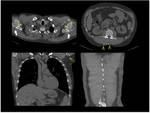
Interstitial lung disease and pulmonary arterial hypertension are the main causes of mortality and morbidity among patients with collagen vascular diseases. Intrathoracic involvement may also be secondary to the disease therapy,
including drug toxicity and infections by bacteria or opportunistic organisms,
as a result of immunosuppression.1,2 Thoracic manifestations of CVD also include disease specific findings,
for example necrobiotic nodules in RA,
lupus pneumonitis,
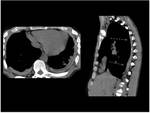
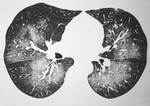
esophageal dilatation and dysmotility among patients with SScl and hypoventilation due to weakness of the respiratory muscles in polymyositis (Fig.
1).
Interstitial lung disease
Interstitial pneumonias represent the most common intrathoracic manifestations of CVD.
Collagen vascular diseases may be associated with virtually all patterns of diffuse interstitial pneumonia and may progress to pulmonary fibrosis.2
Most often,
interstitial pneumonia arises within the context of an established CVD,
but it is not uncommon for the interstitial pneumonia to be the first,
and possibly the sole,
manifestation of an otherwise occult CVD3.
The occurrence of interstitial lung disease may precede the development of clinical CVD for months or even for years2.
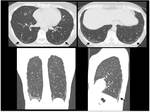
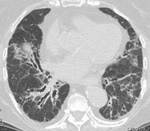
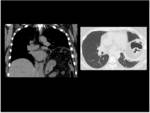
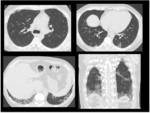
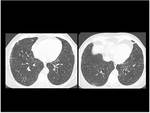
The most common histologic pattern of interstitial lung disease in patients with CVD is the nonspecific interstitial pneumonia (NSIP) (Table 1) (Fig.
2).
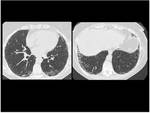
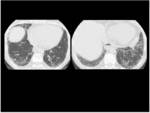
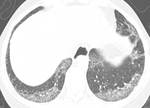
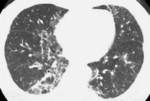
In patients with rheumatoid arthritis,
however,
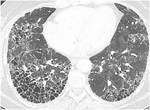
the pattern of usual interstitial pneumonia (UIP)is the most frequent one (Fig 3).
On the other hand,
lymphocytic interstitial pneumonia (LIP),
although rare,
is most common in patients with Sjögren’s syndrome,
while the cryptogenic organizing pneumonia (COP) is more common in inflammatory myopathies and the diffuse alveolar damage (DAD) pattern is more frequent in patients with dermatopolymyositis and systemic lupus erythematosus.
(Tables 1 and 2) 1,2
The concomitant presence of more than one pattern of interstitial pneumonia,
particularly the association between NSIP and COP is not rare in collagen vascular disease,
and is most common in patients with dermatopolymyositis and mixed connective tissue disease2.
In general,
chronic progressive interstitial pneumonias in collagen vascular diseases have a better prognosis than those of idiopathic nature.
Although rare,
patients with CVD,
especially rheumatoid arthritis,
scleroderma and dermatopolymyositis,
may progress with acute exacerbation of fibrotic interstitial pneumonia,
the outcome in these cases is unfavorable.
HRCT findings of acute exacerbation of chronic progressive interstitial pneumonia in these patients consist in diffuse areas of ground-glass attenuation,
superimposed on the underlying reticular abnormalities4.
The main differential diagnosis includes opportunistic infections (particularly by Pneumocystis) and drug-induced lung disease.
Pulmonary Arterial Hypertension
Pulmonary arterial hypertension is defined by a mean resting pulmonary artery pressure of ≥25 mm Hg and a pulmonary capillary wedge pressure of ≤15 mm Hg.
Patients with collagen vascular diseases are considered to have a higher risk for pulmonary arterial hypertension,
which may occur in isolation or in combination with interstitial lung disease in this group of patients.
Pulmonary arterial hypertension is more common in patients with SScl (25% of cases) and mixed connective tissue disease.
It is less common in systemic lupus erythematosus (5%–10%) and even rarer in patients with rheumatoid arthritis,
polymyositis or dermatomyositis,
or Sjögren syndrome.1
Although the pathophysiologic mechanisms of pulmonary arterial hypertension in collagen vascular diseases are not completely understood,
the histologic features resemble those seen in the presence of primary pulmonary hypertension.
