis,
leading to the clinical manifestation of a painless breast mass with overlying peau d’orange and hyperemia of the skin (13);
At mammography,
acute infection is typically seen as a circumscribed,
hyperdense ovoid mass.
A few case reports have described theUSappearance of the “filarial dance” —the nonrhythmic,
nonpulsatile,
rapidly changing movements of organisms within dilated,
cystic lymphatic vessels (Fig.
14).
After the parasite dies,
mammography will show the characteristic pattern of elongated or tubular calcifications in a spiral or coiled configuration,
occasionally with a lucent center.
The calcifications may or may not be associated with a mass representing chronic granuloma or dilated lymphatic vessels (13,14,15);
PARACOCCIDIOIDOMYCOSIS
Paracoccidioidomycosis (also known as South American blastomycosis) is caused by the fungus Paracoccidioides brasiliensis.
The disease is prevalent in South andCentral America (17);
Usually occurs in farmers,
manual laborers,
and other workers engaged in rural occupations and is probably caused by inhalation,
which results in primary pneumonia and secondary systemic dissemination (18,19);
The lungs are the main target organ and the main cause of morbidity and mortality in these patients.
The disease is usually asymptomatic but can progress to severe pulmonary involvement,
leading to cough and shortness of breath (18,19);
Imaging Features
Single or multiple nodules (Fig.
15)
Commonly cavitated
Progressive consolidation,
scarring,
and cavitation
May resemble tuberculosis but tends to involve mainly lower lobes
Other manifestations:
Hilar lymphadenopathy
Disseminated disease: In immunocompromised patient
ASCARIASIS AND STRONGYLOIDIASIS
Ascariasis and Strongyloidiasis are parasitic infections caused by nematodes that present with similar imaging findings (22).
The nematode Ascaris lumbricoides is acquired by ingesting food or fluids contaminated with feces.
The infection is distributed worldwide and is one of the most common parasitic infections,
affecting 1.3 billion people and causing approximately 1,550 deaths per year (Fig.
16) (20);
Parasites migrate from the small intestine to the pulmonary circulation,
where they mature and cause destruction of capillaries and alveolar walls with subsequent edema,
hemorrhage,
and epithelial cell desquamation,
causing chemotaxis of neutrophils and eosinophils (20,
22-26);
Patients complain of fever,
cough,
and expectoration and may have peripheral blood eosinophilia.
The diagnosis is confirmed by identifying larvae in the sputum or eggs in the stool (22,27);
Humans are the primary host of Strongyloides stercoralis,
a microscopic nematode with infective larvae that invade the lungs and small intestine by migrating from the soil through the skin (Fig.
17) (9-17);
A chronic pathway of continuous autoinfection can lead to a massive and life-threatening parasitic infestation (hyperinfection syndrome),
especially in patients with AIDS and in those who are receiving corticosteroid therapy,
in whom mortality may exceed 70% (18);
This parasite is found in all tropical and subtropical regions.
Approximately 35 million people are infected worldwide (9);
Clinical manifestations include pneumonia,
bronchospasm or bronchitis,
abdominal pain,
and diarrhea.
The patients usually have peripheral eosinophilia.
Hyperinfection occurs in severely immunocompromised patients,
in whom eosinophilia may be absent.
Definitive diagnosis is made by identifying the larvae in the sputum (18-21);
Imaging Features
Patchy,
fleeting areas of airspace consolidation (Fig.
18)
Focal areas of consolidation (Fig.
19)
Rarely:
Strongyloides hyperinfection in immunocompromised patient, Miliary pattern,
ARDS
TUBERCULOSIS
Tuberculosis is a chronic,
recurrent,
contagious infection caused by Mycobacterium tuberculosis.
It is a major cause of morbidity and mortality worldwide (33-25);
Patients with active pulmonary TB may be asymptomatic,
have mild or progressive dry cough,
or present with multiple symptoms including fever,
fatigue,
weight loss,
night sweats,
and cough hemoptysis (36);
Inhaled mycobacteria are phagocytized by alveolar macrophages and lead to the formation of parenchymal granulomas. The initial focus of parenchymal disease is termed the Ghon focus.
