Keywords:
Infection, Epidemiology, Education and training, Socio-economic issues, Screening, Diagnostic procedure, Ultrasound, CT, Thorax, Lung
Authors:
D. Cozzi1, F. Giannelli1, C. Moroni1, E. Cavigli2, A. Bindi2, F. Rinaldi1, P. G. Rogasi1, M. Bartolucci1, V. Miele1; 1Florence/IT, 2Firenze/IT
DOI:
10.26044/esti2019/P-0062
Results
All patients underwent BAL that confirmed TB infection in 23/33 (70%).
LUS was negative in 3/33 patients (10.1%) because of the absence of subpleural alterations detectable with an ultrasound exam.
LUS was positive in 30/33 patients (90.9%).
In these patients,
we found:
- parenchymal-subpleural consolidations in 25/30 (83.3%)
- interstitial syndrome (b-lines,
comet-tail artifact) in 20/30 (66.7%)
- pleural effusion with parenchymal atelectasis in 5/30 (16.7%)
- cavitated areas in 6/30 (20%)
- pleural empyema in 1/30 (3.33%)
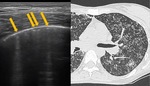
- miliary TB in 1/30 (3.33%)
Only in one patient,
we found multiple subpleural micronodules that referred to miliary distribution of TB infection (Fig.
1).
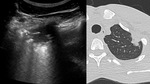
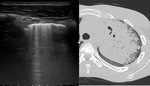
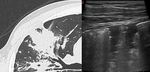
The extension of parenchymal involvement detected with LUS was consistent with the evidence of subpleural alterations in CT in 93% of cases (Fig.
2-3).
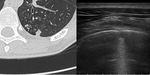
Upper and middle lobes were often involved.
Lowe lobes were usually involved in case of more aggressive disease (Fig.
4-5).
Using only LUS,
it was not possible to distinguish patients with active TB (BAL +) or not (BAL -).