Thromboembolic disease also may play a role in patients with pulmonary arterial hypertension associated with collagen vascular disease,
especially in those with systemic lupus erythematosus and antiphospholipid antibodies.
The most common clinical manifestation of pulmonary arterial hypertension is dyspnea during physical exertion,
a nonspecific symptom.
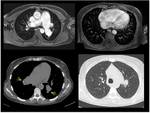
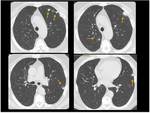
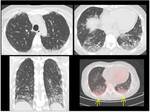
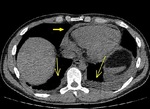
HRCT in patients with pulmonary arterial hypertension may show:
- increased diameter of the pulmonary arterial trunk (>2.9 cm),
main pulmonary arteries and their segments (Fig.
4);
- artery wall calcification may be identified in patients with severe and longstanding hypertension,
as well as thrombi (Fig.
4);
- enlargement of the right heart chambers (Fig 4) and azygos-hemiazygos venous system;
- contrast material reflux into the inferior vena cava and hepatic veins,
a result of elevated right heart pressures;
- centrilobular nodules and diffuse or patchy ground-glass opacities (may represent proliferation of small muscular arteries,
deposition of cholesterol granulomas,
focal areas of hemorrhage) (Fig.
4);
- pericardial effusion is a common finding that indicates a poor prognosis.
Rheumatoid Arthritis
Rheumatoid arthritis is a common collagen vascular disease,
wich occurs more often in women,
with the highest incidence between 25 and 50 years-old.
Approximately 50% of the patients present some form of extraarticular involvement.
Lung disease is the second most common cause of death (18% of patients with rheumatoid arthritis),
after infection.1
The most frequently intrathoracic manifestation are:
- pleural disease (thickening or effusion),
which is found in up to 70% of patients (Fig.5);
- large or small airways disease - bronchiectasis (up to 30% of cases) (Fig.
6),
constrictive bronchiolitis and follicular bronchiolitis;
- cricoarytenoid arthritis,
frequently overlooked,
with symptoms diverse and nonspecific (dyspnea,
soreness or fullness in the throat,
hoarseness,
dysphagia…);
- interstitial lung disease (5%),
mainly UIP (Fig.
7) and NSIP,
also COP and LIP;
- rheumatoid pulmonary nodules – occur more often in men,
usually smokers with subcutaneous nodules and high rheumatoid factor titers.
Nodules may cavitate,
increase in size or resolve spontaneously (Fig.
8).
Systemic Lupus Erythematosus
Systemic lupus erythematosus is a complex systemic autoimmune disease,
with numerous immunologic and clinical manifestations.
The disease occurs predominantly in women of reproductive age (≥ 90% of cases).
The most frequent intrathoracic manifestations of LE are:
- pleural effusions are present in 30-50% of the patients during the course of the disease.
- pleuritis: chest pain,
usually associated with fever,
cough and dyspnea.
- infectious diseases - second most frequent cause of death;
- acute pneumonitis – uncommon,
but associated with high mortality rates,
characterized by acute onset of clinical signs and symptoms that may include a fever,
dyspnea,
a cough,
pleuritic chest pain,
and arterial hypoxemia.
Histopathologic findings of diffuse alveolar damage (DAD);
- alveolar hemorrhage – also rare and severe.
An abrupt onset of symptoms,
new radiographic or CT findings of diffuse alveolar opacities,
and a decrease in the serum hemoglobin level,
with or without hemoptysis,
suggest the diagnosis (Fig.
9);
- thromboembolic disease – usually associated with active disease and the presence of antiphospholipid antibodies;
- Interstitial lung diseases – rare in LE,
mainly NSIP;
- shrinking lung syndrome - a progressive loss of lung volume with associated dyspnea and pleuritic chest pain.
Restrictive defect on pulmonary functions tests,
with absent or minimal imaging findings of unilateral or bilateral diaphragmatic elevation without evidence of parenchymal lung disease (Fig.
10).
Progressive Systemic Sclerosis
Progressive systemic sclerosis (SScl) is a chronic multisystem autoimmune disease of unknown etiology with a characteristic pathophysiologic triad of inflammation,
vascular damage,
and fibrosis.
It occurs predominantly in women,
with a peak incidence in those between 45 and 64 years of age.
Pulmonary involvement is common in patients with SScl and most often comprises interstitial lung disease and pulmonary vascular disease leading to pulmonary arterial hypertension.