It either enlarges as the disease progresses or,
much more commonly,
undergoes healing.
Healing may result in a visible scar that may be dense and contain foci of calcification.
During the early stage of infection,
organisms commonly spread through lymphatic channels to regional hilar and mediastinal lymph nodes and through the bloodstream to more distant sites in the body.
The combination of the Ghon focus and affected lymph nodes is known as the Ranke complex (37);
The initial infection is usually clinically silent.
Development of specific immunity is usually adequate to limit further multiplication of the bacilli (38).
Some of the bacilli remain dormant and viable for many years.
In approximately 5% of the infected population,
endogenous reactivation of latent infection develops many years after the initial infection (39).
Such reactivation is frequently associated with malnutrition,
debilitation,
or immunosuppression (40);
Postprimary TB tends to involve predominantly the apical and posterior segments of the upper lobes and the superior segments of the lower lobes (37,
41).
The main abnormalities are progressive extension of inflammation and necrosis,
frequently with the development of communication with the airways and cavity formation (37).
Hematogenous dissemination may result in miliary TB;
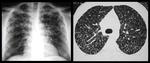
Imaging Features
Primary tuberculosis:
Hilar and/or mediastinal lymphadenopathy
Airspace consolidation
Consolidation may involve upper or lower lung zones
Pleural effusion
Postprimary tuberculosis (Fig.
20):
Apical and posterior segment of upper lobe predominance
2-4 mm diameter centrilobular nodules
Tree-in-bud pattern
Patchy or lobular consolidation
5-10 mm diameter nodules
Cavitation
Bronchovascular distortion
Hilar and/or mediastinal lymphadenopathy
Pleural effusion
Miliary tuberculosis:
1 to 3 mm diameter nodules randomly distributed throughout both lungs (Fig.
21)
Thickening of interlobular septa and fine intralobular networks are frequently evident
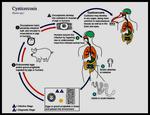
CYSTICERCOSIS
Cysticercosis is an infection of both humans and pigs with the larval stages of the parasitic cestode,
Taenia solium (Fig.
22).
The tapeworm that causes cysticercosis is found worldwide.
Infection is found most often in rural,
developing countries with poor hygiene where pigs are allowed to roam freely and eat human feces. In the United States affects mainly immigrants from Latin America,
where the disease is endemic.
However,
cysticercosis acquired in the United States has been repeatedly documented,
and travel-related infection in US-born persons has been reported.
The symptoms of cysticercosis are caused by the development of cysticerci in various sites. Of greatest concern is cerebral cysticercosis (or neurocysticercosis),
which can cause diverse manifestations including seizures,
mental disturbances,
focal neurologic deficits,
and signs of space-occupying intracerebral.In some cases,
inflammation around degenerating cysticerci may have severe consequences,
including focal encephalitis,
edema,
and vasculitis.
The most frequent symptom is epilepsy () Extracerebral cysticercosis can cause ocular,
cardiac,
or spinal lesions with associated symptoms. Asymptomatic subcutaneous nodules and calcified intramuscular nodules can be encountered.
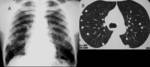
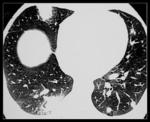
Figure 23 demonstrates multiple pulmonary nodules in a patient with cysticercosis.
DIROFILARIASIS
Human pulmonary dirofilariasis is a rare disease caused by the parasite Dirofilaria immitis.
The usual hosts of these infective nematodes are domestic and wild carnivores.
Human dirofilariasis typically manifests as either subcutaneous nodules or lung parenchymal disease,
in many cases asymptomatically.
The clinical implication of human dirofilariasis is that,
in many cases,
pulmonary lesions and,
less commonly,
subcutaneous lesions are initially misidentified as malignant tumors,
requiring invasive investigation and surgery before the correct diagnosis is made.
The pathology of the condition results from the aberrant localization of immature worms intended for nonhuman hosts.
Although this disease is considered benign,
its diagnosis often requires an excisional lung biopsy.
Imaging features
Pulmonary nodules (Fig.
24)
Lung parenchymal disease