The most frequent thoracic manifestations are:
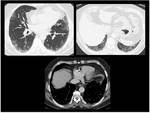
- interstitial lung diseases – mainly NISP and,
less frequently UIP; ground-glass opacities that are irreversible after treatment are extremely common (Fig.11 and Fig.12);
- pulmonary hypertension in almost 15% of the patients;
- esophageal involvement – (97% of patients) dysmotility and enlargement,
leading to aspiration pneumonia and bronchiolitis.
HRCT findings consist of bronchiectasis,
bronchiolectasis,
mucous plugs,
centrilobular nodules and patchy opacities (Fig.
11).
Patients with SScl have a high incidence of esophageal and pulmonary involvement,
especially interstitial disease pattern of NSIP and pulmonary arterial hypertension.
Esophageal dysmotility can lead to aspiration pneumonia and bronchiolitis.
Polymyositis and Dermatomyositis
Polymyositis and dermatomyositis (PM/DM) are the most common inflammatory myopathies,
a heterogeneous group of idiopathic diseases of skeletal muscle that are manifested by weakness and inflammation.
Polymyositis usually is manifested as a subacute myopathy,
with weakness of the proximal muscles that evolves over weeks or months.
Dermatomyositis is distinguished from polymyositis by characteristic cutaneous manifestations that either precede or accompany the evolution of muscle weakness,
typically a heliotrope rash (bluepurple discoloration) on the upper eyelids and a raised violaceous rash (Gottron papules) over the knuckles.
These diseases occur more frequently in women,
with a peak of incidence between 40 and 50 years-old.
Pulmonary involvement of the inflammatory myopathies may be secondary to:
- compromised function of the respiratory muscles;
- interstitial lung disease,
mainly NSIP and COP,
both patterns can be often seen in the same patient (Fig.
13);
- aspiration-related pneumonia due to weakness of the pharyngeal muscle, with aspiration-related pneumonia probably being the most common occurrence.
- calcinosis: complication of dermatomyositis more common in pediatric and adolescent than in adult patients,
characterised by the deposition of insoluble salts of calcium in skin,
subcutaneous tissues and muscle,
which may be responsible for pain and functional disability.
May be a consequence of untreated or unaggressively treated dermatomyositis (Fig 14).6
Mixed Connective Tissue Disease
Mixed connective tissue disease is a condition in which manifestations of systemic lupus erythematosus,
rheumatoid arthritis,
progressive systemic sclerosis,
and polymyositis or dermatomyositis are combined.
The disease is characterized by the following clinical and laboratory findings: Raynaud phenomenon,
swollen hands,
arthritis or arthralgia,
acrosclerosis,
esophageal dysmotility,
myositis,
pulmonary hypertension,
a high titer of speckled fluorescent antinuclear antibodies,
and the presence of a moderate to high serum level of antibodies against ribonucleoprotein.
Ninety percent of those affected are female,
and the highest incidence is in the 2nd and 3rd decades of life.
The most important thoracic complications in mixed connective tissue disease are:
- pulmonary arterial hypertension - up to 45% of patients,
predictive of poor prognosis;
- interstitial lung disease,
mainly NSIP (Fig 15),
but also UIP,
LIP and COP;
- esophageal motor impairment,
with gastroesophageal reflux;
- pleural thickening or effusion (Fig.
16).
Sjögren Syndrome
Sjögren syndrome is an autoimmune disease characterized by T lymphocyte infiltration of various organs,
most often the lacrimal and salivary glands and respiratory tract.
It usually affects women in the 4th or 5th decade of life.
The syndrome can be classified as primary,
when it occurs in the absence of other disorders,
or secondary,
in association with an underlying condition,
usually a collagen vascular disease.
Symptoms include: xerophthalmia (dry eyes),
xerostomia (a dry mouth) and extraglandular manifestations in one-third of patients (dryness and crusting of the nasal mucosa,
epistaxis,
otitis media,
dry cough,
dyspnea and recurrent bronchitis.
Main thoracic manifestations are:
- interstitial lung diseases,
including LIP (Fig.
17),
NSIP,
UIP,
OP.
- airway diseases – bronchiectasis and follicular and constrictive bronchiolitis.
- amyloidosis – nodular (single or multiple nodules,
usually in patients with SS and LiP,
may have foci of calcification and localization in the pulmonary parenchyma or within pulmonary cysts) and diffuse presentation - rare,
but may be found in patients with RA and SS (diffuse micronodules and interlobular septal thickening).
Patients with Sjögren syndrome have an increased risk for lymphoma,
usually B cell type,
which arises in the salivary glands or from mucosa-associated lymphatic tissue in the stomach and lung.
Pulmonary lymphoma should be suspected if consolidation,
large nodules,
or effusions are present.
Interstitial Pneumonia with Autoimmune Features (IPAF)
Interstitial pneumonia with autoimmune feature (IPAF) is a newly recognized term that comprises patients with interstitial pneumonia,
including NSIP (Fig.
18),
OP and LIP,
and features suggestive of a CTD that do not meet established classification criteria for a characterizable CTD.3
Other features that may be present in these patients are: unexplained intrinsic airways disease (bronchiolitis or bronchiectasis),
peribronchovascular cysts and pulmonary hypertension,
pleural (Fig.
20) or pericardial abnormalities.3
Treatment complications
Drug Toxicity
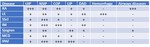
Several drugs used to treat patients with CVD have been associated with drug-induced lung injury (Table 3).
Drug-induced interstitial lung disease (DI-ILD) is a diagnosis of exclusion and requires: (1) detailed history of drug exposure; (2) clinical,
radiological,
and histopathologic patterns consistent with previous observations with the same drug; (3) exclusion of other possible causes; (4) improvement after drug removal; and (5) recurrence of identical symptoms after drug reintroduction.5 DI-ILD have usually a satisfactory prognosis,
when timely diagnosed.
However,
failure to identify DI-ILD may significantly increase patient morbidity and mortality.
Clinical and radiological findings of DI-ILD are nonspecific and usually mimic those of opportunistic infections or of exacerbation of CTD-related lung disease.
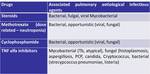
Methotrexate is considered to be the drug with more potential to cause DI-ILD among all the medications used to treat patients with CVD; the most common manifestations are NSIP,
hypersensitivity-like reactions resembling hypersensitivity pneumonitis and COP (Fig.
19).
Patients usually become symptomatic months after starting the treatment.5,7
Toxicity to cyclophosphamide may occur between 2 weeks and 13 years after drug administration and usually presents as DAD,
NSIP,
or COP.7Both methotrexate- and cyclophosphamide-induced lung toxicities show no evident relationship with dose and duration of therapy and are associated with satisfactory prognosis after drug withdrawal.7Association between TNFα antagonists and new-onset or exacerbation of ILD is also described in the literature.7
Opportunistic Infections
Patients with CTDs have increased risk of developing pulmonary infections.
Although intrinsic immunologic abnormalities predispose the patient to nonspecific infections (such as community-acquired pneumonia in LE and aspiration pneumonia in SScl),
severe immunosuppression related to several therapeutic agents (e.g.,
corticosteroids,
methotrexate,
and cyclophosphamide) might lead to atypical or more severe pulmonary and systemic infections (Table 4).5
Immunosuppression is more commonly associated with the drugs used to treat these disorders than with the diseases themselves.8High-dose corticosteroids reduce lymphocyte and antigen presenting cell function,
increasing the risk of unchecked growth of even weakly pathogenic bacteria,
viruses,
fungi,
and mycobacteria.
Extensive or disseminated infectious complications may develop with a paucity of inflammatory signs or symptoms.
8Methotrexate,
a folate antimetabolite,
interferes with numerous intracellular metabolic processes,
particularly affecting cell proliferation.
For this reason,
it is effective in treatment of a number of malignancies and inflammatory conditions.
Even at low doses,
methotrexate inhibits the replication and function of T and B lymphocytes and can suppress secretion of proinflammatory cytokines,
including interleukin (IL)-1,
IFN-,
and tumor necrosis factor (TNF).
It also decreases chemotaxis of neutrophils.
The effects are dependent on the dose and length of exposure.
Most infections associated with methotrexate are a result of absolute neutropenia.
8 Cyclophosphamide functions as an alkylating agent and is active against many neoplastic diseases and in lupus nephritis,
nephrotic syndrome,
Wegener’s granulomatosis,
rheumatoid arthritis,
and graft-versus-host disease or graft rejection.
Cyclophosphamide also causes lymphopenia (both B cells and T cells) and selective suppression of T- and B-lymphocyte activity.
8
Successful management of any immunocompromised patients requires a high index of suspicion for infection,
frequent clinical assessment,
and aggressive diagnostic approaches that include biopsy or sampling of any organ that seems abnormal.
8
As treatment with high doses of corticosteroids or immunosuppressive drugs is associated with reactivation of latent tuberculosis,
regular screening is recommended in countries where tuberculosis is endemic.5